Pain Control for Operative Dentistry
Pain Control
Historically, the public has associated dental treatment with pain. This association is no longer valid because techniques for the elimination of pain, including atraumatic injection, have been available for years and are essential to a successful dental practice. Local anesthesia for operative dentistry must be profound, often to depths required for pulpal anesthesia. The following information, if understood and practiced, should eliminate pain associated with dental procedures. For additional information the reader is referred to Malamed’s Handbook of Local Anesthesia.1
Local Anesthesia
A therapeutic dose of a drug is the smallest amount that is effective when properly administered and does not cause adverse reactions. An overdose of a drug is an excessive amount that results in an overly elevated local accumulation or blood level of the drug, which causes adverse reactions. The normal healthy patient can safely receive five to eight cartridges of anesthetic per appointment. Each 1.8-mL cartridge contains anesthetic, with or without a vasoconstrictor (e.g., lidocaine 2% [anesthetic] with epinephrine 1 : 100,000 [vasoconstrictor], lidocaine 2% plain [no vasoconstrictor]). The number of permissible cartridges increases as body weight increases. According to Malamed, the maximum recommended dose of 2% lidocaine with epinephrine 1 : 100,000 is 4.4 mg/kg, or 2 mg/lb, to an absolute maximum of 300 mg (Online Table 20-1).1 Online Tables 20-1 and 20-2 will help calculate the maximum dose for a specific agent depending on the weight of the patient. These dosages are averages, however, and the dentist must be alert to adverse systemic effects when injected dosages approach the recommended limits.1
Online Table 20-1
Maximum Recommended Dosages (MRDs) of Local Anesthetics Available in North America
| MANUFACTURER’S AND FDA (MRD) | |||
| Local Anesthetic | mg/kg | mg/lb | MRD, mg |
| Articaine | |||
| With vasoconstrictor | 7.0 | 3.2 | None listed |
| Bupivacaine | |||
| With vasoconstrictor | None listed | None listed | 90 |
| With vasoconstrictor (Canada) | 2.0 | 0.9 | 90 |
| Lidocaine | |||
| With vasoconstrictor | 7.0 | 3.2 | 500 |
| Mepivacaine | |||
| No vasoconstrictor | 6.6 | 3.0 | 400 |
| With vasoconstrictor | 6.6 | 3.0 | 400 |
| Prilocaine | |||
| No vasoconstrictor | 8.0 | 3.6 | 600 |
| With vasoconstrictor | 8.0 | 3.6 | 600 |
| CALCULATION OF MILLIGRAMS OF LOCAL ANESTHETIC PER DENTAL CARTRIDGE (1.8 ml CARTRIDGE) | |||
| Local Anesthetic | Percent Concentration | mg/ml | × 1.8 ml = mg/Cartridge |
| Articaine | 4 | 40 | 72* |
| Bupivacaine | 0.5 | 5 | 9 |
| Lidocaine | 2 | 20 | 36 |
| Mepivacaine | 2 | 20 | 36 |
| 3 | 30 | 54 | |
| Prilocaine | 4 | 40 | 72 |
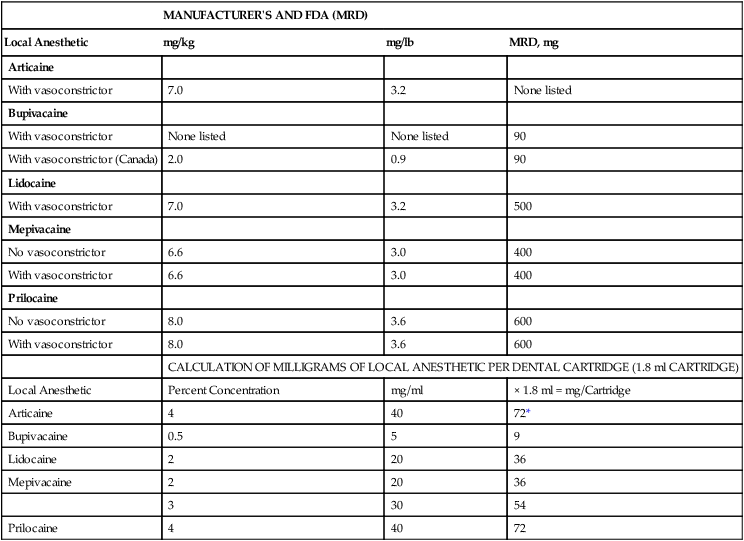
MRD, Maximum recommended dose.
*Cartridges of some drugs in the United States read, “1.7 ml. each” The actual volume of all local anesthetic cartridges is approximately 1.76 ml.
(From Malamed SF: Handbook of local anesthesia, ed 6, St. Louis, 2013, Mosby.)
Local anesthetics have different durations of action for pulpal and soft tissue anesthesia. Pulpal (deep) anesthesia varies from 30 to 90 or more minutes. Soft tissue anesthesia varies from 1 to 9 hours, depending on the specific agent and whether or not a vasoconstrictor is included. Local anesthetics are selected on the basis of the estimated length of the clinical procedure and the degree of anesthesia required (Online Box 20-1). Two (or more) anesthetic agents can be administered when needed. The total dose of both anesthetics should not exceed the lower of the two maximum doses for the individual agents. Anesthetics also are available in amide and ester types. Hypersensitivity and allergic reactions in affected patients are much less frequent with the amide type of local anesthetic.1
Patient Factors
Cardiovascular System
Before administering any drug, the condition of the cardiovascular system (heart and blood vessels) must be assessed. At minimum, blood pressure, heart rate, and rhythm should be evaluated and recorded for all patients. According to the latest guidelines, patients with a systolic pressure less than 160 mm Hg and a diastolic pressure less than 100 mm Hg (stage 1 hypertension) are good candidates for all dental procedures. Patients with blood pressure consistently greater than the aforementioned numbers (stage 2 hypertension) should be referred to their physicians, particularly if the elevation is greater than 20 mm Hg.2 Malamed suggested that any resting patient with a pulse rate less than 60 beats per minute (beats/min) or greater than 110 beats/min be questioned further. Athletes in good physical condition may have a lower heart rate, but without this information, the lower heart rate may indicate a heart block. Additionally, five or more “missed beats” (premature ventricular contractions) per minute with no obvious cause is an indication for medical consultation. Patients with valvular heart disease or a predisposition to bacterial endocarditis should have prophylactic antibiotics prescribed before dental treatment; the American Heart Association defines the recommended regimen for these antibiotics.3
Central Nervous and Respiratory Systems
The central nervous system (CNS) is more easily affected by overdose of injected anesthetic drugs compared with the cardiovascular system. Anesthetics depress the CNS, but when administered properly for local anesthesia, little or no clinical evidence of depression is encountered. At minimal to moderate overdose levels, depression is manifested in excitation (e.g., talkativeness, apprehension, sweating, elevated blood pressure and heart rate, elevated respiratory rate) or drowsiness. At moderate to high overdose levels, tonic-clonic seizure activity may occur, followed by generalized CNS depression, depressed blood pressure, reduced heart rate (<60 beats/min), depressed respiratory rate, and respiratory arrest. With lidocaine and procaine, the usual progression of excitatory signs and symptoms described previously may not be seen, and the first clinical evidence of overdose may be mild sedation or drowsiness.1 The respiratory system is not affected by properly administered therapeutic doses of anesthetic drugs. The system may, however, be depressed and arrested by CNS depression resulting from overdose.
Allergy
Malamed stated that documented, reproducible allergy is an absolute contraindication for administration of local anesthetic.1 When a patient reports a history of “sensitivity” or “reaction” to an injected dental anesthetic, the dentist must believe the patient until further investigation disproves the patient’s claim. Anaphylactic shock from an allergic reaction can be immediate and life threatening. Fast injection and intravascular injection of anesthetics are reasons for allergy-like reactions reported by patients. Some patients have proven allergy to bisulfite, an antioxidant used in anesthetic cartridges as a preservative for the vasoconstrictor.1
Benefits
Salivation Control
Saliva control is a primary reason for the use of profound anesthesia in most patients. For years, it has been observed that complete anesthesia of all tissues (teeth and gingival tissues) in the dental operating site results in a marked reduction of salivation.4 Sometimes, a tooth is not sensitive and does not require anesthesia. If all other sensations from the operating site are eliminated, however, salivation is controlled.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


