Chapter 2
Prevention
Aim
To provide an insight into how traumatic injuries to teeth may be prevented.
Objective
After studying the chapter readers should appreciate the ways in which they can help to reduce the incidence of traumatic injuries to teeth.
Introduction
Broadly speaking, approaches to unintentional injury prevention can be divided into:
-
education (provision of information and training)
-
environmental change (modification of products/environment, or use of additional safety devices)
-
enforcement (usually through regulation or legislation).
The prevention of dental injuries may be primary, secondary or tertiary.
Primary prevention is the prevention of circumstances that lead to injury.
Secondary prevention is the prevention or reduction of injury severity in incidents that do happen.
Tertiary prevention is the optimal treatment and rehabilitation of the injured person to minimise the impact of the injury.
Primary Prevention
Playground Surfaces
The most common cause of tooth injury in children is falling onto a hard surface. Most countries have legislation that places the responsibility on any organisation that purchases play equipment to ensure that the equipment conforms to internationally accepted safety standards, and an impact-absorbing surface is provided under items from which children are most likely to fall (Fig 2-1). Studies of accidents to children in playgrounds have shown that the majority of the more serious cases were head injuries caused by striking hard ground. The resilient or compliant elastomeric composition of impact-absorbing surfaces is expensive. A cheaper alternative is tree bark chippings, but these have the disadvantage of needing daily raking to remove, for example, broken glass and animal faeces. Nevertheless, supervision of small children at play (parental or professional) is very important, and probably the most effective way of preventing serious injury.

Fig 2-1 Play areas in a public park with an impact-absorbing surface.
Dentists can play an active part in the provision of appropriate playgrounds by lobbying their local councillors and playing an active part in the surveillance of all play areas for children.
Early (Mixed Dentition) Treatment of Large Overjets
In the UK, there is evidence that the incidence of accidental damage to permanent incisors significantly increases with overjets greater than 9 mm (Fig 2-2). However, the exact relationship between overjet size and the concomitant risk of trauma remains unclear. A recent systematic review has shown that overjets of >3 mm may pose a significant risk for dental trauma, and there is support for including such a measurement in an orthodontic treatment index (Nyugen et al, 1999). The roles of some confounders (lip posture, sports participation, tendency for accidents) remain to be elucidated. Overjet may actually play less of a role as a risk factor in boys, probably because the nature of their activities overrides any effect of overjet.
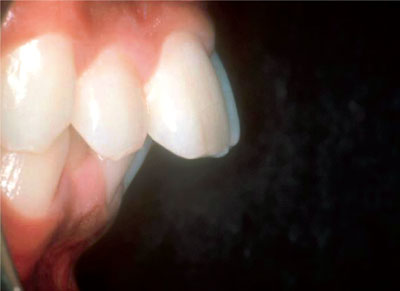
Fig 2-2 Large overjet predisposing to trauma.
Orthodontic treatment in the early mixed dentition is classically carried out in uncrowded arches using functional appliances or extraoral traction. Both treatments work best during active growth and may have a favourable influence on growth in some cases. An early start to treatment does not always mean an early finish, and treatments can be prolonged. If treatment is undertaken in crowded arches, then it is inevitably longer and involves two stages:
-
Primary canine extraction and overjet reduction.
-
Relief of crowding in the permanent dentition by extraction followed by arch realignment with fixed orthodontic appliances.
While it may be feasible to correct incisor relationship in the early mixed dentition, a number of problems may arise. Treatment should not be attempted unless there are strong indications for doing so, and certainly not without a precise orthodontic diagnosis and treatment plan (Richardson, 1989).
Provision of Mouth Protecti/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


