Chapter 18
Short-Scar Face-Lift Options
Introduction
Aging, like fashion trends, changes from generation to generation. In just one generation, today’s aging society is significantly different from that of their immediate forefathers. Aging Americans are living longer, working longer, exercising longer, sexually active longer, and looking younger longer than the previous generation. This current age group, sometimes labeled as the baby boomers, has taken better care of their health and has embraced diet, exercise, and aesthetic interventions that have allowed them to age more gracefully and more youthfully.
More than ever, today’s average patient seeking facial rejuvenation desires more limited procedures, minimal risks, a rapid return to usual activities, and a natural, “nonplasticized” look. Patients will often demonstrate their desires for aesthetic improvement by lifting their cheeks upwards vertically toward the crown of the head, a maneuver they have repeated many times in the mirror prior to presenting for consultation (Figure 18.1). It is important to remember that there is no surgical procedure more elective than face-lift surgery. Consequently, cosmetic surgeons must continually strive to maximize results while, at the same time, minimizing complications and postoperative recovery. Patients’ wishes, as outlined above, may not always be shared by all cosmetic surgeons, many of whom often prefer a more aggressive surgical facial rejuvenation program. Recent reports of serious sequelae or even death associated with face-lift surgeries have patients questioning the value of aggressive face-lifts and lengthy anesthesia.1
Figure 18.1 Patient demonstrating her aesthetic desires. Note the primarily vertical vector of this mock rejuvenation lifting.

As early as 1919, Passot reported a technique of short-scar rhytidectomy.2 A significant advancement in face-lifting resulted from the discovery of the superficial musculoaponeurotic system (SMAS) by Mitz and Peyronie.3 The application of SMAS suspension to face-lifting by Skoog truly revolutionized the procedure.4 Hamra eloquently described the highly sophisticated and technically challenging “composite rhytidectomy” in 1992, encouraging a trend toward more aggressive, lengthier multiplanar procedures.5 Perhaps not surprisingly, a concomitant increase in facial nerve injuries and dyskinesias were noted precipitating Seckel’s 1994 publication, Facial Danger Zones: Avoiding Nerve Injury in Facial Plastic Surgery.6
Seckel is both a neurologist and a plastic surgeon and a particular expert on facial nerve injuries. He notes in the preface of his book that he had been referred three face-lift-related facial nerve injuries in 1 month, two following “composite” rhytidoplasty. Seckel further stated that,
With today’s more aggressive and deeper facial dissection in the course of the face-lift surgery, the peripheral nerves of the face are more often exposed, lie closer to the plane of dissection, and in my opinion are more likely to be injured. Injury to one of the major facial nerve branches creates a catastrophe and occasionally irreversible facial deformity. Even patients who do recover muscle function following injury are often left with permanent involuntary muscle twitching or distortion of the normal facial expression by contracture and shortening of partially denervated muscles. Additionally, interruption of one of the major sensory nerves in the face can result in permanent disability secondary to numbness or, worse, intractable dysesthesia and pain.
6
In my opinion, with the timing of Seckel’s book, the swing of the pendulum toward more aggressive face-lifting had reached it pinnacle and was entering a decline brought on by public dissatisfaction on the adverse events associated with these procedures. Enter the S-lift, a short-scar, short-flap face-lift technique reintroduced by Saylan in 1999 (Figure 18.2). The S-lift combines the advantages of a limited incision and dissection with the advantages of SMAS lifting and manipulation. Saylan’s original contribution to the technique involves the effective use of “U”- and “O”-shaped purse-string sutures to suspend the mobile SMAS and the platysma SMAS to the fixed periosteum and fascia of the zygomatic arch7 (Figure 18.3).
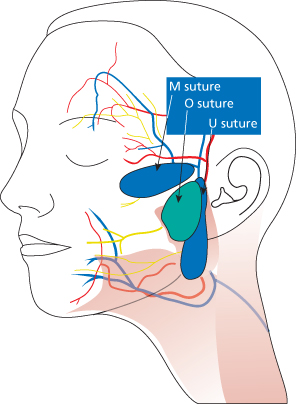
Figure 18.2 S-lift incision demonstrating three key advancement closure points: A–A1, B–B1, C–C1.
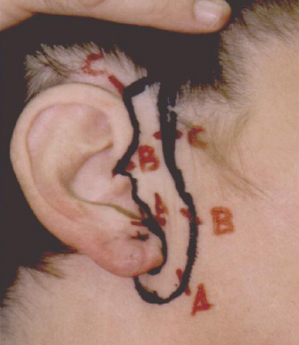
Figure 18.3 Diagrammatic depiction of U, O, and M purse-string sutures.
The “short-scar face-lift” series, referenced by this author as the S-lift rhytidectomies, is a conceptually new approach to face-lifting and is particularly applicable to younger patients and patients requiring secondary face-lifts (Table 18.1). It is important to note that the S-lift is not a simple “mini lift” skin excision, but is rather an advanced “SMAS” multiplanar rhytidectomy. The S-Plus lift combines aspects of the technique of lateral SMASectomy described by Baker8 and malar fat pad suspension utilizing a purse-string suture, suspending the ptotic malar fat pad from the temporalis fascia (M suture), described by Tonnard et al.9 (Figure 18.4).
Table 18.1 Clinical indications for S-lift rhytidectomies
| Clinical findings | Procedure |
| Mild—moderate neck laxity, mild—moderate jowling | S-lift (short flap) |
| Moderate—severe neck laxity, moderate—severe jowling, | S-Plus lift |
| Moderate, severe midface laxity | |
| Mental and/or malar insufficiency | Add chin and/or cheek implants |
| Platysma banding at rest | Add midline platysmaplasty |
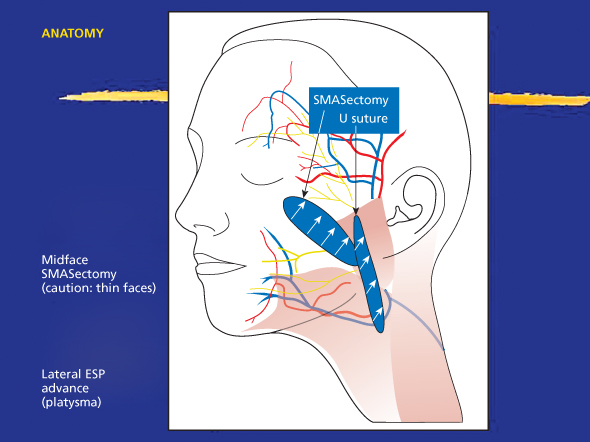
Figure 18.4 S-Plus lift with a diagram of U suture and SMASectomy. ESP: extended SMAS platysma.
The S-Plus lift extends the efficacy of the S-lift in those patients who have significant midfacial ptosis. The aesthetic effectiveness of extended SMAS face-lifts and their equality to composite rhytidectomies has been documented.10
The S-lift is generally a “short-flap” face-lift procedure, whereas the S-Plus lift, with its midface extension, is a “long-flap” rhytidectomy. Finally, the S-lift with implants (also referred to by this author as the “contour lift”) is indicated for patients with both facial laxity and volume deficiencies in the malar and mental areas. Combining the S-lift with alloplastic facial implants can give significantly improved long-term aesthetic results to patients with volume inadequacies.
The S-lift is indicated for patients with mild to moderate neck laxity and jowling (Figure 18.5). The S-Plus lift is indicated for patients with moderate to severe neck laxity and jowling (Figure 18.6). Patients with poor facial structure are best suited for a contour lift, which is an S-lift with alloplastic implants (Figure 18.7). Patients with platysmal banding at rest are candidates for the S-lift with midline platysmaplasty (Figure 18.8).
Figure 18.5 S-lift candidate with mild to moderate neck laxity, and mild to moderate jowling.
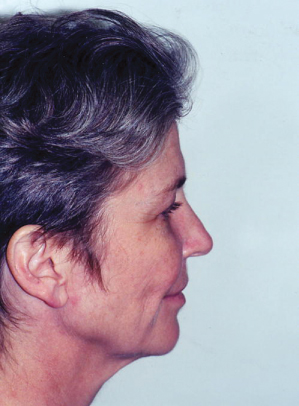
Figure 18.6 S-Plus lift candidate with moderate neck laxity, moderate to severe jowling, and midface laxity.
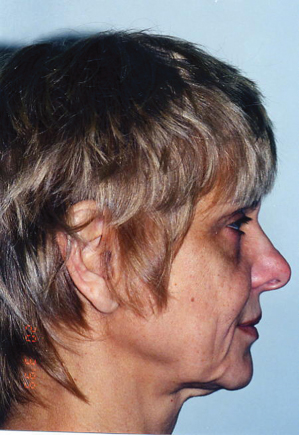
Figure 18.7 Contour lift (S-lift with alloplastic implants) candidate with malar and mental insufficiencies.
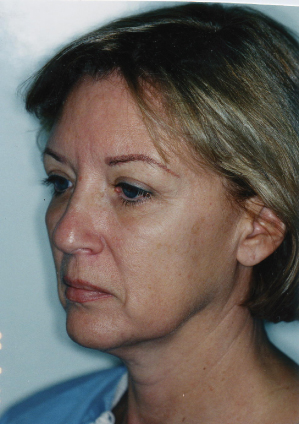
Figure 18.8 Platysma banding at rest. Good candidate for S-lift with midline platysmaplasty.
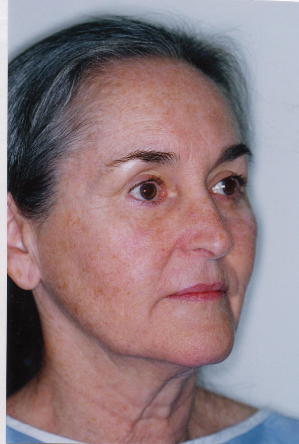
The Advantages of S-Lift Rhytidectomies
Limited incisions means limited scarring. Preauricular scars generally heal more favorably than postauricular and occipital scars. The S-lift is “ponytail friendly” by avoiding the postauricular hairline scar.
The S-lift rejuvenates in a primarily vertical vector. A key factor in aesthetically pleasing results in most patients is vertical rotation and reorientation of the cheek-neck flap. The key tension suture is C–C1 (Figure 18.2) at the superior aspect of the auricle.
The S-lift avoids extensive posterior neck dissection, the anatomical area responsible for many hematomas and injury to the great auricular nerve, the most commonly injured sensory nerve in face-lifting.
The S-lift can provide excellent rejuvenation of the neck and jowl. The U and O purse-string SMAS placation or imbrication sutures allow an excellent “block and tackle” lifting of these structures. The purse-string sutures to the rigidly fixed ligamentous structures of the zygomatic arch maneuver the SMAS more vertically.
The S-lift procedures required less surgical and anesthesia time compared with the more classic or multiplanar face-lift. There is more than a little bit of truth in the old surgical adage that shorter anesthesia times are associated with fewer complications. Reduced operating time also allows the cosmetic surgeon the luxury of adding other complementary procedures that can often significantly enhance aesthetic outcomes. For example, endoscopic or minimal incision brow lift, blepharoplasty, cheek or chin augmentation, and fat transfers to name a few.
The S-lift is an SMAS face-lift. It is not just a “skin lift” as some detractors would suggest. The U, O, and M sutures are SMAS plication sutures that effectively advance and tighten this fascial system. The SMASectomy resection and closure in the S-Plus lift represents a true SMAS imbrication. Indeed, one can even accomplish a “deep-plane,” composite lift through the limited S-lift incision. The possibilities are limited only by the imagination.
The S-lift is generally associated with a shorter recovery period. Shorter scars and certainly shorter flaps mean less bruising, less edema, and faster return to normal social activities.
The Disadvantages of S-Lift Rhytidectomies
The S-lift gives limited direct visibility to the neck. Surgical exposure to the poster neck is compromised compared with the classical rhytidectomy approaches. The novice surgeon might be bothered by such limited exposure and the resultant difficulties with instrumentation. By extending the S-lift incision 1–2 cm postauricularly, direct visualization of the posterior, inferior, and anterior neck structures can be much improved.
The S-lift can result in a posterior “dog ear” the can last 1–3 months and that may require revision surgery. There are techniques to help minimize this postoperative sequelae including wide undermining of the short postauricular limb of the incision, liposculpture of the posterior neck, and closing from posterior to anterior utilizing the technique of “halfing” the unequal length flaps with interrupted skin mattress sutures that also incorporate the deeper facial tissues.
Some patients can experience pain over the zygomatic arch secondary to the O and U suture knots. Triamcinolone acetonide injections have been helpful in resolving this problem, but often, the suture knot needs to be removed. The patient can palpate the suture knot as well, and in a few instances the knot has actually extruded through the skin. The author recommends using a 2-0 dissolvable suture made of braided polyglactin 910 rather than permanent suture material.
Surgical Technique
The facial markings are made in the upright position with the patient observing while holding a hand mirror. The platysma muscle is delineated first after asking the patient to clench his or her teeth. Knowing the position of the anterior and posterior edges/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


