CHAPTER 19 Treatment of Deep Caries, Vital Pulp Exposure, and Pulpless Teeth
DIAGNOSTIC AIDS IN THE SELECTION OF TEETH FOR VITAL PULP THERAPY
CLINICAL SIGNS AND SYMPTOMS
Abnormal tooth mobility is another clinical sign that may indicate a severely diseased pulp. When such a tooth is evaluated for mobility, the manipulation may elicit localized pain in the area, but this is not always the case. If pain is absent or minimal during manipulation of the diseased mobile tooth, the pulp is probably in a more advanced and chronic degenerative condition. Pathologic mobility must be distinguished from normal mobility in primary teeth near exfoliation.
RADIOGRAPHIC INTERPRETATION
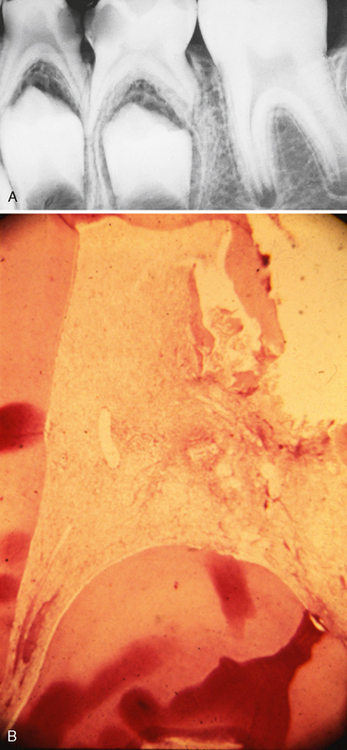
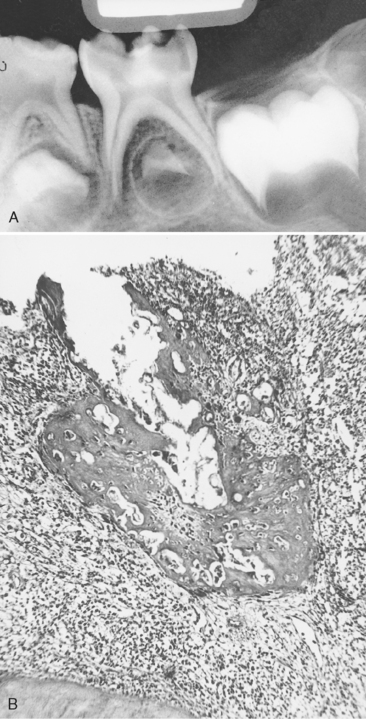
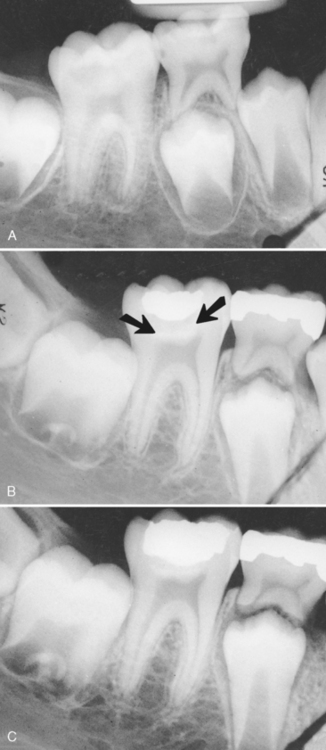
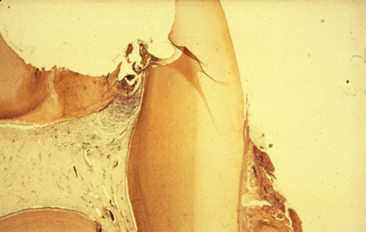
The proximity of carious lesions to the pulp cannot always be determined accurately in the x-ray film. What often appears to be an intact barrier of secondary dentin protecting the pulp may actually be a perforated mass of irregularly calcified and carious material. The pulp beneath this material may have extensive inflammation (Fig. 19-1). Radiographic evidence of calcified masses within the pulp chamber is diagnostically important. If the irritation to the pulp is relatively mild and chronic, the pulp will respond with inflammation and will attempt to eliminate the irritation by blocking with irregular dentin the tubules through which the irritating factors are transmitted. If the irritation is intense and acute and if the carious lesion is developing rapidly, the defense mechanism may not have a chance to lay down the reparative dentin barrier, and the disease process may reach the pulp. In this instance the pulp may attempt to form a barrier at some distance from the exposure site. These calcified masses are sometimes evident in the pulp horn or even in the region of the pulp canal entrance. A histologic examination of these teeth shows irregular, amorphous masses of calcified material that are not like pulp stones (Fig. 19-2). The masses bear no resemblance to dentin or to a dentinal barrier. In every instance they are associated with advanced degenerative changes of the coronal pulp and inflammation of the tissue in the canal.
PULP TESTING
The value of the electric pulp test in determining the condition of the pulp of primary teeth is questionable, although it will give an indication of whether the pulp is vital. The test does not provide reliable evidence of the degree of inflammation of the pulp. A complicating factor is the occasional positive response to the test in a tooth with a necrotic pulp if the content of the canals is liquid. The reliability of the pulp test for the young child can also be questioned sometimes because of the child’s apprehension associated with the test itself. Thermal tests have reliability problems in the primary dentition, too. The lack of reliability is possibly related to the young child’s inability to understand the tests.
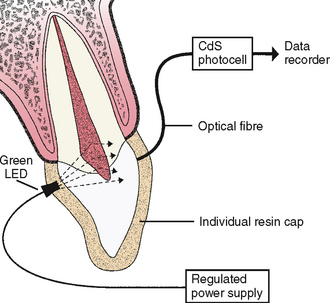
Several methods have been developed and advocated as noninvasive techniques for recording the blood flow in human dental pulp. Two of these methods include the use of a laser Doppler flowmeter and transmitted-light photoplethysmography. As shown in the schematic in Fig. 19-3, these methods essentially work by transmitting a laser or light beam through the crown of the tooth; the signal is picked up on the other side of the tooth by an optical fiber and photocell. A distinct advantage of this technique is its noninvasive nature, particularly in comparison to electric pulp testing. Not only is there inaccuracy in the response of the pulp to electric stimuli, but the electric pulp tester may elicit pain. Because the testing may be uncomfortable for young patients, further dental treatment may be affected. A study by Miwa and colleagues suggests that the transmitted-light technique can detect pulpal blood flow in young permanent teeth and is thus applicable to the assessment of pulp vitality.1
EVALUATION OF TREATMENT PROGNOSIS BEFORE PULP THERAPY
Other factors to consider include the following:
TREATMENT OF THE DEEP CARIOUS LESION
Children and young adults who have not received early and adequate dental care and optimal systemic fluoride and do not have adequate oral hygiene often develop deep carious lesions in the primary and permanent teeth. Many of the lesions appear radiographically to be dangerously close to the pulp or to actually involve the dental pulp. Approximately 75% of the teeth with deep caries have been found from clinical observations to have pulpal exposures. Work by Dimaggio and Hawes supports this observation.2,3 They also showed that well over 90% of the asymptomatic teeth with deep carious lesions could be successfully treated without pulp exposure using indirect pulp therapy techniques. This procedure is described herein.
INDIRECT PULP TREATMENT (GROSS CARIES REMOVAL OR INDIRECT PULP THERAPY)
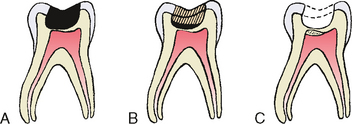
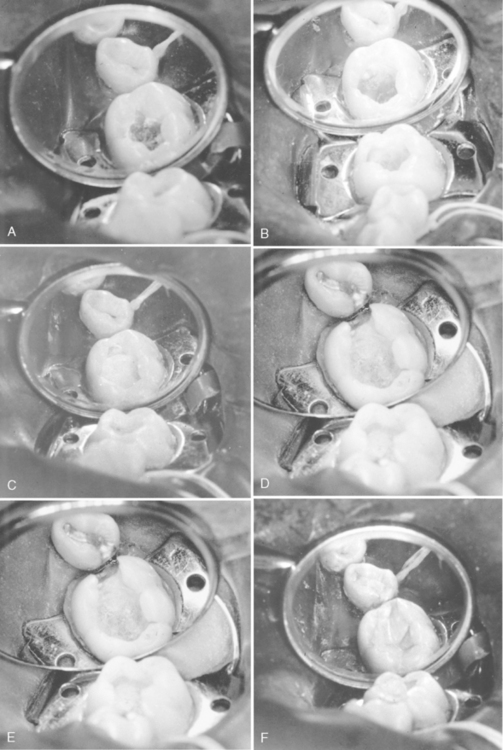
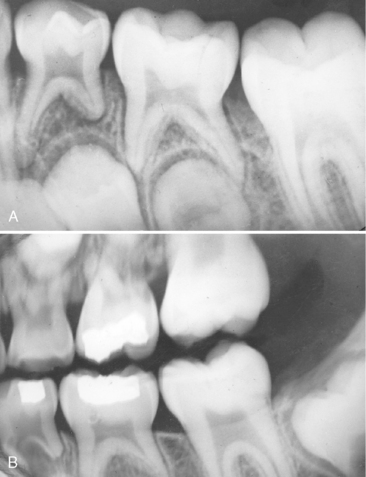
The procedure in which only the gross caries is removed from the lesion and the cavity is sealed for a time with a biocompatible material is referred to as indirect pulp treatment (Fig. 19-4). Indirect pulp treatment is not a new procedure but has attracted renewed interest. Laboratory studies and favorable clinical evidence justify its routine use. Teeth with deep caries that are free of symptoms of painful pulpitis are candidates for this procedure.
The clinical procedure involves removing the gross caries but allowing sufficient caries to remain over the pulp horn to avoid exposure of the pulp. The walls of the cavity are extended to sound tooth structure because the presence of carious enamel and dentin at the margins of the cavity will prevent the establishment of an adequate seal (extremely important) during the period of repair. The remaining thin layer of caries in the base of the cavity is covered with a radiopaque biocompatible base material and sealed with a durable interim restoration (Fig. 19-5). Some interim restorative materials may also serve as the base material. It is sometimes helpful to adapt and cement a preformed stainless steel band to the tooth to support the interim restoration during the observation period (Fig. 19-6).
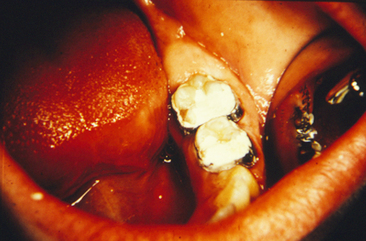
Figure 19-6 Preformed steel band has been cemented to the tooth to support the indirect pulp treatment material.
At the conclusion of the minimum 6- to 8-week waiting period, the tooth is reentered. Careful removal of the remaining carious material, now somewhat sclerotic, may reveal a sound base of dentin without an exposure of the pulp. If a sound layer of dentin covers the pulp, the tooth is restored in the conventional manner (Fig. 19-7). Al-Zayer and associates reported that the use of a base over the calcium hydroxide liner, in addition to a stainless steel crown, dramatically increases the success rate.4 If a small pulp exposure is encountered, a different type of treatment, based on the clinical signs and symptoms and local conditions, must be used.
Studies by Traubman, who used television linear and density measurement instrumentation, indicated that the rate of regular dentin formation during the indirect pulp treatment was highest during the first month, but dentin formation continued during the year of experimental observation.5 At the end of the 1-year observation period, some teeth had formed as much as 390 μm of new dentin on the pulpal floor. This observation provides justification for leaving the sealed interim restoration in place for longer than the minimal 6 weeks.
Nirschl and Avery performed indirect pulp therapy on 38 carefully selected primary and young permanent teeth.6 Gross caries removal under rubber dam isolation was accomplished, calcium hydroxide was used in each tooth as a sedative base, and the teeth were restored with amalgam.
Successful treatment occurred in 32 (94.1%) of the 34 teeth that were available for the 6-month evaluation procedure. In all cases of successful treatment the base material and the residual carious dentin were observed to be dry on reentry and clinical examination. Of the successfully treated teeth, only four had residual carious dentin that felt somewhat soft when probed with an explorer; in the remainder the dentin felt hard. Pinto and colleagues showed similar dentin consistency results, as well as significantly decreased bacterial counts at the end of treatment.7
Indirect pulp therapy has been proved to be a valuable therapeutic procedure in treating asymptomatic teeth with deep carious lesions. The procedure reduces the risk of direct pulp exposure and preserves pulp vitality. One may question the need to reenter the tooth if it has been properly selected and monitored, if a durable restoration is placed initially, and if no adverse signs or symptoms develop. Most clinicians are successfully practicing indirect pulp treatment without reentry after the initial caries excavation. The inexperienced dentist, however, may want to consider performing the treatment in two appointments until confidence in proper case selection has been achieved.
VITAL PULP EXPOSURE
SIZE OF THE EXPOSURE AND PULPAL HEMORRHAGE
The most favorable condition for vital pulp therapy is the small pinpoint exposure surrounded by sound dentin. However, a true carious exposure, even of pinpoint size, will be accompanied by inflammation of the pulp, the degree of which is usually directly related to the size of the exposure (Fig. 19-8).
DENTAL HEMOGRAM
Guthrie’s findings have substantiated the previously mentioned observations.8 His study was designed to investigate the value of a white blood cell differential count (hemogram) of the dental pulp as a diagnostic aid in determining pathologic or degenerative changes in the pulp. The first drop of blood from an exposed pulp was used for making the hemogram. The teeth were subsequently extracted. Based on a histologic examination it was decided whether they would have been good candidates for a pulpotomy procedure. Those teeth in which the inflammatory process was localized to the coronal pulp area were classified as good candidates for a pulpotomy. If the inflammation extended into the pulp canal beyond the area of convenient amputation, the tooth was considered a poor candidate. Although there was no consistent blood picture throughout the group, the teeth considered to be poor risks all had an elevated neutrophil count and gave evidence of profuse bleeding and pain other than at mealtime. In the histologic examination, numerous teeth in the poor risk group showed evidence of internal resorption in the pulp canal.
VITAL PULP THERAPY TECHNIQUES
It is generally agreed that the prognosis after any type of pulp therapy improves in the absence of contamination by pathogenic microorganisms. Thus biocompatible neutralization of any existing pulpal contamination and prevention of future contamination (e.g., microleakage) are worthy goals in vital pulp therapy. If the treatment material in direct contact with the pulp also has some inherent quality that promotes, stimulates, or accelerates a true tissue-healing response, so much the better; however, it is recognized that vital pulp tissue can recover from a variety of insults spontaneously in a favorable environment.
DIRECT PULP CAPPING
It is generally agreed that pulp-capping procedures should be limited to small exposures that have been produced accidentally by trauma or during cavity preparation or to true pinpoint carious exposures that are surrounded by sound dentin (Fig. 19-9). Pulp capping should be considered only for teeth in which there is an absence of pain, with the possible exception of discomfort caused by the intake of food. In addition, there should be either no bleeding at the exposure site, as is often the case in a mechanical exposure, or bleeding in an amount that would be considered normal in the absence of a hyperemic or inflamed pulp.
All pulp treatment procedures should be carried out under clean conditions using sterile instruments. Use of the rubber dam will help keep the pulp free of external contamination. All peripheral carious tissue should be excavated before excavation is begun on the portion of the carious dentin most likely to result in pulp exposure. Thus most of the bacterially infected tissue will have been removed before actual pulp exposure occurs. The work of Kakehashi and colleagues9 and of Walshe,10 which is described later in this chapter, supports the desirability of using a surgically clean technique to minimize bacterial contamination of the pulpal tissue.
Calcium hydroxide remains the standard material for pulp capping normal vital pulp tissue. The possibility of its stimulating the repair reaction is good. A hard-setting calcium hydroxide capping material should be used. If the tooth is small (such as a first primary molar), the hard-setting calcium hydroxide may also be used as the base for the restoration. Some studies have shown successful results with direct capping of exposed pulps with adhesive bonding agents, whereas others have reported pulp inflammation and unacceptable results using this technique.11 In addition, the use of mineral trioxide aggregate has shown promise, but further research would be helpful.12 Therefore the traditional practice of using calcium hydroxide can be maintained.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses