14 The Measurement of Oral Disease
EPIDEMIOLOGY: AN INTRODUCTION
Heredity has received a lot of recent attention with the rapid growth of molecular epidemiology, that is, the application of the techniques of molecular biology to epidemiology. DNA typing has been used to identify the genotype of pathogenic microorganisms, and viral DNA can be measured in host cells and their genomes.13 DNA typing can also identify the genotypes of people who are especially susceptible to certain diseases. Molecular epidemiology holds enormous potential for disease control during the twenty-first century.
We should remember, however, that this is not the first time in history that there has been great optimism about prospects for disease control. In the late nineteenth century, when the bacterial agents in many infectious diseases were being identified, the “end of disease” was confidently being predicted. The concept of disease at that time was dominated by acute, mortal infections with a single bacterial agent, and little thought was given to chronic conditions. Today we are more aware that disease is multifactorial, meaning that multiple causative circumstances can be defined for just about any disease. Heart disease, the leading cause of death in the United States, is associated with genetics, stress, diet, exercise, smoking, blood pressure, and blood cholesterol levels. So what is the “cause” of heart disease? Dental caries is of bacterial origin but is also associated with sugar consumption, fluoride exposure, saliva quality and quantity (which are likely to be genetically controlled), family education and income, and other factors in the physical and social environment. So what is the “cause” of dental caries? Within the multifactorial tangle, epidemiology attempts to identify the risk factors (see Chapter 13) associated with a disease and to determine which of them are the most important for prevention and control.
Early Studies
In 1854 John Snow, a medical practitioner in the Soho area of London, went so far as to control an outbreak of cholera by the application of his epidemiologic conclusions. His investigation took place some years before the germ theory of disease was understood, so Snow began by trying to identify the features common to those who died from the disease. After he mapped out the residences of those who had died (Fig. 14-1), his subsequent inquiries disclosed that all of the victims had used water from the same source. That source, in the days before indoor plumbing, was a pump on Broad Street (now Broadwick Street, where the site of the pump is currently occupied by a public toilet). Snow reached the rational conclusion that something in the water was responsible for the spread of the disease. Snow’s method of controlling the epidemic, still without knowing its cause, was to persuade the authorities to remove the pump handle. The epidemic soon subsided.
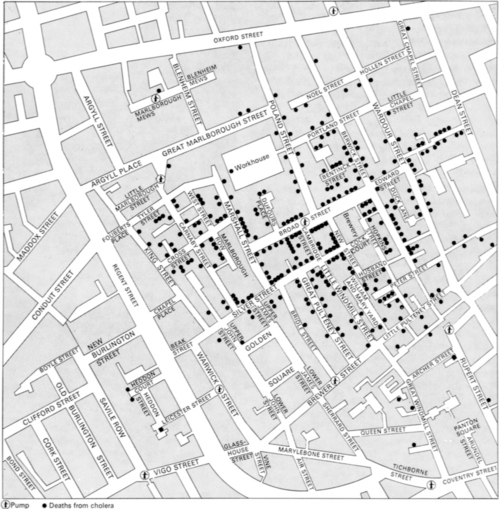
Fig. 14-1 John Snow’s map of the Soho area of London, showing deaths from cholera during the epidemic of 1854.18
(From Longmate, N. Alive and well: Medicine and public health, 1830 to the present day. Hammondsworth, Penguin, 1970.)
Snow’s subsequent investigations on the relation between cholera and the source of water supply are epidemiologic classics. The results of the patiently executed research of nineteenth-century workers such as Snow still benefit present-day society. Their investigations led to gradual but profound improvements in sanitation and personal hygiene, and the development of the public health codes for housing, water supply, and food processing that are now taken for granted. The fact that infectious diseases such as cholera, typhoid, yellow fever, plague, scarlet fever, and relapsing fever are now rare in high-income countries is not simply chance but is due largely to the pioneering work of these early epidemiologists. Their work continues today: our understanding of the mode of transmission of the human immunodeficiency virus and its translation into public health education to prevent acquired immunodeficiency syndrome followed remarkably quickly on the first identification of the virus in 1983.21,30 That, too, is epidemiology.
The types of study design used in epidemiology were described in Chapter 13 and the various uses of the epidemiologic method in research are shown in Box 14-1.
BOX 14-1 Uses of the Science of Epidemiology
The Concept of Measuring Disease
The good clinician thinks in qualitative terms. During a diagnostic examination the dental practitioner not only looks for existing disease but also tries to look ahead to the possibility of future disease. Measuring the oral health of a population, however, requires a more standardized and objective approach. Specific diagnostic criteria, written explicitly for clinical, radiographic, microbiologic, or pathologic examination, provide an objective framework for the practitioner’s judgment. These criteria are applied to judge the condition of the oral tissues as they are at examination time, not as they might be in the future. This objective application of diagnostic criteria is the most important philosophical difference between the epidemiologic examination and the examination carried out for treatment planning.
Acute diseases, such as measles, are characterized by a sudden onset of symptoms, so that the patient progresses rapidly from a state in which the disease is clearly absent to one in which the disease is clearly present. Remission of the acute phase of the disease is equally rapid, so little time is spent in the “gray areas.” Chronic diseases, however, are usually characterized by a much slower onset. It is difficult to establish exactly when arthritis, alcoholism, mental illness, dental caries, and periodontitis become definitely established; there is a considerable gray area. In dentistry this problem is handled by counting as lesions only those that meet specific criteria.
SAMPLING FROM HUMAN POPULATIONS
Examples of representative sampling are found in the national surveys of the health status of the United States population carried out continuously by the National Center for Health Statistics (http://www.cdc.gov/nchs). Obviously no one project can physically examine or ask questions of all 280 million or so Americans, so sampling is required. The process itself is compl/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


