Chapter 3
Patient Assessment and Treatment-Planning
Aim
The aim of this chapter is to discuss the importance of obtaining a thorough medical history and clinical patient assessment before embarking on tooth extraction and starting implant therapy. The techniques available to aid patient examination are covered briefly.
Outcome
After reading this chapter the reader should be familiar with the systematic approach used for obtaining a patient history and carrying out a clinical examination.
Introduction
A systematic approach to patient assessment is required. It is carried out in a very similar way to any assessment of a patient needing prosthodontic treatment. The mystique that sometimes surrounds implant therapy should be dispelled. It is worth noting, however, that implant therapy is an unforgiving discipline, and patient expectations are often high.
Clinical Assessment
The first part of the assessment is to define the patient’s requirements and expectations. Unrealistic expectations need to be identified and discussed. This is particularly important when significant hard and soft tissue has been lost and when the placement of multiple implants is critical to a successful aesthetic outcome.
Medical History
A full medical history is taken. In addition to the usual contraindications for surgery, it is important to pay particular attention to the following:
-
smoking
-
uncontrolled diabetes
-
facial pain
-
psychological problems.
Smoking
Although implants may be placed in patients that smoke, failure rates are considerably higher in smokers, with the probability that the failure rate increases with the extent of smoking. The risks need to be evaluated and carefully explained to the patient. Ideally he or she should be encouraged to stop smoking.
Diabetes
Implants can be placed in patients with diabetes if the condition is controlled. Uncontrolled diabetes should be stabilised before contemplating implant placement.
Facial Pain
The origin of any facial pain needs to be carefully diagnosed, with specialist help as appropriate. Particular care must be taken with patients suffering from “atypical facial pain”, as an implant may become a focus for this pain, leading to an intractable problem.
Psychological Problems
The suitability of patients with psychological disorders needs to be assessed most carefully before agreeing to proceed with treatment.
Dental History
A full dental history, including detailed extra- and intraoral examination, is essential. Special attention needs to be paid to progressive periodontal disease, active caries and destructive parafunctional activities.
If split roots, typically relating to post crowns, are present these tend to be associated with rapid bone loss and should be removed as a matter of urgency to preserve a possible implant site.
Clinical Examination
Extraoral
A full extraoral examination should be carried out, with particular attention being paid to the following:
-
temporomandibular joints (TMJ) and muscles of mastication
-
facial profile and lip support
-
smile line.
The TMJ and muscles of mastication are examined for anatomical abnormalities, signs of dysfunction and pathology.
The facial profile and lip support, with and without any existing denture, needs to be carefully evaluated and any atypical features noted.
The smile line relates to the level of the upper and lower lips in relation to the corresponding gingival margins. The smile line is of particular importance in cases in which gingival defects and long teeth are included in the smile. A high lip line may be demanding aesthetically.
Intraoral
A comprehensive intraoral examination must be completed, with special attention to a number of general and site specific features (Fig 3-1) as follows:
-
General:
-
primary disease
-
parafunction (Fig 3-2a)
-
prognosis of remaining teeth
-
occlusal support and control.
-
-
Specific to site:
-
space-interdental and interocclusal
-
ridge thickness and shape
-
nature, thickness and condition of the soft tissues
-
availability of bone, taking account of features such as concavities.
-
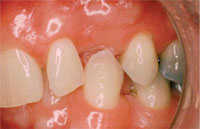
Fig 3-1 Lack of occlusal space.
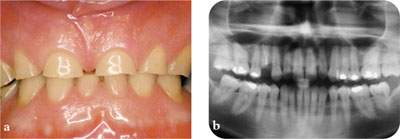
Fig 3-2 (a) Tooth wear caused by parafunctional activity. (b) Axial tomogram used for initial assessment.
Study Casts
It is invariably necessary to obtain articulated study casts to allow a well-considered treatment plan to be formulated.
Radiographic Examination
Radiographic examination is required to evaluate the quantity and, as best as possible, the quality of bone available for implant placement. It is also essential to identify and locate anatomical structures. The radiographs need to be accurate to allow for precise measurements to be made before implant placement. The structures of particular interest include:
-
Maxilla:
-
maxillary sinus
-
nasal floor
-
incisive canal
-
labial concavities.
-
-
Mandible:
-
inferior dental canal
-
mental foramen
-
lingual concavities.
-
The radiographic examinations need to balance accuracy and diagnostic value against the exposure to ionising radiation. The techniques available for radiographic examination include:
-
axial tomograms (DPT/OPG)
-
long-cone periapical radiographs
-
computed tomography (CT) scans
-
computer-guided technology
-
tomograms.
Axial Tomograms
Axial tomograms give an excellent overall view of the jaws and teeth and are usually the first radiograph taken as part of an implant assessment. The images are enlarged and, as a consequence, it />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


