Chapter 14
Denture Lining Materials
14.1 Introduction
Denture lining materials are of several types and are used for a variety of reasons. Occasionally, the fitting surface of an acrylic denture needs replacement in order to improve the fit of the denture. In this case, there are two options. Either the whole of the denture base can be replaced with fresh heat curing acrylic resin, or a lining of a self-curing resin may be applied to the fitting surface of the existing base.
Sometimes it is necessary to apply a very soft material to the fitting surface of a denture in order to act as a ‘cushion’ which will enable traumatized soft tissues to recover before recording an impression for a new denture.
Some patients are unable to tolerate a ‘hard’ denture base and must be provided with a ‘permanent’ soft cushion on the fitting surface of the denture.
The materials which satisfy the various requirements listed above can be classified into three groups:
14.2 Hard reline materials
The materials discussed in this section are those products which are used to provide a chairside reline to the denture. The method should be distinguished from laboratory relining and rebasing techniques which involve replacing most of the denture base resin with fresh, heat cured polymer.
Composition: The materials are generally supplied as a powder and liquid which are mixed together. Table 14.1 gives the composition of the two types of material in common use. The major difference between the two types is that the liquid in the type 1 material contains methylmethacrylate monomer, whilst the liquid of the type 2 material contains butylmethacrylate monomer. Both type 1 and type 2 materials may be classified as autopolymerizing resins and will readily polymerise at room temperature or mouth temperature.
Manipulation: The normal procedure is to ‘relieve’ the fitting surface of the denture by grinding away some of the hard acrylic denture base. The powder and liquid of the hard reline material are then mixed in the recommended proportions to give a fluid mix of material. This is applied to the fitting surface of the denture which is seated in the patient’s mouth whilst still fluid. The reline procedure must be undertaken using a ‘closed mouth’ technique in which the patient’s denture or dentures are inserted into the mouth and the patient is then asked to close into gentle contact. Care needs to be taken to ensure that the dentures maintain an appropriate relationship to the underlying alveolar ridge. Both of these steps are designed to prevent major positional or occlusal errors being produced in the relined dentures. The reline material soon becomes rubbery and the impression of the patient’s soft tissues is recorded. The denture is then removed from the patient’s mouth and allowed to bench cure. Setting may be accelerated by placing the denture in warm water or using a combination of warm water and pressure in an appropriately designed pressure vessel. The materials are not allowed to remain in the patient’s mouth throughout setting since the exothermic heat of reaction may cause an unbearably high temperature rise. The relined denture is normally ready for trimming and polishing within 30 minutes.
Table 14.1 Composition of typical hard reline materials.
| Type 1 | Powder | |
| Polymer beads | Polymethylmethacrylate | |
| Initiator | Benzoyl peroxide | |
| Liquid | ||
| Monomer | Methylmethacrylate | |
| Plasticizer | Di-n-butylphthalate | |
| Chemical activator | Tertiary amine | |
| Type 2 | Powder | |
| Polymer beads | Polyethylmethacrylate | |
| Initiator | Benzoyl peroxide | |
| Liquid | ||
| Monomer Pigments |
Butylmethacrylate or isobutylmethacrylate or some other higher methacrylate monomer |
|
| Cross-linking agent | Di-methacrylate | |
| Chemical activator | Tertiary amine |
Properties: The major disadvantage of the type 1 materials is that they involve direct contact between the oral soft tissues and a fluid mixture of reline material containing methylmethacrylate monomer. The latter material is known to be irritant and may also sensitize patients who may then suffer allergic responses in the future. The advice offered by some manufacturers, to smear the soft tissues with petroleum jelly prior to recording the impression, is probably inadequate.
The type 2 materials contain butylmethacrylate monomer in the liquid component. This is known to be a far less irritant substance than methylmethacrylate.
Both type 1 and type 2 materials have low values of glass transition temperature (Tg). The reasons for this are the presence of plasticizer in type 1 materials and the use of higher methacrylates (ethyl and butyl) in the type 2 materials. This may lead to increased dimensional instability in the relined denture, particularly if the existing hard base has been significantly relieved in order to accommodate the lining.
The reline materials are often porous due to air inclusions during mixing of the powder and liquid. The initial fluidity of the mix, coupled with a relatively rapid increase in viscosity during setting at atmospheric pressure, ensure that it is difficult to eliminate voids. This is often considered unsightly and may affect patient acceptance. In addition such a porous surface will be more likely to become contaminated with oral debris and be colonized by micro-organisms including Candida albicans, and will be more difficult to clean.
One criticism of the direct reline materials is that the dentist has little control over the thickness of the lining achieved and therefore over the ‘height’ of the denture. A reline to the fitting surface is usually undertaken to improve denture stability/retention, not to correct an occlusal error nor to modify the vertical relationship between the dentures. The ‘cushion’ of relining material can result in a marked increase in thickness of the denture base and infringement of the freeway space that is normally present between the dentures with the jaws at rest. Furthermore, there is no guarantee, even when using a closed mouth technique, that an antero-posterior positional error or lateral cant is not produced during this procedure, either as a result of poor operator technique or a greater bulk of lining material on one side of the mouth compared with the other. Such errors are highly undesirable.
A final problem is an increase in thickness of the ‘palate’ of an upper denture using this technique which patients often find unacceptable.
It follows that the direct reline materials should be considered as only a temporary or at best semipermanent solution to the problem of an ill-fitting denture.
14.3 Tissue conditioners
Tissue conditioners are soft denture liners which may be applied to the fitting surface of a denture (see Fig. 14.1). They are used to provide a temporary cushion which prevents masticatory loads from being transferred to the underlying hard and soft tissues. These materials should undergo a degree of plastic flow for 24–36 hours after mixing to allow for soft tissue changes once ‘trauma’ has been removed and to capture the shape of the supporting tissues in function as opposed to a static or unloaded relationship.
Tissue conditioners have several applications. For example, when the soft tissues have become traumatized due to wearing an ill-fitting denture the dentist would like the tissue to recover before recording impressions for new dentures. Ideally, the patient would refrain from wearing his denture for a period, but this is not popular. In these circumstances, a layer of a cushioning tissue conditioner on the fitting surface of the denture will enable the soft tissue to recover without depriving the patient of their dignity.
Tissue conditioners are often applied to the dentures of patients who have undergone surgery. This reduces pain and helps prevent traumatization of the wound. They are also useful when a tooth or teeth are being added to a denture as an immediate procedure (very shortly after the extraction). The dental technician modifies the cast of the patient’s mouth by removing the teeth that will be extracted and by estimating the amount of change in soft tissue contour. If this estimate is wrong there can be a large gap between the denture base and the socket. A tissue conditioner can be used to fill this gap to assist with stabilization of the prosthesis at the time of insertion of the immediate denture.
Fig. 14.1 Showing a tissue conditioner applied to the surface of an upper denture.
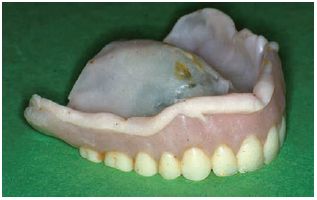
Another application of tissue conditioners is as functional impression materials. A layer of tissue conditioner in the fitting surface of the denture enables a functional impression to be obtained over a period of a few days.
Requirements: Tissue conditioners should remain soft during use in order to maintain an adequate cushioning effect on the underlying soft tissues. The material should be resilient in order that masticatory loads are absorbed without causing permanent deformation of the lining. Paradoxically, when the materials are being used to obtain a functional impression a degree of permanent deformation under load is required. This enables the impression of the soft tissues to be altered during normal function.
Composition: The materials are normally supplied as powder and liquid components (see Fig. 14.2) which are mixed together. Table 14.2 gives the composition of a typical product. The relative amounts of solvent and plasticizer as well as the type of plasticizer used vary significantly from one product to another. These variations control the softness and elasticity of the set material. Commercial products contain from 7.5% to 40% alcohol in the liquid component, whilst the plasticizer is normally a phthalate or benzoate ester. The powder may be pigmented to give a pink coloured lining similar to that of a pink denture base. It is more common, however, for the powder to be unpigmented, giving a white lining which is easily distinguished from the pink denture base.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


