Chapter 32 Microbiology of dental caries
Classification
Dental caries can be classified with respect to the site of the lesion (Fig. 32.1):
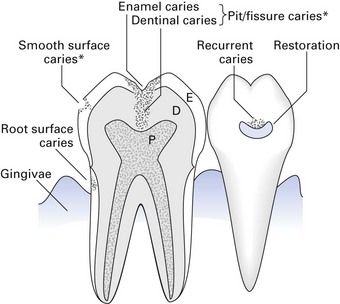
Fig. 32.1 Nomenclature of dental caries. D, dentine; E, enamel; P, pulp. *Also termed occlusal caries.
Clinical presentation
The primary lesion of caries is a well-demarcated, chalky-white lesion (Fig. 32.2) in which the surface continuity of enamel has not been breached. This ‘white-spot’ lesion can heal or remineralize, and this stage of the disease is therefore reversible. However, as the lesion develops, the surface becomes roughened and cavitation occurs. If the lesion is not treated, the cavitation spreads into dentine and eventually may destroy the dental pulp, finally leading to the development of a periapical abscess and purulent infection (see Chapter 34).
Diagnosis
Diagnosis is usually by a combination of:
Aetiology
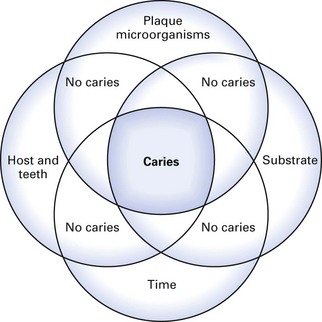
The major factors involved in the aetiology of caries (Fig. 32.3) are:
Diet
Microbiology
Microorganisms in the form of dental plaque are a prerequisite for the development of dental caries. The different types of plaque and the factors involved in their development are described in Chapter 31.
Specific and non-specific plaque hypothesis
There is conflicting opinion for and against the specific plaque hypothesis:
The role of mutans streptococci
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses