17 Access Cavity Preparation
Root canal treatment begins with preparation of the access cavity, which should always be carried out with the rubber dam in situ. Difficulties encountered during instrumentation of a root canal can usually be traced to insufficient access cavity preparation and the lack of straight-line access to the root canals.
The entrance (orifice) of the root canal must be directly visible. This can often be facilitated by the use of loupes or a dental microscope. It is important to remove as much enamel and dentin as necessary. On the one hand, the access cavity must never be that small so as to inhibit visual detection of the root canal orifices. On the other hand, excessive preparation will reduce the structural strength of the remaining tooth tissues and hence the resistance to fracture (Reeh et al. 1983).
Errors made during the preparation of the access cavity usually result in a series of problems during the rest of the endodontic procedure. Such errors include insufficient excavation of caries as well as insufficient removal of the softened and unsupported hard tissues of the tooth. Incomplete removal of inadequate or poorly sealed restorations or crowns will lead to salivary and bacterial contamination of the instrumented root canal, which further leads to postoperative inflammation and other clinical consequences and ultimately failure. A lack of straight-line access to the root canals from within the pulp chamber can lead to ledge formation within a curved root canal and lateral perforation.
Therefore, a thorough knowledge of dental and root canal anatomy is of paramount importance when planning the shape and extent of the access cavity, because it must provide a complete view of the pulp chamber without compromising the tooth structure.
If previous restorations appear to be intact and do not show any inadequate areas on the radiographs, they can be left undisturbed. On the other hand, one must keep in mind that only after compete removal of an old restoration or a crown can the extent of carious penetration as well as poorly sealed areas be determined, the root canal orifices more easily detected, and straight-line access for root canal instrumentation guaranteed.
Build-up Restorations
Within a comprehensive treatment plan, only teeth with a favorable prognosis and which can be successfully restored should be included. Once the old restorations have been removed it is necessary to provide interim restorations, so that there is a stable coronal reference point for determination of endodontic working length and also to protect the tooth from overloading and possible fracture between endodontic appointments (Gutmann et al., 1991). In addition, it is necessary to ensure a seal against the oral milieu to prevent salivary contamination of the root canal.
The extent of the enamel or dentin defect and the amount of time the interim restoration has to be in place, as well as the expected masticatory loads on the tooth, will determine the type of interim restoration. Glass ionomer cements show very good marginal adaptation early on, but continued occlusal forces soon lead to substance loss, compromising the restoration margins (Krejci et al., 1986).
Today, a resin composite adhesive build-up restoration is often the interim restoration of choice. The long-term marginal seal, resistance to masticatory forces, and color stability of modern composites are so good that the preendodontic build-up can often serve as the postendodontic definitive restoration or as a secure base for definitive prosthetic reconstruction.
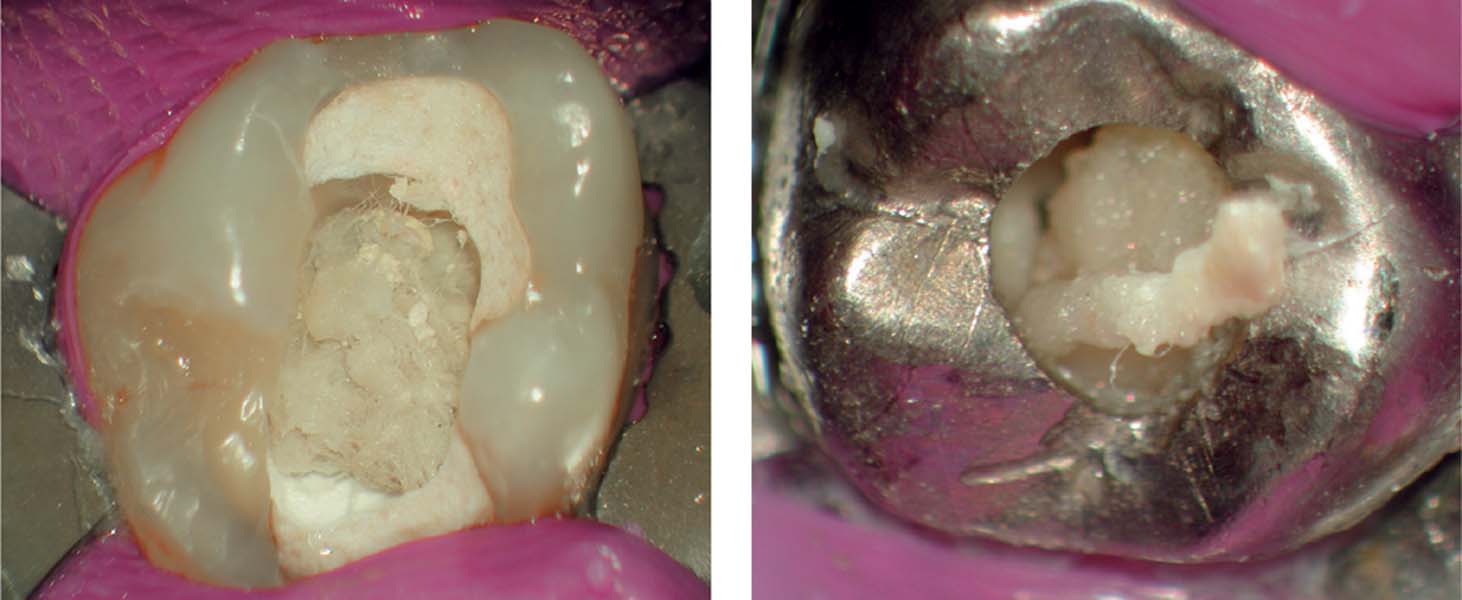
17.1 Inadequate temporary restoration
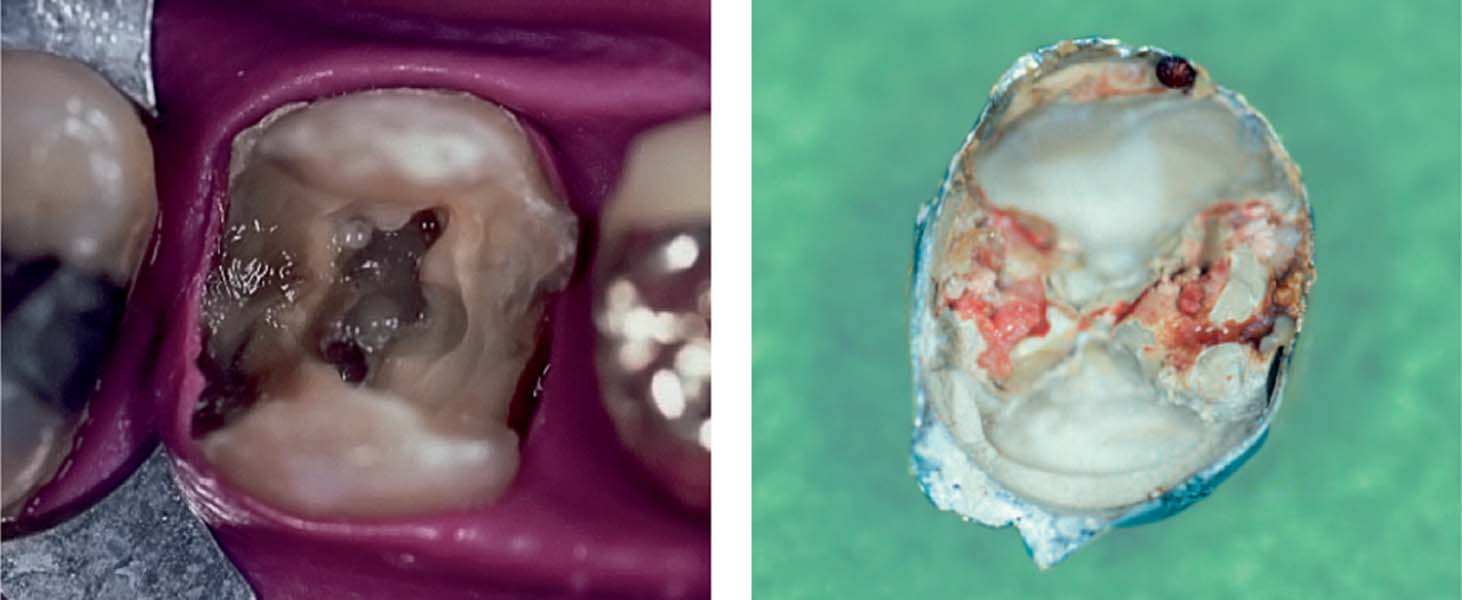
Left: Tooth 26 was treated 6 months previously. Beneath the temporary restoration is an inadequately opened pulp chamber with dentin overhangs as well as considerably large areas with caries in place.
Right: The inside surface of the temporary, prefabricated crown contains some cement as well as impacted food remnants. The margins of the crown were not adapted to the tooth, and where thus being exposed to the oral environment.
17.2 Initial opening
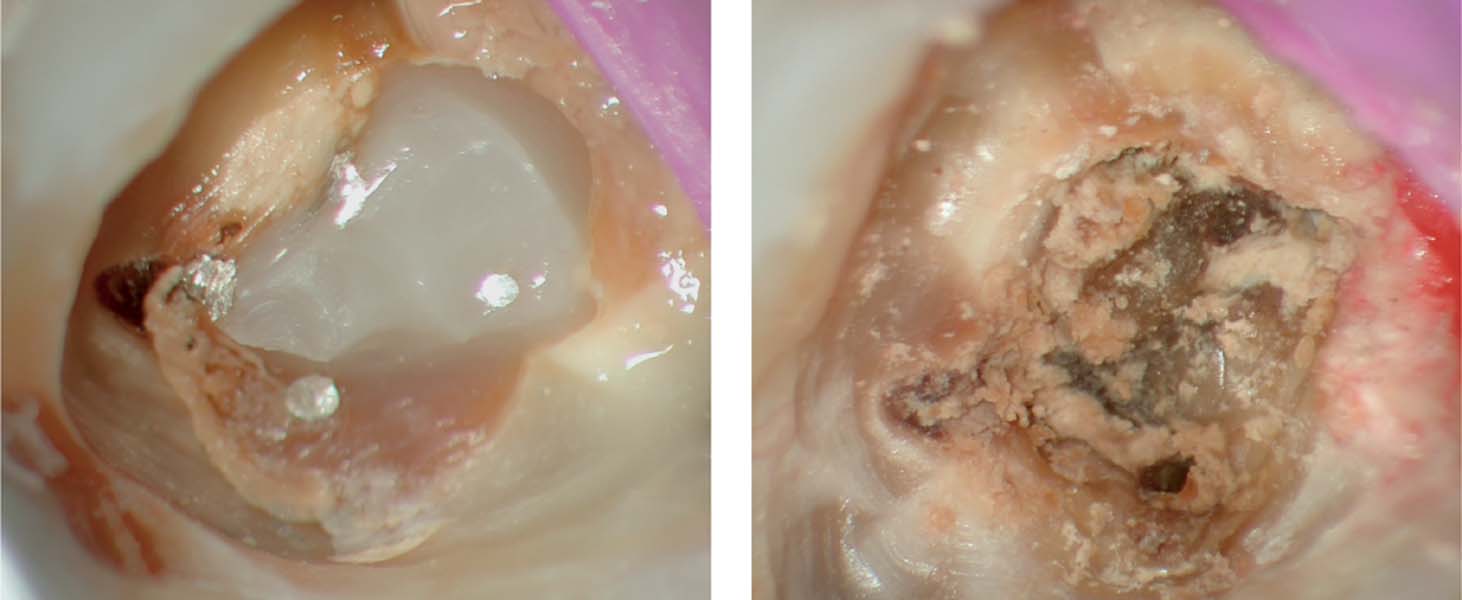
Left: This maxillary molar with four silver cones had to be re-treated. On re-opening the pulp cavity there were large areas of caries.
Right: Following successful removal of all four silver cones, the extent of the secondary caries became apparent.
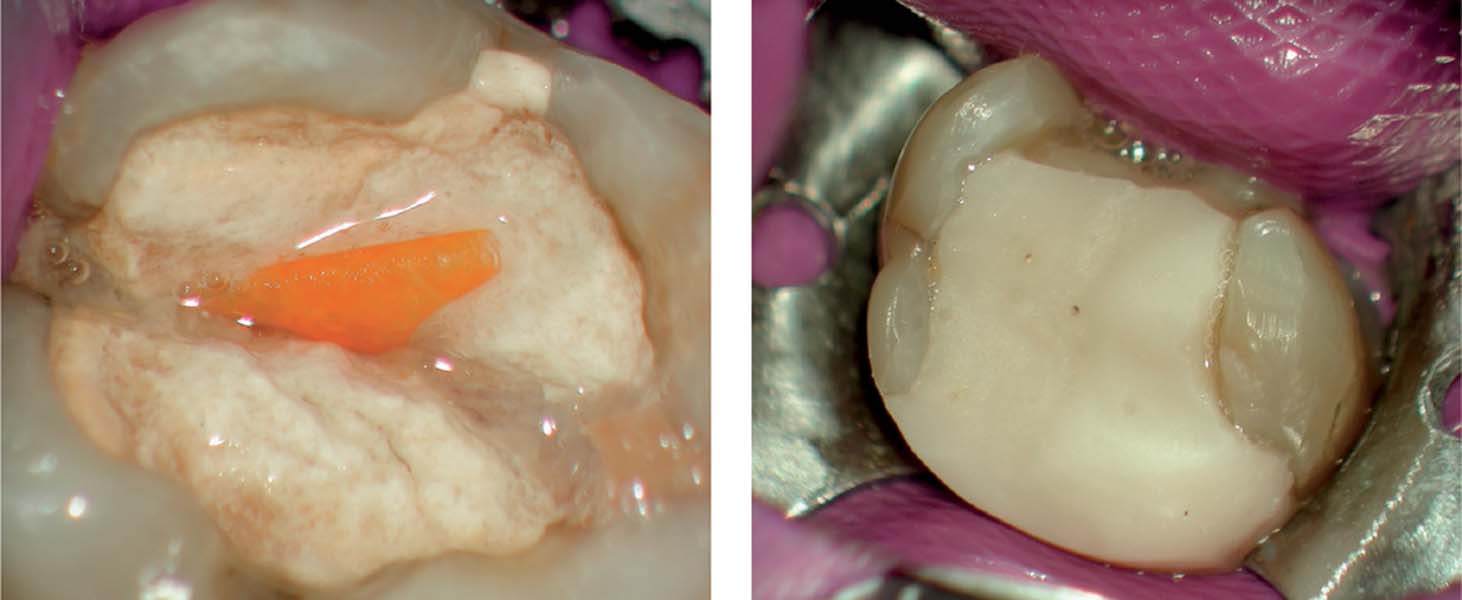
17.3 Build-up restoration
Left: Following complete removal of all carious dentin, the mesial cavity wall was etched with phosphoric acid.
Right: Using a flowable composite resin material, the mesial wall was restored, providing protection against salivary contamination.
Temporary Restoration
If the endodontic treatment procedure cannot be completed at a single sitting, an interim temporary restoration of the tooth will be required.
Cavit (3M Espe; zinc oxide, zinc, and calcium sulfate, glycol, etc.) is the most frequently used temporary filling material (Vail and Steffel, 2006) for both anterior teeth (54%) and posterior teeth (48%). Other agents commonly employed are IRM ([intermediate restoration material] 20% vs. 27%) and Cavit G (13% vs. 11%), which is usually used for inlays and is softer than Cavit.
It is interesting that about 80% of all surveyed endodontic specialists reported that they placed a cotton pellet under the temporary cavity seal (Dillard et al., 2002; Vail and Steffel, 2006). Sixteen percent placed no other material beneath the temporary filling, while 1% reported using foam/sponge (Vail and Steffel, 2006).
However, research has clearly demonstrated that the presence of even a few (one to five) cotton fibers leads to a marked reduction in closure/seal afforded by the temporary restoration (New-comb et al., 2001). Furthermore, the minimum layer thickness of 3.5 mm required for adequate sealing (Webber et al., 1978) will not be achieved.
17.4 Leaving the pulp chamber open
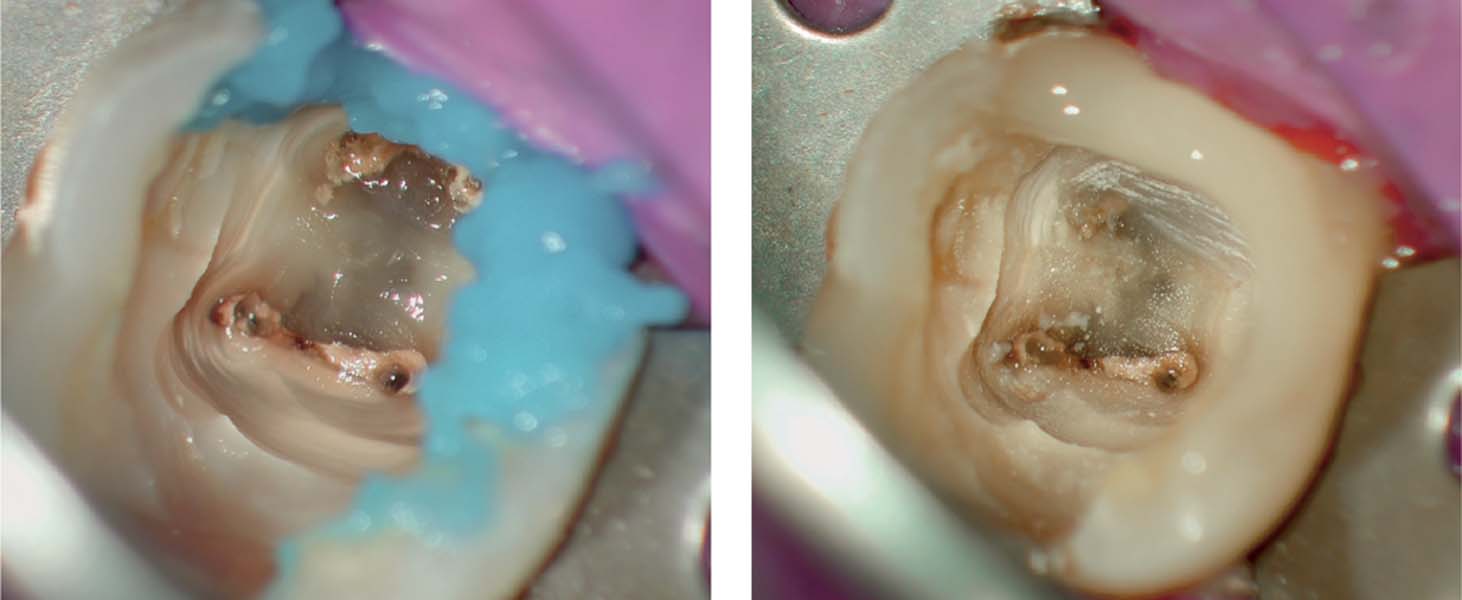
Left: Tooth 36 had been treated over a period of several months and mostly closed with a temporary restoration between sittings, but also left open if the patient experienced pain. At the initial sitting, a large amount of food debris was present in the pulp chamber.
Right: After cleaning up the pulp chamber and initial preparatory measures to have an adequate access cavity it became apparent that the pulpal roof was still partially intact. The distobuccal cusp was undermined by caries and had collapsed.
17.5 Preparation—Ledermix—Cotton—Cavit
Left: The almost universally accepted standard method for temporary endodontic restorations often leads to failure of the temporary cavity restoration because the minimal thickness for a temporary restoration of 4 mm cannot be achieved and Cavit can only withstand occlusal forces for 2–3 weeks.
Right: Placing paper points within the root canal and cotton pellets in the pulp chamber before placing the temporary restoration are for the most part counterproductive.
17.6 Failure of a temporary restoration
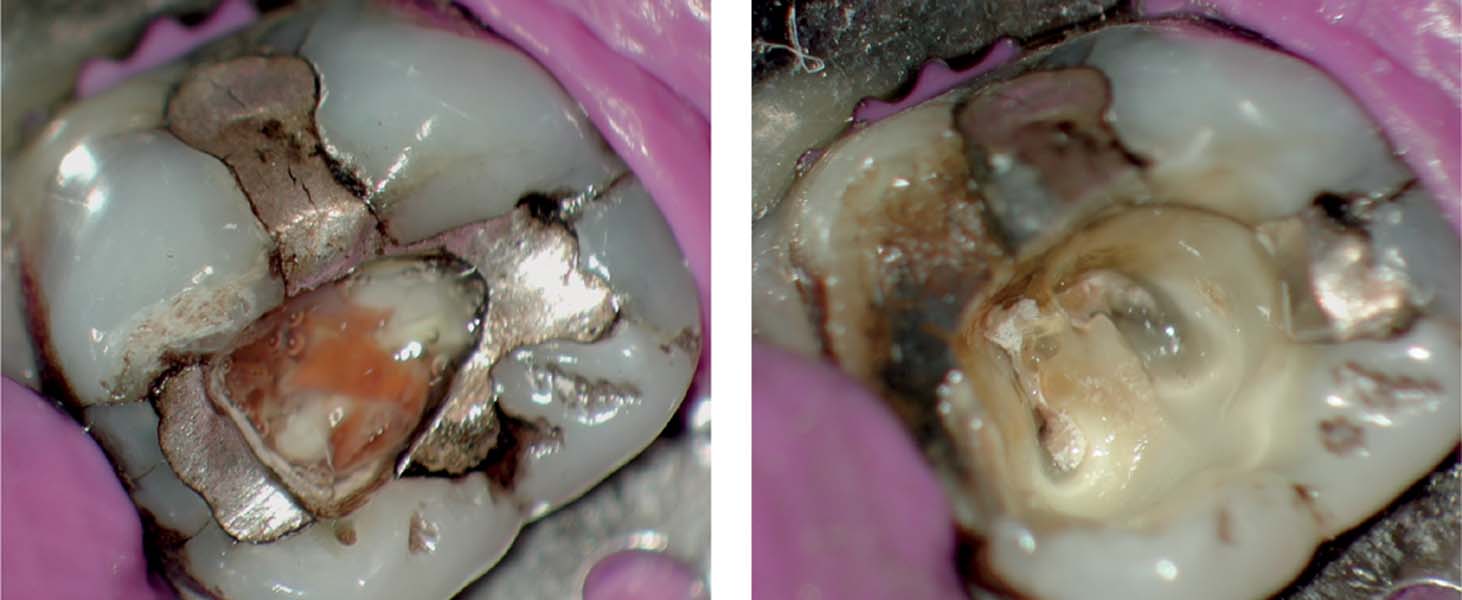
Left: In this molar, shortly after the initial treatment sitting including access cavity preparation as well as caries excavation and temporary closure with Cavit, a longitudinal fracture occurred. The cause was probably an initially existing in-line fracture and the preparation of the endodontic access cavity.
Right: Glass ionomer cement is often the material of choice for temporary closure of an access cavity. In the long term, however, this often leads to marginal imperfections and leakage.
Opening the Pulp Chamber
A potential major problem during opening of the pulp chamber, in addition to insufficient access preparation, is an incorrect estimation of the angle between the crown and the root. This error makes it much more difficult to locate the root canal orifices, and this can often be avoided with the use of a diagnostic radiograph. In teeth with large restorations, a bitewing radiograph should also be taken. To prevent excessive preparation at or perforation of the floor of the pulp chamber, the required length of the diamond bur can be assessed on a radiograph.
In addition to the classic diamond burs (round or cylindrical), combination shapes have been introduced, such as the Endo Access Bur (Dentsply, Maillefer) or the stainless-steel EndoZ. Because in many cases metal or porcelain/ceramic restorations must be drilled through during access cavity preparation, special burs may be required. Within a comprehensive endodontic instrument set, the practitioner should readily find the ideal instruments for a variety of approaches. With the increasing use of the clinical microscope, special designs such as the pulp bur “Müller” (Komet Brasseler, Savannah, GA, USA) incorporating a long delicate shaft are particularly useful.
17.7 Access cavity preparation and removal of old restorations
Left: Round burs as well as cylindrical burs, such as the EndoZ or the Endo Access Bur (Entsply Maillefer), are available worldwide for use in access cavity preparation.
Right: Special burs for the removal of amalgam (Komet Brasseler, Savannah, GA, USA). Metal and ceramic and composite burs (from left to right respectively) are available for extending the cavity opening.
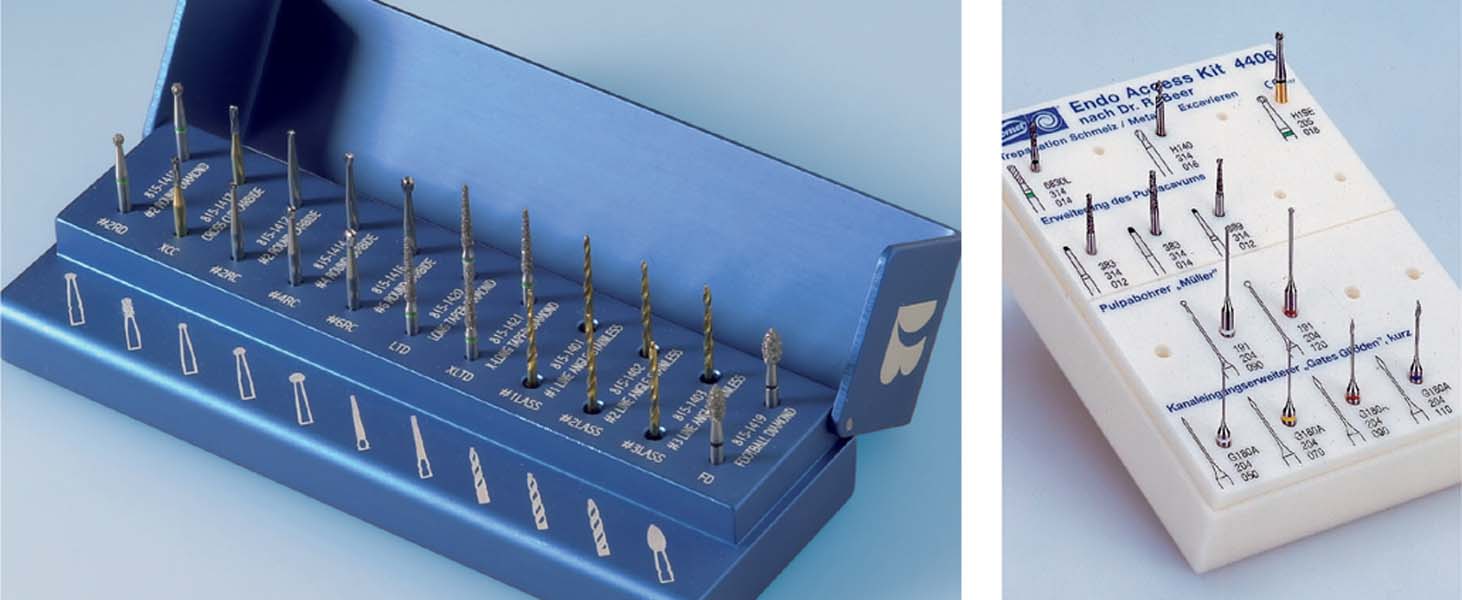
17.8 Instrument sets for access cavity preparation
As in other areas of dentistry, instrument sets for endodontics are commercially available. This makes the clinician’s selection easier, combining well-known instruments with additional aids within a well-organized tray (here: Sybron Endo, Orange, CA, USA).
Right: The Endo Access Kit (Komet Brasseler) has diamond burs, round burs, Müller burs, and Gates-Glidden burs.
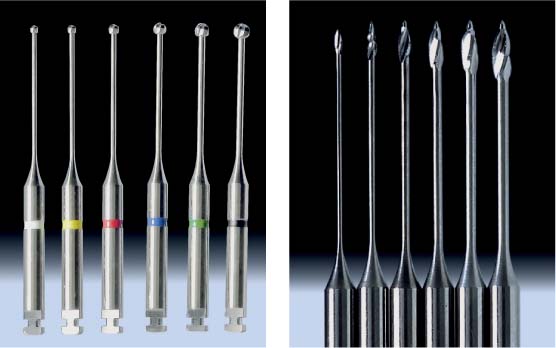
17.9 Aids for pulp chamber access
Left: The pulpal burs (Müller) combine a working end similar to a round bur with an especially long and elegant shaft. This provides excellent vision, even when working under the clinical microscope.
Right: The Gates-Glidden drills continue to be used effectively for drilling of the root canal orifices even after 100 years. The sizes start from 50 (= 0.5 mm) to 70, 90, and 110, and up to 130 and 150 (1.5 mm).
Traditionally, the pulp chamber is opened at a 45° angle to the long axis of the tooth. This procedure, however, can easily lead to perforation at the cervical margin on the labial side. Mandibular incisors often show an anatomic variation that requires locating the pulp chamber opening almost at the incisal edge to achieve straight-line access to the root canal (Sonntag et al., 2006). Because of the small size of these teeth, this procedure can lead to perforation, or even to failure to identify the root canal orifice.
Access cavities in premolars should have an oval shape with the long axis directed buccolingually. In maxillary molars, the cavity is located in the central fossa with the bur inclined toward the mesio/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses