Reconstruction of the Nose
Introduction
During the last decade, reconstruction of the nose has reached a high level of sophistication with enhancement of aesthetic results.1–3 This has been achieved by emphasizing the necessity of replacing surgically ablated tissue with like tissue. Skin is replaced with skin that matches in color and texture as closely as possible. Cartilage and bone are replaced, and mucosa is used to replace any loss of the nasal lining. The concept of nasal aesthetic units has emerged with an emphasis on replacing the skin of an entire unit if the majority of the skin is missing. Another important concept that has led to enhancement in the results of restorative surgery has been the emphasis on the placement of incisions for local flaps along borders of aesthetic regions or units to maximize camouflage of scars. Whenever possible, local flaps are designed so that they are not transferred across the borders of aesthetic regions, particularly if the border has a concave topography. An example of such a border is the alar-facial sulcus, which represents a concave border between three aesthetic facial regions: the nose, the cheek, and the upper lip.4,5
Topographic Analysis
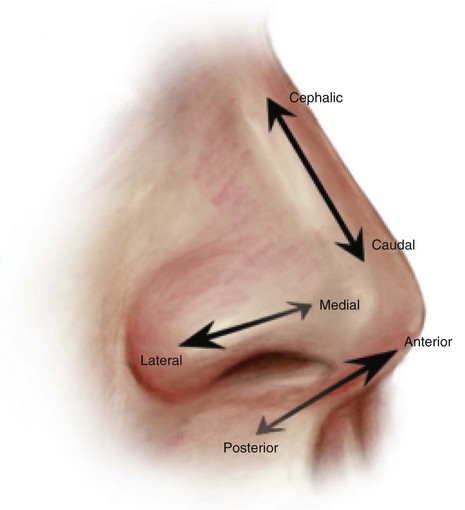
The aesthetic proportions of the ideal nasal shape and size have been established. On the lateral view, the distance from the vermilion border of the upper lip to the subnasale is equal to the distance from the subnasale to the pronasale.6 The distance from the alar-facial sulcus to the midpoint of the nares ideally equals that from the midpoint to the caudal edge of the nasal tip. On the lateral view, a right-angle triangle with the ratios of its sides being 3 : 4 : 5 and the vertices being at the nasion, alar-facial sulcus, and tip has been described to illustrate the ideal nasal proportions and size.7 Figure 18-1 illustrates the standard directional nomenclature.
Facial Aesthetic Regions
The face can be divided into topographic regions, each with its individual intrinsic characteristics of skin color, texture, contour, and hair growth.5 Each has an individual shape created by the underlying facial skeleton. The nose is one of the aesthetic regions of the face and may be divided into several aesthetic units (Fig. 18-2). Each unit may be proportionally overdeveloped or underdeveloped relative to other noses, but there is a consistent general configuration from nose to nose. There are nine aesthetic units of the nose identified by distinctive convex or concave surfaces, including the nasal tip (lobule), dorsum, paired sidewalls, paired alae, paired soft tissue facets, and columella. In general, the shape of the tip is determined by the size and contour of the alar cartilages and specifically by the domal portion of the nasal cartilages. It is covered by relatively thick skin containing many sebaceous glands (sebaceous skin). Each dome causes a point of reflected light. Above the tip is a supratip depression that separates the tip from the dorsum. The skin of the dorsum tends to be less thick and sebaceous than the skin of the tip, becoming progressively thinner as it ascends to the rhinion and thickening again as it approaches the glabella. The nasal bones together with the upper lateral cartilages and cartilaginous septum provide skeletal support for the dorsum. The lateral borders of the dorsum are defined by the lateral shoulders of the upper lateral cartilages and the junction of the nasal bones with the frontal processes of the maxillae. These structures separate the dorsum from the sidewalls and create a line of reflected light and shadows separating the lateral walls from the dorsum. The nasal sidewalls are most often a combination of convex and concave elements extending laterally from the dorsum to the junction of the nose with the cheek. Structurally, the sidewalls are supported by the lateral extensions of the nasal bones and upper lateral cartilages and the medial extension of the frontal processes of the maxillae. The skin of the sidewalls is thin and contains fewer sebaceous glands than that of the dorsum and tip; it is separated from the ala by the alar groove, which is the deepest contour line of the nose. This groove is continuous laterally with the alar-facial sulcus, and together they circle the alae, delineating them from the tip, sidewalls, and cheeks. The alar unit itself is a smooth bulge reflecting a single spot of light and is covered with thick skin similar in texture and porosity to the skin of the tip. The structural support of the ala is provided by thick fibrofatty tissue that does not contain cartilage.
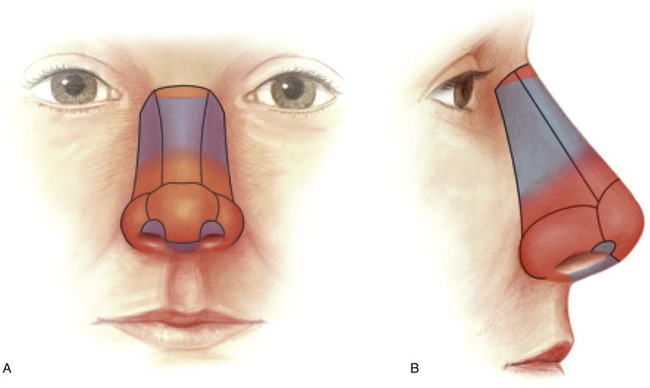
FIGURE 18-2 A, B, Aesthetic units of nose. Blue represents thin-skinned regions; red represents regions of thicker skin. (From Jewett BS: Anatomic considerations. In Baker SR, editor: Principles of nasal reconstruction, ed 2, New York, Springer, 2011.)
Menik has stressed that the goal of restorative nasal surgery is not simply to fill a defect.2 Depending on the extent of the defect, wounds should be altered in size, configuration, and depth to allow reconstruction of an entire unit. If the majority of the surface area of a unit is lost, resurfacing of the entire unit is usually preferable. This is accomplished by discarding the remaining skin of the unit and designing the covering flap so it will compensate for the discarded skin. This arrangement places scars at the junction between units, where they will lie in depressions or along shadow lines, maximizing scar camouflage. In these junctions, scars blend with normal contour lines of the nose and distract the viewing eye. Resurfacing of an entire aesthetic unit causes a mild trap-door scar contraction phenomenon, which in turn causes the entire unit to bulge slightly, simulating the normal convexity of the tip and alae.2 The columella, dorsum, and sidewalls are not convex, and I do not routinely resurface the entire surface of these aesthetic units when defects occupy more than half of their entire surface area.
An aesthetic nasal unit that is to be entirely resurfaced is covered with a flap that exactly duplicates its surface area and pattern whenever possible. A fresh wound is always enlarged by retraction of its margins; thus, the contralateral unit should be used to design covering flaps. If the contralateral counterpart is missing or a unit does not have a matching pair, a template replicating the ideal unit size for that specific patient is used. The nose is a three-dimensional structure and reconstruction of each unit must duplicate the normal contour. This is accomplished by concomitantly integrating structural support in each step of the repair. Reconstructed skeletal elements are attached to a stable foundation, such as remaining nasal cartilages or the bone of the maxilla, to prevent collapse or distortion of the unit during the healing process.2 Within the defect, the constructed skeletal structures are designed to completely span the defect. This is accomplished before wound healing to prevent distortion from scar contraction during the healing process.
Lining Flaps
The vascular supply to the internal nose is shown in Figure 18-3. On the basis of the vascular anatomy, Burget and Menik have demonstrated that the entire ipsilateral septal mucoperichondrium can be transferred with a narrow pedicle containing the septal branch of the superior labial artery.1 Likewise, the entire contralateral mucoperichondrium can be turned laterally as a dorsally based hinge flap based on the anterior and posterior ethmoid arteries to line the sidewall of the nose.1 Burget and Menik have also shown that if both right and left septal branches are included in the pedicle, the entire septum can be rotated out of the nasal passage as a composite flap containing a sandwich of cartilage between the two mucoperichondrial leaves.1 Such flaps, whether they are composite or simple mucoperichondrial hinge flaps, can be designed to extend from the floor of the nose to within 1 cm of the junction of the upper lateral cartilage and cartilaginous septum. The flaps may extend posteriorly well beyond the bone-cartilage junction of the septum, producing a hinged mucosal flap measuring as much as 3 cm wide and 5 cm long.1 Burget and Menik advocate a back cut of the mucosa in the area of the anterior septal angle to facilitate flap transfer.3 I prefer to leave the flap hinged on the entire length of caudal septum to maintain a wider pedicle and to enhance the vascularity of the flap. These authors have also described a bipedicle flap of vestibular skin and mucosa based medially on the septum and laterally on the floor of the nasal vestibule. Such a flap may be elevated away from the undersurface of the lateral crus and mobilized inferiorly to reline alar defects. All of these lining flaps have a reliable vascularity and are thin and supple, providing natural physiologic material for the interior of the nasal passage.
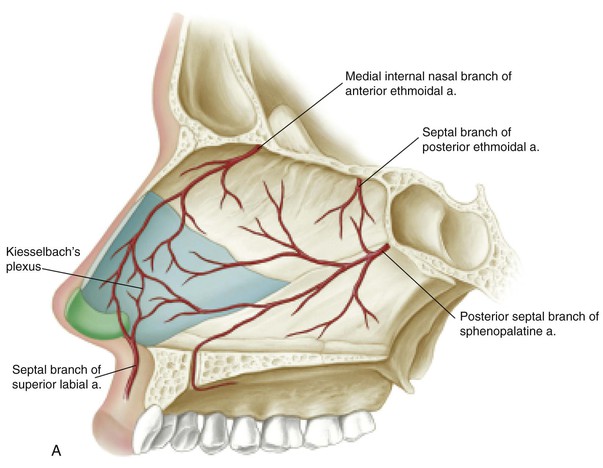
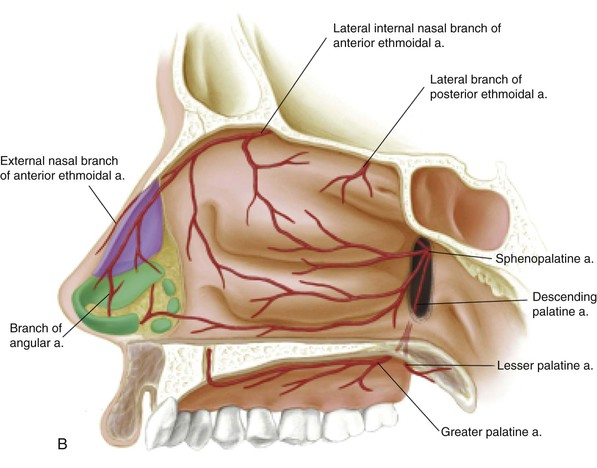
FIGURE 18-3 Arterial blood supply of left septum (A) and right lateral wall (B) of nasal cavity. (From Jewett BS: Anatomic considerations. In Baker SR, editor: Principles of nasal reconstruction, ed 2, New York, Springer, 2011.)
Bipedicle Vestibular Skin Advancement Flap
Lining for full-thickness alar or unilateral tip defects that have a vertical dimension (caudal to cephalic) of 1.0 cm or less can be provided by the thin skin of the remaining nasal vestibule. Defects with vertical dimensions as large as 1.5 cm may sometimes be lined by this method if the remaining skin of the lower nasal vault is of sufficient size. Before the bipedicle flap is created, the vertical height of the remaining vestibular skin is measured to ensure that there will be sufficient width for the flap to cover the lining defect. An extended intercartilaginous incision is made between the lateral crus and caudal aspect of the upper lateral cartilage. The incision extends from the anterior septal angle to the most lateral aspect of the floor of the vestibule. The remaining vestibular skin is then mobilized caudally in the form of a bipedicle advancement flap by elevating it away from the overlying lateral crus (Fig. 18-4).8 Dissection of the flap is assisted by hydrodissection, accomplished by infiltrating the subdermal plane with an anesthetic solution of lidocaine containing epinephrine. Mobilization is continued until the caudal border of the flap can be easily positioned without tension 1- to 2-mm below the caudal margin of the lining defect. To accomplish this, it is occasionally necessary to extend the intercartilaginous incision inferomedially from the anterior septal angle toward the membranous septum.
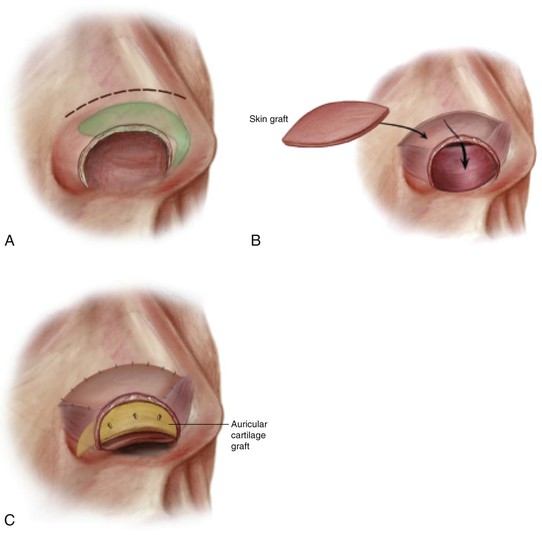
FIGURE 18-4 A, Bipedicle vestibular skin advancement flap created by making an intercartilaginous incision between upper and lower lateral cartilages. B, Flap mobilized sufficiently to allow caudal border to reach nostril margin. Thin full-thickness skin graft used to repair flap donor site. C, Auricular cartilage graft provides framework for nostril margin. Lining flap secured to cartilage graft with mattress sutures. (From Baker SR: Internal lining. In Baker SR, editor: Principles of nasal reconstruction, ed 2, New York, Springer, 2011.)
The bipedicle vestibular skin advancement flap consists only of skin. The overlying alar cartilage and fibrofatty tissue of the ala are left intact. As the flap is advanced caudally, redundancy occurs near the caudal aspects of the medial and lateral pedicles. This represents the standing cutaneous deformities that form with all advancement flaps. The tissue redundancy should not be trimmed because it will dissipate during wound healing. In the case of full-thickness defects that extend through the margin of the nostril, the flap is positioned so that the caudal border extends 1- to 1.5-mm below the inferior aspect of the framework used to reinforce the nostril margin. This enables the inferior border of the covering flap to be sutured to the vestibular skin flap, restoring the delicate nostril margin. When the lining defect does not extend through the nostril margin, the caudal border of the flap is sutured to the caudal border of the lining defect. Structural support for the flap is provided by septal or auricular cartilage grafts. The flap is suspended to the overlying cartilage grafts with 5-0 polydioxanone sutures (see Fig. 18-4). The sutures pass from the external surface of the cartilage graft, through cartilage and flap, and back through the flap and overlying cartilage. Three or four loosely tied sutures are usually required to support the flap and to suspend it completely to the framework. The number of sutures is limited to minimize risk of vascular impairment of the flap. The donor site of the flap is repaired with a thin full-thickness skin graft. If an interpolated cheek flap is used for covering, the standing cutaneous deformity that forms along the inferior aspect of the medial cheek during primary closure of the cheek donor site becomes the source of the skin graft.
Ipsilateral Septal Mucoperichondrial Hinge Flap
In general, the septal mucoperichondrial hinge flap should be designed as large as possible. Large flaps measuring 4.0 to 4.5 cm in length and 2.5 to 3.0 cm in width can provide sufficient mucoperichondrium to line the entire lower nasal vault and limited portions of the caudal aspect of the middle vault. A solution of lidocaine containing epinephrine is infiltrated in the subperichondrial plane along the entire length of the septum. Two horizontal incisions extending from anterior to posterior are made with a scalpel on an extended handle (Fig. 18-5). The dorsal incision begins 0.75 cm posterior to the anterior septal angle and extends along a line 0.5 to 1.0 cm below the roof of the middle vault. It should extend 1 to 2 cm posterior to the bone-cartilage junction of the septum. The inferior incision starts 1.0 cm posterior to the anterior nasal spine and usually extends along the junction of the nasal crest and the floor of the nose. The incision should extend as far posteriorly as the dorsal incision. A posterior vertical incision is then made between the ends of the dorsal and inferior septal incisions. This is accomplished with a right-angled scalpel. A No. 66 Beaver eye blade is useful for this purpose.
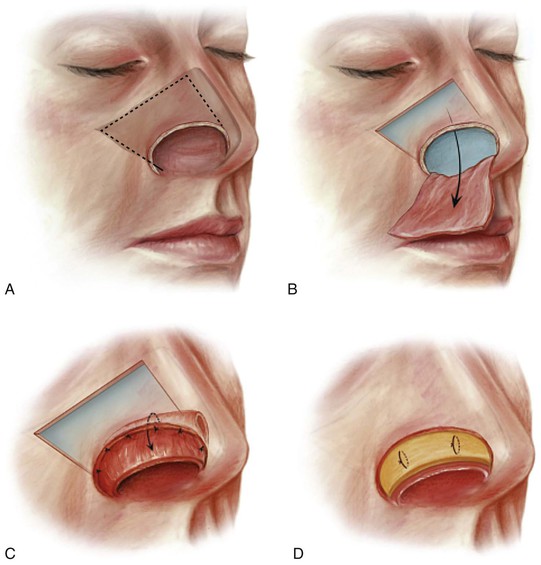
FIGURE 18-5 A, Unipedicle septal mucoperichondrial hinge flap developed by incising through mucosa and perichondrium along floor of nose and 1.5 cm below and parallel to cartilaginous dorsum. Incisions extend posteriorly beyond septal bony cartilaginous junction. B, Flap dissected from superior to inferior and anterior to posterior. Anterior dissection remains 1 cm posterior to caudal border of septum and 1.5 cm posterior to nasal spine. Flap based on intact mucoperichondrium of caudal septum and septal branch of superior labial artery. C, Hinged on caudal septum, flap is reflected laterally to line lower nasal vault. D, Cartilage graft provides nasal framework. Lining flap secured to framework with mattress sutures. (From Baker SR: Internal lining. In Baker SR, editor: Principles of nasal reconstruction, ed 2, New York, Springer, 2011.)
Bilateral Caudally Based Septal Mucoperichondrial Hinge Flaps
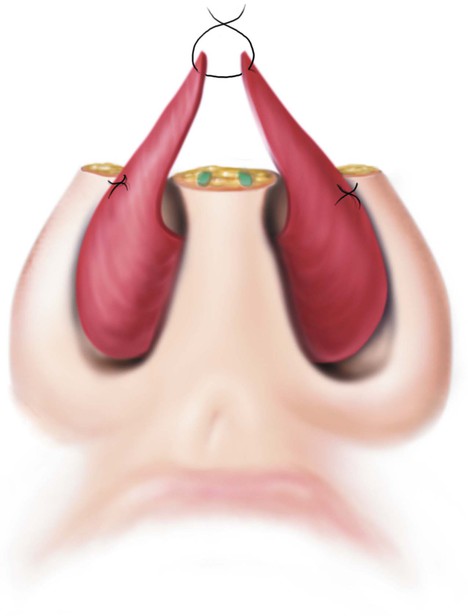
A septal mucoperichondrial hinge flap based on the caudal septum may be developed bilaterally (Fig. 18-6). Concurrent bilateral flaps preclude the use of a dorsally based septal mucoperichondrial hinge flap for repair of more cephalically located lining deficits. Bilateral flaps are indicated when a full-thickness defect of the entire nasal tip is present but with an intact columella. In this situation, each flap provides lining for the ipsilateral hemi-tip and any portions of the adjacent ala that may be absent. The flaps are designed, incised, and dissected in a fashion identical to the methods for a unilateral flap. The exposed septal cartilage is removed, leaving a permanent septal perforation as bilateral resurfacing of the cartilage by secondary intention healing is unlikely. A 1.5-cm-wide dorsal and caudal strut of septal cartilage is maintained for proper support of the nasal bridge. Each flap is turned laterally and anteriorly in a hinged fashion with the raw surface of the mucoperichondrium turned outward. The flaps are sutured to their respective lining defects and suspended to a framework of cartilage grafts used to restore the structure and topography of the nasal tip and any portions of the alae that may be missing.
Contralateral Dorsal Septal Mucoperichondrial Hinge Flap
A mucoperichondrium hinge flap harvested from the side opposite the nasal defect and based on the nasal dorsum may be turned laterally to resurface the roof and lateral wall of the middle vault of the nose (Fig. 18-7).8 The flap may be designed to include all of the mucosa covering the cartilaginous septum, except for the mandatory maintenance of the caudal and dorsal strut of the septum. Similar to the mucoperichondrial flap hinged on the caudal septum, the elevation is facilitated by hydrodissection with a solution of local anesthetic injected beneath the perichondrium. Anterior and posterior vertical incisions are made with a right-angled scalpel. Incisions extend from the floor of the nose to within 1 cm of the nasal dorsum. The incisions are separated by the distance appropriate for the desired width of the flap. The mucoperichondrium is dissected with a Freer elevator as a bipedicle flap attached to the dorsum above and the floor of the nose below. Once the mucoperichondrium has been completely freed from the septal cartilage, it is released from the floor with a scalpel blade attached to an extended handle. The exposed septal cartilage is removed for grafting purposes (Fig. 18-8), leaving adequate dorsal support for the nasal bridge. The flap is reflected laterally across the midline toward the side of the lining defect while maintaining its attachment to the contralateral nasal dorsum. This maneuver turns the raw undersurface of the mucoperichondrium outward, away from the nasal passage. This flap is most commonly combined with an ipsilateral mucoperichondrial flap hinged on the caudal septum. The dorsally based flap passes through the large septal perforation necessitated by the use of the two flaps. The caudal border of the dorsally based flap is sutured to the undersurface of the hinge ipsilateral flap (see Fig. 18-7C). This maneuver seals off the nasal passage from the exterior portion of the nasal defect. A continuous carpet of mucoperichondrium can then be used to nourish an overlying cartilage framework. The flaps are suspended to the framework with mattress sutures so there is intimate contact between the mucoperichondrium and the entire undersurface of the cartilage grafts used for framework.
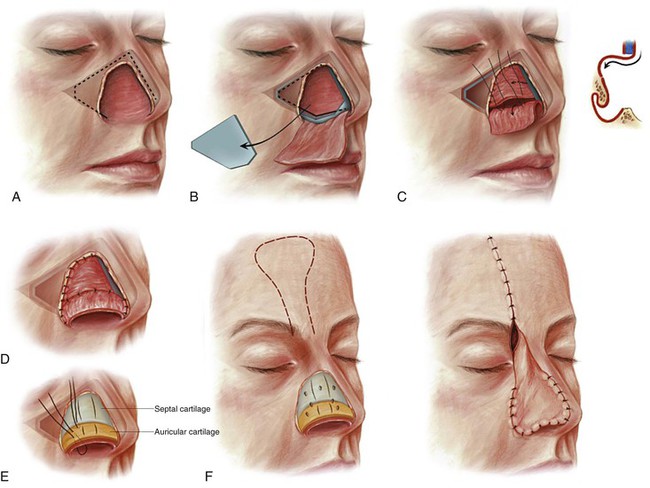
FIGURE 18-7 A, Broken line indicates incision for ipsilateral septal mucoperichondrial flap. B, Flap reflected outward and exposed septal cartilage removed. Broken and solid lines indicate incisions used to create contralateral dorsal septal mucoperichondrial hinge flap. C, Dorsally based flap reflected laterally and sutured to borders of middle vault lining defect. Caudal border of flap sutured to raw surface of ipsilateral flap to seal nasal passage from exterior. D, Caudally based hinge flap provides lining for lower nasal vault; contralateral dorsally based hinge flap provides lining for middle and upper nasal vaults. E, Septal cartilage (blue) provides framework for middle nasal vault; auricular cartilage (yellow) provides framework for lower nasal vault. Cartilage grafts scored to create desired convex contour. Lining flaps attached to framework with mattress sutures. F, Nasal framework covered by paramedian forehead flap. (From Baker SR: Internal lining. In Baker SR, editor: Principles of nasal reconstruction, ed 2, New York, Springer, 2011.)
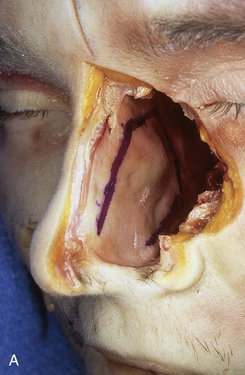
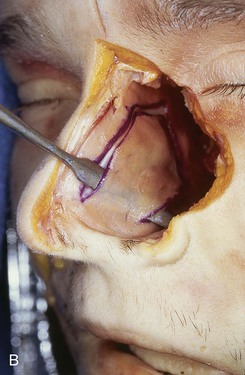
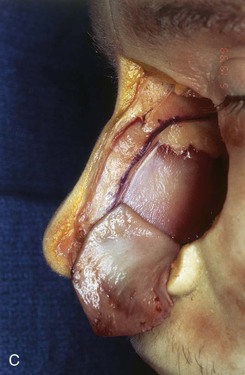
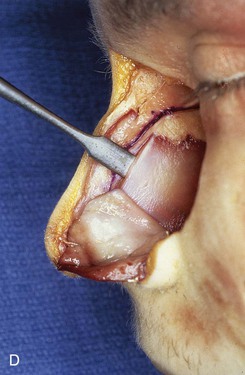
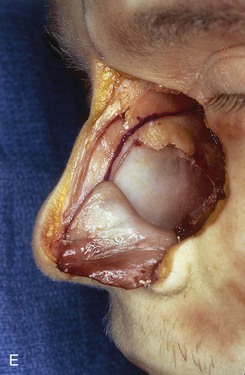
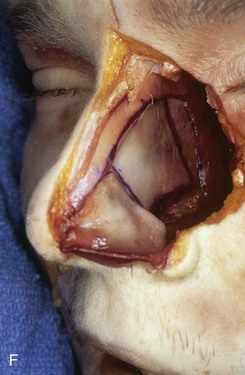
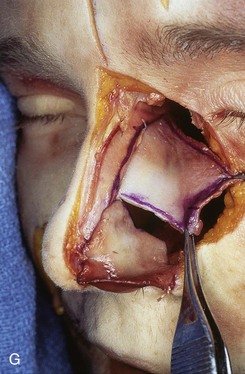
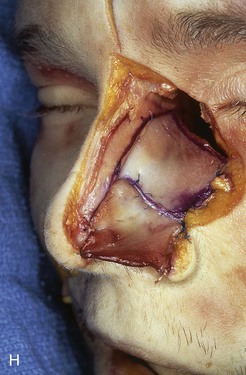
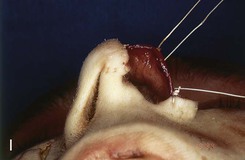
FIGURE 18-8 A, Outline of ipsilateral mucoperichondrial hinge flap. Dorsal incision is parallel and 1 cm below attachment of upper lateral cartilage to nasal septum. Inferior incision extends along junction of nasal crest with cartilaginous septum. B, Flap is elevated in subperichondrial plane from anterior to posterior. C, Mucoperichondrium based on caudal septum is reflected laterally as hinge flap. D, Exposed septal cartilage is freed from contralateral mucoperichondrium. L-shaped strip of septal cartilage 1 to 1.5 cm wide is preserved dorsally and caudally to support middle and lower nasal vaults. E, Septal cartilage removed for grafting purposes. Contralateral mucoperichondrium remains intact. Exposed bony septum may be removed or left in place. F, Contralateral dorsal septal mucoperichondrial hinge flap outlined. The majority of contralateral mucoperichondrium is incorporated in flap. Flap is created by two vertical and one inferior horizontally oriented incisions. G, Flap incised and reflected laterally. H, Flaps sutured in position. Caudal edge of contralateral flap is tacked to exposed raw submucosal surface of ipsilateral flap to seal off nasal passage from exterior. I, Ipsilateral flap is reflected laterally to line lower nasal vault. Suture suspension of flap to overlying cartilaginous framework (not yet in place) restores arc of nasal vestibule. (From Baker SR: Intranasal flaps. In Baker SR, editor: Principles of nasal reconstruction, ed 2, New York, Springer, 2011.)
Septal Composite Chondromucosal Pivotal Flap for the Tip and Columella
When the columella and nasal tip are both missing, a septal composite chondromucosal pivotal flap provides the cartilage necessary for the framework of the columella and the concomitant lining to resurface the area of the membranous septum and nasal domes (Fig. 18-9). The flap is designed with the maximum width possible while still preserving an adequate dorsal septal strut. The flap is extended the entire length of the cartilaginous septum and usually includes portions of the bony septum. Typically, the flap is 3 cm wide and 5 cm long. Bilateral mucoperichondrial flaps are created with a periosteal elevator along the anterior floor of the nose adjacent to the nasal spine. Access to this dissection is through the anteroinferior margin of the defect near the nasal spine. The dissection is extended superiorly over the lateral aspect of the nasal crest until the septal cartilage is encountered.
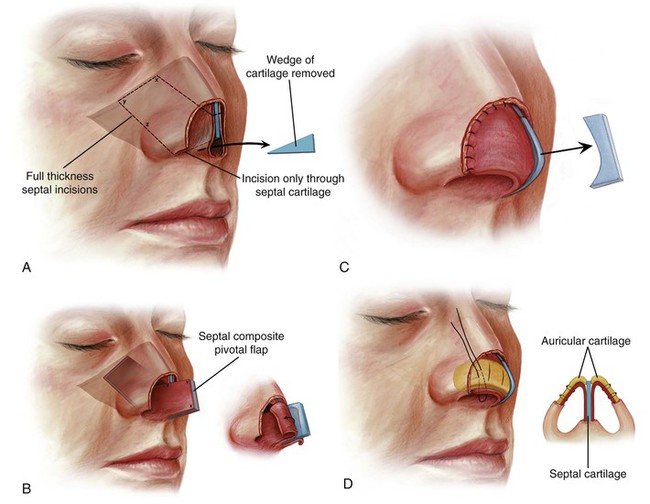
FIGURE 18-9 A, Bold broken line indicates full-thickness incision through septal cartilage, bone, and bilateral mucosa to create composite septal chondromucosal pivotal flap. Faint broken line indicates incision made only through septal cartilage, preserving overlying mucoperichondrium. Wedge of cartilage removed to enable flap to pivot anterocaudally. B, Cephalic aspect of pivotal flap locked into place by abutting it against remaining cartilaginous dorsum. Bilateral mucoperichondrial flaps reflected laterally to provide lining for nasal tip. C, Excess septal cartilage trimmed. Reflected mucoperichondrial flaps sutured to borders of lining defect. D, Auricular cartilage graft (yellow) provides bilateral framework for nasal tip, replacing missing lateral crura. Septal cartilage (blue) of composite flap serves as medial crura for reconstruction. Mucoperichondrial flaps attached to framework with mattress sutures. (From Baker SR: Internal lining. In Baker SR, editor: Principles of nasal reconstruction, ed 2, New York, Springer, 2011.)
A 4-mm-wide osteotome is used to excise a 2-cm-long segment of anterior nasal crest at the pivotal point of the flap while preserving the anterior septal spine. A No. 11 scalpel blade is used to make a full-thickness incision through the cartilaginous septum parallel to and 1.0 cm below the attachments of the upper lateral cartilages to the septum. The incision extends in an anterior direction from the bony perpendicular plate through the exposed margin of the caudal septum. A similar full-thickness incision is made with the same blade along the interface of the cartilaginous septum and the nasal crest, extending anteriorly from the vomer until it is juxtaposed to the previously resected nasal crest. The incision should remain 1.5 cm posterior to the anterior nasal spine to ensure a sufficient vascular pedicle. The pedicle is represented by bilateral mucoperichondrial flaps that are in continuity with the floor of the nose anteriorly and nourished by septal branches of the superior labial arteries.1 A posterior vertical incision is then made to connect the two previously performed parallel horizontal incisions. If the flap extends only to the bone-cartilage junction, the incision is made with a right-angled scalpel; however, it is usually necessary to include bony septum in the flap to achieve adequate flap length. In these instances, the horizontal incisions are extended posteriorly full thickness through the bony septum and the covering mucosa on either side with heavy-duty angled turbinectomy or bone-cutting scissors. It is important to ensure that the superior horizontal incision of the bony septum is completed before an osteotome is used to make the vertical incision through the bony septum so that the force of the osteotome is not transmitted to the region of the cribriform plate.
Once the septal incisions are completed, the composite flap is pivoted 90° on its base in an anterocaudal direction until the inferior border of the flap locks in place, bracing it against the remaining dorsal septal strut (see Fig. 18-9).9 After the flap is positioned, bilateral septal mucoperichondrial hinge flaps are dissected from the distal portion of the flap’s bone and cartilage. The flaps are reflected laterally to provide lining to the nasal domes. Denuded cartilage and bone extending beyond the planned dorsal line are resected and used for framework grafts. The borders of the reflected mucoperichondrial flaps are sutured to the margins of the lining defect. A framework of cartilage grafts is created from septal and auricular cartilage to replace the missing portions of the dome complex and lateral crura. The cartilage remaining within the composite flap serves as the medial crura for the construction and provides support to the columella. It also serves as the foundation for the framework grafts used for the nasal domes. These grafts are sutured directly to the cartilage of the composite flap and are then scored and bent in a fashion to restore the contour of the domes. The mucoperichondrial flaps reflected laterally from the composite chondromucosal flap are approximated to the overlying framework grafts with sutures placed through the framework cartilage and underlying flaps. Some of the cartilage of the caudal aspect of the composite flap may require trimming if it causes excessive caudal positioning of the reconstructed columella.
Septal Composite Chondromucosal Pivotal Flap for Dorsum
There are occasions when a patient presents with an intact nasal tip but has a full-thickness dorsal defect involving loss of cartilaginous dorsum and nasal bones. In these circumstances, the remaining septum may be used as a composite chondromucosal pivotal flap to provide a mucosal lining and structural support for the roof of the middle and upper nasal vaults (Fig. 18-10). The anterior septal angle is usually missing along with the upper lateral cartilages, and the composite flap is used to resurface the interior of the entire dorsal defect. The flap is harvested in a manner similar to that described for the pivotal flap used to reconstruct full-thickness defects of the tip and columella. The flap pivots only 45°, compared with 90° for repair of the tip and columella, so it is not necessary to remove the anterior nasal crest bone. Working through an endonasal approach as well as through the dorsal defect, a full-thickness horizontal incision is made through the septum along the length of the nasal crest. The anterior extent of this incision remains 1.5 cm posterior to the anterior nasal spine. The length of the incision depends on the defect but usually extends 2 to 3 cm posteriorly through the bony septum. This is usually necessary to ensure sufficient length to enable the flap to engage the frontal bone or remaining nasal bones once it is pivoted into position. A vertical incision is extended from the posterior end of the horizontal incision along the floor of the nose. This septal incision extends upward to join the most cephalic aspect of the bony or cartilaginous septum exposed by the defect. The flap is delivered from the nasal passage by manually pivoting the flap 45° on its pedicle. It may be necessary to remove cartilage in the area of the posterior septal angle to pivot the flap. This should be performed so that the adjacent mucoperichondrium is not damaged; this tissue represents the pedicle for the flap.
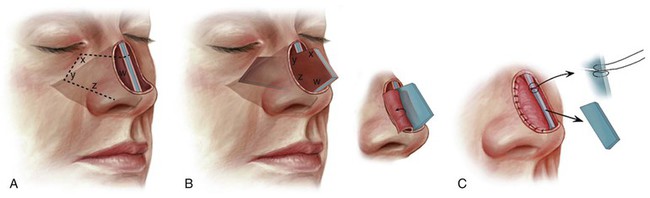
FIGURE 18-10 A, Broken line indicates full-thickness incision through septal cartilage, bone, and bilateral mucosa to create composite septal chondromucosal pivotal flap. B, Cephalic aspect of pivoted flap locked into place by abutting it against remaining nasal bony septum. Bilateral mucoperichondrial flaps reflected laterally to provide lining to nasal passage. C, Excess septal cartilage and bone trimmed and mucoperichondrial flaps sutured to borders of lining defect. Figure-of-eight suture fixes composite flap to remaining nasal bony septum. (From Baker SR: Internal lining. In Baker SR, editor: Principles of nasal reconstruction, ed 2, New York, Springer, 2011.)
Septal Composite Chondromucosal Pivotal Flap for the Tip, Columella, and Dorsum
Total and near-total nasal reconstruction may use the septum for internal lining if sufficient septum remains. This requires incorporation of the entire remaining nasal septum in the composite flap (Fig. 18-11). These cases are frequently associated with resection of the caudal cartilaginous septum and loss of the septal branches of the superior labial artery. In these circumstances, the flap is based on the mucoperiosteum of the anterior floor of the nose, and delay of the flap is necessary. Three stages are used to line the nose.
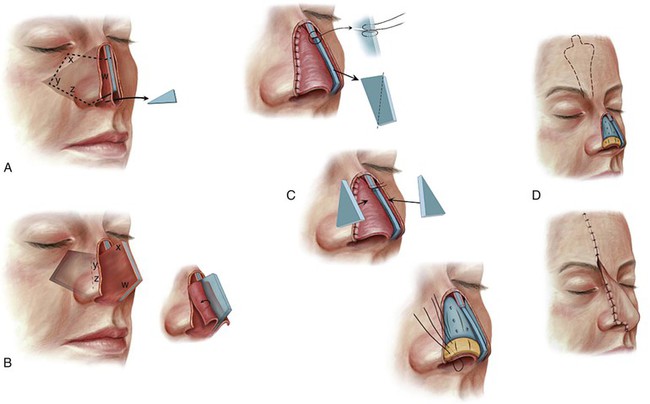
FIGURE 18-11 A, Bold broken line indicates full-thickness incision through septal cartilage, bone, and bilateral mucosa. Solid bold line indicates incision only through septal cartilage, preserving mucoperichondrium. Wedge of cartilage removed to enable flap to pivot anterocaudally. B, Cephalic aspect of pivoted flap locked into place by abutting it against nasal process of frontal bone. Bilateral mucoperichondrial flaps reflected laterally to provide lining to nasal passages. C, Excess septal cartilage and bone trimmed and mucoperichondrial flaps sutured to borders of lining defect. Figure-of-eight suture stabilizes composite flap to nasal process. Septal cartilage (blue) and auricular cartilage (yellow) provide nasal framework. Cartilage grafts scored to create desired convex contour. Mucoperichondrial flaps attached to framework with mattress sutures. D, Nasal framework covered by paramedian forehead flap. (From Baker SR: Internal lining. In Baker SR, editor: Principles of nasal reconstruction, ed 2, New York, Springer, 2011.)
Stage one consists of making the previously described inferior horizontal incision along the floor of the nose and vertical incision through the mucosa on either side of the septum but not through the bone and cartilage. Stage two is completed 3 weeks later by making incisions through the cartilage and bone of the septum, following the previous incision lines made in the covering mucosa. The composite flap is delivered from the nasal passage and is pivoted 90° to provide the maximum amount of mucosa for construction of the lining of the caudal portion of the nose. If the cephalic portion of the dorsum is missing, there will not be a buttress on which to stabilize the pivoted flap. In this case, nasal packing is used to stabilize the flap. Packing is left in place for 5 days. The flap is left protruding from the nasal passage for 4 to 6 weeks before proceeding with reconstruction of the nasal lining. Stage three consists of creating bilateral mucoperichondrial flaps based on the anteroinferior border of the mobilized composite flap. The flaps are reflected laterally to line the roof and sidewalls of the caudal nose. If the flaps are lacking sufficient tissue to line the cephalic portions of the nasal passage, local turn-in flaps or a paramedian forehead flap is used as lining for this portion of the nose. The reflected mucoperichondrial flaps are supported by an overlying framework of cartilage and bone that is covered by a paramedian forehead flap.
Turbinate Mucoperiosteal Flap
The middle and inferior turbinates may be used to line limited mucosal defects of the nose.10 These turbinates are richly supplied by a vascular network arising from a lateral descending branch of the sphenopalatine artery. The main supply to the inferior turbinate from this artery enters 1.0 to 1.5 cm from its posterior border and passes forward, giving off an anastomotic network of vessels. The artery also has anastomotic connections with the anterior blood supply of the turbinate. The anterior blood supply originates from the angular artery and is sufficient to allow the entire turbinate to be pedicled on this source.11,12
Middle and inferior turbinate flaps are harvested by a similar technique (Fig. 18-12). A local anesthetic solution containing a concentration of epinephrine of 1 : 100,000 is infiltrated along the turbinate, floor of the nose, and middle or inferior meatus, depending on which turbinate is used. The turbinate is medialized with a blunt elevator or the handle of a scalpel to open the meatus below the turbinate. A Cottle elevator or a 2-mm osteotome is placed in the meatus below the turbinate and pushed superiorly to perforate the bony attachment to the lateral nasal wall. Multiple perforations of the bone are made along the length of the turbinate, starting 1 cm posterior to the anterior end of the turbinate. The cutting instrument is maintained in a vertical plane against the lateral nasal wall to maximize the amount of tissue obtained without penetrating the paranasal sinuses. Pedicled anteriorly, the posterior aspect of the mobilized turbinate is pivoted toward the nasal defect with Takahashi forceps. The bone of the delivered turbinate is removed, leaving a mucosal flap that is transferred to the recipient site and sutured in position. If the location of the lining defect is the nasal tip, the pedicle of the flap will, by necessity, span the nasal passage and partially obstruct the airway. In this case, detachment of the pedicle is accomplished under local anesthesia 3 weeks later.
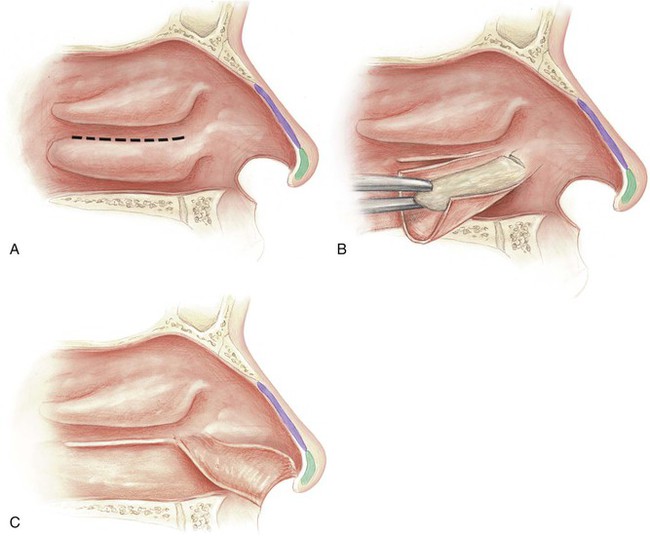
FIGURE 18-12 A, Inferior turbinate released from bony attachment to lateral nasal wall (dotted line). B, Mucoperiosteum dissected from underlying concha bone and unfurled. Bone removed. C, Pedicled anteriorly, inferior turbinate mucoperiosteal flap is usually sufficient to line entire ala. (From Baker SR: Intranasal flaps. In Baker SR, editor: Principles of nasal reconstruction, ed 2, New York, Springer, 2011.)
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses