CHAPTER 11. Disorders of the temporomandibular joints and periarticular tissues
Temporomandibular joint (TMJ) disorders can cause various combinations of limitation of movement of the jaw, pain, locking or clicking sounds. Pain, in particular, is a frequent cause of limitation of movement. These complaints are rarely due to organic disease of the joint and many are due to trauma. However, these functional disorders must be considered in the differential diagnosis. Important causes of limitation of mandibular movement are summarised in Boxes 11.1 and 11.2.
Box 11.1
Causes of limitation of mandibular movement
Intracapsular causes*
• Infective arthritis
• Juvenile arthritis
• Traumatic arthritis and disk damage
• Intracapsular condylar fracture
Pericapsular causes*
• Irradiation and other causes of fibrosis
• Dislocation
• Condylar neck fracture
• Infection and inflammation in adjacent tissues
Muscular
• TMJ dysfunction syndrome
• Myalgia caused by bruxism
• Haematoma from ID block
• Tetanus
Other
• Oral submucous fibrosis
• Systemic sclerosis
• Zygomatic and maxillary fractures
• Drugs
Box 11.2
Important causes of intracapsular ankylosis (‘true ankylosis’)
Trauma
• Intracapsular comminuted fracture of the condyle disorganises the joint. Bleeding may be followed by organisation and bone formation. Early mobilisation of such injuries should prevent bony ankylosis
• Penetrating wounds
• Forceps delivery at birth
Infection
• Otitis media/mastoiditis
• Osteomyelitis of the jaws
• Haematogenous – pyogenic arthritis
Arthritides
• Systemic juvenile arthritis
• Psoriatic arthropathy
• Osteoarthritis (rarely)
• Rheumatoid arthritis (rarely)
Neoplasms
• Chondroma
• Osteochondroma
• Osteoma
Miscellaneous
• Synovial chondromatosis
Trismus may be defined as inability to open the mouth due to muscle spasm, but the term is usually used for limited movement of the jaw from any cause and usually refers to temporary limitation of movement. The term ankylosis usually refers to persistent limitation of movement and can be either bony or fibrous. However, the term trismus is sometimes loosely used to mean ankylosis. Inability to open the mouth fully is usually temporary and causes are summarised below.
TEMPORARY LIMITATION OF MOVEMENT (TRISMUS)
Infection and inflammation in or near the joint
The main cause is acute pericoronitis with associated muscle spasm. Mumps can also cause transient and unnoticed limitation of movement. Rare causes include suppurative arthritis, osteomyelitis, cellulitis and suppurative parotitis. Submasseteric abscess results in profound trismus and infection in the pterygoid, lateral pharyngeal or submandibular spaces may also cause varying degrees of trismus.
Mandibular block injections may cause inflammation of the muscles around the joint and oedema, either because of irritation by the local anaesthetic or by introduction of infection, but rarely do so.
Injuries
Unilateral condylar neck fracture usually produces only mild limitation of opening with deviation of the jaw to the affected side, but closing into intercuspal occlusion may be difficult. Bilateral displaced condylar fractures cause an anterior open bite with limited movement. Rarely, a fall on the chin can result in unilateral or bilateral dislocation of the condylar head into the middle cranial fossa and severe restriction of all movements. Less severe injuries frequently result in an effusion into the temporomandibular joint; both wide opening and complete closure are then obstructed.
Any unstable mandibular fracture causes protective muscle spasm and limitation of movement. Patients suffering from displaced Le Fort II or III fractures often complain of limited opening whereas, in reality, they are fully open with the jaws wedged apart by the displaced middle third. Reduction of the fracture allows closure.
Tetanus and tetany
These are rare causes of masticatory muscle spasm. Trismus (lockjaw) is a classical early sign of tetanus which, though rare, must be excluded because of its high mortality. This possibility should be considered whenever a patient develops acute severe limitation of movement of the jaw without local cause, but has had a penetrating wound, even if small, elsewhere.
Tetany is most likely to be seen as a result of anxiety and hyperventilation syndrome.
Temporomandibular pain dysfunction syndrome
Pain dysfunction syndrome is one of the most common causes of temporary limitation of movement of the temporomandibular joint, as discussed later.
Hysterical trismus
Inability to open the mouth is occasionally the main symptom in disturbed patients.
Drugs
Phenothiazine neuroleptics can cause tardive dyskinesia with uncontrollable, involuntary grimacing or chewing movements. Tardive dyskinesia is typically a result of long-term treatment: unlike drug-related Parkinsonism, there is little response to treatment. Metoclopramide, which has phenothiazine-like properties, can cause limitation of movement of the jaw.
Management
In all these conditions the essential measure is to relieve the underlying cause.
DISLOCATION
The temporomandibular joint may become fixed in the open position by anterior dislocation; this is due to forcible opening of the mouth by a blow on the jaw, or during dental extractions under general anaesthesia. In the latter case, the condition should be noticed immediately. It must be corrected before the patient recovers consciousness, by pressing downwards and backwards on the lower posterior teeth. Occasionally, a patient will dislocate spontaneously while yawning. Epileptic patients sometimes also dislocate during fits.
Occasionally, the dislocation remains unnoticed and, surprisingly, a patient may tolerate the disability and discomfort for weeks or even months (Fig. 11.1, Fig. 11.2 and Fig. 11.3). In these cases, effusion into the joint, following injury, becomes organised to form fibrous adhesions. When this happens, manual reduction may be impossible and open reduction, with division of adhesions, must be carried out.
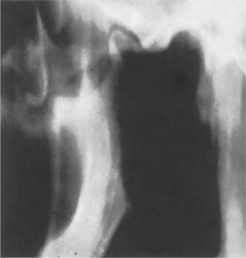 |
| Fig. 11.1 |
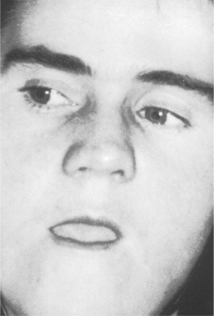 |
| Fig. 11.2
Longstanding dislocation of the jaw: the teeth had been extracted about a month previously; in spite of the patient’s inability to close her mouth and the distorted appearance, the dislocation remained unrecognised.
|
 |
| Fig. 11.3
Reduction of the dislocation (performed by open operation because of development of fibrous adhesions) restores the patient’s normal appearance and movements of the jaw.
|
Recurrent dislocation
Recurrent dislocation of the temporomandibular joint is more common and is typically seen in adolescent girls and young adults. It is a typical feature of floppy joint syndromes, notably Ehlers–Danlos and Marfan’s syndromes, or there may be no underlying systemic disorder.
Augmentation of the eminence by bone graft or down-fractureof the eminence are overall the most successful procedures.
Ehlers–Danlos syndrome
Ehlers–Danlos syndrome (see Ch. 2) is a heritable disease of collagen formation causing, among other features, hyper-extensibility of the skin, easy bruising and loose jointedness. Ten subtypes are recognised. Mitral valve prolapse is associated in types I and II in particular.
A very small minority of patients with pain dysfunction syndrome appear to have Ehlers–Danlos syndrome. In addition to the risk of TMJ dislocation, other features as discussed earlier are summarised in Box 11.3.
Box 11.3
Ehlers–Danlos syndrome: important features
• Hypermobility of joints (in types I, VI and VII especially)
• Risk of TMJ subluxation
• Bleeding tendencies and purpura especially in type IV
• Mitral valve prolapse and risk of infective endocarditis in types I and II
• Severe early-onset periodontitis in type VII
• Often, teeth with short or distorted roots and pulp stones
PERSISTENT LIMITATION OF MOVEMENT
Management of ankylosis depends on its aetiology and can be classified for surgical purposes as shown in Box 11.4.
Box 11.4
Management of ankylosis
Mechanical interference with opening (‘pseudoankylosis’). Causes include:
• Trauma: depressed fracture of the zygomatic bone or arch
• Hyperplasia: developmental overgrowth of the coronoid process
• Neoplasms: osteochondroma, osteoma, osteosarcoma of the coronoid process
• Miscellaneous: myositis ossificans, congenital anomalies
Extracapsular ankylosis (‘false ankylosis’). Causes include:
• Trauma: periarticular fibrosis (wounds/burns). Posterior or superior dislocation. Longstanding anterior dislocation
• Infection: chronic periarticular suppuration
• Neoplasia: fibrosarcoma of the capsule. Chondroma or chondrosarcoma
• Periarticular fibrosis
Irradiation
Oral submucous fibrosis
Progressive systemic sclerosis
Irradiation
The penetrating power of modern sources, such as cobalt 60 or linear accelerators, is such that high doses can damage deep tissues without a superficial burn. Radiation involving the region of the masticatory muscles, for the treatment of a maxillary tumour for instance, often leads to fibrosis of muscle and adhesions to the surrounding fascial layers, causing fibrous ankylosis.
Treatment is difficult and may involve division of muscle attachments from the jaw or section of the angle or body of the mandible to produce a false joint. Bone surgery is complicated by the risk of osteoradionecrosis and infection (see Ch. 6).
Oral submucous fibrosis
Oral submucous fibrosis is an important condition that causes not only limitation of opening, but is also premalignant. Symmetrical fibrosis of such sites as the buccal mucosa, soft palate and the pillars of the fauces renders the mucosa immobile and prevents opening. Fibrosis extends deeply into muscles of mastication and is progressive. Ultimately, opening the mouth may become so limited that eating and dental treatment become increasingly difficult and tube feeding may become necessary. There is no effective treatment. This condition is considered in detail in Chapter 16.
Progressive systemic sclerosis (scleroderma)
Systemic sclerosis is an uncommon connective tissue disease characterised by widespread subcutaneous and submucous fibrosis. Though the most obvious feature is the progressive stiffening of the skin, the gastrointestinal tract, lungs, heart and kidneys can also be affected.
Systemic sclerosis is a connective tissue (collagen vascular) disease associated with a variety of autoantibodies (see Ch. 25).
Clinically, women between the ages of 30 and 50 are predominantly affected. Raynaud’s phenomenon is the most common early manifestation, often associated with arthralgia. A hallmark of the disease is involvement of the hands causing such changes as atrophy of or ischaemic damage to the tips of the fingers and contractures preventing straightening of the fingers (see Fig. 1.3).
The skin becomes thinned, stiff, tethered, pigmented and marked by telangiectases. The head and neck region is involved in over 75% and, in a minority, symptoms start there. Narrowing of the eyes and taut, mask-like limitation of movement (Mona Lisa face) can give rise to a characteristic appearance. The lips may be constricted (fish mouth) or become pursed with radiating furrows. Occasionally, involvement of the periarticular tissues of the temporomandibular joint together with the microstomia may greatly limit opening of the mouth, but this is typically much less frequent and severe than in the case of oral submucous fibrosis. Involvement of the oral submucosa may cause the tongue/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


