Chapter 34 Dentoalveolar infections
Source of microorganisms
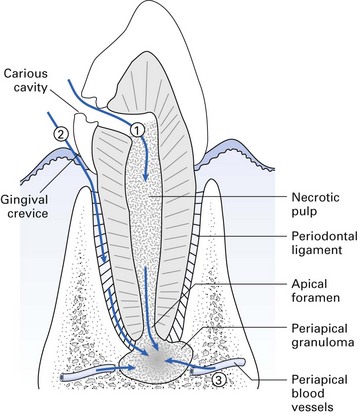
Endogenous oral commensals, usually from the apex of a necrotic tooth or from periodontal pockets as a result of either caries or periodontal disease (Fig. 34.1).
Dentoalveolar abscess
A dentoalveolar abscess usually develops by the extension of the initial carious lesion into dentine, and spread of bacteria to the pulp via the dentinal tubules (Figs 34.1 and 34.2). The pulp responds to infection either by rapid acute inflammation involving the whole pulp, which quickly becomes necrosed, or by development of a chronic localized abscess with most of the pulp remaining viable. Other ways in which microbes reach the pulp are:
Sequelae
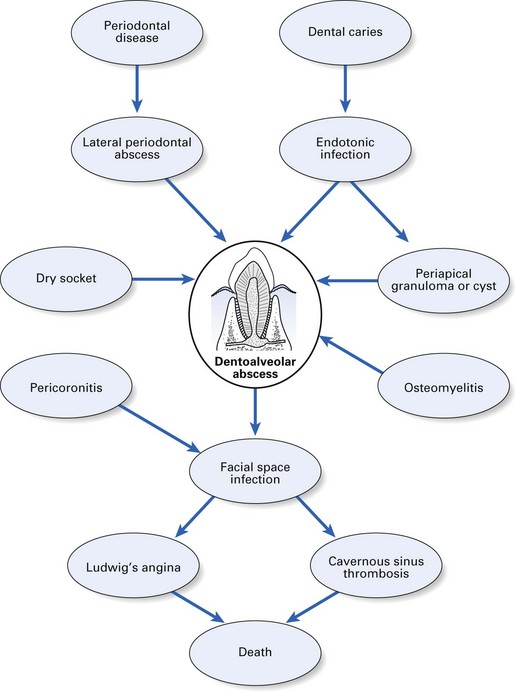
Once pus formation occurs, it may remain localized at the root apex and develop into either an acute or a chronic abscess, develop into a focal osteomyelitis, or spread into the surrounding tissues (Figs 34.2 and 34.3).
Direct spread
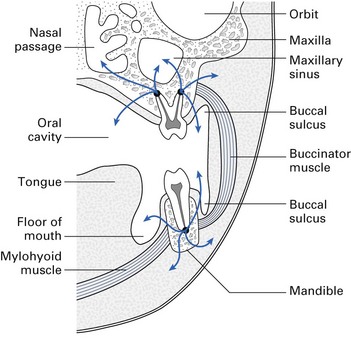
Table 34.1 Sites of contiguous spread of dentoalveolar infection (see also Fig. 34.3)
| Site of spread | Maxillary teeth | Mandibular teeth |
|---|---|---|
| Palate | Palatal roots of premolars and molars; also lateral incisors with a palatally curved root | – |
| Buccal space | Canines, premolars and molars | Canines, premolars and molars |
| Infraorbital/periorbital region | Canines mainly | – |
| Maxillary sinus | Canines, premolars and molars | – |
| Upper lip | Central and lateral incisors | – |
| Masseteric space, pterygomandibular space, lateral pharyngeal space | – | Lower third molars |
| Lower lip | – | Incisors and canines |
| Submandibular space | – | Root apices below insertion of mylohyoid – usually molars but can also be premolars |
| Submental space | – | Incisors and canines |
| Sublingual space | Root apices above mylohyoid/geniohyoid – usually incisors, canines and premolars; rarely molars |
Microbiology
Microbiologically, the dentoalveolar abscess is characterized by the following features:
The common species isolated from dentoalveolar abscesses are Prevotella, Porphyromonas and Fusobacterium spp., and anaerobic streptococci; facultative anaerobes are the second largest group, e.g. Streptococcus milleri (Table 34.2). There is evidence that some strictly anaerobic bacteria, especially Porphyromonas gingivalis and Fusobacterium spp., are more likely to cause severe infection than other species, and that synergistic microbial interactions play an important role in the severity of dentoalveolar abscesses.
Table 34.2 Bacteria commonly isolated from dentoalveolar abscesses
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses