Instrumentation for Client Assessment and Care
Instrument Design
Parts of an Instrument
A Handle—the part of a periodontal instrument that the clinician holds; various shapes, weights, sizes, and surface serrations (smooth, ribbed, or knurled) exist
B Shank—connects the working end with the handle; usually bent in one or more places to facilitate placement of the working end against the tooth surface
1. Functional shank—the part of the shank that allows the working end to be adapted to the tooth surface; begins below the working end and extends to the last bend in the shank nearest the handle
a. Instruments with short functional shanks are used on teeth crowns
b. Instruments with long functional shanks are used on both the crown and the root (Figure 17-1)
2. Lower (terminal) shank—the bent portion of the functional shank nearest to the working end (see Figure 17-1)
3. Extended lower shank—3 mm longer than a standard lower shank; provides additional leverage, acting like a fulcrum, and is ideal when using advanced levering techniques or for working in deep periodontal pockets
4. Simple shank—bent in one plane (front to back); used primarily on anterior teeth; also called a straight shank
5. Complex shank—bent in two planes (front to back and side to side) to facilitate instrumentation of posterior teeth; this design is necessary to reach around the crown and onto the root surface; also called an angled shank or curved shank
C Working end—the part of the dental instrument that contacts the tooth or soft tissue to perform the work of the instrument; begins where the instrument shank ends; an instrument may have one or two working ends
1. Parts of the working end—identified as the face, back, lateral surfaces, toe, and tip; on a hand-activated debridement instrument, a cutting edge is formed by the union of a lateral surface and the face of the working end
2. Application of the working end—the tooth surfaces or areas of the mouth on which an instrument can be used
a. Anterior use—one single-ended instrument (e.g., anterior sickle scaler, such as a Jacquette 33) can be used to perform procedures on the facial, lingual, mesial, and distal surfaces of anterior teeth
b. Posterior use—one double-ended instrument (e.g., posterior sickle scaler, such as a Jacquette 34/35) can be used to perform procedures on the facial, lingual, mesial, and distal surfaces of posterior teeth
c. Universal use—one double-ended instrument (e.g., universal curet, such as a Columbia 13/14) can be used to perform procedures on both anterior and posterior teeth
d. Area-specific use—an instrument that can be applied only to specific surfaces and areas of the mouth; a set of area-specific instruments (e.g., area-specific curets, such as the Gracey series) is needed for procedures on the entire dentition
Design Characteristics
A Instrument balance—a balanced instrument has working ends that are aligned with the long axis of the handle
1. During a work stroke, for example, in calculus removal balance ensures that finger pressure applied against the handle is transferred to the working end, which results in pressure against the tooth
2. An instrument that is not balanced is more difficult to use and increases stress on the muscles of the user’s hand and arm
B Instrument identification—the unique design name and number that identify each periodontal instrument
1. Design name—identifies the school or individual responsible for the original design or development of an instrument or group of instruments (e.g., ODU 11/12 periodontal explorer, in which the ODU stands for Old Dominion University; and the TU-17, in which TU stands for Tufts University School of Dental Medicine)
2. Design number—the number designation of the working end that, when combined with the design name, provides the exact identification of the working end (e.g., Gracey 11, in which Gracey is the design name, and 11 is the design number)
3. Identification of the working ends of a double-ended instrument—a double-ended instrument will have two design numbers, one number for each working end of the instrument
a. If the design name and number are stamped along the length of the handle, each working end is identified by the number closest to it
b. If the design name and number are stamped across the handle, the first number identifies the working end at the top of the handle, and the second number identifies the working end at the bottom
Hand-Activated Instruments
Classifications
A Hand-activated nonsurgical periodontal instruments are classified as periodontal probes, explorers, sickle scalers, periodontal files, universal curets, area-specific curets, hoes, or chisels; hoes and chisels are rarely used because their functions have been largely replaced by mechanized instruments
B Periodontal instruments are divided into classifications based on the specific design characteristics of the working end; design characteristics include:
1. Design of the cutting edges, back, lateral surfaces, and shank
2. Cross-section of the working end
3. Relationship of the face to the lower shank (Table 17-1)
TABLE 17-1
Use of Hand-Activated Instruments

From Nield-Gehrig JS: Fundamentals of periodontal instrumentation and advanced root instrumentation, ed 6, Philadelphia, 2008, Lippincott Williams & Wilkins.
C In selecting an instrument for a specific task, one of the most important considerations is the classification of the working end
Dental Mirror
1. The working end has a reflecting (mirrored) surface
a. Front surface—the reflecting surface is on the front surface of the glass; produces a clear mirror image with no distortion
b. Concave—the reflecting surface is on the front surface of the mirror lens; produces a magnified but slightly distorted image
c. Plane—the reflecting surface is on the back surface of the mirror lens; this type of surface is less easily scratched than a front surface mirror but produces a double or “ghost” image
1. Indirect vision—the mirror’s reflecting surface provides a view of the tooth surface or intraoral structure that cannot be seen directly
2. Retraction—using the mirror to hold the client’s cheek or tongue to view tooth surfaces or other structures that are otherwise hidden by the cheeks or tongue
3. Indirect illumination—reflecting light from the mirrored surface into a dark area of the mouth
4. Trans-illumination—reflecting light from the mirrored surface through anterior teeth
Probe
1. Calibrated probe (e.g., Williams, PSR screening probe) has a slender rod-shaped, blunt working end marked in millimeter increments; can be used as a miniature ruler for making intraoral measurements, such as for measuring sulcus and pocket depths, clinical attachment levels, width of attached gingiva, or the size of oral lesions; also used to assess for the presence of bleeding, or purulent exudate (pus)
2. Furcation probe (e.g., Nabers 1N) is a curved, blunt-tipped instrument used to detect and assess bone loss in the furcation areas of bifurcated and trifurcated teeth
C Calibrations—millimeter marks at intervals that are specific for each probe design
a. Probe designs may differ in millimeter markings (Table 17-2); only certain millimeter increments may be indicated on the probe (e.g., 1—2—3—5—7—8—9—10 mm), or each millimeter may be indicated (e.g., 1—2—3—4—5—6—7—8—9—10—11—12—13—14—15 mm)
TABLE 17-2

From Nield-Gehrig JS: Fundamentals of periodontal instrumentation and advanced root instrumentation, ed 6, Philadelphia, 2008, Lippincott Williams & Wilkins.
b. Color-coded probes are marked in bands (often black), with each band being several millimeters in width (e.g., 3–5 mm and 8–10 mm)
Explorer
1. Assessment instrument with a fine, flexible wire-like working end
2. Provides the best tactile information to the clinician’s fingers; used to locate calculus deposits, tooth surface irregularities, and defective margins on restorations
1. The working end is 1 to 2 mm in length and is referred to as the tip; the side of the tip, rather than the actual point, is used for detecting calculus
2. Circular in cross-section, the explorer may have paired or unpaired working ends
C Types—available in a variety of design types; not all design types are well suited to subgingival use; therefore, the clinician must be knowledgeable about the recommended use of each design type
1. Shepherd hook (e.g., #23 and #54 explorers)—an unpaired explorer with a short, highly curved shank and a sharp point; used for supragingival examinations to detect irregular margins of restorations; not recommended for calculus detection because subgingival use could result in tissue trauma
2. Straight explorer (e.g., 6, 6A, 6L, 6XL)—an unpaired explorer with a short lower shank and a sharp point; used for examinations to detect irregular margins of restorations; not recommended for subgingival calculus detection
3. Curved explorer (e.g., 3, 3A)—an unpaired explorer with a curved shank and a sharp point; limited for use in examining normal sulci or shallow pockets; may be used for calculus detection; however, care must be taken not to injure the junctional epithelium when the working end is used subgingivally
4. Orban-type explorer (e.g., TU-17, Orban 20)—an unpaired explorer with a straight lower shank that can be used in deep pockets with only slight tissue displacement (stretching of the tissue wall away from the tooth); the explorer tip is bent at a 90-degree angle to the terminal shank, which allows the back of the tip (instead of the point) to be directed toward the junctional epithelium; useful for detecting subgingival calculus on anterior teeth or on the facial and lingual surfaces of posterior teeth; however, the straight lower shank makes it difficult to adapt to the line angles and proximal surfaces of posterior teeth
5. Pigtail or cowhorn explorer (e.g., 3MI, 3CH, 2A)—a paired universal explorer with a short, broadly curved lower shank and a sharp point; the curved lower shank causes considerable tissue displacement; useful for detecting calculus in normal sulci or shallow pockets extending no deeper than the cervical third of the root
6. The 11/12-type explorer (e.g., ODU 11/12, 11/12 AF)—a paired universal explorer with an extended lower shank and a tip that is bent at a 90-degree angle to the terminal shank; the tip design allows the back of the tip to be applied to the pocket base without lacerating the junctional epithelium; this effective explorer design adapts well to all surfaces throughout the mouth and is equally useful when exploring a shallow sulcus or a deep periodontal pocket
Sickle Scaler
1. Cutting edges—two cutting edges that meet in a point
2. Back—sharp, pointed back; some types of scalers are made with flattened backs
3. Cross-section—triangular; lateral surfaces meet the instrument face at an internal angle between 70 and 80 degrees
4. Face—perpendicular to the lower shank so that the cutting edges are level with each other; level cutting edges require that the lower shank be tilted slightly toward the tooth surface to establish correct angulation
5. The anterior sickle scaler has an unpaired working end and a simple shank; primarily used on anterior teeth (e.g., Jacquette 33)
6. The posterior sickle scaler has paired working ends, with complex shanks; primarily used on posterior teeth but may be used on anterior teeth (e.g., Jacquette 34/35)
Periodontal File
1. Calculus removal instrument used to prepare calculus deposits before removal with another instrument
1. Cutting edges—multiple cutting edges at a 90- to 105-degree angle to the lower shank
2. Working end—thin in width with a large circumference at the base; the base may be round, oval, or rectangular in shape
3. Area-specific application—each working end is designed for use on a single surface (four working ends are needed for procedures on all tooth surfaces); files with simple shanks work best on anterior teeth; those with complex shanks work best on posterior teeth
1. Preparation of burnished calculus deposit (a deposit with a smooth outer surface) before removal of the deposit with a curet; a file is used to scratch the surface of a burnished deposit so that it can be removed with another instrument
2. Crushing of a large calculus deposit; once a deposit has been crushed with a file, it is easier to remove with a curet
3. Smoothing overextended or rough amalgam restoration in sites where the file can be effectively adapted
Universal Curet
1. One of the most frequently used and versatile of all the debridement instruments
2. Used both supragingivally and subgingivally; two curets usually are paired on a double-ended instrument (the paired working ends are mirror images of each other)
1. Cutting edges—two cutting edges that converge in a rounded toe
2. Back—the rounded back is ideal for subgingival use
3. Cross-section—semi-circular; lateral surfaces meet the instrument face at an internal angle between 70 and 80 degrees
4. Face—perpendicular to the lower shank so that the cutting edges are level with each other; the level cutting edges require that the lower shank be tilted slightly toward the tooth surface to establish correct angulation
5. Universal use—one double-ended instrument can be applied to all tooth surfaces in the anterior and posterior regions of the mouth
Area-Specific Curet
1. Debridement instrument with one cutting edge (only one cutting edge per working end is used for procedures); a set of curets is needed to perform procedures throughout the mouth
2. The curet is used supragingivally and subgingivally; especially well suited for root surface debridement within periodontal pockets
3. Designs include area-specific curets with miniature working ends, extended shanks, and flexible and rigid shanks
1. Cutting edge—one working cutting edge per working end; only the lower, longer cutting edge is used
2. Back—rounded back; ideal for subgingival use
3. Cross-section—semi-circular; the lateral surfaces meet the instrument face at an internal angle between 70 and 80 degrees
4. Face—tilted at a 60- to 70-degree angle in relation to the lower shank, making one cutting edge (the working cutting edge) lower than the other; this tilted relationship makes the working cutting edge “self-angulated” (that is, when the lower shank is parallel to the tooth surface, the cutting edge is at the correct angulation)
5. Area-specific use—each working end is limited to use only on certain teeth and on certain surfaces
Hand Instruments for Root Debridement
1. The treatment of clients with periodontitis requires specialized instruments with longer shank lengths and miniature working ends for instrumentation of root concavities and furcation areas
2. Designs include area-specific curets with miniature working ends, extended shanks, flexible and rigid shanks, and diamond-coated working ends
B Examples of advanced root debridement instruments—a variety of periodontal instruments have been developed to increase treatment effectiveness on root surfaces within deep periodontal pockets
1. The 11/12-type periodontal explorer—an 11/12 AF (After Five) explorer has an extended shank and is ideal for use in deep periodontal pockets
2. Advanced curet designs—several curets are ideal for instrumentation within deep periodontal pockets
a. Vision curvette curet series—have a working end that is shortened to half the length of a standard Gracey curet, a curved working end, and an extended lower shank
(1) Several varieties of modified Gracey curets—include modified Gracey curets with extended shanks, miniature Gracey curets, and micro Gracey curets
(2) Design features for modified Gracey curets—include extended lower shank length, thinner working ends, and working ends that are shorter in length than in a standard Gracey curet
c. Quetin Furcation curets—specialized instruments that are used to debride furcation areas and root concavities; each miniature working end has a single, straight cutting edge with rounded corners; the working ends are available in either 0.9-mm or 1.3-mm size
d. O’Hehir debridement curets—area-specific curets that are designed to remove light residual calculus deposits and bacterial contaminants from root surfaces
(1) The working end of an O’Hehir curet is a tiny circular disc; the entire working end is a cutting edge; the working end curves into the tooth for easy adaptation in furcation areas and developmental grooves
e. Instruments with diamond-coated working ends
(1) The working ends of these instruments do not have cutting edges; instead, they are coated with a very fine diamond grit, for example, a version of the Nabers furcation probes are diamond coated
(2) Diamond-coated instruments can be used to remove light residual calculus deposits and bacterial contaminants from root surfaces
(3) Because of the abrasive nature of their working ends, these instruments should be used with light, even pressure against the root surface to avoid gouging or grooving
Principles of Instrumentation
Position of the Clinician
A Neutral, seated position (Figure 17-6)
1. Head—tilt of 0 to 15 degrees
2. Shoulders—in a horizontal line
3. Back—straight or leaning forward slightly from the waist or hips
4. Thighs—hips slightly higher than the knees
5. Upper arms—parallel to the long axis of the torso
6. Elbows—at waist level; held slightly away from body
7. Forearms—parallel to the floor; raised or lowered, if necessary, by pivoting at the elbow joint rather than by raising the elbows
8. Feet—seat height should be positioned low enough so that the heels of the feet can rest on the floor
B Relationship to the client and the dental unit
1. The client’s chair should be positioned such that the tip of the client’s nose is at a lower level at a level slightly lower than clinician’s elbows; clinician should not have to raise the elbows above his or her waist level to reach the client’s mouth; lower arms should be in a horizontal position or raised slightly so that the angle formed between the lower and upper arm is slightly less than 90 degrees
2. All instruments and equipment should be positioned within easy reach of the clinician
Stabilization During Instrumentation
A Modified pen grasp—the recommended grasp for holding a periodontal instrument that allows precise control of the working end; precise placement of the fingers in the modified pen grasp is important to be successful in instrumentation technique
1. Finger placement and function (Figure 17-7)
a. Index finger and thumb—finger pads hold the instrument handle
b. Middle finger—the side of the finger pad rests on the instrument’s shank; the clinician’s fingers should be able to feel the vibrations in the instrument’s shank as the working end encounters roughness on the tooth surface
c. Ring finger—fingertip rests on a stable surface, usually the occlusal or incisal tooth surface, which stabilizes the hand for control and strength
a. A light grasp is needed for increased tactile sensitivity during assessment procedures (e.g., subgingival use of explorer or probe)
b. A firm grasp is used with hand-activated instruments during calculus removal
3. Glove fit—proper fit of sterile gloves is important in avoiding muscle strain during instrumentation
a. Fulcrum—the point of support on which the clinician rests the hand; used to stabilize the clinician’s hand during instrumentation; the pad of the ring finger serves as the fulcrum finger during instrumentation to control stroke pressure and length
b. Finger rest—the place where the fulcrum finger rests during instrumentation
(1) The finger rest is placed on a tooth, close to the tooth being worked on; should not be positioned in the line of the instrument’s stroke to prevent instrument stick
(2) The intraoral fulcrum is considered the most desirable because it provides the greatest stability and strength for calculus removal
b. Basic extraoral fulcrum—placed outside the client’s mouth, usually on the chin or cheek
c. Advanced fulcrums—variations of the basic fulcrum that may be required for access to posterior teeth or root surfaces within periodontal pockets; advanced fulcrums require greater skill and stroke control than the basic intraoral fulcrum
3. Advanced fulcrum techniques
a. Piggy-backed—intraoral fulcrum in which the middle finger is stacked on top of the ring finger
b. Cross-arch—intraoral fulcrum in which the finger rests on the side of the arch opposite the treatment area
c. Opposite arch—intraoral fulcrum in which the finger rests on the arch opposite to the treatment area
d. Finger-on-finger—intraoral fulcrum in which the finger of the nondominant hand serves as the resting point for the ring finger of the dominant hand
e. Stabilized—intraoral or extraoral fulcrum in which a finger of the nondominant hand is used to concentrate lateral pressure against the tooth surface and to help control the instrument stroke
Adaptation
A Definition—positioning the first 1 or 2 mm of the lateral surface of the working end of the instrument in contact with the tooth surface
1. Explorer—the first few millimeters of the tip (not the point) are adapted to the tooth surface for calculus detection
2. Probe—the side of the probe tip is maintained against the tooth surface, with the length of the probe almost parallel to the tooth surface being probed
3. Sickles and curets—the leading one third of the cutting edge is positioned to conform to the tooth surface
Angulation
A Definition—the relationship between the face of a calculus removal instrument and the tooth surface to which the working end is applied
1. For insertion beneath the gingival margin—the face-to-tooth surface angulation is between 0 and 40 degrees
2. For debridement—the face-to-tooth surface angulation is between 45 and 90 degrees; a 60-degree angulation works well for removing plaque, whereas a 70- to 80-degree angulation is ideal for calculus removal (Figure 17-8)
Activation
A Definition—moving an instrument to produce a stroke; it is the action of an instrument in the performance of the task for which it was designed
C Stabilization and lateral pressure
a. Stabilization—preparing for an instrument’s stroke by locking the joints of the ring finger and pressing the fingertip against the tooth surface to provide control for the stroke
b. Lateral pressure—applying pressure equally with the index finger and the thumb inward against the instrument’s handle to engage the working end against a calculus deposit or the tooth surface before and throughout an instrument’s stroke
a. Pressure during stroke activation—stroke pressure is applied in a coronal direction; the pressure ranges from light to firm, depending on the amount of pressure needed for the particular task (e.g., assessment, calculus removal)
b. Pressure between strokes—finger muscles should be relaxed as the working end is repositioned, using light stroke pressure
D Maintaining adaptation during stroke production
1. Hand pivot—turning the hand and arm slightly while resting on the fulcrum to maintain adaptation; used when moving around line angles and onto proximal surfaces
2. Handle roll—rolling the instrument handle slightly between the thumb and the index finger to maintain adaptation as the instrumentation strokes advance around the tooth surface; either the thumb or the index finger is used to roll the instrument
E Neutral wrist position—correct wrist position is important to avoid muscle discomfort and injury during the procedure; the wrist should be aligned with the long axis of the forearm; bending the wrist up, down, or to the side should be avoided
Instrumentation Strokes
1. Placement stroke—used to position the working end at the base of the sulcus pocket or apical to a calculus deposit
2. Assessment strokes—used to evaluate the tooth surface or the health of periodontal tissue
a. Used with probes, explorers, curets
b. Angulation—50 to 70 degrees
c. Lateral pressure—in contact with the tooth surface; light pressure
d. Character—fluid strokes of moderate length
e. Number—many strokes used to cover the entire root surface
3. Calculus removal work strokes—used to remove calculus deposits
a. Used with hand-activated sickle scalers, curets, and files
b. Angulation—70 to 80 degrees
c. Lateral pressure—moderate to firm
d. Character—powerful strokes; short in length
e. Number—the number of strokes should be limited to the areas where needed
4. Root debridement work strokes—used to remove residual calculus deposits, plaque biofilm, and plaque byproducts from root surfaces
1. Vertical—parallel to the long axis of the tooth; used on facial, lingual, and proximal surfaces of anterior teeth and on the mesial and distal surfaces of posterior teeth
2. Oblique—diagonal to the long axis of the tooth; used most commonly on facial and lingual surfaces
3. Horizontal—perpendicular to the long axis of the tooth; used at the line angles of posterior teeth, furcation crotch areas, and within pockets that are too narrow to allow vertical or oblique strokes
4. Multidirectional—a combination of vertical, oblique, and horizontal strokes, one by one, used in succession; for assessment or debridement of a subgingival tooth surface
1. Length—short, powerful stroke for calculus removal; longer, lighter stroke for root surface debridement
2. Overlap—strokes should overlap to ensure complete coverage; long ridges of calculus are treated in sections, in overlapping scaling zones
a. Large calculus deposits should be removed in sections with a series of short, firm strokes
(1) A calculus deposit should not be removed in layers because removing the outermost layer will leave the deposit with a smooth surface (burnished surface)
(2) burnished calculus deposit may be indistinguishable (when explored) from the tooth surface
b. For subgingival instrumentation, it is helpful to imagine that the root surface is divided into a series of narrow, diagonal instrumentation zones
Steps for Calculus Removal with Hand-Activated Instruments
A Position the dental mirror, and establish a finger rest
B Grasp the instrument in a modified pen grasp
1. Locate the finger rest near the site of instrumentation in the dental arch; precise control of the instrument’s stroke becomes more difficult as the finger rest is moved farther away from the site of the procedure
D Adjust the hand–wrist–forearm as a unit
1. Position the thumb and the index finger across from each other on the instrument handle, near the junction of the handle and shank
2. Lightly rest one side of the middle finger pad on the instrument shank
3. Place the other side of the middle finger pad against the ring finger to allow the hand to function as a unit during the production of the stroke
4. Balance the tip of the ring finger on an occlusal or an incisal surface to support the weight of the hand and instrument
5. Position the wrist in a neutral position so that it is aligned with the long axis of the forearm (Figure 17-9)
1. If working subgingivally, close the face of the working end toward the tooth, and slide the working end to the junctional epithelium; use a light grasp while positioning the working end
2. Adapt the toe-third of the cutting edge to the tooth surface
3. Establish the instrument face-to-tooth surface angulation of 70 and 80 degrees
F Stabilize the grasp, and apply lateral pressure
1. Press down with the ring finger against the finger rest
2. Apply pressure against the instrument handle with the index finger and the thumb
G Activate a pulling stroke away from the junctional epithelium
1. Use hand–forearm activation for strength and control
2. Activate pulling strokes in a coronal direction to prevent particles of calculus from being pushed into soft tissue
3. Use vertical and oblique strokes in most areas; supplement these strokes with horizontal strokes, as needed
4. Use short, powerful strokes for calculus removal and longer, lighter strokes for root surface debridement
5. Use overlapping strokes to ensure complete coverage of the entire root surface
H Pause briefly at the end of a stroke
1. Relax the grasp, the finger rest, and the lateral pressure
2. Use a relaxed grasp to reposition the working end of the instrument for the next stroke
I Check the instrumentation area frequently with an explorer
Instrumentation for Assessment
Basic Concepts
A Thorough assessment involves examining all aspects of the periodontium and teeth
B Client preparation, based on information from the personal, comprehensive health and dental histories, is essential for safe instrumentation
C Successful treatment depends on well-developed assessment skills, before instrumentation, for dental care planning, and during and after instrumentation for evaluating treatment outcomes
Assessments with Periodontal Probes
A Purposes of the periodontal examination
1. Aid in planning dental care by determining gingival characteristics, probing depth, level of attachment, and presence of bone loss
2. Determine the extent of inflammation in conjunction with the probing depth and attachment level; bleeding resulting from probing is an early clinical sign of inflammation (Figure 17-10)
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


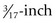 ) handles, with smooth or flat texture, decrease the user’s control and increase muscle fatigue
) handles, with smooth or flat texture, decrease the user’s control and increase muscle fatigue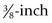 ) handles that are lightweight and have bumpy texturing maximize the user’s control and reduce muscle fatigue
) handles that are lightweight and have bumpy texturing maximize the user’s control and reduce muscle fatigue






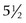 , 6,
, 6, 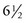 , rather than those marked in size ranges of small, medium, and large
, rather than those marked in size ranges of small, medium, and large


