The periapical tissues
Normal radiographic appearances
A reminder of the complex three-dimensional anatomy of the hard tissues surrounding the teeth in the maxilla and mandible, which contribute to the two-dimensional periapical radiographic image, is given in Fig. 18.1.
The periapical tissues of permanent teeth
The three most important features to observe are:
• The radiolucent line that represents the periodontal ligament space and forms a thin continuous black line around the root outline
• The radiopaque line that represents the lamina dura of the bony socket and forms a thin, continuous, white line adjacent to the black line
• The trabecular pattern and density of the surrounding bone:
Important points to note
• There is considerable variation in the definition and pattern of these features from one patient to another and from one area of the jaws to another, owing to variation in the density, shape and thickness of the surrounding bone.
• The limitations imposed by contrast, resolution and superimposition can make radiographic identification of these features particularly difficult, hence the need for ideal viewing conditions and digital image enhancement software.
The effects of normal superimposed shadows
Radiolucent shadows
• The radiolucent line of the periodontal ligament may appear MORE radiolucent or widened, but will still be continuous and well demarcated.
• The radiopaque line of the lamina dura may appear LESS obvious and may not be visible.
• There will be an area of radiolucency in the alveolar bone at the tooth apex (see Figs 18.5 and 18.6).
• The fact that the radiopaque lamina dura shadow may not be visible does not mean that the bony socket margin is not present clinically. It only means that there is now not enough total bone in the path of the X-ray beam to produce a visible opaque shadow. Since the bony socket is in fact intact, it still defines the periodontal ligament space. Thus, the radiolucent line representing this space still appears continuous and well demarcated.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


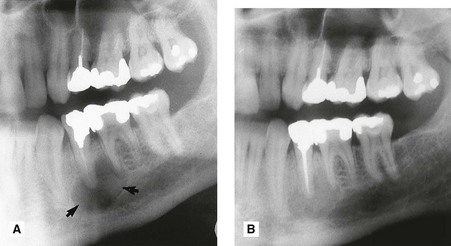
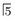 . B Same patient 6 months later following successful root filling at
. B Same patient 6 months later following successful root filling at 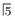 . Note the bony fill-in in the apical area.
. Note the bony fill-in in the apical area.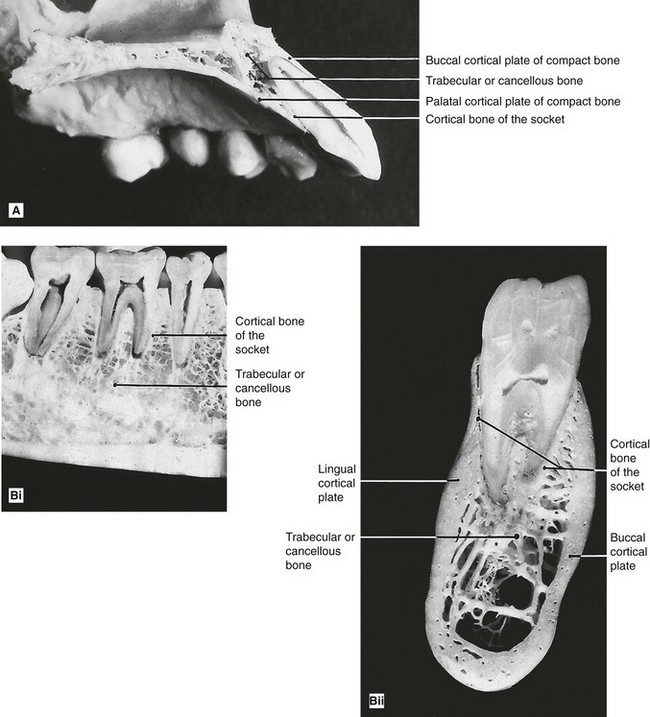
 , B
, B  , C
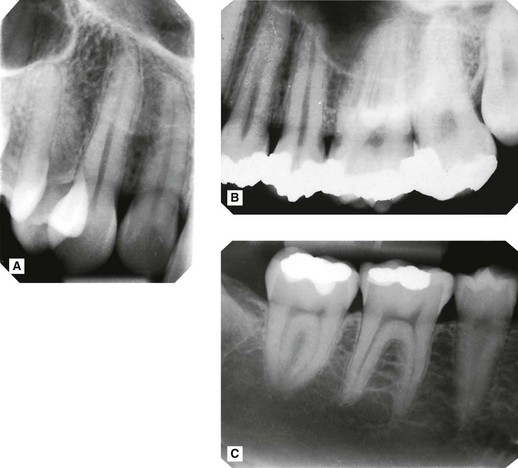
, C  showing the normal radiographic anatomy of the periapical tissues in different parts of the jaws. Note the continuous radiolucent line of the periodontal ligament shadow and the radiopaque line of the lamina dura outlining the roots.
showing the normal radiographic anatomy of the periapical tissues in different parts of the jaws. Note the continuous radiolucent line of the periodontal ligament shadow and the radiopaque line of the lamina dura outlining the roots.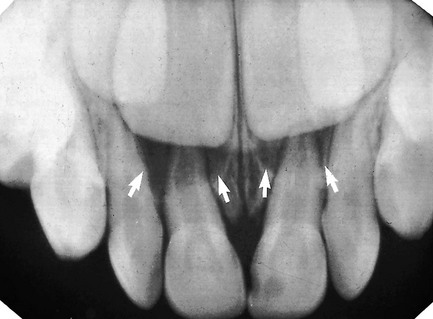
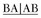 in a 4-year-old child, showing normal periapical tissues. Note the confusing shadows created by the radiopaque crowns and radiolucent crypts (arrowed) of the developing permanent incisors.
in a 4-year-old child, showing normal periapical tissues. Note the confusing shadows created by the radiopaque crowns and radiolucent crypts (arrowed) of the developing permanent incisors.
 , B
, B  . Note the circumscribed areas of radiolucency of the radicular papillae (arrowed) and the funnel-shaped roots.
. Note the circumscribed areas of radiolucency of the radicular papillae (arrowed) and the funnel-shaped roots.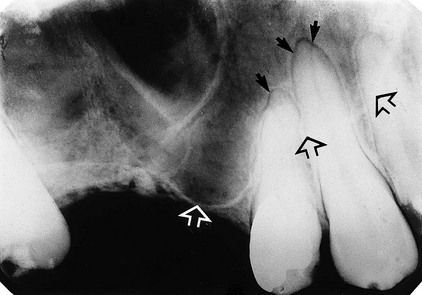
 showing normal healthy apical tissues but with the radiolucent shadow of the antrum superimposed (the antral floor is indicated by the open arrows). As a result the radiolucent line of the periodontal ligament appears widened and more obvious around the apices of the canine and premolar, but it is still well demarcated, while the radiopaque line of the lamina dura is almost invisible (solid arrows).
showing normal healthy apical tissues but with the radiolucent shadow of the antrum superimposed (the antral floor is indicated by the open arrows). As a result the radiolucent line of the periodontal ligament appears widened and more obvious around the apices of the canine and premolar, but it is still well demarcated, while the radiopaque line of the lamina dura is almost invisible (solid arrows).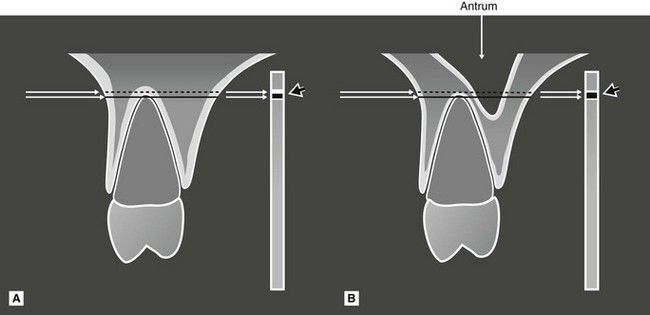
 showing the anatomical tissues that the X-ray beam passes through to reach the image receptor. A Without a normal anatomical cavity superimposed. B With the antral cavity in the path of the X-ray beam. The different resultant radiopaque (white) and radiolucent (black) lines of the apical lamina dura and periodontal ligament are shown on the image receptor (arrowed).
showing the anatomical tissues that the X-ray beam passes through to reach the image receptor. A Without a normal anatomical cavity superimposed. B With the antral cavity in the path of the X-ray beam. The different resultant radiopaque (white) and radiolucent (black) lines of the apical lamina dura and periodontal ligament are shown on the image receptor (arrowed).