Chapter 23 Infections of the respiratory tract
Normal flora
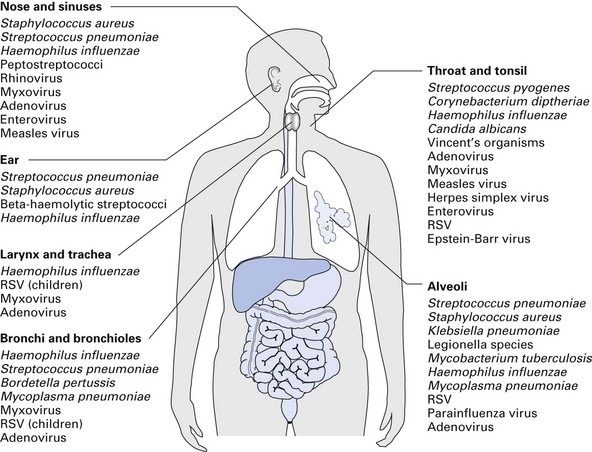
In health, the nose and the throat are colonized by commensal bacterial species, while the lower respiratory tract (the lower bronchi and alveoli) contain only a few, if any, organisms. The nose is the habitat of a variety of streptococci and staphylococci, the most significant of which is Staphylococcus aureus, especially prevalent in the anterior nares. Other commensal flora of the upper respiratory tract include corynebacteria, Haemophilus spp. and neisseriae. In health, these endogenous (and other exogenous) organisms are unable to gain access to the tissues and cause disease because there is an effective array of defence mechanisms (Table 23.1).
Table 23.1 Natural antimicrobial defences of the respiratory tract
IgA, immunoglobulin A.
Important pathogens of the respiratory tract
The major causative agents of bacterial and viral respiratory infections of both the upper and lower respiratory tract are illustrated in Figure 23.1.
Infections of the upper respiratory tract
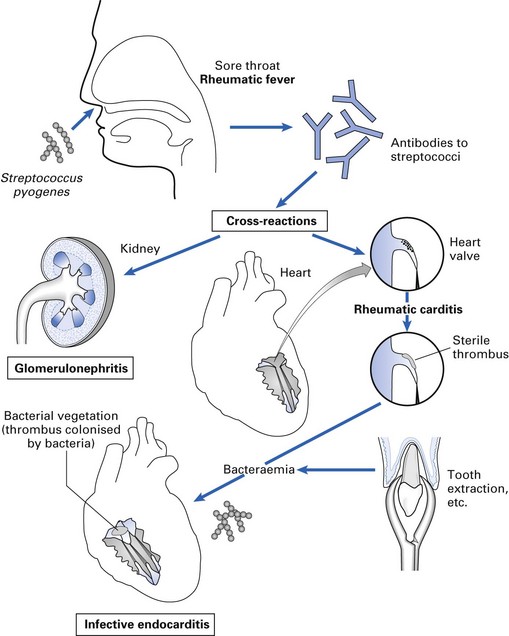
Rheumatic fever
Clinical features
The disease clears spontaneously but may lead to chronic valvular diseases of the heart such as stenosis or incompetence of the mitral or aortic valves in about 70% of patients. Affected individuals are highly susceptible to bacterial endocarditis later in life, when bacteraemias are created during dental or surgical procedures such as scaling. This complication can be prevented by prudent antibiotic prophylaxis prior to such procedures (see Chapter 24).
Pathogenesis
A number of theories have been proposed for rheumatic carditis:
Acute glomerulonephritis
Pathogenesis
Vincent’s angina
Vincent’s angina is caused by the fusospirochaetal complex (fusobacteria and oral spirochaetes). These are normal commensals of the mouth and may overgrow, mainly as a result of poor oral hygiene superimposed on nutritional deficiency, leukopenia or viral infections. The outcome may be necrotizing ulcerative gingivitis (Vincent’s stomatitis) if the infection is localized in the mouth (Chapter 33) or Vincent’s angina leading to massive tissue involvement in the tonsillar area. (Similar fusospirochaetal infections may occur in bite wounds, lung abscesses, bronchiectasis and leg ‘tropical’ ulcers.) The primary cause of these diseases is the anaerobic environment, due to local or systemic factors, which precipitate polymicrobial anaerobic growth.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses