Chapter 21 Viruses of relevance to dentistry
This chapter gives an outline of the viruses that are of special relevance to dentistry. The DNA viruses are described first, followed by the RNA viruses (see Table 4.1).
DNA viruses
Papovaviruses
These DNA viruses infect both humans and animals; however, human disease is infrequent.
Skin warts
Herpesviruses
There are a range of different human herpesviruses, currently numbered 1–8 (see Table 4.3). All of them are structurally similar (enveloped, icosahedral with double-stranded DNA) and infect both humans and animals. They are the most common causes of human viral infections. All have the important property of remaining latent, with the ability to reinfect the host a variable period after the primary infection. Important human pathogens include herpes simplex virus types 1 and 2 (HSV-1 and HSV-2), varicella-zoster virus (VZV), cytomegalovirus (CMV) and Epstein–Barr virus (EBV) (see Chapter 4). Students of dentistry should be thoroughly conversant with the herpes group of viruses as the majority of them either cause oral infection or are intimately associated with orofacial tissues and saliva.
HSV (human herpesviruses 1 and 2)
Clinical disease
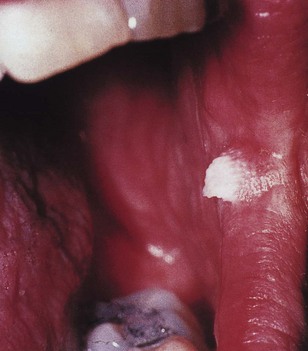
Primary infection
Recurrent infections
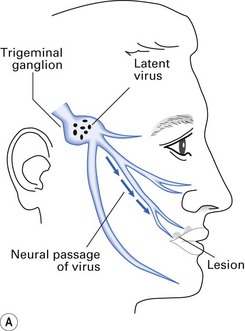
Recurrence or reactivation of HSV entails activation of the non-infectious form of the latent virus residing in the neurons of either the trigeminal ganglion (Fig. 21.3) or the sacral ganglia. Reactivation is provoked by menstruation, stress, sunlight (possibly ultraviolet rays), local trauma, etc.; the lesions tend to recur at the site of the primary lesion. HSV has been implicated in Bell’s palsy.
Epidemiology
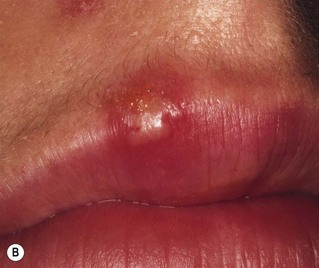
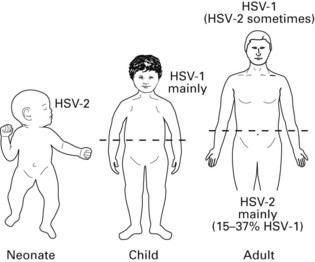
Humans are the only known reservoir for HSV-1 and HSV-2; experimental infection can be induced in animals and cell cultures. As the virus is highly labile, most primary infections are acquired through direct contact with a lesion or contaminated secretions. In general, HSV-1 causes orofacial lesions or lesions ‘above the belt’, while HSV-2 causes lesions ‘below the belt’, i.e. genital herpes (Fig. 21.4). However, because of sexual promiscuity or for other reasons, this may not be always true. HSV-1 is acquired early in life, while HSV-2 appears after the onset of sexual activity.
Diagnosis
Varicella-zoster virus (human herpesvirus 3)
Clinical disease
Zoster (shingles)
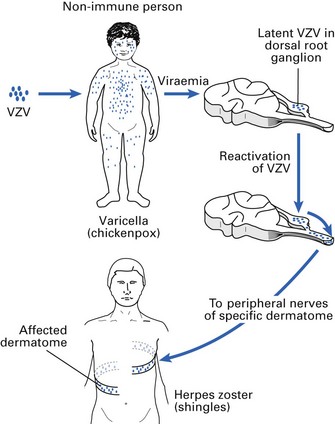
Occurs primarily as a reactivation of the virus in dorsal root or cranial nerve (usually trigeminal) ganglia (Fig. 21.6). The disease usually affects adults, and the virus is reactivated despite circulating antibodies. Zoster is triggered by trauma, drugs, neoplastic disease or immunosuppression.
The trigeminal nerve is affected in about 15% of cases, with involvement of the ophthalmic, maxillary and mandibular divisions (in that order of precedence). Severe localized oral pain precedes the rash and may be easily confused with toothache (see Chapter 35). Involvement of the ophthalmic nerve may lead to eye lesions and sometimes blindness.
Diagnosis
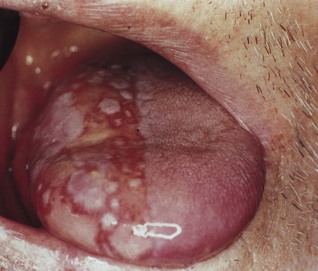
The clinical picture is pathognomonic, as the lesion distribution overlaps and accurately maps the distribution of the sensory nerve (Fig. 21.7). Serology, if needed, entails detecting a fourfold rise in antibody titre in paired sera (compare herpes simplex reactivation, where antibody rise is not significant).
EBV (human herpesvirus 4)
Infectious mononucleosis
Signs and symptoms
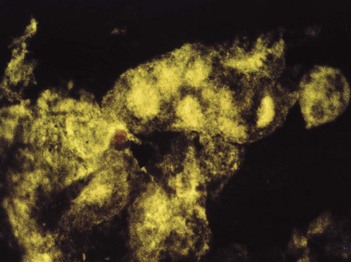
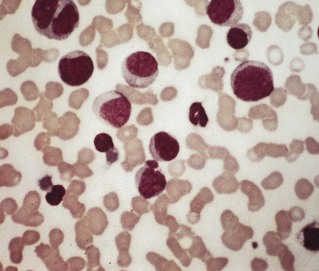
Low-grade fever with generalized lymphadenopathy and abnormal lymphocytes in the blood (note that a similar illness, glandular fever-like syndrome, develops during the first fortnight after infection with human immunodeficiency virus (HIV)). Fever, tonsillitis and fatigue are common, and many patients have splenomegaly. Lymphocytosis is a characteristic feature, hence the term ‘mononucleosis’; some 10% of the lymphocytes are atypical, with enlarged misshapen nuclei and increased cytoplasm (Fig. 21.8).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses