Chapter 19 Mycobacteria and legionellae
Mycobacteria
Mycobacterium tuberculosis
Culture and identification
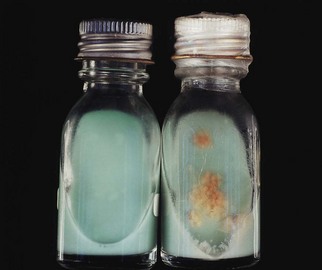
This species does not grow on ordinary media and requires Löwenstein–Jensen medium for growth (constituents: whole egg, asparagine, glycerol, malachite green). Slow-growing (2–3 weeks; sometimes up to 6 weeks) at 37°C. They grow as ‘rough, tough and buff’ colonies – rough due to dry, irregular growth; tough due to difficulty in lifting the colony from the surface; and buff due to the pale yellow colour (Fig. 19.1).
Pathogenicity
This organism is the agent of tuberculosis, a chronic, granulomatous, slowly progressive infection, usually of the lungs; eventually, many other organs and tissues may be affected. A pandemic disease, tuberculosis is especially common in the developing world owing to HIV infection (15–20% of individuals with HIV disease may have tuberculosis). The oral cavity is affected secondary to primary disease elsewhere (see Chapter 35). The hallmark of the disease is granuloma formation and caseation mediated by cellular immunity. No exotoxins or endotoxins.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses