Chapter 20
Managing bone deficiencies for implant surgery
< ?xml:namespace prefix = "mbp" />
Rebuilding alveolar bone width is more predictable than vertical bone grafting. The focus of this chapter is limited to bone grafting in cases with inadequate bone width.
Generally, two different surgical approaches are indicated in cases with inadequate bone width: simultaneous or staged bone grafting (
Table 20.1 Advantages and disadvantages of staged and simultaneous bone augmentation
| Staged (block graft) | Simultaneous (particulate bone) | |
|---|---|---|
| No. of surgeries | Two-stage procedure involving separate grafting and implant placement surgery | Single procedure in which implant is placed and bone grafted |
| Morbidity | Higher because two separate surgical sites, including risk to lower anterior teeth | Reduced |
| Predictability | Predictable | Predictable |
| Scope of grafting | Potentially greater than simultaneously using particulate bone | Predictable in horizontal but unpredictable in vertical augmentation |
| Treatment time | Significantly increases treatment time | Much shorter treatment time |
| Cost | Higher | More cost-effective for the patient |
The former technique, also called simultaneous guided bone regeneration (GBR), is carried out using particulate bone, which is protected under a barrier membrane during healing. This is based on similar principles as guided tissue regeneration in periodontal defects, which was discussed in
On the contrary, if the ridge defect is significant, a staged approach is necessary. This involves grafting with a block of bone of appropriate dimension to rebuild the surgical site. Autogenous bone is still considered to be a gold standard, and this can be harvested from either the mandibular ramus or the symphysial area. The former allows a limited size of bone block, whereas the latter can offer a larger size extending from lower right to left canine.
This chapter discusses two cases illustrating the previously mentioned techniques.
Surgical placement of an implant with simultaneous guided bone regeneration
History
 History of complaint
History of complaint
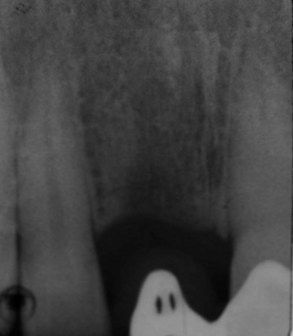
The tooth had a previous history of trauma and reimplantation following avulsion, subsequently developed root resorption, and was extracted when the patient was 16 years old.
 Dental history
Dental history
The patient has been a regular dental attendee and had had several years of endodontic treatment in UR1 before its extraction. The patient is now concerned about the long-term prognosis of UR1 and wishes to have a more predictable solution for the missing tooth. She has lost confidence due to repeated failure of the RBB.
Examination
 Intraoral examination
Intraoral examination
The dentition is minimally restored, with a good level of oral hygiene.
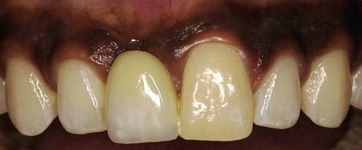
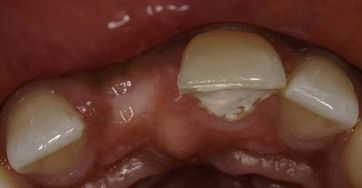
UR1 is missing (
A detailed examination and assessment as discussed in
What important factors would you consider when placing implants with simultaneous GBR?
In order to achieve a successful functional and aesthetic result, several surgical factors must be considered:
It is imperative that the position of the implant is not compromised due to lack of optimal bone volume. For a successful outcome, prosthetically driven ideal three-dimensional position should be the goal.
A good primary stability is necessary for this surgical approach.
Angiogenesis and space maintenance are two important prerequisites for successful GBR. Angiogenesis is promoted by carrying out corticotomy holes. These are holes drilled with a small bur perforating the cortical plate to encourage bleeding from the bone trabeculae. When using particulate bone under a resorbable and malleable membrane, overcontouring with bone graft is recommended to maintain adequate long-term bone volume.
4. Tension-free primary closure
A tension-free primary closure is of significance to ensure the flap remains completely closed during submerged healing. Dehiscence is the most common postoperative complication, which is primarily attributed to forced flap clos/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses