Indirect Tooth-Colored Restorations
Edward J. Swift, Jr., John R. Sturdevant and Lee W. Boushell
Class I and II Indirect Tooth-Colored Restorations
Chapters 8, 9, and 10 describe direct tooth-colored composite restorations. Teeth also can be restored using indirect techniques, in which restorations are fabricated outside of the patient’s mouth. Indirect restorations are made on a replica of the prepared tooth in a dental laboratory or by using computer-aided design/computer-assisted manufacturing (CAD/CAM) either chairside or in the dental laboratory (Fig. 11-1). This chapter reviews the indications, contraindications, advantages, disadvantages, and clinical techniques for Class I and II indirect tooth-colored restorations.
Indications
 Esthetics: Indirect tooth-colored restorations are indicated for Class I and II restorations (inlays and onlays) located in areas of esthetic importance for the patient.
Esthetics: Indirect tooth-colored restorations are indicated for Class I and II restorations (inlays and onlays) located in areas of esthetic importance for the patient.
 Large defects or previous restorations: Indirect tooth-colored restorations should be considered for restoration of large Class I and II defects or replacement of large compromised existing restorations, especially those that are wide faciolingually or require cusp coverage. Large intracoronal preparations are best restored with adhesive restorations that strengthen the remaining tooth structure.1–3 The contours of large restorations are more easily developed using indirect techniques. Wear resistance of direct composite resins has improved greatly over the years and is not a concern with small- to moderate-sized restorations.4 However, in larger restorations, indirect restorative materials should be considered.5
Large defects or previous restorations: Indirect tooth-colored restorations should be considered for restoration of large Class I and II defects or replacement of large compromised existing restorations, especially those that are wide faciolingually or require cusp coverage. Large intracoronal preparations are best restored with adhesive restorations that strengthen the remaining tooth structure.1–3 The contours of large restorations are more easily developed using indirect techniques. Wear resistance of direct composite resins has improved greatly over the years and is not a concern with small- to moderate-sized restorations.4 However, in larger restorations, indirect restorative materials should be considered.5
Contraindications
Contraindications for indirect tooth-colored restorations include the following:
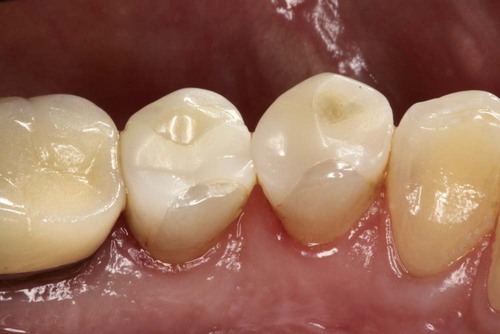
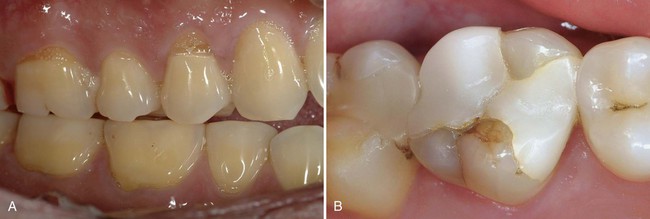
 Heavy occlusal forces: Ceramic restorations can fracture when they lack sufficient thickness or are subject to excessive occlusal stress, as in patients who have bruxing or clenching habits.6 Heavy wear facets or a lack of occlusal enamel are good indicators of bruxing and clenching habits (Fig. 11-2).
Heavy occlusal forces: Ceramic restorations can fracture when they lack sufficient thickness or are subject to excessive occlusal stress, as in patients who have bruxing or clenching habits.6 Heavy wear facets or a lack of occlusal enamel are good indicators of bruxing and clenching habits (Fig. 11-2).
 Inability to maintain a dry field: Despite limited research suggesting that some contemporary dental adhesives might counteract certain types of contamination, adhesive techniques require near-perfect moisture control to ensure successful long-term clinical results.7–9
Inability to maintain a dry field: Despite limited research suggesting that some contemporary dental adhesives might counteract certain types of contamination, adhesive techniques require near-perfect moisture control to ensure successful long-term clinical results.7–9
 Deep subgingival preparations: Although this is not an absolute contraindication, preparations with deep subgingival margins generally should be avoided. These margins are difficult to record with an elastomeric or even a digital impression and are difficult to evaluate and finish. Additionally, dentin bond strengths at gingival floors are not particularly good, so bonding to enamel margins is greatly preferred, especially along gingival margins of proximal boxes.10,11
Deep subgingival preparations: Although this is not an absolute contraindication, preparations with deep subgingival margins generally should be avoided. These margins are difficult to record with an elastomeric or even a digital impression and are difficult to evaluate and finish. Additionally, dentin bond strengths at gingival floors are not particularly good, so bonding to enamel margins is greatly preferred, especially along gingival margins of proximal boxes.10,11
Advantages
 Improved physical properties: A wide variety of high-strength tooth-colored restorative materials, including laboratory-processed and computer-milled ceramics, can be used with indirect techniques. These have better physical properties than direct composite materials because they are fabricated under relatively ideal laboratory conditions. For CAD/CAM restorations, although some are fabricated chairside, the materials themselves are manufactured under nearly ideal industrial conditions.12
Improved physical properties: A wide variety of high-strength tooth-colored restorative materials, including laboratory-processed and computer-milled ceramics, can be used with indirect techniques. These have better physical properties than direct composite materials because they are fabricated under relatively ideal laboratory conditions. For CAD/CAM restorations, although some are fabricated chairside, the materials themselves are manufactured under nearly ideal industrial conditions.12
 Variety of materials and techniques: Indirect tooth-colored restorations can be fabricated with ceramics using traditional laboratory processes or using chairside or laboratory CAD/CAM methods.
Variety of materials and techniques: Indirect tooth-colored restorations can be fabricated with ceramics using traditional laboratory processes or using chairside or laboratory CAD/CAM methods.
 Wear resistance: Ceramic restorations are more wear resistant than direct composite restorations, an especially important factor when restoring large occlusal areas of posterior teeth.
Wear resistance: Ceramic restorations are more wear resistant than direct composite restorations, an especially important factor when restoring large occlusal areas of posterior teeth.
 Reduced polymerization shrinkage: Polymerization shrinkage and its resulting stresses are a major shortcoming of direct composite restorations. With indirect techniques, the bulk of the preparation is filled with the indirect tooth-colored restoration, and stresses are reduced because little resin cement is used during cementation. Although shrinkage of resin materials in thin bonded layers can produce relatively high stress, clinical studies indicate ceramic inlays and onlays have better marginal adaptation, anatomic form, color match, and overall survival rates than do direct composite restorations.5,13,14
Reduced polymerization shrinkage: Polymerization shrinkage and its resulting stresses are a major shortcoming of direct composite restorations. With indirect techniques, the bulk of the preparation is filled with the indirect tooth-colored restoration, and stresses are reduced because little resin cement is used during cementation. Although shrinkage of resin materials in thin bonded layers can produce relatively high stress, clinical studies indicate ceramic inlays and onlays have better marginal adaptation, anatomic form, color match, and overall survival rates than do direct composite restorations.5,13,14
 Support of remaining tooth structure: Teeth weakened by caries, trauma, or preparation can be strengthened by adhesively bonding indirect tooth-colored restorations.1–3 The reduced polymerization shrinkage stress associated with the indirect technique also is desirable when restoring such weakened teeth.
Support of remaining tooth structure: Teeth weakened by caries, trauma, or preparation can be strengthened by adhesively bonding indirect tooth-colored restorations.1–3 The reduced polymerization shrinkage stress associated with the indirect technique also is desirable when restoring such weakened teeth.
 More precise control of contours and contacts: Indirect techniques usually provide better contours (especially proximal contours) and occlusal contacts than do direct restorations because of the improved access and visibility outside the mouth.
More precise control of contours and contacts: Indirect techniques usually provide better contours (especially proximal contours) and occlusal contacts than do direct restorations because of the improved access and visibility outside the mouth.
 Biocompatibility and good tissue response: Ceramics are considered chemically inert materials with excellent biocompatibility and soft tissue response.15 The pulpal biocompatibility of the indirect techniques is related more to the resin cements than to the ceramic materials used.
Biocompatibility and good tissue response: Ceramics are considered chemically inert materials with excellent biocompatibility and soft tissue response.15 The pulpal biocompatibility of the indirect techniques is related more to the resin cements than to the ceramic materials used.
 Increased auxiliary support: Most indirect techniques allow the fabrication of the restoration to be delegated totally or partially to the dental laboratory. Such delegation allows for more efficient use of the dentist’s time.
Increased auxiliary support: Most indirect techniques allow the fabrication of the restoration to be delegated totally or partially to the dental laboratory. Such delegation allows for more efficient use of the dentist’s time.
Disadvantages
The following are disadvantages of indirect tooth-colored restorations:
 Increased cost and time: Most indirect techniques, except for chairside CAD/CAM methods, require two patient appointments plus fabrication of a provisional restoration. These factors, along with laboratory fees, contribute to the higher cost of indirect restorations in comparison with direct restorations. Although indirect tooth-colored inlays and onlays are more expensive than amalgam or direct composite restorations, they are usually less costly than more invasive esthetic alternatives such as all-ceramic or porcelain-fused-to-metal (PFM) crowns.
Increased cost and time: Most indirect techniques, except for chairside CAD/CAM methods, require two patient appointments plus fabrication of a provisional restoration. These factors, along with laboratory fees, contribute to the higher cost of indirect restorations in comparison with direct restorations. Although indirect tooth-colored inlays and onlays are more expensive than amalgam or direct composite restorations, they are usually less costly than more invasive esthetic alternatives such as all-ceramic or porcelain-fused-to-metal (PFM) crowns.
 Technique sensitivity: Restorations made using indirect techniques require a high level of operator skill. A devotion to excellence is necessary during preparation, impression, try-in, bonding, and finishing the restoration.
Technique sensitivity: Restorations made using indirect techniques require a high level of operator skill. A devotion to excellence is necessary during preparation, impression, try-in, bonding, and finishing the restoration.
 Difficult try-in and delivery: Indirect composite restorations can be polished intraorally using the same instruments and materials used to polish direct composites, although access to some marginal areas can be difficult. Ceramics are more difficult to polish because of potential resin-filled marginal gaps and the hardness of the ceramic surfaces.
Difficult try-in and delivery: Indirect composite restorations can be polished intraorally using the same instruments and materials used to polish direct composites, although access to some marginal areas can be difficult. Ceramics are more difficult to polish because of potential resin-filled marginal gaps and the hardness of the ceramic surfaces.
 Brittleness of ceramics: A ceramic restoration can fracture if the preparation does not provide adequate thickness to resist occlusal forces or if the restoration is not appropriately supported by the resin cement and the preparation. With weaker ceramic materials, fractures can occur even during try-in and bonding procedures.16
Brittleness of ceramics: A ceramic restoration can fracture if the preparation does not provide adequate thickness to resist occlusal forces or if the restoration is not appropriately supported by the resin cement and the preparation. With weaker ceramic materials, fractures can occur even during try-in and bonding procedures.16
 Wear of opposing dentition and restorations: Some ceramic materials can cause excessive wear of opposing enamel or restorations.17 Improvements in materials have reduced this problem, but ceramics, particularly if rough and unpolished, can wear opposing teeth and restorations.
Wear of opposing dentition and restorations: Some ceramic materials can cause excessive wear of opposing enamel or restorations.17 Improvements in materials have reduced this problem, but ceramics, particularly if rough and unpolished, can wear opposing teeth and restorations.
 Short clinical track record: Compared with traditional methods such as cast gold or even amalgam restorations, bonded indirect tooth-colored restorations have a relatively short record of clinical service. They have become popular only in recent years, and relatively few controlled clinical trials are available, although these are increasing in number.5,18–35
Short clinical track record: Compared with traditional methods such as cast gold or even amalgam restorations, bonded indirect tooth-colored restorations have a relatively short record of clinical service. They have become popular only in recent years, and relatively few controlled clinical trials are available, although these are increasing in number.5,18–35
 Low potential for repair: When a partial fracture occurs in a ceramic inlay or onlay, repair is usually not a definitive treatment. The actual procedure (mechanical roughening, etching with hydrofluoric [HF] acid, and application of a silane coupling agent before restoring with adhesive and composite) is relatively simple. However, because many ceramic inlays and onlays are indicated in areas where occlusal wear, esthetics, and fracture resistance are important, composite repairs frequently are not appropriate or successful.
Low potential for repair: When a partial fracture occurs in a ceramic inlay or onlay, repair is usually not a definitive treatment. The actual procedure (mechanical roughening, etching with hydrofluoric [HF] acid, and application of a silane coupling agent before restoring with adhesive and composite) is relatively simple. However, because many ceramic inlays and onlays are indicated in areas where occlusal wear, esthetics, and fracture resistance are important, composite repairs frequently are not appropriate or successful.
Types of Ceramic Inlays and Onlays
Although some laboratory-processed composite systems have been available, and at least one machinable composite (Paradigm MZ100, 3M ESPE, St. Paul, MN) is available for CAD/CAM, most tooth-colored indirect posterior restorations are fabricated from ceramic materials.12 Therefore, this chapter will address ceramic inlays and onlays only, with the understanding that the techniques for composite inlays and onlays are generally similar.
Ceramic inlays and onlays have become popular not only because of patient demand for esthetic, durable restorative materials but also because of improvements in materials, fabrication techniques, adhesives, and resin-based cements. Among the ceramic materials used are feldspathic porcelain, leucite-reinforced pressed ceramics, lithium disilicate, and various types of machinable (milled) ceramics designed for use with either chairside or laboratory CAD/CAM systems.36
Feldspathic Porcelain
Dental porcelains are partially crystalline minerals (feldspar, silica, alumina) dispersed in a glass matrix.36 Porcelain restorations are made from finely ground ceramic powders that are mixed with distilled water or a special liquid, shaped into the desired form, and then fired and fused together to form a translucent material that looks like tooth structure. Currently, some ceramic inlays and onlays are fabricated in the dental laboratory by firing dental porcelains on refractory dies, but more are fabricated by pressing or milling methods, which are described later. The fabrication steps for fired ceramic inlays and onlays are summarized as follows:
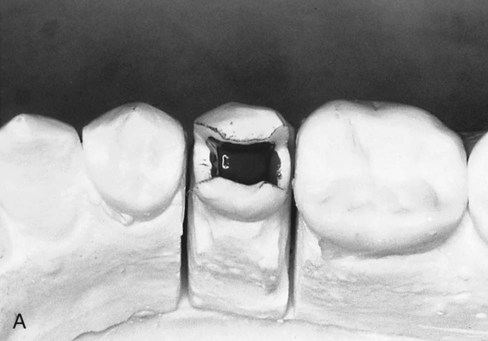
 After tooth preparation, an impression is made, and a die-stone master working cast is poured (Fig. 11-3, A).
After tooth preparation, an impression is made, and a die-stone master working cast is poured (Fig. 11-3, A).
 The die is duplicated and poured with a refractory investment capable of withstanding porcelain firing temperatures. The duplication method must result in the master die and the refractory die being accurately interchangeable (see Fig. 11-3, B).
The die is duplicated and poured with a refractory investment capable of withstanding porcelain firing temperatures. The duplication method must result in the master die and the refractory die being accurately interchangeable (see Fig. 11-3, B).
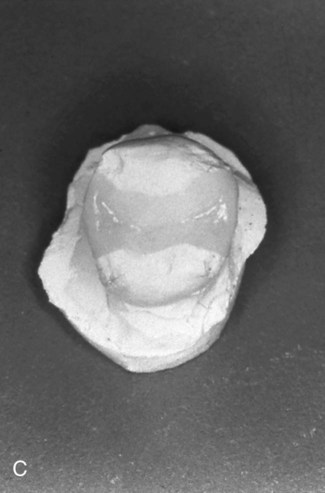
 Porcelain is added into the preparation area of the refractory die and fired in an oven. Multiple increments and firings are necessary to compensate for sintering shrinkage (see Fig. 11-3, C).
Porcelain is added into the preparation area of the refractory die and fired in an oven. Multiple increments and firings are necessary to compensate for sintering shrinkage (see Fig. 11-3, C).
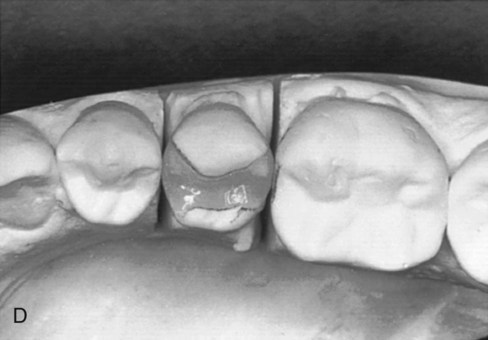
 The ceramic restoration is recovered from the refractory die, cleaned of all investment, and seated on the master die and working cast for final adjustments and finishing (see Fig. 11-3, D).
The ceramic restoration is recovered from the refractory die, cleaned of all investment, and seated on the master die and working cast for final adjustments and finishing (see Fig. 11-3, D).
Although feldspathic porcelain inlays and onlays are less popular than in the past, some dental laboratories continue to use this method because of its low startup cost. The ceramic powders and investments are relatively inexpensive, and the technique is compatible with most existing ceramic laboratory equipment such as firing furnaces. The major disadvantage is its technique sensitivity, both for the technician and the dentist. Inlays and onlays fabricated with this technique must be handled gently during try-in and bonding to avoid fracture. Feldspathic porcelains are weak, so even after bonding, the incidence of fracture can be relatively high.36
Pressed Glass-Ceramics
Over 40 years ago, it was discovered that certain glasses could be modified with nucleating agents and, on heat treatment, be changed into ceramics with organized crystalline forms. Such “glass-ceramics” were stronger, had a higher melting point than noncrystalline glass, and had variable coefficients of thermal expansion.37 At first, these glass-ceramics were developed primarily for cookware and other heat-resistant products. However, in 1984, the glass-ceramic material Dicor (DENTSPLY International, York, PA) was patented and became a popular ceramic for dental restorations. A major disadvantage of Dicor was its translucency, which necessitated external application of all shading.
Dicor restorations were made using a lost-wax, centrifugal casting process. Newer leucite-reinforced glass-ceramic systems (e.g., IPS Empress, Ivoclar Vivadent, Amherst, NY) also use the lost-wax method, but the material is heated to a high temperature and pneumatically pressed, rather than centrifuged, into a mold. Although some studies indicate that hot pressed ceramics are not substantially stronger than fired feldspathic porcelains, they do provide better clinical service.28,29,38,39 The fabrication steps for one type of leucite-reinforced pressed ceramic restoration (IPS Empress) are summarized as follows:
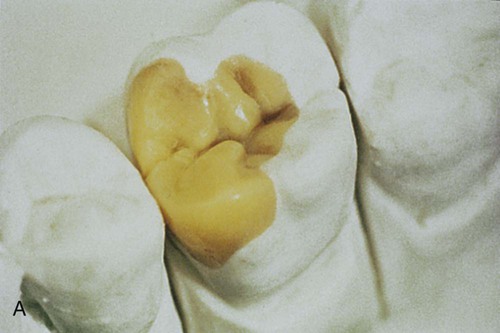
1. After tooth preparation, an impression is made, and a working cast is poured in die-stone. A wax pattern of the restoration is made using conventional techniques (Fig. 11-4, A).
2. After spruing (see Fig. 11-4, B), investing, and wax pattern burnout, a shaded ceramic ingot and aluminum oxide plunger are placed into a special furnace (see Fig. 11-4, C). The shade and opacity of the selected ingot (see Fig 11-4, D) are based on the information provided by the clinician, specifically the desired shade of the final restoration and the shade of the prepared tooth.
3. At approximately 2012°F (1100°C), the ceramic ingot becomes plastic and is slowly pressed into the mold by an automated mechanism.
4. After being separated from the mold, the restoration is seated on the master die and working cast for final adjustments and finishing.
5. To reproduce the tooth shade accurately, a heavily pigmented surface stain is typically applied. The ceramic ingots are relatively translucent and available in a variety of shades, so staining for hot pressed ceramic inlay and onlay restorations is typically minimal.
The advantages of leucite-reinforced pressed ceramics are their (1) similarity to traditional “wax-up” processes, (2) excellent marginal fit, (3) moderately high strength, and (4) surface hardness similar to that of enamel.40,41 Although pressed ceramic inlays and onlays are stronger than porcelain inlays made on refractory dies, they are still somewhat fragile during try-in and must be bonded rather than conventionally cemented. IPS Empress inlays and onlays have performed well in clinical trials ranging up to 12 years in duration.22,24,28,29,42
Lithium Disilicate
A newer type of ceramic, lithium disilicate (e.max, Ivoclar Vivadent Inc., Amherst, NY), is available in both pressed (IPS e.max Press) and machinable (IPS e.max CAD) forms, and either can be used to fabricate inlays and onlays.43 The two forms of e.max are slightly different in composition, but lithium disilicate is a moderately high-strength glass ceramic that also can be used for full crowns or ultra-thin veneers. In vitro testing of this ceramic material has shown very positive results, and it has become a highly popular alternative for inlays and onlays. However, because the material is relatively new, long-term clinical studies to demonstrate superior performance are lacking.
CAD/CAM
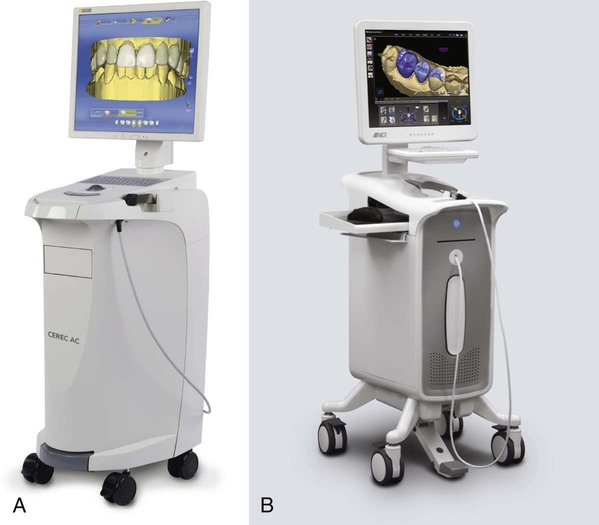
Improvements in technology have spawned increasingly sophisticated computerized devices that can fabricate restorations from high-quality ceramics in a matter of minutes. Some CAD/CAM systems are expensive laboratory-based units requiring the submission of an elastomeric or digital impression of the prepared tooth. The CEREC system was the first commercially available CAD/CAM system developed for the rapid chairside design and fabrication of ceramic restorations. The most popular dental CAD/CAM systems in use today are the CEREC 3D (Sirona Dental Systems, LLC, USA, Charlotte, NC) and E4D (D4D Technologies, LLC, Richardson, TX) (Fig. 11-5).
Generation of a chairside CAD/CAM restoration begins after the dentist prepares the tooth and uses a scanning device to collect information about the shape of the preparation and its relationship with the surrounding structures (Fig. 11-6). This step is termed optical impression. The system projects an image of the preparation and surrounding structures on a monitor, allowing the dentist or the auxiliary personnel to use the CAD portion of the system to design the restoration. The operator must input or confirm some of the restoration design such as the position of the gingival margins (Fig. 11-7).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses