Dental Care for the Child and Adolescent with Disabilities
Gunilla Klingberg, June Nunn, Johanna Norderyd, and Pernille Endrup Jacobsen
Context
Disability is a term that evokes different images for readers, depending on their cultural background, their personal experiences of disabling conditions, and the norms of the society in which they live. In recent years there has been a move away from the fairly narrow definition imposed by the medical model, with its emphasis on an individual’s impairment “handicapping” that person. For example, a child with Down syndrome is disabled by being intellectually impaired and unable to keep up educationally with his or her peers. Advocates for people with disabilities, including parent support organizations, have promoted a more inclusive definition that places an emphasis on an individual’s ability, rather than what they cannot do. This is in part captured in the social model, in which it is acknowledged that it is society that disables an individual with an impairment, rather than the other way round. For example, a flight of stairs into a dental surgery disables a person who has quadriplegic cerebral palsy and so needs to use a wheelchair to move around.
The World Health Organization’s International Classification of Functioning Disability and Health (ICF) [1] and the children and youth version (ICF‐CY) [2] seek to stress the health status and functioning of the individual, rather than their potential disability. These classifications are based on a biopsychosocial model that aims to integrate the medical and social models referred to above. Functioning and disability are defined in relation to the outcomes between the health condition(s) of the person and the context in which he or she operates. This context is defined at three levels of functioning: at the level of a body part, at the level of the whole individual, and lastly, functioning that occurs at the level of society (Figure 24.1).
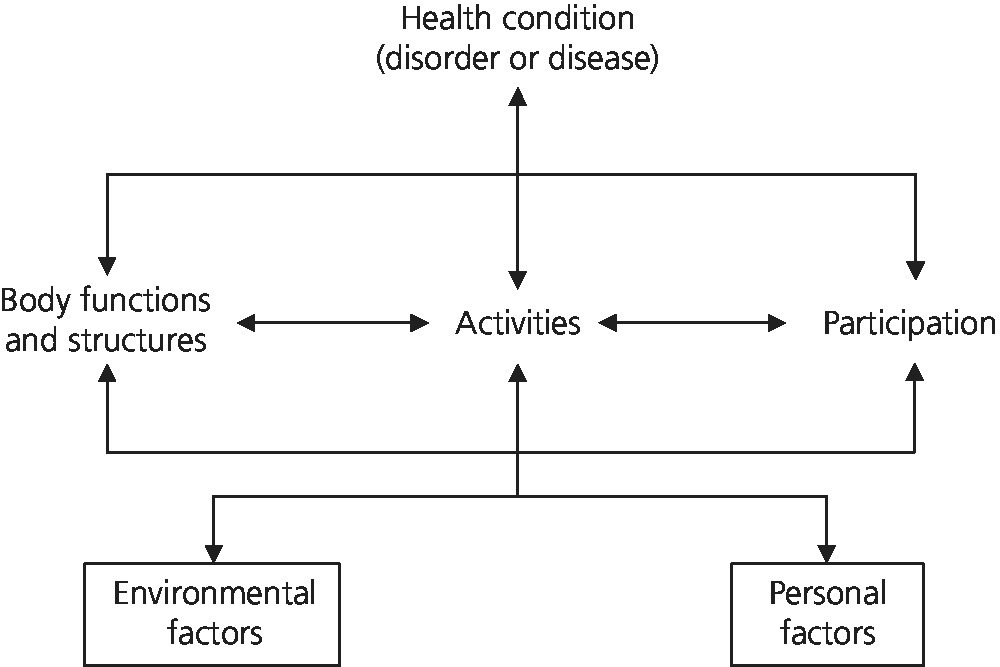
Figure 24.1 The ICF theoretical, biopsychosocial model defines functioning and disabilities in relation to outcomes between the health conditions of a person and the context in which they operate. This context is defined at three levels of functioning, at the level of a body part, at the level of the whole individual, and the functioning that occurs at the level of society.
Clearly, this framework opens up the possibility of refining the definitions of, for example, which children it is considered need special care dentistry and which do not, judged by the functioning needs of the child rather than a mere diagnosis. Examples of this are given in Table 24.1 [3]. In both these examples, the need for specialist facilities such as expert knowledge about different conditions, conscious sedation, or wheelchair‐accessible dental surgeries may mean that special dental care is required.
Table 24.1 ICF structure and domains applied on example patients: a child with Autism spectrum disorder and a child with quadriplegic cerebral palsy and epilepsy.
Source: Faulks & Hennequin 2006 [3]. Reproduced with permission of Stephen Hancocks Limited.
| Domain (examples) | Example 1: child with Autism spectrum disorder | Example 2: child with quadriplegic cerebral palsy and epilepsy |
| Body function (physiological and psychological functions of body systems) | Global mental functions (e.g., global psychosocial functions) Specific mental functions (e.g., emotional functions) | Control of voluntary movement functions Involuntary movement functions |
| Body structures (anatomical parts of the body) | Structure of the brain | Structure of upper extremity Structure of lower extremity |
| Impairments (significant deviation or loss of body function or structure) | Impaired ability to sustain attention Impaired control of voluntary movements | Impaired involuntary movement reaction functions (e.g., posture) |
| Delayed acquisition of the mental functions of language | Impaired control of voluntary movements and functions | |
| Impaired psychosocial functions | Impaired involuntary movement functions (e.g., involuntary muscle contraction) | |
| Activity (the execution of a task or action) | Undertaking single or multiple tasks Handling stress and other psychological demands | Undertaking single or multiple tasks |
| Participation (involvement in a life situation) | Maintaining one’s health | Maintaining one’s health |
| Activity limitations (difficulty in executing activities) | Difficulty in completing a given task, e.g., simple dental instruction | Difficulty in washing oneself Difficulty in caring for teeth |
| Participation restrictions (problems in involvement in life situations) | Problems with seeking care and accepting dental treatment | Problems with cooperating with dental treatment due to movement disorder |
| Environmental factors (physical, social, and attitudinal environment) | Support given by health professionals Attitudes of health professionals, health services |
Support given by health professionals Attitudes of health professionals, health services |
| Environmental facilitators | Well‐informed and understanding dental team | Well‐informed and understanding dental team |
| Appropriate adaptation of dental services (e.g., assimilation of patient’s routine) | Appropriate adaptation of dental services (e.g., wheelchair access, nonflickering lighting) | |
| Additional services (e.g., use of conscious sedation) | Additional services (e.g., use of conscious sedation) |
The ICF and the ICF‐CY complement the World Health Organization’s (1993) ICD‐10 codes [4], which is an international statistical classification of diseases and health‐related problems. The latter system will identify people with an intellectual disability, for example, and divide them into four categories of intellectual functioning based on intelligence quotient (IQ), with people with an IQ <70 classified as having intellectual disability and those with an IQ <50 having severe intellectual disability.
Prevalence
For the reasons outlined in the preceding section, the definitions of impairments may vary so that determining accurate prevalence figures for some disabling conditions can be difficult. In a review of disability in children conducted in 2004, the prevalence of all disabilities in children varied between 5.8% in the USA and 9.8% in Finland [5]. One finding from most prevalence studies is that there are more boys than girls affected, with respiratory disorders (e.g., asthma) being the most frequently occurring impairment. In the USA, children living in poverty or whose parents had little formal education were at greater risk of disability [6]. Adolescents with disabilities were three times more likely to visit a doctor each year and nine times more likely to have hospital visits annually compared with their nondisabled peers.
As in some other countries, Denmark has a birth cohort of children that are being followed longitudinally. Of the 9125 children born prematurely, some 673 did not survive beyond the first 28 days of life [7]. Many of these babies will have had impairments that were not compatible with life. Of the survivors, 11.2% were diagnosed with a disability. In Sweden, a survey of 10‐year‐old children concluded that 26% had health problems that significantly impacted on the child’s day‐to‐day functioning [8]. Physical disorders were the most frequent, occurring in 11.7% of the sample of children. In the UK there are approximately 0.8 million children living with a disability [9]. Some families care for two or more children with severe disability. Such families are more likely to be single parents, less likely to be in paid employment but, if they are, for them to be in semi‐skilled or unskilled jobs. They are thus families who are reliant on state aid and less likely to own their own homes. A hidden group of children are those who, because of chronic physical or mental illness, may be in health care settings for prolonged periods and thus not accessible to, or looked after by, dental services. In one study in England over a year, children aged between birth and 19 years occupied two million “bed days” because of their complex needs [10].
Survival from life‐threatening illnesses is increasing among children and adolescents; those with, for example, cystic fibrosis have improved their median survival from 14 years in 1969 to 32 years in 2000. The median life expectancy of a baby with cystic fibrosis now is approximately 40 years.
Oral health and disability
Impairments tend to occur more commonly in boys, in those from low‐income families, and in school‐age children. Their health needs, including oral and dental needs, are frequently unmet. Oral and dental diseases may be more prevalent in children and adolescents with impairments because of the potential for increased risk. Some countries have undertaken national surveys of children with disabilities, others have taken samples of children with different types of impairments and compared the data collected with those from a nondisabled population. No data exist on the outcome from implementation of policy arising out of the survey findings.
Most of these national or local studies report similar findings; while the numbers of children with impairments who are caries‐free may be higher than for non‐impaired children, the management of dental disease is different. Children with impairments are more likely to have untreated dental caries and, where it is managed, this has in the past been by extraction rather than restoration. However, as dental care is developing with improvements in both oral health and management/treatment techniques there is a chance that these differences will diminish. Preventive dental services vary in different countries. In some places prevention is provided and well organized while in others it is only accessible for a minority of patients.
Despite overt needs, there is a lack of awareness among medical professionals of the oral and dental needs of their child patients with impairments, and dentists express an unwillingness to treat because of uncertainty, as well as a lack of competence to manage such groups in the population. Families often experience severe financial hardship in obtaining necessary dental care for their children, although in Scandinavian countries comprehensive dental care is free from birth to 18 or 19 years.
Children with impairments are more likely to use publicly funded services and increasingly to access those services that can provide care under sedation or general anesthesia. In those countries where people with impairments are still in residential care in large units, there are reports of poorer oral hygiene and worse dental health.
There are risk factors that are more prevalent in children with impairments, compared with the rest of the child population. Many more children with impairments will be taking sweetened liquid oral medicines over the long term with consequences for poor dental health including dental caries and possibly erosion. The prevalence of another form of tooth wear, bruxism, is more frequently seen in children with disabilities. Periodontal health is often poorer in children who are impaired because of underlying host factors, as in Down syndrome, as well as poor manual dexterity and no or inefficient plaque removal.
However, it is aspects of oral health and function, as depicted in the earlier discussion of the World Health Organization’s ICF classification, that often concern parents and carers, namely drooling, grinding, and feeding problems, not necessarily dental caries and periodontal diseases. This should be acknowledged. However, it is important that dentists also pay attention to the dental and gingival health in these patients and encourage the parents and family to be committed to the prevention of these diseases. If not, there is a risk that, for example, dental caries is overlooked.
Consent
As for any child, parents or legal guardians are the only people entitled to give consent for dental care. In some countries this will be until the age of 16 years, in others, 18 years. In a number of countries, adolescents, if they are judged to have the maturity to give their consent, or indeed to withhold their agreement for a dental procedure, will be able to make that decision without the need for parents to give their consent. However, many young people who have a communication disorder and especially those with a learning disability may never develop the capacity to give consent, verbal or written, for dental procedures. It will be for the members of the dental team to decide if the person has the capacity to consent and, if not, to work with the legislation in their country to manage issues of consent for the adolescent near or above the usual age of consent. Capacity will vary from day to day and will depend on the nature of the procedure. Regardless of this, the patient should always receive individually tailored information about treatment and be given the opportunity to give or refuse their consent.
Neuropsychiatric disorders
Neuropsychiatric disorders constitute a substantial group of diagnoses, for example, autism spectrum disorder and attention deficit hyperactivity disorder (ADHD). It has been estimated that at least 5% of the child population may have a neuropsychiatric disorder. The diagnoses are based on a specific set of symptoms describing the main domains of problems experienced by the individual person. A person’s diagnosis may change over time, as problems and symptoms change with individual development [11].
Autism spectrum disorder
An estimated prevalence for autism spectrum disorder (ASD) has been suggested as 6 per 1000 people [12]. In the 2013 fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM‐5) [13] autism spectrum disorder replaced a number of diagnoses, for example, autism and Asperger syndrome. ASD is a behavioral expression of neurobiological dysfunction. The prevalence varies, but is approximately one to three per 1000, and some increase in prevalence has been noted since the 1990s. This is probably due to more knowledge about the diagnoses leading to higher ascertainment rates. More boys than girls are affected [11]. According to DSM‐5, four criteria need to be met in order to be diagnosed with ASD:
- persistent deficits in social communication and social interaction across context, not accounted for by general developmental delays
- restricted, repetitive patterns of behavior, interests, or activities
- symptoms must be present in early childhood (but may not become fully manifest until social demands exceed limited capacities)
- symptoms together limit and impair everyday functioning.
Additional problems that may affect some individuals include hyperactivity, sleeping problems, and abnormal and strong reactions to perception (hearing, sight, physical contact). Up to 50% of people diagnosed with ASD never achieve spoken language. They also have problems with social interaction and communication including difficulties in using and understanding eye contact, facial expressions, and gestures, as well as in understanding, especially language’s deeper meaning. Children and adolescents with ASD are often engaged in a restricted range of behaviors, interests, and activities; repetitive and stereotypic behaviors are common. Comorbidity, that is having one or more diagnoses in addition to the main diagnosis, in this case autism, is frequently seen. In particular, there is an increased risk of epilepsy. ASD occur more frequently in individuals with, for example, some syndromes and in persons with intellectual disability. It is important to recognize that ASD has a very wide range in phenotype, i.e., there are large variations between individuals.
The former Asperger syndrome represents a high functioning autism spectrum disorder with a prevalence of three to five per 1000 people, and affects boys more often than girls; the disorder can range from mild to severe. People with this type of ASD usually have a normal or above normal IQ and many exhibit exceptional skills or talents in specific areas. At the same time, they have significant deficiencies regarding social skills and can be preoccupied with their special interests. Although having a rich vocabulary, the patient may sound like a “little professor” and the language development may appear normal on the surface, but there are often deficits in pragmatics and prosody.
ASD is a lifelong disability but many children can develop considerably provided early and individually tailored educational input is provided. It is important to help the child with tools for communication and in the structured training for daily living; different pedagogic concepts have developed. It is important to provide good information and education to parents and family and to establish a trusting relationship between the family and the educational system. Depending on the individual’s deficits, the need for assistance varies considerably between people with autism spectrum disorders. Some may be in need of assistance full time, while others only require help in organizing their studies or for some special activities.
Oral health considerations
As many patients with ASD are dependent on others for their daily life, risk factors may be different compared with nonaffected children. Provided there is no other underlying medical condition, the literature reports no differences in caries prevalence. This is probably due to family or caregivers being able to provide a good diet for the child, with a low intake of cariogenic items. On the other hand, there are reports of a higher prevalence of plaque and gingivitis compared with healthy children. Again the reason may relate to family/caregivers’ influence as many children and adolescents are dependent on help from others to carry out oral hygiene procedures and brushing the teeth of, for example, a teenager with ASD is often difficult.
Special considerations for dental care
People with ASD need help to understand and focus on dental treatment. Often several appointments are required just for an introduction to dentistry. It is important for the patient to meet the same dentist and preferably the same assistant or dental hygienist in order to get to know the personnel and be able to trust them. If the dental team knows beforehand that a patient has ASD it is advisable to contact the family by phone in advance. It is useful to get as much information about the patient as possible from this telephone interview: focusing on her or his strengths, what the child likes, what rewards are appropriate, does the child speak and, if not, the best way to communicate, does the child have fears of particular things like noise or strong light, etc. Often, people with ASD are overly sensitive to sounds, tastes, smells, and sights. Sometimes it is good for the parents or carers to visit the clinic beforehand without the child in order to get to know the facilities, where to park, what door to enter, who to meet, and so on.
The introduction to examination or treatment can be carried out over a number of appointments scheduled just one or a few days apart, or as several short, clearly constructed appointments sequentially on the same day. It is usually possible to carry out a good examination with mirror and probe and to perform preventive items such as toothbrushing, polishing, and applying topical fluorides, after this kind of special introduction to dental care. However, exposing radiographs or carrying out treatment such as fillings often requires sedation or general anesthesia. To reduce the need for general anesthesia, it is very important to emphasize prevention of oral/dental disease. The preventive care may be carried out by a dental hygienist or a trained dental nurse, but regular appointments with short intervals in between, in order to maintain contact and ensure a successful experience for the child, are vital.
Many children and adolescents with ASD use pictures or photographs as an aid in communication. Today, modern techniques with digital cameras and high‐quality printers have made it easy for the dentist to create this kind of individually customized help. Photos of the dental clinic and the dentist and staff the patient will meet should be included. Also, photos of an open mouth symbolizing “open your mouth,” a toothbrush, equipment for polishing, mirror, operatory lamp, and dental chair are useful (Figure 24.2). The pictures or photographs can be put in the sequence the patient will see them at the appointment in a photo album. This can be used both at home when preparing for the visit, and during the appointment as a help to remember and understand what is going to happen. This kind of aid is useful also when treating other patients, such as patients with ADHD, intellectual disability, children with another language, or even young or anxious children [14,15].

Figure 24.2 Examples of photographs that can be used as pedagogic tools in patients with neuropsychiatric disorders. Based on individual needs: pictures showing the entrance, the dental chair, the operatory light, a toothbrush, a mirror and an open mouth (symbolizing “open your mouth”) were chosen in this case. The photos can be put in sequence in a photo album.
Communication with a patient with autism should be very clear and objective as he or she understands you literally and will have a great deal of difficulty reading nonverbal cues (body language). Tell the patient what you want and avoid “small talk.” This will help the patient to focus on the dental treatment. See further under section “Attention deficit hyperactivity disorder.”.
Attention deficit hyperactivity disorder
Attention deficit hyperactivity disorder (ADHD) is a common disorder affecting 3–7% of children and adolescents and thus something that all dental health care personnel working with young patients are likely to meet. Knowledge about the condition is therefore important. ADHD is caused by neurobiological dysfunction. There is evidence of a genetic background affecting the frontal lobe and dopamine and norepinephrine neurotransmitters, although the etiology is not fully understood. The main problems in ADHD are displayed as inattention, hyperactivity, and impulsivity. The diagnosis can be either of a combined type (most common) where the individual exhibits symptoms in all domains, or inattentive, or hyperactive–impulsive type, depending on the main grouping of impairments. The prevalence varies considerably between different studies, mainly due to differences in definitions applied, but also due to differences in ascertaining study populations. Boys are diagnosed more often than girls, who are supposed to be underdiagnosed. The reason for this is likely to be that girls present with fewer observable impairments such as hyperactivity. Many of the problems in ADHD are persistent as the individual grows older, and many of the patients have difficulties as adults. These include higher frequencies of alcohol or drug abuse and psychiatric disorders.
Therapy for ADHD includes the use of psychoeducative strategies with educational programs for parents and teachers. Medication, mainly with methylphenidate (inhibiting dopamine and noradrenaline transport) or atomoxetine (increasing noradrenaline levels in the brain), has been shown to be effective in many children.
Oral health considerations
It is likely that children with attention disorders of various types have difficulties adjusting their activity level to situational demands and have more problems complying with dental care. There are reports of more behavioral management problems during dental care in patients with ADHD, and probably a risk of more dental anxiety. Many patients with ADHD behave and function at a lower age level in the dental setting. With respect to oral health, dental caries studies have reported somewhat contradictory results but, on balance, there would appear to be an increased risk. Children with ADHD have also been reported to have poorer oral health behavior in terms of higher frequency of sugary food and beverage intakes and a lower frequency of toothbrushing [16]. Furthermore, side effects of the medication for ADHD include risk of xerostomia, altered or decreased feelings of hunger, and nausea/vomiting, which increase the risk of oral health problems.
Special considerations for dental care
Prevention of oral health problems should be the main target together with promoting a positive attitude and acceptance of dental care. Many patients with ADHD have problems in concentrating and focusing on the dental treatment. In order to help the patients, disturbing visual and auditory noise should be reduced. For example, there should be no radio on, the door to the treatment room should be closed to reduce disturbance, and visual distractions such as toys or books should be kept to a minimum in the room. Communication should focus on clear information to the child about what will happen during treatment, who will be involved, how long the procedure will last, and what to do afterwards. Direct and objective guidance during the treatment can help the patient to focus; for example, directions like “Sit in the chair” rather than “Would you like to sit in the chair?” [16]. As for many other children with neuropsychiatric disorders, pictures or photos can be used as pedagogic tools to provide a “travel plan” of the appointment. Pictures can also be used as tools and aids for toothbrushing at home. Praising is essential as in all dental care for children, and should come directly when the child is cooperating instead of summing up at the end of the appointment.
Tourette syndrome
Tourette syndrome is defined by multiple involuntary motor and vocal tics, present for more than a year. The prevalence is approximately 1% and boys are affected three to four times more often than girls. The motor tics may be complicated, involving the entire body, such as kicking and stamping. The verbal tics include making sounds like grunting, throat clearing, shouting and barking, and may also be expressed as coprolalia (involuntary use of obscene words or sentences). Associated conditions can include ADHD, anxiety, and obsessive compulsive disorder. Therapy includes, apart from psychoeducative strategies, cognitive behavior therapy and in the case of obsessive compulsive disorder, medication often with selective serotonin reuptake inhibitors.
Oral health considerations
Children and adolescents with Tourette syndrome have more difficulties complying with dental care. This probably leads to an increased risk of both dental behavior management problems and also in the long term, dental anxiety. The oral health considerations are similar to those of patients with ADHD.
Special considerations for dental care
See under section “Attention deficit hyperactivity disorder.”
Other disorders
Intellectual disability
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


