CHAPTER 25
Dentoalveolar Cleft Repair
Jeremiah Jason Parker1 and Christopher T. Vogel2
1Private Practice, Montgomery, Alabama, USA
2Department of Oral and Maxillofacial Surgery, University of Missouri–Kansas City, Kansas City, Missouri, USA
The reconstruction of congenital anterior maxillary alveolus and maxilla defects, and the closure of associated oronasal fistulae.
Indications
- To provide a stable osseous medium for the eruption and orthodontic movement of teeth within a region of a maxillary cleft
- Closure of oronasal fistulae
- Improvement of facial aesthetics by providing osseous support to the nasal base and continuity to the dentoalveolar arches
- To establish proper periodontal support for neighboring dentition
- To provide an osseous medium for the eventual placement of endosteal implants
- To provide a stable and intact maxillary arch for future orthognathic procedures
Contraindications
- Active infection
- Poor patient compliance concerning oral hygiene
- Collapsed cleft with plans for future orthodontic expansion. The palate is expanded in order to widen the cleft to the desired arch shape prior to grafting. The expanded cleft permits greater visualization and instrumentation of the cleft. Additionally, it is exceptionally difficult to orthodontically widen the cleft space once the graft has consolidated (refer to Key Point 1, this chapter)
Technique
- The patient is positioned supine and orally intubated with an oral RAE tube.
- The neck is hyperextended for better visualization of the palate and alveolar process. A throat pack is placed within the posterior oropharynx. The patient is prepped to include the oral cavity, the nasal passages, the surrounding maxillofacial skeleton, and, if present, the oronasal fistula. The patient is draped to allow for exposure of the oral cavity and nasal passages.
- Local anesthesia containing a vasoconstrictor is injected along the palate, nasal floor, maxillary vestibule, and attached and unattached tissue of the anterior maxilla or cleft. The local anesthesia needle is used as a probe and allows the operator to determine the extent of the cleft and the position of the bone prior to making an incision. In cases involving a complete bilateral cleft with a mobile anterior segment, injection of the anterior segment with a vasoconstrictor is contraindicated due to the tenuous blood supply to the segment.
- An incision is initiated along the lateral aspect of the cleft (Figure 25.1). A #15 blade is utilized to create a full-thickness mucoperiosteal incision along the lateral aspect of the cleft overlying sound bone. The anterior aspect of the incision extends to the height of the maxillary vestibule, and the posterior aspect of the incision extends along the posterior border of the cleft within the hard palate. The incision should divide the oral and nasal mucosa.
- The incision is extended laterally utilizing buccal and palatal intrasulcular incisions. The lateral extent of the incision extends to the distal aspect of the last molar and terminates with a buccal posterior and superior releasing incision (Figure 25.2).
- The medial incision extends in an intrasulcular fashion along the buccal and palatal surfaces of the teeth and terminates at the contralateral canine or first molar for unilateral clefts (Figure 25.2). The medial incision terminates at the midline for bilateral clefts.
- A subperiosteal dissection is utilized to expose the piriform aperture, the anterior nasal spine, and the floor of the nose. Supernumerary or malformed teeth are extracted at this time. Care is taken to avoid exposure of the crown of developing impacted canine teeth. If the crown of an impacted canine tooth is exposed during the cleft dissection, strong consideration for the extraction of the tooth should be made. Grafting procedures adjacent to the crown of an exposed tooth significantly decrease the overall success rate of the graft.
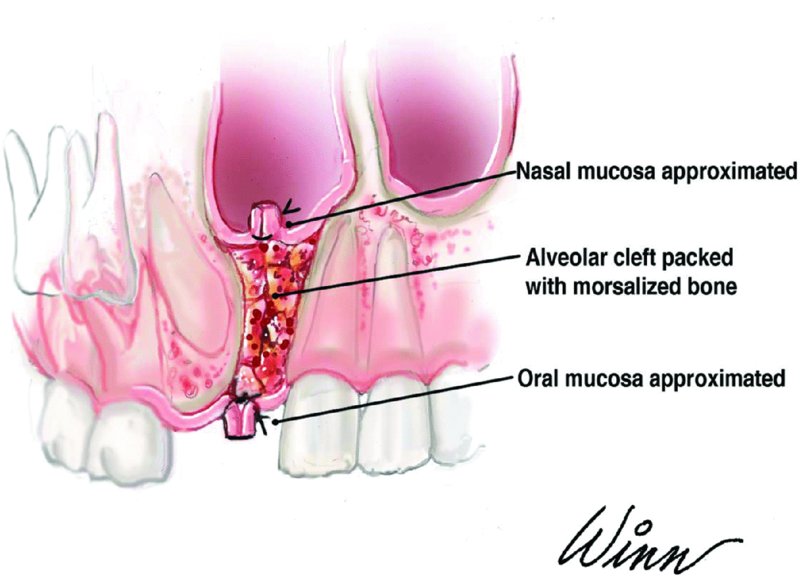
- In cases where a fistula is present, a subperiosteal, full-thickness tissue dissection is initiated along the internal aspect of the cleft and is extended superiorly along the lateral walls of the cleft to the floor of the nose and the cartilaginous nasal septum. The tissue reflected from the internal aspect of the cleft is carefully elevated, inverted, and sutured together to form a new nasal barrier. The tissue edges are sutured together using 5-0 Vicryl buried sutures in a horizontal mattress fashion, resulting in the tissue edges being inverted within the nasal cavity (Figure 25.3). A biological collagen membrane is trimmed and adapted to the nasal floor.
- Periosteal releasing incisions are made within the full-thickness mucoperiosteal tissue reflections, and the labial mucosa is advanced until the tissue can easily be approximated over the cleft defect without tension.
- Grafting material is placed within the cleft defect and compacted to eliminate dead space. The authors prefer to use either bone marrow from the anterior hip or a mixture of mineralized and demineralized human cadaveric bone depending on the size and nature of the cleft. The grafted area should extend from the nasal floor to the alveolar crest.
- A second biological collagen membrane is trimmed and adapted to contain the graft material within the cleft defect. The mucoperiosteal tissue elevations are closed over the grafted defect and membrane in a tension-free manner. Additional releasing incisions, subperiosteal dissection, and/or periosteal scoring is accomplished in order to obtain a tension-free primary closure (Figure 25.4).
- In the case of a bilateral cleft, the procedure described in Steps 1 through 12 would be performed on the largest cleft side first. The contralateral cleft is repaired in a similar fashion after a healing period of at least 6 months.
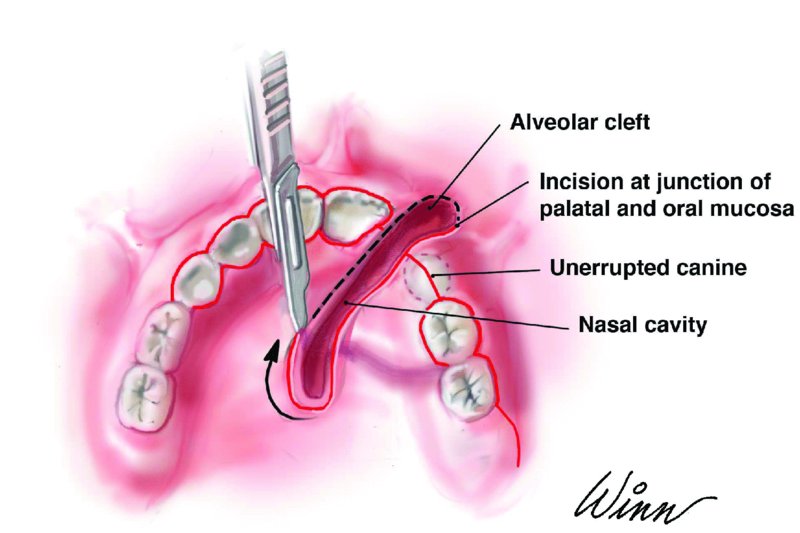
Figure 25.1. An incision is initiated along the lateral aspect of the cleft overlying sound bone within the keratinized tissue lateral to the cleft. The anterior aspect of the incision extends to the height of the maxillary vestibule, and the posterior aspect of the incision extends along the posterior border of the cleft within the hard palate.
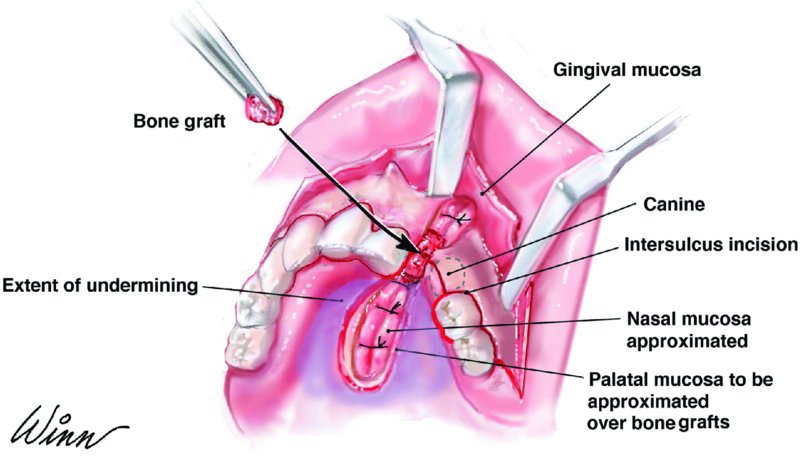
Figure 25.2. The incision extends medially to the canine and laterally to the tuberosity. The nasal mucosa is inverted and closed, and grafting material is placed within the cleft defect.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


