Chapter 2
Case Selection
Aim
The aim of this chapter is to discuss the reasons for tooth loss and how this may influence the method of replacement. We will examine the need to replace missing teeth and outline the advantages and disadvantages of each method of tooth replacement.
Outcome
After reading this chapter the reader should have an understanding of how the aetiology of tooth loss influences treatment planning and the options available for tooth replacement.
Introduction
Dental implants may be considered the means of tooth replacement of choice in modern dentistry. It should not be forgotten, however, that there are other methods of tooth replacement that should be considered each time the patient asks for a tooth space to be filled.
Reasons for Tooth Loss
The reason for the loss of the teeth must be ascertained, as this can often influence treatment planning. The prognosis of the dentition as a whole, together with the prognosis for the teeth adjacent to the tooth space, must be determined. If further tooth loss is anticipated, then contingencies for subsequent tooth replacement must be built into any treatment plan. In cases in which the prognosis of the remaining dentition is poor a radical treatment plan may prove to be more beneficial to the patient in the long term. Depending on the nature of the dental disease and the ease of tooth extraction there will be a variable degree of soft and hard tissue loss once the teeth have been removed. With implants tissue loss should be minimal, but in severe cases of tissue loss a compromised result may occur unless some form of augmentation is considered.
The main reasons for tooth loss or missing teeth are as follows:
-
periodontal disease
-
dental caries
-
endodontic failure
-
trauma
-
hypodontia.
Periodontal Disease
If the patient has advanced progressive periodontal disease there should be concern for the prognosis of the whole dentition. The patient in Fig 2-1 displays features of an unstable dentition with a poor appearance. Conventional tooth and implant abutments may be equally at risk from future bone loss. Progression of periodontal disease leads to recession and loss of soft tissues. This results in lengthened clinical crowns and the appearance of “black triangles” interdentally. This will lead to a poor aesthetic outcome unless flanges are considered on bridgework or partial dentures. With dental implants some form of soft tissue or bone augmentation is typically required.
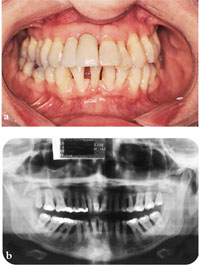
Fig 2-1 (a) An unstable periodontally compromised dentition with impending tooth loss. (b) Orthopantomogram showing severe irregular bone loss.
Dental Caries
Dental caries weakens tooth structure. Treatment of dental caries with plastic or cast restorations results in further loss of tooth structure. The restorative cycle of repair and replacement further weakens the tooth so that endodontic treatment may be required, followed by the need for auxiliary retention by means of pins or posts. The potential for early failure of heavily restored teeth makes treatment-planning uncertain.
Endodontic Failure
Endodontic treatment is generally successful. Success rates of 95% over 10 years have been published. However, limited coronal tooth structure is of greater concern. The lack of remaining tooth structure leaves the tooth weakened and sometimes necessitates a post and core to retain a crown. Not infrequently the endodontic treatment remains satisfactory, but further loss of tooth structure or root fracture leads to tooth loss (Fig 2-2). When endodontic failure occurs repeat treatments may suffer limitations, in particular if surgical endodontics are required on heavily restored teeth. It is useful to fully assess the expected prognosis of such teeth and to carry out a cost/benefit analysis of retreating them. Often it may be more appropriate to consider removal and replacement of the tooth rather than attempting a repair or replacement restoration.
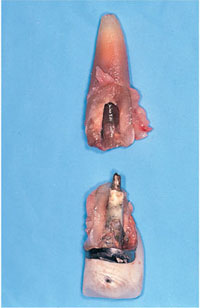
Fig 2-2 Vertical root fracture of a central incisor tooth restored with a post crown, necessitating extraction.
Trauma
Severe trauma may lead to hard and soft tissue loss. Teeth may be avulsed or fractured. It is often difficult to predict the prognosis of traumatised teeth. A significant proportion of such teeth lose their vitality perhaps five to 10 years after the initial trauma. This reduces their ability to perform as potential abutments for bridges or dentures. Traumatized teeth can be affected by internal and external resorption.
Hypodontia
Approximately 6% of the population are affected by hypodontia or congenital absence of teeth. This also includes patients with cleft lip and palate or other craniofacial anomalies. These patients often have microdontia and malocclusions. Where teeth are missing, the alveolar ridge is often narrow or wasted. This complicates orthodontic treatment and subsequent tooth replacement – for example, Fig 2-3 shows a partial denture for a patient with hypodont/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


