Chapter 7
Permanent Dentition: Root Fractures and Splinting
Aim
To provide a review of current practice for the treatment of root fractures in permanent teeth.
Outcome
After reading this chapter the reader should be aware of the appropriate treatment for root fractures and methods of splinting.
Aetiology
The causes of root fractures are no different from those of coronal fractures. They are an uncommon injury in both the primary and the permanent dentition. A prevalence of up to 7% of all injuries has been quoted in the permanent dentition.
Diagnosis
Teeth with root fractures may show mobility, coronal luxation and traumatic occlusion. They may be tender to vertical and horizontal pressure. In these respects they may be clinically indistinguishable from a luxation or a subluxation injury. Not uncommonly, patients with root fractures may exhibit no obvious injury or alternatively may have another more obvious injury. Radiographic confirmation of a root fracture can be difficult because many are oblique and may require radiographs at right angles to each other.
Root fractures may be transverse (horizontal), oblique or vertical. The last type occurs infrequently as a primary injury in young permanent incisors, but may result from secondary trauma to a tooth restored with a post crown restoration.
Vertical root fractures are commoner in heavily restored posterior teeth. Transverse and oblique root fractures are most commonly seen in previously undamaged incisors. They may be single or multiple. Single fractures carry the best prognosis. Root fractures are classified according to the level of the fracture – apical, middle, and coronal (or gingival) third of the root. Coronal root fractures carry the worst prognosis, in particular if they communicate with the gingival sulcus or involve part of the crown. Treatment options are considered in the next section.
For the purpose of this chapter both complicated crown-root fractures and root fractures will be considered.
Treatment
Complicated Crown-root Fracture
Endodontic requirements need to be considered (see Chapter 6). If extrusion is planned then the final root length must be no shorter than the final crown length, otherwise the result will be unstable. Root extrusion can be successful in a motivated patient and can lead to a stable periodontal condition.
Root Fracture
Root fractures occur most frequently in the middle or the apical third of the root. The coronal fragment may be extruded or luxated. If displacement has occurred, the coronal fragment should be repositioned as soon as possible by gentle digital manipulation and the position checked radiographically. Mobile root fractures need to be splinted to encourage repair of the fracture. Apical third fractures, in the absence of concomitant periodontal ligament injury, are often firm and do not require splinting, but need to be regularly reviewed to check pulpal status and treated endodontically if necessary.
Middle third and coronal third fractures must be splinted, as repair of the fracture is essential to the long-term stability and prognosis of the tooth. A functional splint is one that includes one abutment tooth on either side of the fractured tooth and should remain in place for three to four weeks initially (Fig 7-1). Splinting for longer periods may be required in individual cases, in particular if the fracture is in the coronal third. The splint should allow colour observations and sensitivity testing and access to the root canal if endodontic treatment is required. Splint design and placement techniques are discussed in the next section.
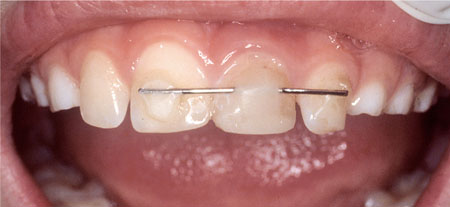
Fig 7-1 Functional composite wire splint. Root fractured 21.
Four main categories of healing are recognised:
-
Repair with calcified tissue: invisible or hardly discernible fracture line.
-
Repair with connective tissue: narrow radiolucent fracture line with peripheral rounding of the fracture.
-
Repair with bone and connective tissue: a bony bridge separates the two fragments.
-
Interposition of the fractured ends by granulation tissue.
In addition to these changes in the fracture area, pulp canal obliteration is commonly seen.
Fractures in the cervical third of the root will not repair if a communication exists between the fracture line and the gingival crevice. If such a communication exists, then splinting is not recommended and an early decision must be made to:
-
extract the coronal fragment and retain the remaining root
-
internally splint the root fracture or
-
extract the two fragments.
Extraction of the coronal fragment and retention of the remaining root
The remaining radicular pulp should be removed and the canal temporarily dressed with non-setting calcium hydroxide prior to root filling with gutta percha and sealer. Three options are now available for the root treated radicular portion:
-
Post, core and crown restoration if access is adequate.
-
Extrusion of root either surgically or orthodontically if the fracture extends too subgingivally for adequate access. Rapid orthodontic extrusion over four to six weeks aiming to move the root a maximum of 4 mm is the best option. This is achieved by cementing a ‘J’ hook made from 0.7 mm stainless steel wire into the canal and using elastic traction applied over an arch wire cemented between one abutment tooth on either side of the injured tooth (Fig 7-2a, b). Retention for one month at the end of movement is advised to prevent relapse. If aesthetics are a particular concern then an orthodontic bracket can be bonded to a temporary crown ma/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


