Chapter 9
Permanent Dentition: Intrusive and Extrusive Luxations
Aim
To provide a review of current practice for the treatment of intrusive and extrusive luxations involving permanent teeth.
Outcome
After reading this chapter the reader should be aware of the appropriate treatment for intrusive and extrusive luxations involving permanent teeth.
Intrusive Luxations
Aetiology
These injuries are the result of the tooth being driven upwards into the socket. There is extensive damage to periodontal ligament, pulp, cementum, and alveolar plate(s). The amount of damage to the pulpal neurovascular bundle will depend on the degree of displacement.
Diagnosis
A large degree of force is needed to severely intrude permanent incisor teeth and one should be alert to the possibility of other injuries, including injuries to the head, neck and facial region. Coronal tooth fractures may be superimposed on the intrusive injury but root fractures are rare.
In the established dentition a diagnosis is based on a difference in the position of the incisal edges of affected and unaffected teeth, while in the mixed dentition a high metallic note on percussion is indicative of intrusion or lateral luxation. Radiographic examination is necessary and may reveal differences in apical levels, alveolar fractures or signs of damage to adjacent teeth.
Treatment
The aim of treatment is to maintain the tooth in its normal position in the arch for as long as possible, so that adjacent teeth will erupt into their correct positions and the height and the width of the alveolus will be preserved to facilitate later prosthetic replacement, if the intruded tooth is subsequently lost. In severe intrusion, extraction may be unavoidable.
Extra and intraoral lacerations and wounds should be cleaned and sutured as appropriate. Systemic antibiotics are usually advised. A tetanus booster should be given if external contamination has occurred. Chlorhexidine mouthwash will facilitate plaque removal and the maintenance of good oral hygiene during the initial treatment of the injury.
Two distinct treatment categories exist in intrusive injuries: the open and closed apex. Both categories can be discussed, depending on whether the intrusive injury is: mild (<3 mm); moderate (3–6 mm); or severe (>6 mm). Some authorities would merge the first two categories (<3 mm and 3–6 mm) as the treatment advocated in each is very similar.
Open Apex
-
Mild intrusion: <3 mm. Excellent eruptive potential. Treat conservatively and review. If no eruption in two to four months move orthodontically.
-
Moderate intrusion: 3–6 mm. Disimpact (with forceps if necessary) and either allow spontaneous eruption for two to four months before extruding orthodontically, or apply orthodontic forces early. The relative merits of either treatment option is unproven scientifically. Treatment choice is by clinical judgement and preference.
-
Severe intrusion: >6 mm. In this case the alveolus is grossly dilated labially and occasionally fractured. Orthodontic extrusion should start without delay (Fig 9-1a–g). There is often severe soft tissue displacement and the crown may be completely buried. In such circumstances orthodontic repositioning may not always be possible and disimpaction followed by surgical repositioning is appropriate. Help from a specialist centre may be required. Once the tooth has been repositioned then a functional splint is required for two to three weeks.
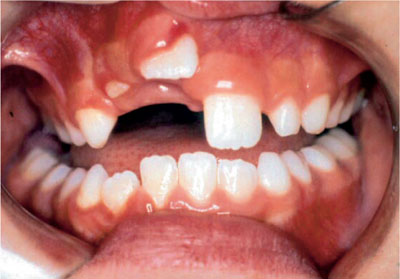
Fig 9-1a Severe intrusion in a patient of eight years of age of tooth 11.
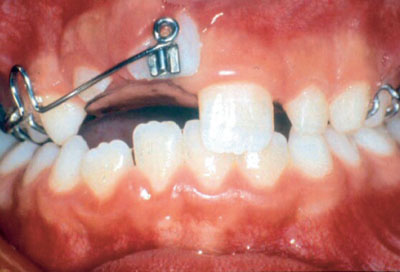
Fig 9-1b Orthodontic extrusion (courtesy of Oxford University Press).
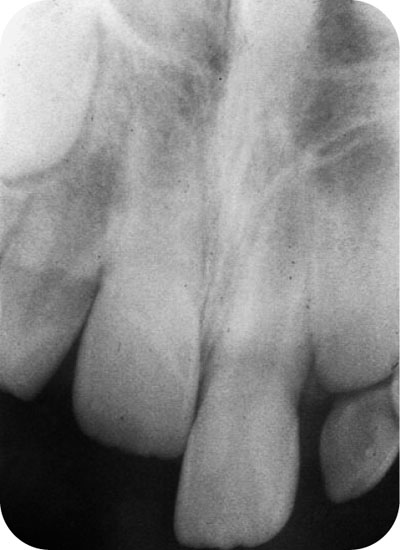
Fig 9-1c Failure of root to mature, tooth 11.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


