Chapter 2
Viewing conditions
Introduction
Conventional imaging is represented by both digital and analog technologies, whose main features are outlined and compared in Table 2.1. Conventional imaging almost invariably precedes advanced imaging, because it imparts less radiation dose, is generally cheaper, is more widely available and—particularly in regard to intraoral technology—affords the best spatial resolution. This last feature has so far not been remotely achieved by the enormous advances in cone-beam computed tomography (CBCT).
Table 2.1. A comparison between the imaging technologies available to dentists*
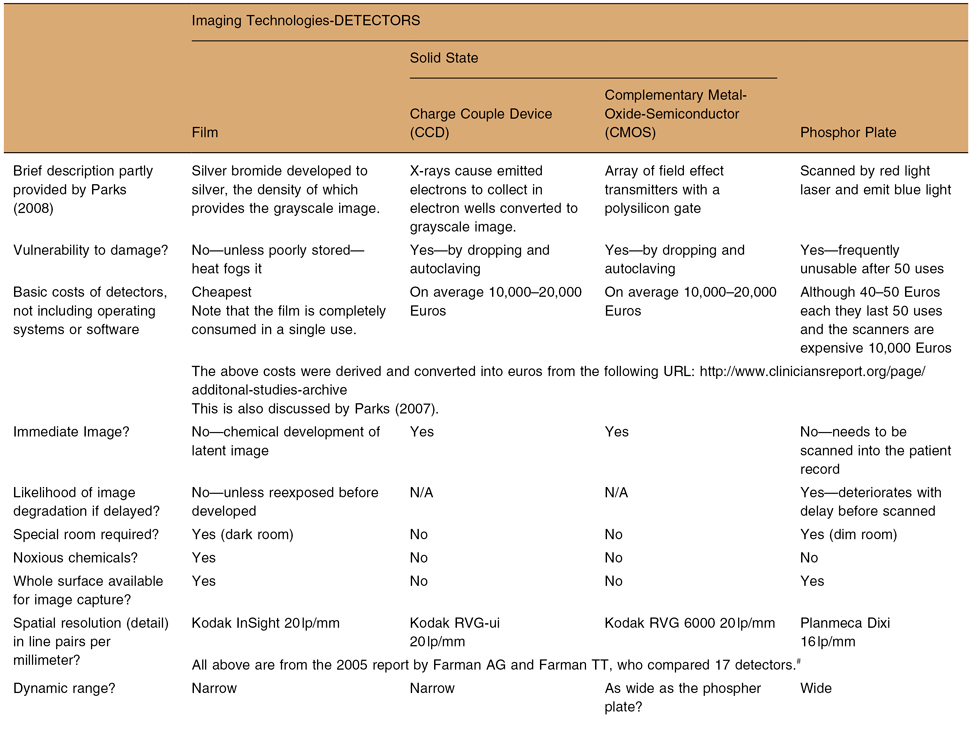
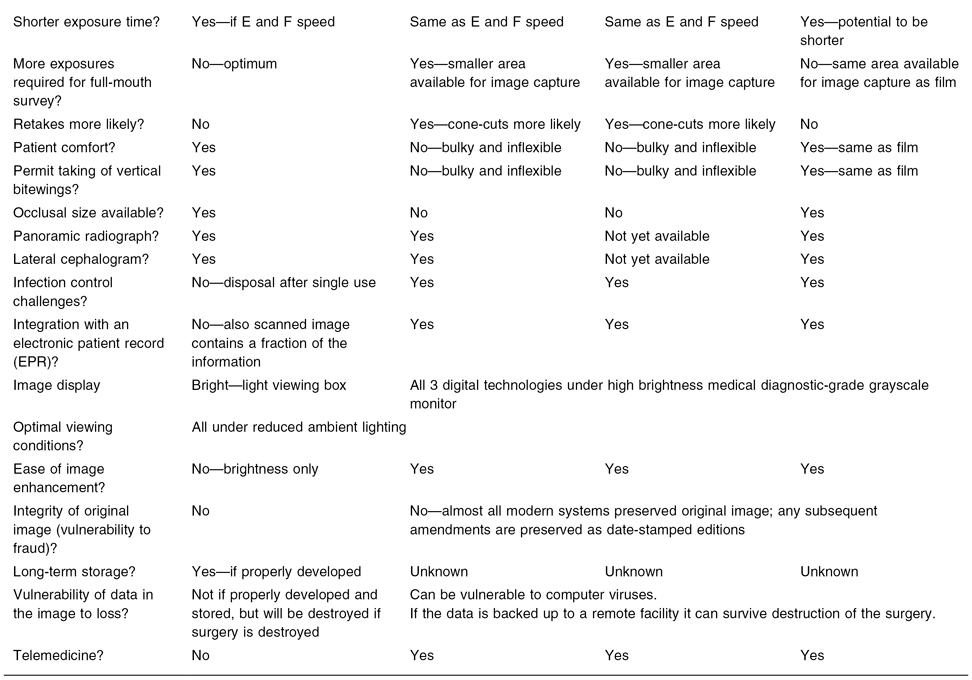
*Adapted from MacDonald DS. Factors to consider in the transition to digital radiological imaging.
Journal of the Irish dental Association. 2009;55:26–34.
#Farman AG, Farman TT. A comparison of 18 different x-ray detectors currently used in dentistry.
Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2005;99:485–489.
The optimal viewing conditions of the images produced by conventional radiography employed by specialist radiologists may differ markedly from those used by many other clinicians. The latter may generally review their radiographic imaging in brightly lit clinical areas. Although this bright lighting assists in the proper evaluation of the patient, it can catastrophically degrade the displayed radiographic image. Because most dentists and oral and maxillofacial specialists are their own radiologists, they should use the same viewing conditions as specialist radiologists for primary readings (radiological diagnosis) of their patients’ images.
Image Display
Although Krupinski et al. found no difference between the performance of radiologists using monitors of differing luminance, the dwell-time (time spent reviewing the image prior to diagnosis) was significantly longer when it was read under suboptimum viewing conditions.1 The two factors affecting display are the quality of the monitor and the ambient lighting at the time of the review of the image displayed on that monitor.
MONITORS
In medicine conventional radiographs taken for diagnosis are read by radiologists on medical-grade diagnostic grayscale (MGDG) monitors under reduced ambient lighting. These monitors are monochromatic. The main advantage of MGDG monitors is their high luminence, which makes it easier to see the entire grayscale from black to white (Figure 2.1). The radiologist produces a report, which accompanies the images. The referring clinician, using a “point-of-care” monitor (usually a standard commercially available monitor of variable quality, which may have a color display) has the radiologist’s report to guide him/her (Figure 2.1c). Other important features of a MGDG monitor are an optimal spatial resolution (image detail, measured in line-pairs per millimeter (lp/mm)) and contrast resolution (discerning the difference between two adjacent densities and commonly expressed in bit-depth or gray levels), high brightness, adjustment for the human eye’s nonlinear perception, and self-calibration (Table 2.2.).
Table 2.2. Comparison between medical diagnostic grayscale monitor and ordinary general purpose monitors
| Medical Diagnostic Grade Grayscale Monitor | General Purpose (Ordinary Commercially Available) Monitors | |
| Color | No (monochromatic)* | Yes |
| Electronic patient record | Yes (but without color)* | Yes |
| Primary radiographic diagnosis (primary read) | Yes | No—used only as aide-memoire at point-of-care |
| Primary read in reduced ambient lighting | Yes—essential | No—advisable but not essential |
| DICOM | Yes 12-bit | No 8-bit |
| Brightness (luminance) | 500 cd/mm | Maximum is 250 cd/mm; most are much lower |
| Grayscale with Windows operating system (OS) | 8-bit | 8-bit |
| Maximum grayscale possible |
10.5-bit for mammography | 8-bit |
| Spatial resolution | 2 megapixel = 1600 × 1200 3 megapixel = 2560 × 2048 |
1080 × 1024 but can be higher |
| Grayscale standard display function | Yes | No |
| Luminance fades over time | Yes | Yes |
| Self-calibration | Yes (if has 12-bit needed for DICOM) | No (almost all have only 8-bit) |
*There are some color medical diagnostic-grade monitors.
Figure 2.1. Monitors. Monitor A is a 3-megapixel medical-grade diagnostic grayscale monitor used for primary radiological diagnosis; monitor B is a 2-megapixel medical-grade diagnostic grayscale monitor used for primary radiological diagnosis; monitor C is the point-of-care color monitor used at the chairside for accessing the electronic patient record, which integrates those images already read on monitor A or B. Note that the lighting chosen was to optimize photography and is not the reduced ambient lighting optimal for primary reading.

The displayed image should fully represent all the data captured by the detector. Ideally, the display of each pixel of the image captured by the de/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


