Chapter 36 Principles of infection control
Cross infection
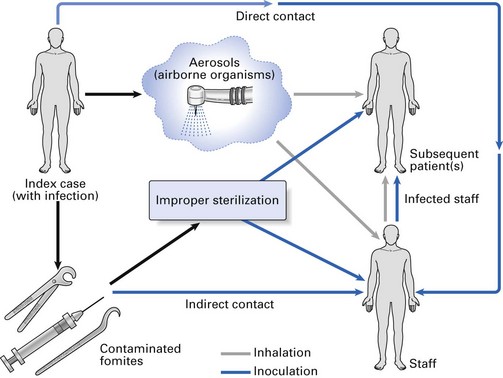
Cross infection may be defined as the transmission of infectious agents between patients and staff within a clinical environment. Transmission may result from person-to-person contact or via contaminated objects (fomites) (Fig. 36.1). Organisms capable of causing cross infection in humans are derived from:
Principles of infection transmission
Transmission of infection from one person to another requires:
2. a mode or vehicle by which the infective agent is transmitted, e.g. blood, droplets of saliva, instruments contaminated with blood, saliva and tissue debris. (Animals or insects may act as vehicles or vectors of transmission, for example, in malaria, but are not described here)
Source of infection
The sources of infection in clinical dentistry are mainly human; they include:
1. People with overt infections who liberate large numbers of organisms into the environment (e.g. droplets and discharges from the mouth or other portals; wounds, ulcers and sores on the skin). Fortunately, in routine clinical dentistry, few patients with acute diseases are seen.
2. People in the prodromal stage of certain infections. During the prodrome or the incubating period, the organisms multiply without evidence of infection; although patients are healthy at this stage, they are highly infectious. Viral infections, such as measles, mumps and chickenpox, easily spread in this manner.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses