Endodontic Management of Primary Teeth
Monty S. Duggal and Hani Nazzal
Pulpal complications such as pain, infection, and loss of teeth at a young age can pose considerable effects to the child’s psychological development [1], quality of life [1,2], growth [3], school attendance, arch space loss [4] in addition to posing considerable morbidity risk [5]. Successful endodontic management of these teeth is therefore crucial in order to maintain these teeth until physiologic exfoliation.
Endodontic management of primary teeth should be considered as part of the overall patient’s management plan. Careful planning including consideration of short‐ as well as long‐term prognosis must be done before any endodontic treatment is considered. Furthermore, other factors such as the effect of the treatment on the underlying permanent tooth germ, patient’s oral hygiene, patient’s medical history and patient’s behavior and future attitudes towards dentistry should be considered before embarking on any endodontic management.
The successful management of pulpally affected primary teeth demands an accurate diagnosis and knowledge of the appropriate endodontic management techniques. Appropriate medical and dental history, radiographic evaluation, and clinical assessment are, therefore, crucial prior to any endodontic management.
Diagnosis of pulpal status of primary teeth
Endodontic management of primary teeth depends on accurate diagnosis of the pulp status; therefore; it is important to differentiate between vital teeth showing signs of reversible pulpitis and those teeth with irreversible pulpitis and necrotic pulps (Box 16.1). Eighty percent of primary teeth with carious exposures but no clinical or radiographic pathology showed inflammation limited to the coronal part of the pulp (chronic coronal pulpitis) [6] (Figure 16.1). Teeth with total chronic pulpitis may show clinical as well as radiographic symptoms, and may not be expected to heal.
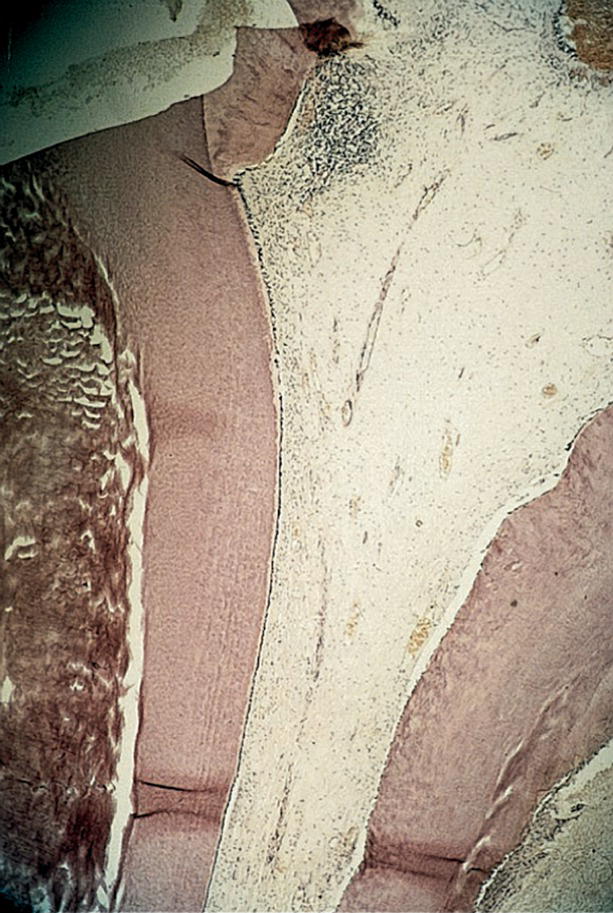
Figure 16.1 Histologic view of partial chronic pulpitis of a primary molar. Note the restricted area of chronic inflammation at the site of carious exposure.
Diagnosis of the pulpal status of teeth depends on careful clinical and radiographic assessment of these teeth. Careful assessment of the causative factors, signs, symptoms, and radiographic findings is, therefore; important in order to assess the tooth pulpal status (Box 16.1). This is particularly important where a deep carious lesion is present with breakdown of the marginal ridge.
An understanding of the pulp response to caries as well as correctly interpreting a patient’s symptoms is crucial in deciding whether an indirect pulp capping could be performed or whether more radical intervention would be required. For example, in cases where no pulp exposure is found clinically on removal of all caries for a deep proximal cavity, but where symptoms suggest pulp inflammation, it would be prudent to give consideration to a pulpotomy before restoration of the tooth. However, if there are no symptoms or other signs suggesting pulp inflammation, an indirect pulp capping approach should suffice.
Should endodontic interventions be carried out in the primary dentition?
There are several factors that should be considered when answering this question, such as:
- The pulpal diagnosis
- Occlusal considerations (Box 16.2)
- The patient’s ability to cooperate. Can the treatment be performed conventionally or is sedation/general anesthesia needed?
- Patient’s general and oral health
- Patient’s and parents’ motivation and consent
- Patient’s caries risk
- The risk of injury/infection of the underlying permanent tooth germ
- The effect of the proposed endodontic intervention on the patient’s health, for example infective endocarditis in children who have congenital heart defects or have had heart surgery
- The effect of the proposed endodontic intervention on the underlying permanent tooth germ.
These factors should help the clinician decide whether retaining or extracting the tooth is in the patient’s best interest. The placement of a temporary restoration or stepwise excavation could be considered to monitor the tooth prior to making a decision on endodontic intervention.
Endodontic techniques in primary teeth
The various endodontic techniques are presented in (Box 16.3). All endodontic treatment should be performed with due consideration for pain control and disinfection. Therefore, the tooth should be adequately anesthetized and isolated with a rubber dam.
Since most pulpal treatment of primary teeth involves a vital pulp, it is of utmost importance that the surgical technique is gentle—atraumatic—in order not to decrease the healing capacity of the residual pulp. The recommended technique includes use of diamond burs on high‐speed equipment and irrigation with water in order not to burn the residual pulp. This procedure has been shown under experimental as well as clinical conditions to be the most gentle to the residual pulp [7,8].
The wound treatment is also important. The presence of an extrapulpal blood clot has been shown to interfere with healing and cause chronic inflammation and internal dentin resorption [7]. The wound surface should therefore be gently irrigated with sterile saline in order to achieve hemostasis before application of the medicament. With the increasing use of ferric sulfate as a pulpotomy medicament, achieving hemostasis is no longer a major problem. However, if persistent bleeding is observed even after the application of ferric sulfate, the diagnosis of the state of pulp inflammation should be reconsidered. After pulpal treatment, it is important to provide a tight coronal seal to the oral cavity to prevent leakage and thereby reinfection and future complications.
Stepwise excavation and indirect pulp capping
In general, a nonexposed pulp has a more favorable healing capacity than an exposed pulp. However, it has been shown recently that pulpal inflammation in response to proximal caries is more severe as compared to occlusal caries of the same depth (Figure 16.2). This should be an important consideration when planning stepwise excavation or indirect pulp capping for occlusal caries as compared to a deep proximal lesion.
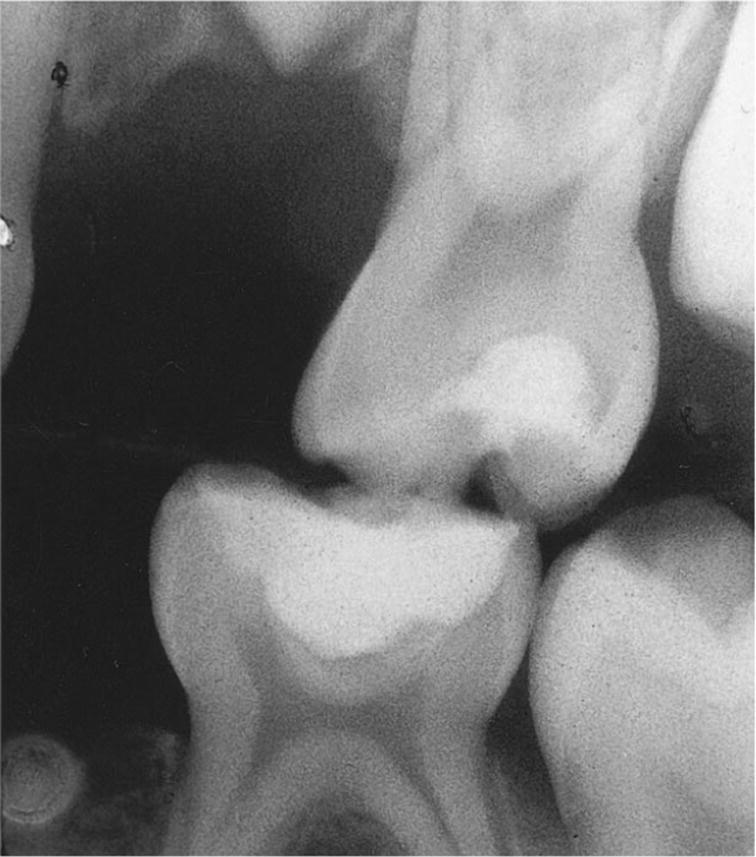
Figure 16.2 Radiograph showing stepwise excavation performed in two primary second molars in order to keep them in situ and without subjective symptoms at least until the permanent first molars are in occlusion.
In the authors’ opinion a more radical approach is often required for a deep proximal lesion as compared to one in an occlusal surface. This is important to consider when treating extensive carious lesions, where an exposure of the pulp may be expected if all carious dentin is removed. If this is expected in proximal caries then a pulpotomy would probably be the preferred option, whereas for occlusal caries, in the same situation, a more conservative approach could be adopted in the absence of any patient symptoms suggestive of pulpitis. Severe caries in first primary molars might lead to poor prognosis for the tooth, and for this particular tooth, extraction should be considered as an alternative to stepwise excavation or any pulp treatment.
The stepwise excavation technique includes removal of most of the soft carious dentin, application of a glass ionomer liner, and sealing the cavity with a semi‐permanent material such as a resin‐reinforced zinc oxide–eugenol cement or glass ionomer cement. The tooth is left for at least 3–6 months, while secondary dentin formation continues, which means less or no risk of exposing the pulp when re‐entering the cavity for final removal of carious dentin and restoration of the tooth [9].
Although stepwise excavation is included in this chapter for the sake of completeness, it is not recommended as a favored approach for the treatment of deep caries in primary molars. The technique requires a second appointment with further administration of local anesthetic to the child. In such cases, if an assessment of pulp inflammation indicates that the patient has reversible pulp inflammation then a one‐visit indirect pulp capping should be considered, with an excellent coronal seal such as a stainless‐steel or an esthetic crown such as zirconia crowns that are widely available these days.
Direct pulp capping
Direct pulp capping is a technique that involves covering the exposed healthy pulp with a medicament, preferably calcium hydroxide, without any surgical intervention. Direct capping should not be considered in primary molars where removal of all caries has resulted in a pulp exposure. The reason is that it has been shown that inflammation of the pulp in primary molars precedes the exposure of the pulp [10,11]. Due to the wide dentinal tubules in primary molars, bacteria penetrate the pulp before it is clinically exposed, causing inflammation. By the time the pulp is clinically exposed, inflammation is usually too extensive for healing to occur with pulp capping, and an inflamed pulp needs to be removed before restoring the tooth. The only situation where direct pulp capping could be considered in primary teeth is where the pulp exposure is traumatic and not due to caries.
Partial pulpotomy
Partial pulpotomy is the treatment of choice only for primary molars with healthy pulps or partial chronic pulpitis (Figure 16.3). However, the diagnosis can be difficult to establish. Partial pulpotomy should be considered in very limited situations where the operator is certain that pulp inflammation is localized to the area just below the site of the exposure. This can be judged by taking a thorough history to assure absence of any signs of pulpitis. Clinically normal bleeding should be observed after the removal of the inflamed pulp from just below the exposure site, and this bleeding should be easily controlled by application of gentle pressure with a cotton pledget. In case more extensive and difficult‐to‐control bleeding is observed, a full coronal pulpotomy should be performed.
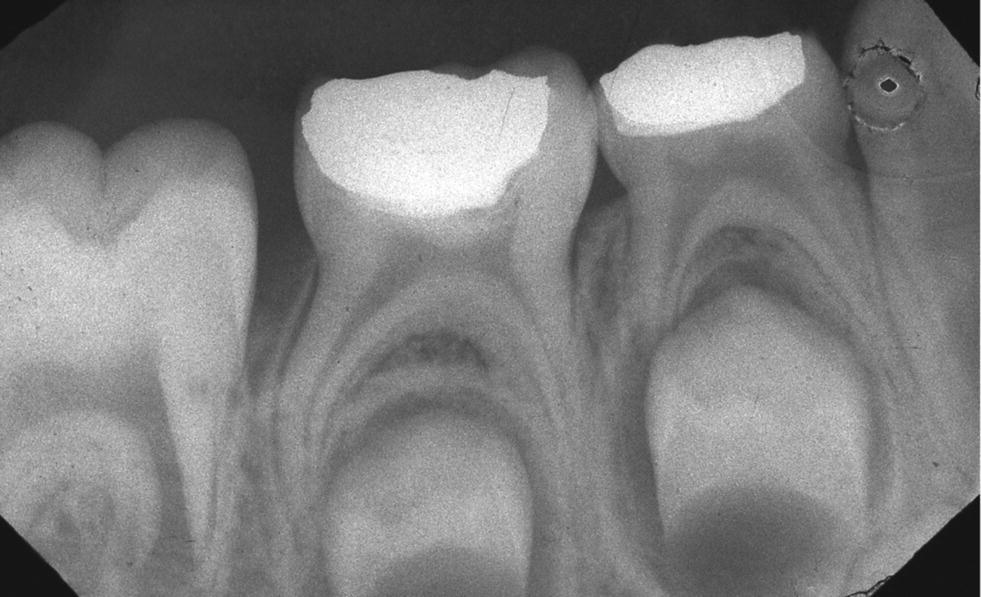
Figure 16.3 Radiograph of primary second molar after partial pulpotomy. The hard tissue barrier indicates wound healing; note absence of periradicular pathology.
The technique includes removal of a small part of the pulp just at the site of exposure using high speed and a diamond bur during irrigation with water in order to avoid traumatizing the pulp. Until relatively recently, application of calcium hydroxide on the wound was preferred, but high failure rates have been observed with this material. Nowadays, mineral oxide aggregate (MTA) is considered to be a more biological material for use on the pulp, and many clinicians now prefer its use. The tooth is restored to establish a good coronal seal.
Pulpotomy
Pulpotomy, or vital amputation of the coronal pulp, includes removal of all of the coronal pulp (Box 16.4). The surgical technique and the treatment of the wound are the same as described for partial pulpotomy, but the wound surface is placed at the orifices of the root canals.

VIDEdental - Online dental courses


