Chapter 19
Promoting Oral Health Care in Long-Term Care Facilities
Mickey Emmons Wener1, Carol-Ann Yakiwchuk2, and Mary Bertone3
1 School of Dental Hygiene, Faculty of Dentistry, University of Manitoba, Winnipeg, MB, Canada
2 Faculty of Dentistry, University of British Columbia, Vancouver, BC, Canada
3 Centre for Community Oral Health, Faculty of Dentistry, University of Manitoba, Winnipeg, MB, Canada
Introduction
Along with longer life spans comes the increased likelihood that many of us will experience challenges managing routine activities of daily living (ADLs, which include independently moving between locations, transferring, eating, using the toilet, and performing personal hygiene tasks). Dependent older adults reside in a variety of settings, such as at home, in an assisted living residence, in hospital for rehabilitation or an extended stay, or in a long-term care (LTC) facility. The majority of elders prefer to receive care at home and enter a facility only when their health concerns become unmanageable (Canadian Healthcare Association, 2009). A renewed focus on improving quality of life and deinstitutionalizing care has led to new models of elder-centered continuous care communities (see Appendix 19.1, Resources for Promoting Oral Health in Long-Term Care). As demands grow for assistance at all levels of LTC, a variety of informal and formal caregivers are needed, including family and friends, a myriad of healthcare providers, and advocates such as social workers.
Mouth care is the foundation of maintaining the oral health of older adults in LTC (Stein & Henry, 2009). Brushing teeth, cleaning dentures – all seemingly simple tasks – become quite complex when individuals are no longer able to care for themselves. Daily mouth care needs vary greatly – from a reminder that it’s time to brush, to keeping the mouth comfortable during palliative care (see also Chapter 2, Palliative Care Dentistry). Advocating for oral health in LTC is of increasing importance as mouth care is at risk for widespread neglect, perhaps as a function of the fact that oral health professionals (OHPs) are typically not part of the healthcare team (MacEntee, 2011). How can we work together to ensure that vulnerable elders have dignity and comfort, are able to eat a nutritious diet, and are not putting their overall health at risk?
The content of this chapter is based on the collective experience of a team of dental hygienists promoting oral health in LTC. Oral health promotion is an “upstream” approach, heavily weighted toward prevention and addressing existing problems early, before more complex treatment is required “downstream.” Our practical approach to oral health promotion for dependent older adults is illustrated in Fig. 19.1, a model using colored rings (oral health promotion strategies) of increasing size stacked on a center cylindrical post (oral health of the older adult). In sequence, from bottom to top in Fig. 19.1, they include: (i) standards, (ii) commitment, (iii) education and training; (iv) assessment and professional care; and (v) daily mouth care. The size of the ring gives stability with the larger ones forming the base from which to build a solid structure. The model recognizes that the base is not necessarily the first ring to be set. For example, education and training may occur first to inform others about oral systemic health and outcomes of poor daily oral hygiene, which then leads to action in the form of being committed to change or developing standards. Until all the rings are in their designated position, the structure is less stable, and correspondingly, the individual’s oral health is less protected. Surrounding the rings are the principle actions in which oral health promotion occurs; these include (a) assess strengths and challenges; (b) collaborate; (c) use personnel effectively; and (d) apply best practices. These four critical environmental elements are described in the following section.
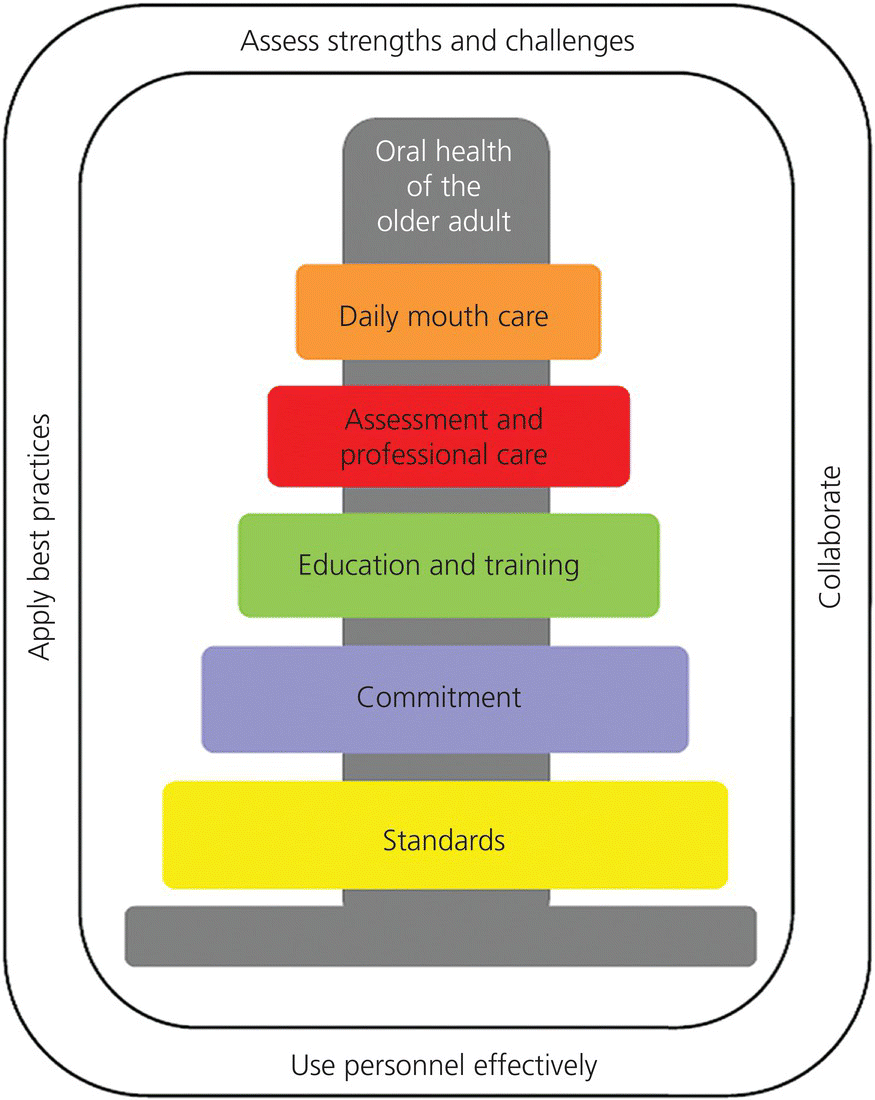
Figure 19.1 An oral health promotion model with application to a variety of long-term care (LTC) settings. Created by Wener, Bertone, and Yakiwchuk, 2012
Assess strengths and challenges
The first step in assessing the oral health promotion environment is to assess the LTC environment. Be aware of the caregiving milieu as settings vary greatly based on size, management, and funding; and, similarly, individual needs vary based on general health, functional and cognitive abilities, and social and financial supports. Barriers to achieving oral health for dependent older adults are pervasive and well-documented (Canadian Dental Association, 2009; Jablonski et al., 2005; MacEntee et al., 2008; McNally & Lyons, 2004; Matthews et al., 2012; Pronych et al., 2010; Stein & Henry, 2009). This growing population has complex medical issues, many of which require medications that cause dry mouth (xerostomia) (see Chapter 2, Palliative Care Dentistry, and Chapter 14, Xerostomia, for additional information). Although oral disease is rampant due to competing concerns and financial challenges, families often relegate dental care to the lowest priority. Loss of function and autonomy is a major “tipping point” in an individual’s oral health status. Being dependent on others for daily mouth care, acquiring oral hygiene products, and arranging for access to dental care contributes to poor oral health. Families and friends, who are the sole caregivers for 70% of the elderly in the USA (US Dept. of Health and Human Services, 2009), are often stressed with multiple responsibilities and limited resources. Caregivers have heavy workloads, view mouth care as an unpleasant, often strictly cosmetic task (Dharamsi et al., 2009; Forsell et al., 2011), and can significantly overestimate residents’ ability to independently care for their own mouths (Forsell et al., 2009; Stewart, 2013). LTC facilities may have mouth care protocols, but often they are not enforced by the facility or by regulatory agencies (Seniors’ Oral Health Secretariat, 2011; Weintraub, 2011). Educational preparation for promoting oral health, from administrators to front-line staff, is woefully inadequate. OHPs themselves often have little preparation and expertise in providing this specialized care, are unfamiliar with and unwilling to explore the LTC milieu (Nunez et al., 2011), and have limited experience being part of a healthcare team (Institute for Oral Health, 2008; MacEntee, 2011). Add to these barriers the lack of integration between dental and medical care, discriminatory ageism (stereotypical prejudicial attitudes and practices regarding older people), and the frequently present physical and cognitive challenges that impact upon the abilities of elders, and we are in the midst of the perfect storm for oral and overall health problems. A chilling example of the result of oral neglect is seen in the following newspaper article excerpt:
Nursing home fined $100,000 for death. The resident, a 76-year-old woman who required total assistance with daily living activities, died from a dental abscess that led to cardiopulmonary arrest, according to the California Department of Public Health. The CDPH investigation revealed that the woman was not given a dental exam because “the facility thought the resident had dentures”
(Jackson, 2007).
Collaborate
Interprofessional practice is becoming the cornerstone of improved patient outcomes (Institute of Medicine, 2011a; World Health Organizaiton, 2010). Fostering environments that support collaboration and team communication to discuss perspectives, goals, and roles brings stakeholders together, increasing readiness to move forward with promoting oral health (Yoon & Steel, 2012). Reconnecting the frequently ignored health of the mouth with overall health and wellness to establish common ground and support quality of life is the all-important first step. It takes a person-centered, proactive care team of elders, their families, decision-makers, caregivers, and advocacy bodies such as the Alzheimer’s Society to help create an environment supportive of oral healthcare. On a day-to-day basis, team communication is crucial to ensure feedback and best care. For example, did the home care worker let the family know that the denture is broken and needs repair? Did the dental hygienist providing clinical care connect back with the unit nurse to follow-up on strategies to promote better daily care? Did the dietitian’s recommendation of sugar-laden liquid meal substitutes to assist in weight gain result in appropriate changes to the mouth care protocol?
Use personnel effectively
Promoting oral health requires a motivated, caring champion to act as an advocate (MacEntee et al., 1999, 2008). OHPs need to support or be champions, and likewise, care providers need to recognize the important roles that OHPs can play (Table 19.1). Including OHPs on the healthcare team can increase the likelihood of improving oral health through increased visibility, active participation, and regular evaluation of results (Chalmers et al., 2009; Thorne et al., 2001). Other caregivers are well-positioned to champion oral health, such as the nurse trying to prevent ventilator-acquired pneumonia (VAP) or the concerned administrator who has just experienced a critical incident stemming from poor oral health. Decisions regarding oral care roles need to be based on scope of practice, training, and cost-effectiveness. Remuneration can significantly impact how personnel are utilized. For example, if OHPs are compensated strictly on a fee-for-service basis for specific clinical services provided, this can limit their ability to participate in health promotion activities. Whereas, a salaried OHP position can provide the flexibility needed to provide caregiver education, respond to an on-unit request for mouth care coaching, or to participate in an interprofessional healthcare meeting. There is no proven personnel formula; however, with expertise in oral health promotion, dental hygienists have been identified as being well suited for the LTC environment as they have the requisite skills, are prevention-focused, and are increasingly able and willing to practice as primary healthcare professionals in alternative settings (Coleman et al., 2006; Glasrud et al., 2005; Monajem, 2006).
Table 19.1 Roles in long-term care (LTC) can extend far beyond clinical care
| Oral health professional roles in LTC |
Oral assessment
|
Clinical oral care
|
Mouth care training
|
Policy and protocol development
|
Apply best practices
While bringing available evidence to bear on decision making, keep in mind the efficacy and the effectiveness of any intervention – “Does it work?”; “Will it work?” Feasibility can only be addressed by direct involvement of the care provider and recipient. For example, a therapeutic mouth rinse may be proven effective, but is the individual actually capable of swishing and spitting and avoiding swallowing or aspirating the rinse? Do LTC personnel know the rationale for its use and assume responsibility for including it in daily mouth care? Guidelines do exist for best oral care practices for dependent older adults; however, there is no widely recognized and standardized evidence-based protocol (MacEntee et al., 2012). Much of what is done in practice combines research and protocols from a variety of sources with personal experience and preference. It is an area ripe for research and regulation, and brings us to the first ring of the model: Standards.
Standards (health promotion ring 1)
My mother has just entered long-term care and I am appalled at the lack of oral care provided. What exactly am I allowed to do? What standards exist regarding oral health?
Registered Dental Hygienist
I am pretty sure that we have mouth care policies, but I don’t recall ever seeing them.
Healthcare Aide
Reports of over two-thirds of residents without their own toothbrush, or caregivers wearing gloves with visible feces from a previous task to brush a resident’s teeth (Coleman & Watson, 2006), are telling signs of the oral healthcare crisis in LTC. What governance measures are in place at the national, state/provincial, regional or facility levels in your jurisdiction to protect and promote an elder’s oral health in LTC? And more importantly, are these measures monitored and enforced for quality control?
The foundation of our LTC oral health promotion model upon which all of the other rings rest, represents a range of recognized measures and requirements for providing and evaluating the quality of mouth care including legislated acts and regulations, standards, guidelines, policies, and protocols (Table 19.2). Care providers need to be knowledgeable about relevant legislation that establishes standards, governs the scope of practice of OHPs, and protects vulnerable cognitively impaired older adults as these requirements impact upon how care is provided (Table 19.3).
Table 19.2 Terminology
|
Table 19.3 Regulatory requirements direct and shape practice
Explore legislation in your jurisdiction that:
|
Oral health in LTC legislation
US Federal Law, the Omnibus Budget Reconciliation Act (OBRA) of 1987, requires facilities that accept Medicare or Medicaid residents to do the following (Guay, 2005; Haumschild & Haumschild, 2009):
- assess oral health using the Minimum Data Set (MDS) tool;
- complete an oral examination within 45 days of admission and annually thereafter;
- provide for dental care;
- provide daily oral hygiene care; and
- offer annual staff in-service training sessions.
More than half of the US states have requirements beyond OBRA requirements. For example, Minnesota regulations include that a facility must arrange on-site dental services for residents who cannot travel, establish a resident’s daily oral care plan during the initial assessment, and provide the necessary supplies and assistance for daily oral care (Minnesota Administrative Rules, 1995). In Canada, the government provides medical care for all permanent residents (Canada Health Act), but does not cover home and institutional care for the frail. There is no Canadian national or provincial infrastructure for oral healthcare for elders, and little national consistency in the actual delivery of health care, including LTC, which is provincially regulated (McNally & Lyons, 2004). All of the Canadian provinces but none of the territories have legislation that can be interpreted to incorporate or mandate oral healthcare services in LTC facilities (Abi-Nahed, 2007). Only 2 of the 10 provinces were found to have established government LTC standards that included oral care: Ontario (Long-Term Care Homes Act) and British Columbia (Community Care and Assisted Living Act), while others are anticipating regulatory change.
To become a licensed LTC facility, governments require yearly on-site inspections to determine if established standards, such as those required by OBRA, are being met (Castle, 2012). Even where oral care requirements are legislated, there are still significant gaps in care observed including many with poor oral health, long periods of time without being seen by a dentist or lack of help with daily mouth care (Frenkel et al., 2000; Henry, 2005; Seniors’ Oral Health Secretariat, 2011). Problems enforcing oral care standards have been reported and include lack of awareness of the regulation, lack of collaboration, not expecting inspectors to assess mouth care, and very limited investigation of daily mouth care during scheduled site inspections (Jiang & MacEntee, 2013). Experts call for a more explicit framework to systematically assess oral healthcare programs in LTC (MacEntee, 2011). The ONiIE (Oral Neglect in Institutionalized Elderly), yet to be operationalized, is an assessment tool that defines neglect for 29 oral conditions, which could help provide enforceable guidelines for quality assurance monitoring of LTC facilities (Katz et al., 2010). Legislated government funding of oral health in LTC could improve oral care (Helgeson & Smith, 1996), improve integration with other publicly funded health services (MacEntee et al., 2012), ease consent for treatment from guardians, and increase the number of OHPs willing to provide care (Seniors’ Oral Health Secretariat, 2011).
Oral care guidelines
When health departments, facilities, or home care agencies have standardized policies and procedures, such as valid assessment and daily care plan tools, caregivers’ involvement in maintaining residents’ oral health can improve (Berry et al., 2011; Chalmers et al., 2009). OHPs can play an important leadership role in their development, including educating key decision-makers regarding why particular directives are important. The challenge in developing policies is that there is no consensus on an ideal oral care protocol due to a lack of scientific evidence based in the real world of LTC, multiple factors influencing individual needs, and the wide variety of available oral hygiene products, tools and techniques (Berry et al., 2011). For example, in the development of the Oral Health Care Guideline for Older People in Long-Term Care Institutions, 12 of the 16 recommendations were based on expert opinion, with only 4 based on research evidence (De Visschere et al., 2011). For guideline documents, see Appendix 19.1 (Resources for Promoting Oral Health in Long-Term Care). For policy example see Appendix 19.2 (Example of Oral Health Promotion Guidelines for a Long-Term Care Facility).
Elders access to care legislation
Access to care is maximized by allowing professionals to practice to the full extent of their education in a variety of settings (Institute of Medicine, 2011b). The ability of US dental hygienists to practice independently in LTC varies greatly between states, and is an increasingly topical issue (Jablonski et al., 2005). To help address access to care, Minnesota’s 2001 legislation allows dental hygienists who are in a collaborative agreement with a dentist to practice without the presence, diagnosis, and treatment planning of a dentist in settings other than dental offices. In Canada, significant regulatory reform in the vast majority of the 10 provinces allows dental hygienists to initiate care as primary healthcare professionals. This has led to a growing number of mobile dental hygiene practices able to visit private homes and LTC facilities.
A lack of existing and enforced public policies and guidelines for the provision of accessible oral health care is putting dependent older adults in LTC at risk. OHPs and concerned others must advocate at all levels for legislated, measureable, and enforced standards that support vulnerable elders’ oral health (Canadian Dental Association, 2008; MacEntee et al., 2008; McNally et al., 2012; Petersen & Yamamoto, 2005; Weintraub, 2011). The bottom line is that many believe that achieving oral health is important in LTC, but few follow through. This gap forms the impetus for champions committed to promoting oral health.
Commitment (health promotion ring 2)
Everyone is concerned about the health of older adults. No one is quite sure who is responsible for their ORAL health.
All too often, administrators and caregivers are unclear of the role they should play and why it is necessary to improve their oral healthcare program (Dharamsi et al., 2009; McKelvey et al., 2003). Commitment, the second health promotion ring, provides a crucial foundation toward supporting oral health change for dependent older adults. By serving as strong advocates and meeting with all stakeholders, OHPs can help everyone involved understand the significance of their roles and potential impact of their improved efforts. As commitment builds, the OHP champion’s role can transition toward empowering and inspiring leadership in others through education, collaboration, and mentorship (Table 19.4). Through transformational leadership, OHPs can positively impact caregivers’ attitudes, behavior, and performance toward sustainable change, while creating the synergy and connectivity necessary within the organization to build momentum (Daft, 2008).
Table 19.4 Assessing your readiness to be an oral health champion
|
What appears contingent on sustaining oral healthcare improvements is a strong consideration for the organizational context within the caring environment (MacEntee et al., 2008; Thorne et al., 2001). What culture and values are inherent within the organization? Who are the decision-makers? What internal structural processes can be used to effectively implement change? How ready is the organization to accept change? Results of several studies emphasize the importance of partnering with an internal staff member to help increase the focus of daily mouth care and promote commitment among staff (Pronych et al., 2010; Wardh et al., 2003). Through shared leadership and collaboration with internal champions who have experience working within their organization, sustainable improvements can be made (MacEntee et al., 2007; Weintraub 2011).
Getting to know the players
Many stakeholders are involved in the care of older adults, each with their own abilities, responsibilities, and priorities. In the home setting, family, friends, home care workers, and nurses serve as the primary caregivers. In LTC, there exists a hierarchy of caregivers, including:
- Administrators, who are responsible for meeting legislated requirements, managing finances, and overseeing a level of care that ensures low resident morbidity and mortality rates.
- Directors of Nursing and Unit Nurse Managers, who are concerned with staffing, supervising daily care, and liaising with physicians and family members or other decision-makers.
- Clinical Nurse Specialists or Nurse Educators, who are responsible for introducing new care programs and guidelines and providing ongoing staff education.
- Infection Control Nurses, who oversee wound management, ensure infection control standards are met, and manage infections and viral outbreaks among residents.
Managerial personnel can be powerful advocates and promoters for oral healthcare change; however, it is crucial to involve direct care staff and other health professionals involved in the individual’s care. Certified Nursing Assistants (CNAs) or Residential Care Aides (RCAs) often possess the least amount of formalized education and training of all care staff, yet perform most of the day-to-day care for dependent older adults (Chalmers & Pearson, 2005a; Jablonski et al., 2005). These individuals are responsible for providing daily mouth care, among many other tasks. The literature consistently reports that direct care providers experience many conflicting demands and face numerous organizational, social, and practical barriers (McNally et al., 2012). It is important to take into consideration that their communication channels are typically more informal, relationship-based, and oral rather than written (Caspar, 2012). One must ensure that CNAs/RCAs are supported through effective two-way feedback loops that involve them in care plans and recognize their invaluable contribution. Thus, health promotion efforts must focus on empowering CNAs/RCAs through education, training, and administrative support.
Along with understanding the care environment, you may wonder how to identify the person with the authority to make decisions; whom to speak with first to gain commitment. Beginning the relationship with a LTC facility by meeting with administration provides a connection with key decision-makers who have the power to support your efforts through leadership, funding, policy enforcement, and opportunities for caregiver education. Administrators can identify the facility’s primary oral health concerns, and guide you toward realistic, culturally appropriate interventions. Establishing a high level of commitment from nursing staff is also paramount as these individuals can work to address barriers faced by direct care providers, monitor the quality of mouth care provided, and liaise with families. The OHP champion also needs to establish and maintain a strong commitment from CNAs/RCAs by serving as their educator, mentor, ally, and advocate. You may also find strong supporters among dietitians, speech language pathologists, physiotherapists, occupational therapists, and caring family members. A social worker partner can help identify financial resources for needed care and become an advocate to help reduce costly treatment needs. The topic of oral healthcare holds importance to every individual involved in an older adult’s care; the challenge is to make a meaningful connection.
Collaborating and partnering for a common ground approach
Oral health programs must be built on the connectivity of trusting relationships that promote involvement, collaboration, and empowerment of all stakeholders. A sense of partnership can be fostered using a “common ground, common language” approach. By highlighting the overlapping health concerns that OHPs share with other health professionals in relation to an older adult’s health and quality of life, and tailoring the message to each staff member’s role and responsibilities, the issue of poor oral health and the need for change become more tangible and realistic for everyone involved (Fig. 19.2). For speech language pathologists, it may be our shared concern over aspiration pneumonia; for a direct care provider, it may be resident comfort and maintaining a person’s quality of life. The ability to “talk the same talk” and contextualize oral diseases, with phrases like “mouth care is infection control” and “gum disease is equal in size to a bed sore the size of the palm of your hand” translates oral health concerns into terms that are common to everyone (Figs 19.3 & 19.4). Avoiding blame and recognizing everyone’s important contributions are additional important strategies for OHPs who wish to transformationally champion change.
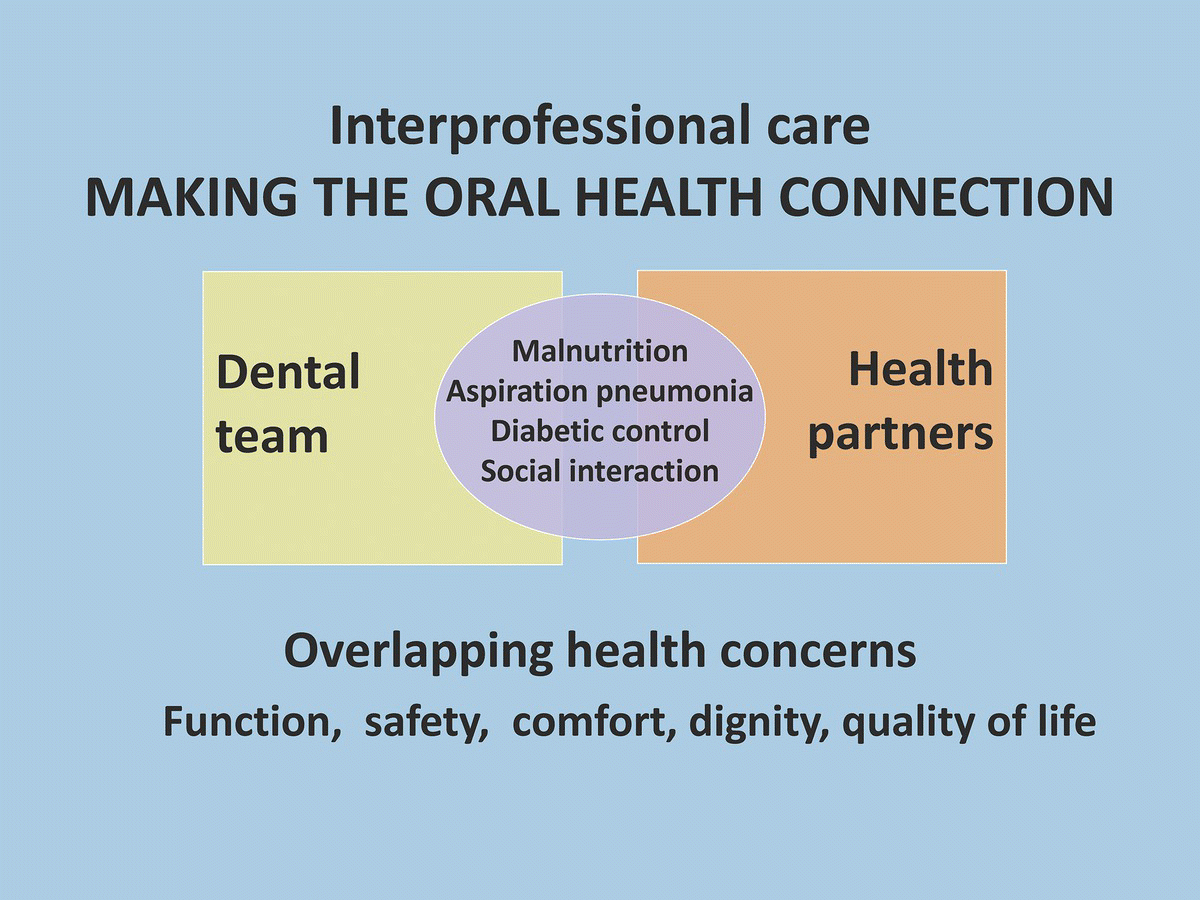
Figure 19.2 Training slide that helps to establish “common ground.” Created by Wener, Bertone, and Yakiwchuk, 2012.
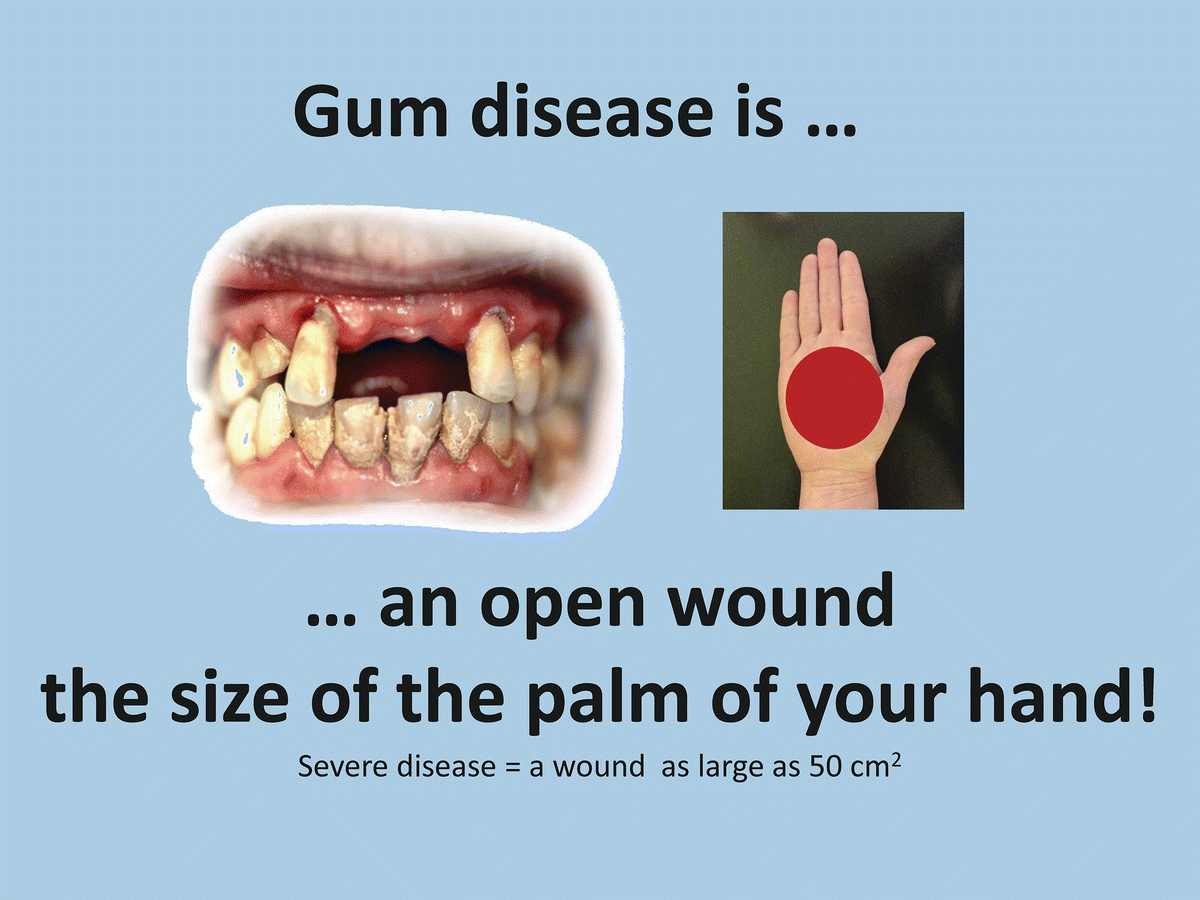
Figure 19.3 Training slide that translates “invisible” oral disease into a visible wound to which caregivers can relate. Reference: Slade et al. (2000). Intraoral photograph permission from J. Morreale. Created by Wener, Bertone, and Yakiwchuk, 2012.

Figure 19.4 Training slide that changes the perception of daily mouth care from that of grooming to preventing infection. Created by Wener, Bertone, and Yakiwchuk, 2012.
Listening to learn and build trust
A good understanding of the environment is vital prior to strategizing ways to build capacity and plan for change. It is crucial to recognize that caregivers are experiencing increasingly heavier demands on their time and skill level as the resident population continues to become more frail, dependent, and medically compromised (McGregor & Ronald, 2011). This begins with asking the right questions, actively listening, and adopting a “move forward” attitude that supports and celebrates even small improvements.
Who is serving as the primary caregiver for those living at home? Are they following a mouth care protocol? Is the older adult able to cooperate? Observing in an open-minded nonjudgmental manner that avoids blaming, and openly exploring these questions with the family and caregivers provides a springboard for change. Similarly, within a facility, listening to their challenges and learning about their practices are crucial steps. What processes are in place for assessment, screening, treatment, and daily care? What policies, protocols, and forms are being used? What is the overall philosophical approach to care? What licensure or accreditation requirements related to oral health need to be met?
The greatest challenge is maintaining ongoing commitment from stakeholders, especially of front-line caregivers who have a high staff turnover rate (Chalmers & Pearson, 2005a; Harrington & Swan, 2003; Jablonski et al., 2005; National Centre for Assisted Living, 2011). Maintaining visibility, keeping everyone informed, and continuing to boost and sustain a commitment to quality oral health care is essential. When an OHP champion visits the unit to help caregivers solve mouth care challenges, this communicates interest and a willingness to sincerely work together toward a common goal, further deepening the level of commitment by everyone involved. The next section describes the educational strategies and content that is crucial for commitment, in particular for the support of daily mouth care.
Caregiver education and training (health promotion ring 3)
The mouth … it’s personal … I don’t feel comfortable doing it.
If a resident refuses to let me brush … I need to respect his or her rights.
Really … taking care of someone’s mouth is not part of nursing.
You mean you’re going to teach me how to brush!
Caregiver education on its own has not consistently resulted in sustainable oral health improvements for older adults, leading many to question its value and importance in supporting oral healthcare change (Gammack & Pulisetty, 2009; MacEntee et al., 2007; McKelvey et al., 2003; Munoz et al., 2009; Peltola et al., 2007; Simons et al., 2000). Yet, there is no denying that education and training is an important part of the solution, based on extensive feedback from caregivers of their need for additional oral health knowledge, training, and skill (Coleman & Watson, 2006; Dharamsi et al., 2009; McKelvey et al., 2003; McNally et al., 2012; Peltola et al., 2007; Unfer et al., 2011). Ageism prejudice, reportedly common among the health professions, also impacts caregivers’ perceptions of this population’s oral healthcare needs (Giles et al., 2002; Larsen & Lubkin, 2009; Whitman & Whitman, 2006) (see also Chapter 4, Palmore’s Facts on Aging Quiz). Caregiver education and training, the third ring of the model, plays a pivotal role in transforming people’s attitudes and beliefs towards oral healthcare when opportunities for discussion, reflection, and feedback are included (Apte, 2009; Mezirow, 2009). Education and training provides caregivers with evidence-based information, tools, and skills that can help strengthen their commitment toward oral healthcare improvements.
Almost everyone involved in an older adult’s circle of care needs education and training. Family members in the home setting may never have brushed another person’s teeth, and be unaware of the impact of prescription medications on one’s comfort and health (McNally et al., 2012). Nurses involved in performing oral screenings may be unprepared to recognize normal versus abnormal findings or how to systematically examine the mouth. RCAs/CNAs may not know why mouth care needs to be provided several times a day, or why they should continue brushing when gums bleed. Oral health content and training is reportedly sparse and out-dated in nursing and other health professions curricula worldwide; hence, most care staff will benefit from initial and ongoing oral health education and training (Hahn et al., 2012; Hein et al., 2011; Jablonski, 2012). Even within the OHPs, there is an urgent need to more adequately prepare individuals to interact and work with geriatric populations and their caregivers through enhanced curricula, experiential learning opportunities, and mentorship (Bardach & Rowles, 2012; National Seniors’ Task Force, 2008).
When planning training, there are many considerations. What format works best for your target audience? Are there other programs that can be used to model or piggy-back training sessions onto? What costs are involved? Where and when should training take place? How will administrative support be communicated? How will the schedule of sessions be publicized? Will this be required of staff, or voluntary, and if required, how will that be conveyed to staff members?
Venues and timing
Caregiver education and training can take place in a number of environments using a variety of approaches. Delivering a seminar to CNA/RNA students, offering a workshop at a local caregiver conference, manning a display in a facility, or even writing newsletter articles for LTC all represent excellent ways to share information. LTC facilities will have established structures and processes for how and when caregivers receive other types of education and training that are important to consider. What classroom facilities are on-site? What time of day and length of session will encourage attendance? Since time away from the unit is time away from caregiving responsibilities, a KISS approach works best: Keep It Short and Succinct. For efficiency, offer one session to both the day and evening shift staff by scheduling the session mid-afternoon and asking those on the evening shift to arrive early. Bedside hands-on training and support, small group learning on-unit, and having staff access online resources (podcasts, blogs, fact sheets), or view videotaped training sessions are other workable strategies. Caregiver training held in preclinical dental education laboratories offers excellent hands-on learning opportunities for both caregivers and OHP students. It is a valuable learning experience for students as they coach caregivers while they practice positioning, opening a closed mouth, or using specialized products on realistic compliant “elders” (Fig. 19.5).

Figure 19.5 Tailor content to participants needs based on their role in supporting oral health in long-term care. Photographs depict training using a preclinical dental laboratory and reusable product kits. Created by Wener, Bertone, and Yakiwchuk, 2012.
The train-the-trainer (TTT) model is particularly suitable when implementing caregiver education and training at larger facilities or across health regions, given its cost-effective collaborative approach that can serve to establish numerous champions and partners. Speech language pathologists in our region attended our 2-hour TTT didactic and hands-on practice session then proceeded to train caregivers at each of the personal care homes where they worked, using a simplified training CD we provided. On-going involvement from an OHP expert as the trainer or a consultant is essential to ensure disseminated information is up-to-date and trainers remain mindful to avoid decision making beyond their knowledge base and scope of practice.
Content
Passionate OHPs can often overload caregivers by providing too much information, while neglecting to incorporate interactive learning activities that help facilitate knowledge translation, trust, and commitment. Avoid this pitfall by clearly identifying the target group’s oral healthcare role, what key pieces of information and skills they will need to do their job better, and how to engage them in meaningful dialogue before developing your presentation. For a family member, include a discussion on the importance of mouth care based on the individual’s medical conditions and risk factors. Support their daily efforts by providing them with an individualized mouth care plan that identifies helpful products, and coaching them as they practice this new skill.
For LTC stakeholders, begin with a strong introduction about the silent oral disease epidemic in care facilities. Highlight some of the issues and barriers faced by caregivers, residents, and others. Provide the “why” before the “how to” of mouth care to raise awareness of how effective daily care can help prevent dental diseases, infections, pain, and systemic illness such as pneumonia. This information serves to “reconnect the mouth to the body” and provides concrete evidence to support a comprehensive oral healthcare program.
For administrators and others not involved in daily mouth care, add information on existing oral health guidelines and standards, the role OHPs and other champions can play, accessing professional dental care, and ordering effective oral health products. Drawing parallels between an oral care program and other successfully integrated programs, such as wound care, could provide the vision and push needed to operationalize oral healthcare (McNally et al., 2012). Regardless of the stakeholder’s role, everyone should be aware of the key components of a comprehensive oral care program, such as the need for regular caregiver education and training, having oral care supplies on hand, oral screening, daily oral care, and on-site professional dental and dental hygiene ca/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


