Click on the DVD icon to watch the video
Aim
The aim of this chapter is to emphasise the importance of deflective contacts, interferences and parafunction in causing damage to both teeth and restorations. We recommend that readers view animations G–I to bring to life figures marked with DVD logos.
Outcome
At the end of this chapter, the clinician should:
-
understand what is meant by the terms centric relation (CR), retruded contact position (RCP) and slide between RCP and intercuspal position (ICP)
-
recognise the influence of damaging deflective contacts, anterior thrust and interferences
-
realise the potential consequences of tooth preparation on “pivoting” deflective and interfering contacts
-
understand what is meant by parafunction and the damage it may cause
-
realise that if problems of occlusal overloading (unexplained pain, attrition, abfraction, drifting and mobility, as well as damage and decementation of restorations) are not explained by function they may be explained by parafunction.
Introduction
In Chapter 2 we talked about normal, functional movements of the mandible, where guidance teeth take on the role of smoothly directing the movement of the mandible into the ICP. We also introduced the concept of interferences to that smooth movement: tooth contacts that disrupt movement by getting in the way. In the first half of this chapter, we introduce the concept of deflective contacts and further explore the potentially deleterious properties of interferences. In the second half, we consider parafunction and the ways in which its effects can be especially damaging to teeth, restorations and supporting tissues.
Deflective Contacts and Excursive Interferences
So far, we have built our understanding of occlusion using ICP as a starting point. This position is fundamentally important to occlusion, but it is dictated entirely by the teeth. To understand interferences and deflective contacts fully we need to take on board the concept of CR, a concept that is not at all related to the teeth, but is completely dictated by the temporomandibular joints (TMJs).
Centric Relation
During function, the mandible travels towards ICP within an envelope of movement defined by the guidance surfaces of the anterior teeth. So far, we have considered the lateral and protrusive guiding surfaces, but at least 90% of the population are also able to move their jaws distal to ICP. This is because for most of us there is a small discrepancy between the musculoskeletally stable position of the mandible, which is determined by the TMJs, and the position of stability determined by the teeth (ICP).
The stable position of the condyles within the TMJs is known as CR. This is defined variously as the most superior-posterior, most superior or most superior-anterior position of the condyles within the glenoid fossae (see Fig 3-1). While academics continue to argue about which of these positions they are talking about, this argument is of little practical relevance. Dentists take a more pragmatic approach to find CR and use manipulative techniques, which comfortably seat the condyles into their most superior position within the glenoid fossae. In this position, the articular discs should be correctly interposed and the mandible can arc around its “terminal hinge axis”. It is a position of health that does not occur in a diseased TMJ in which, for example, there is a disc displacement or arthritis. To find CR we use the technique of bimanual manipulation to guide the mandible; this is such an important and useful skill for understanding occlusion that there is an entire section in this book (Section 8-4) and DVD video (M) to explain how to do it.
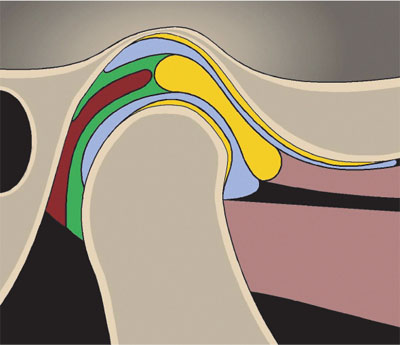
Fig 3-1 CR with the condyles in their most superior position in the glenoid fossae with the discs correctly interposed.
Yellow – fibrocartilage disc and joint surfaces; light brown – superior and inferior lateral pterygoid muscles; dark brown – vascular retrodiscal tissues; green – superior and inferior retrodiscal laminae; blue – synovial fluid in superior and inferior joint spaces.
Retruded Contact Position 
This is simply the relationship between the mandible and maxilla on the terminal hinge axis when the first point of tooth contact occurs. This usually occurs between the posterior teeth (see Fig 3-2). From here the mandible can slide into ICP. The DVD animation G shows this clearly. In a proportion of the population (usually around 10%) this point of contact is ICP; in other words, the patient hinges straight into ICP because ICP lies on that retruded arc of closure. In the remaining 90% of the population there is a slide from the RCP into ICP.
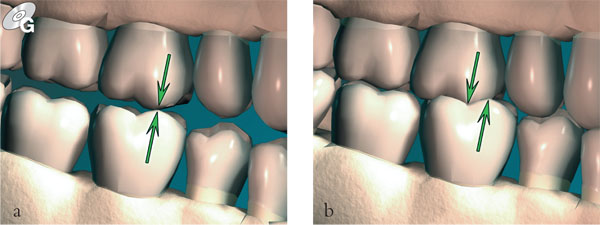
Fig 3-2 (a) RCP: the first tooth contact in CR; (b) the mandible then slides into ICP.
RCP–ICP Slide 
This slide is usually 0.5 to 1 mm in length when viewed at the incisors, but depending on the nature of the tooth contact it can be up to several millimetres long. The direction of the slide is best described in terms of vertical, horizontal and lateral components (see Figs 3-3 and 3-4). To assess a slide you need to view what happens at the incisors from both the side and the front of the patient. With a vertical slide, the mandible moves little, if any, from its retruded arc of closure. With a horizontal slide, the mandible translates forwards so that the lower incisors appear to move both upwards and anteriorly when viewed from the side. With a lateral slide the mandible rotates slightly, with one condyle moving further forward in the slide than the other does. The result is that the mandibular incisor midline shows a shift either to the right or the left between RCP and ICP (see Fig 3-4). The patient examined before an occlusal adjustment in DVD video K (see Sections 8-1 and 8-7) illustrates both horizontal and lateral components of slide.
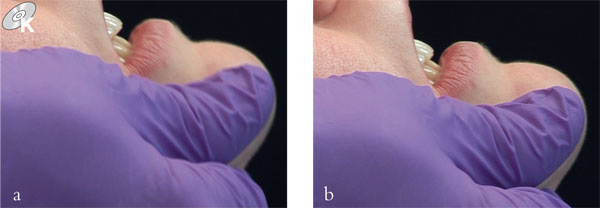
Fig 3-3 Bimanual manipulation of the RCP–ICP slide viewed laterally. (a) Incisor relationship in RCP. (b) Incisor relationship in ICP – the mandible has moved superiorly and anteriorly to this position. The forwards translation (here about 1.5 mm) is the horizontal component of the slide.
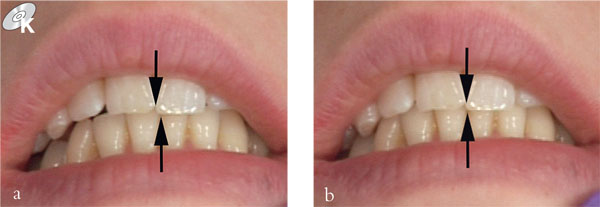
Fig 3-4 The same slide from RCP–ICP as Fig 3-3 viewed anteriorly. (a) Incisors separated by posterior RCP contact between the upper and lower left second premolars. (b) Incisor relationship in ICP. Arrows show the lateral component of the slide.
Deflective Contact 
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


