CHAPTER 25. Allergy and autoimmune disease
Many endocrine diseases are immunologically mediated and most of the immunologically-mediated diseases have some dental relevance (Box 25.1).
Box 25.1
Aspects of immunologically-mediated diseases affecting dental management
• Systemic effects affecting dental management
• Immunologically-mediated oral diseases
• Risks of abnormal reactions to drugs (e.g. penicillin anaphylaxis)
Immunologically-mediated diseases fall into two main groups (Box 25.2). By far the most common are atopic disease and contact dermatitis, which are abnormal reactions to exogenous antigens. The autoimmune diseases, by contrast, are mediated by antibodies directed against host tissues.
Box 25.2
Important immunologically-mediated diseases
Atopic disease and related allergies (reactions to exogenous antigens)
• Asthma; eczema; hay fever; urticaria; food allergies
• Some drug reactions
• Anaphylaxis and acute allergic angio-oedema
• Contact dermatitis
Autoimmune diseases (reactions to endogenous antigens causing autoantibody production)
Connective tissue diseases
Autoimmune diseases with specific autoantibodies
• Pernicious anaemia (chronic atrophic gastritis) *
• Idiopathic and drug-associated thrombocytopenic purpura*
• Drug-associated leucopenia*
• Autoimmune haemolytic anaemia
• Addison’s disease*
• Hypothyroidism (Hashimoto’s thyroiditis)
• Hyperthyroidism
• Idiopathic hypoparathyroidism*
• Pemphigus vulgaris*
• Mucous membrane pemphigoid*
ATOPIC DISEASE
Atopic disease is the common type of allergy and affects approximately 10% of the population. It is mediated by IgE and susceptibility is genetically determined.
There are no oral manifestations of atopic disease itself and there is no such entity as oral eczema. However, acute angio-oedema (sometimes a drug reaction) can indirectly involve the mouth by causing oedematous swelling of the floor of the mouth or lips as discussed below.
Acute severe asthma has a significant mortality and is a potential cause of an emergency in the dental surgery. Drugs (Box 25.3) used to treat it and other atopic diseases may complicate dental treatment.
Box 25.3
Effects of drugs used for atopic disease
• Antihistamines (for minor allergies)
–Drowsiness
–Potentiation of sedating drugs
–Dry mouth
• Corticosteroid inhalers
–Oropharyngeal thrush
• Systemic corticosteroids for severe asthma (see Box 31.10)
Contact dermatitis
Contact dermatitis resembles eczema clinically, but is a cell-mediated (type 4) reaction. There is no convincing evidence of any oral counterpart to contact dermatitis (Figs 25.1 and 25.2). Contact dermatitis of the hands to dental materials is a hazard to dentists and especially to laboratory technicians. Methyl methacrylate monomer, in particular, is a sensitising agent, but contact dermatitis to it is a surprisingly rare occupational hazard of dentistry.
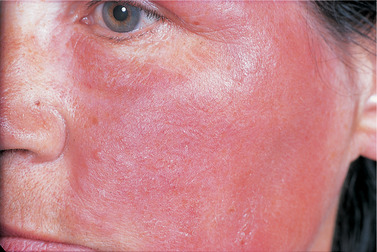 |
| Fig. 25.1
Allergic rash triggered by impression material. There is generalised facial erythema and slight oedema.
|
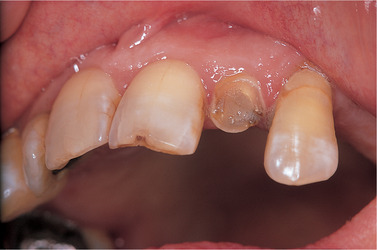 |
| Fig. 25.2
Hypersensitivity to impression material. The same patient as in Figure 25.1, showing the site of the impression photographed at the same time. No allergic response is evident intraorally.
|
Latex allergy
Latex allergy is the main allergic disease affecting healthcare workers.
The necessity for gloving for all clinical work has resulted in a growing frequency of latex allergy. In one dental school, the prevalence of latex allergy was 9%, while 22% complained of chronic glove dermatitis. Once latex allergy to gloves has been acquired, there are reactions to all rubber products such as rubber tubing, anaesthetic masks, catheters and tourniquets. Powdered latex gloves should no longer be used in the UK; the starch powder spread latex proteins into the environment. For those with latex allergy, gloves made from other plastics are required but, as yet, there is no completely satisfactory alternative. Despite this, some centres are phasing out latex gloves.
Patients exposed to latex through medical procedures are also at risk (Box 25.4).
Box 25.4
Individuals at risk of latex allergy
• Healthcare professionals
• Atopic patients
• Spina bifida
• Urogenital anomalies
• Latex industry workers
• Those subject to multiple surgical procedures before the age of 7 years
Latex allergy is important because it most frequently manifests as an urticarial contact reaction. In dentistry, this has the potential to put the airway at risk. More rarely, reactions to latex can be severe and have been fatal.
It is not always obvious that a medical or dental device may contain rubber, for instance bungs in local anaesthetic cartridges may contain latex. Even covered latex, such as a sphygmomanometer cuff, can shed latex proteins and trigger a reaction. For severe cases, it may be necessary to refer patients to a centre with a latex-free surgery. Less severe cases can be premedicated with methylpredisone and chlorpheniramine.
Allergy to mercury and other metals
The main sources of reactions are mercury in amalgam and nickel. Patients allergic to mercury are not prone to contact reactions in the oral mucosa which cannot mount contact dermatitis reactions. Amalgam restorations can safely be inserted, provided that no amalgam reaches the patient’s skin.
Mucosal reactions, such as lichenoid-type lesions, have been reported, but evidence is conflicting as to whether these are true allergic reactions.
Fragments of amalgam lost in the submucosal tissues frequently do not cause any reaction histologically.
Nickel allergy is a less common source of allergic reactions. It may be present in bridges and crowns. Even in patients allergic to nickel, a nickel-containing appliance may cause no reaction in the mouth, but may affect the skin.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


