CHAPTER 18 THE USE OF COMPUTERIZED TREATMENT PLANNING AND A CUSTOMIZED SURGICAL TEMPLATE TO ACHIEVE OPTIMAL IMPLANT PLACEMENT
AN INTRODUCTION TO GUIDED IMPLANT SURGERY
Successful prosthetic dental rehabilitation depends on detailed planning that takes into account both anatomical limitations and restorative goals. That planning must be accurately transferred to the surgical field. To facilitate that task, the use of surgical guides has become well established in implant dentistry.1–7
Over the years, a variety of approaches to implant surgical-guide fabrication have developed. Attention has focused on the results that can be achieved by combining computed tomography (CT) diagnostic scanning with computer-aided design and manufacturing (CAD/CAM) and rapid prototyping. Studies by Ganz8–12 have suggested that the use of such technology can improve the outcome of implant placement by helping to ensure that the implant is placed in the best bone volume. The accuracy of these techniques has been confirmed by other research.13,14
 Case Report: Using the Guided Surgery Approach
Case Report: Using the Guided Surgery Approach
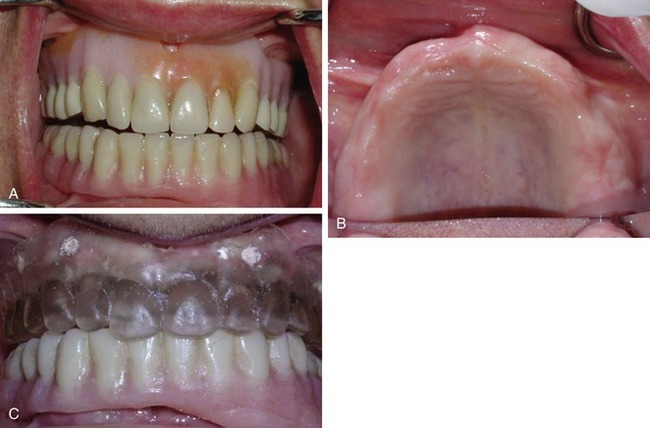
A 56-year-old female patient presented who had been fully edentulous for a number of years. Her mandible had been restored with four implants and a bar-supported over-denture. Tired of the instability of her removable maxillary denture (Figure 18-1, A), she sought an implant-supported solution.
Clinical examination of the edentulous arch (Figure 18-1, B) revealed a thick, healthy ridge. The tissue firmness and tone were ideal, with no preprosthetic surgery indicated. The patient was advised that she appeared to be an ideal candidate for Teeth In An Hour (Nobel Biocare). This is the treatment option the patient chose.
The patient’s dental aesthetics were evaluated, and it was decided to modify her existing denture, adjusting the contours and relining the intaglio surface with a soft-line material to achieve an intimate fit with her soft tissue. Because of the soft lining, it was necessary to duplicate the optimized denture in hard clear acrylic. (The exact thickness of the gingival and palatal tissue cannot be identified precisely with a soft-lined prosthesis.) Ten gutta percha radiographic markers were added to the clear acrylic denture (see Figure 18-1, C).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses