Chapter 26 Infections of the gastrointestinal tract
Normal flora
Important pathogens
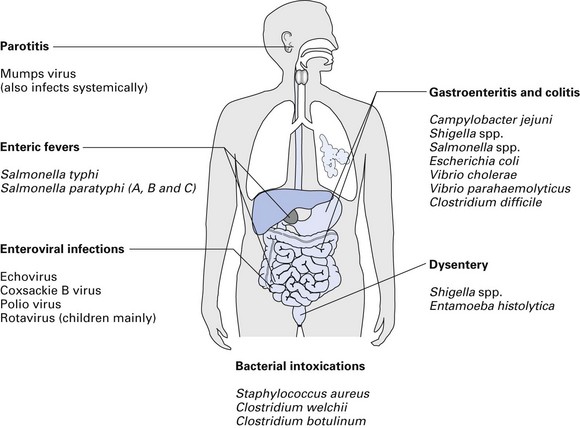
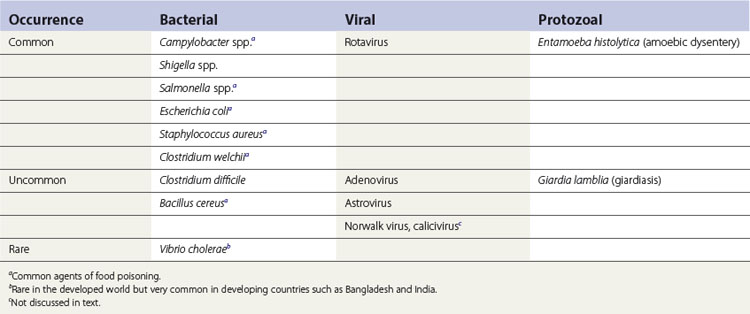
A diverse array of infections of the gastrointestinal tract is caused by an equally varied population of microbial agents (Fig. 26.1). The agents of diarrhoeal diseases, including those that are considered common agents of food poisoning, are listed in Table 26.1. The common bacterial diarrhoeal diseases in the developed world include those caused by:
Less common diseases include infections caused by Clostridium difficile and Bacillus cereus.
Common diarrhoeal diseases
Escherichia coli
E. coli is a normal commensal of the gastrointestinal tract, but certain strains, for some unknown reason, can behave as pathogens. As described in Chapter 15, they produce enterotoxins, and the enteroinvasive strains have the ability to invade the gut mucosa.
Pathogenesis and epidemiology
There are two types of E. coli diarrhoea:
Infantile gastroenteritis
Accompanied by acute and profuse diarrhoea, this infection has an incubation period of 1–3 days. The disease is mainly caused by enteropathogenic E. coli (EPEC), but in a minority of cases, enterotoxigenic E. coli (ETEC) strains contribute (Chapter 15). It is common in the developing world because of poor sanitation and poverty; infection spreads directly from case to case and via fomites (see above for shigellae), and in some cases, the mother may be the source of infection.
Diagnosis
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses