Chapter 3
Principles of Minor Oral Surgery
Aim
This chapter describes the principles involved in minor oral surgery.
Outcome
After reading this chapter you should have an understanding of the principles involved in the successful practice of minor oral surgery.
Introduction
As mentioned in Chapter 2, the successful practice of any form of surgery begins by taking a thorough history, reaching the correct diagnosis and formulating an appropriate treatment plan. Arriving at a diagnosis may involve performing pre-operative special tests such as radiography and pulp testing. Treatment planning includes the choice of anaesthesia.
It is imperative that the surgeon has a thorough knowledge of the anatomy of the area of interest. Surgery should be aseptic and as atraumatic as possible. The operator must have the appropriate instrumentation. Suggested instruments are listed in Table 3-1 and shown in Fig 3-1.
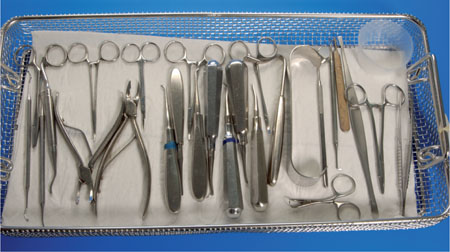
Fig 3-1 A tray of instruments for minor oral surgery.
| Suggested instrumentation for minor oral surgery |
| Scalpel handle and blades (11 and 15) |
| Periosteal elevators (Howarth’s) |
| Tissue retractors (Bowdler Henry/cheek/tongue) |
| Surgical handpiece and burrs |
| 20ml syringes for irrigation |
| Bone files |
| Rongeurs |
| Chisels |
| Osteotomes |
| Curettes (Mitchell’s trimmer) |
| Artery clips (Mosquito) |
| Scissors |
| Tissue forceps |
| Suture holders and sutures (resorbable and non-resorbable) |
| Dental elevators (straight (Couplands) and curved (Warwick James/Cryers)) |
| Dental extraction forceps |
| Mirror |
| Dental probe |
It is worth considering the steps involved in the removal of a buried root as an aid to discussing the principles. These steps are:
-
gaining informed consent
-
localisation of the root
-
operative pain control
-
incision
-
flap design
-
flap raising
-
bone removal
-
root removal
-
curettage and debridement
-
wound closure
-
post-operative pain control
-
review.
Gaining Informed Consent
This was discussed in Chapter 1. When performing surgical procedures it is good practice to obtain written consent. Written informed consent is essential when conscious sedation is used.
Localisation of the Root
This is achieved by clinical examination, both visual and by palpation. In addition radiographs are needed. Radiographs are useful because they:
-
aid in localisation
-
show any associated pathology
-
indicate the quality of surrounding bone
-
demonstrate the proximity of important structures.
Occasionally, it may be necessary to take different radiographs to locate the root using parallax. Such views may be two different intra-oral periapical films or panoramic and occlusal views.
Operative Pain Control
It is imperative that pain control is excellent if surgery is to be performed. As mentioned in Chapter 1, the mainstay for minor oral surgery is local anaesthesia with or without sedation. If pain control is unsatisfactory the procedure cannot be performed to the best standards. Excellent local anaesthesia has benefits at both ends of the syringe. The patient feels no pain and the clinician can work with reduced stress. The use of sedation can be helpful for some patients. However, sedation must not be used as a measure to counter poor local anaesthesia. This topic is discussed further in Chapter 4.
Incision
The incision should be made with a sharp disposable blade. If a number of incisions are involved the blade should be changed. The blade normally used in intra-oral surgery is the number 15 (Fig 3-2). A number 11 blade may be used on occasion (Fig 3-2).

Fig 3-2 Scalpel blades numbers 11 (left) and 15 (right).
The scalpel handle should be held like a pen and the incision made at 90° to the surface. When making an incision for a mucoperiosteal flap the incision is made down on to bone. This is important, as it means that when the flap is raised the bone is directly exposed and there is no soft tissue attached. Pressing the scalpel on to bone during the incision can blunt the blade. This is why the blade should be changed when there are multiple incisions.
Flap Design
The design is such that the flap:
-
is mucoperiosteal
-
has an adequate blood supply
-
avoids damage to important structures
-
allows adequate visibility
-
allows atraumatic reflection
-
has its edges on sound bone at the end of the procedure
-
can be replaced at the end of surgery without tension.
Many flaps have vertical />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


