Chapter 4
Pharmacology and Minor Oral Surgery
Aim
This chapter describes the use of drugs in minor oral surgery.
Outcome
After reading this chapter you will have an understanding of the use of drugs to aid the practice of minor oral surgery.
Introduction
The successful practice of surgery is dependent upon the proper use of drugs. The most obvious example is the provision of anaesthesia during surgical procedures. This chapter will consider the following:
-
pain control
-
anxiety control
-
antibacterial drug use
-
other agents used in minor oral surgery.
Pain Control
Pain control is important at two stages of surgery. These are:
-
operative pain control
-
post-operative pain control.
Operative Pain Control
The practice of pain control for minor oral surgery involves the use of local anaesthesia with or without conscious sedation (see below). The need for general anaesthesia requires referral to a specialist centre such as a hospital clinic.
What is the best local anaesthetic for surgical dentistry? A number of factors have to be considered. An important one is the patient’s medical status. On the basis that the patient is healthy, what is the best choice? In order to reduce operative haemorrhage, a vasoconstrictor-containing solution is required (Fig 4-1). Two different vasoconstrictors are available in local anaesthetic solutions in many countries. These are epinephrine (adrenaline) and felypressin (octapressin). The former produces superior haemorrhage control. Thus an epinephrine-containing solution is preferred.
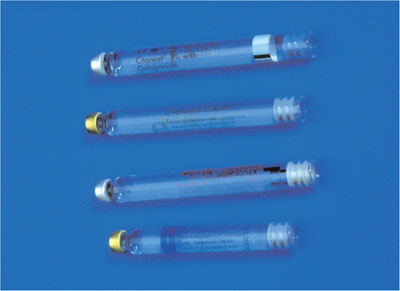
Fig 4-1 A number of local anaesthetic solutions are available for use in dental cartridges. A vasoconstrictor containing solution such as lidocaine with epinephrine is the local anaesthetic of choice for surgical procedures in the mouth.
The use of long-acting local anaesthetics such as bupivacaine or levobupivacaine may help in reducing post-operative pain (see below). However, the operative anaesthesia they produce is not as good as lidocaine with epinephrine. Additionally, in some countries the long-acting agents are not available in dental local anaesthetic cartridges (Fig 4-2).
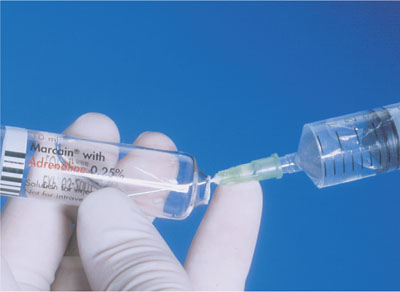
Fig 4-2 Long acting local anaesthetic solutions such as bupivacaine or levobupivacaine can aid post-operative pain control.
Therefore the solution of choice is 2% lidocaine with epinephrine. Mepivacaine (2%) with epinephrine or 4% articaine with epinephrine are alternatives although the latter is best avoided if block anaesthesia is being used, given the potential problem of long-lasting paraesthesia with this drug concentration.
Post-operative pain control
As mentioned above, the use of long-acting local anaesthetics such as levobupivacaine can prolong the duration of anaesthesia and thus reduce postoperative pain experience. It is important to point out that, to achieve this effect, long-acting agents must be employed as regional blocks. When used as infiltration anaesthesia there may be prolonged soft-tissue numbness, but the onset of post-operative pain does not differ from that occurring after the use of a conventional local anaesthetic such as lidocaine.
The mainstay of post-operative pain control is the use of analgesics. As the pain of surgery is inflammatory in nature, it is best controlled by non-steroidal anti-inflammatory drugs. When non-steroidals are contraindicated the drug of choice is paracetamol (up to 1g four times daily). The pain usually begins in the early post-operative period and thus the early use of analgesics is essential. Indeed, the ideal time to commence analgesic therapy is before surgery begins. This is because non-steroidal analgesics prevent the occurrence of pain rather than treat an established pain. The use of analgesics prior to surgery is known as pre-emptive analgesia. Surprisingly, studies into the effectiveness of pre-emptive analgesia have shown conflicting results. Ibuprofen and COX 2 inhibitors have shown a pre-emptive effect. COX 2 inhibitors are not recommended at present, as they have been implicated in the production of cardiovascular complications. Thus the drug of choice is ibuprofen, unless contraindicated. When using ibuprofen a dose of 400mg should be taken around 30 minutes before surgery. Therapy should continue for a variable time dependent upon the surgery performed. The pain following soft tissue biopsy reduces considerably within 24 hours. On the other hand, discomfort following the removal of third molar teeth is still app/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


