Chapter 14
Brow Lifting
Introduction
The brow lift is an integral part of any cosmetic surgeon’s armamentarium as a tool to address the upper one-third of the face. Since its inception, many different variations of the traditional coronal lift have developed. This includes variation in incision placement, plane of dissection, treatment of the brow elevator and depressor muscles, and flap fixation, among other things. The prudent practitioner is familiar and competent in performing multiple techniques as no one technique can be applied to all patients. The following will include a brief discussion of the history of the brow lift followed by epidemiology. The process of the brow aging and patient evaluation will then be discussed followed by the pertinent face and brow anatomy. Finally, the salient features of the different techniques to rejuvenate the upper facial third will be discussed, including ancillary treatments. Lastly, the potential complications will be reviewed with insight on prevention and treatment.
History
The earliest description detailing brow lifting in the literature was by Passot dating back to 1919.1 This involved direct elliptical incisions with primary closure in the pretrichial area to obtain the lift. In 1926, Hunt published a technique resembling an open approach where a coronal incision was made both in the hair-bearing and pretrichial areas with subsequent subgaleal undermining and excision of excess skin.2 Due to the temporary nature of these results, adjunctive measures were sought over the next 50 years to overcome the relapse. These included surgical transection and chemical ablation of the frontal branch of the facial nerve, which resulted in unacceptable brow ptosis and loss of brow animation.3 As it was recognized that one factor causing relapse was the activation of the forehead musculature, the frontalis, corrugator and procerus myotomy, myectomy, and galeotomy evolved. Additionally, ligaments and adhesions were identified in this region that limited elevation. Vinas is credited with recognizing the requirement for extensive undermining and release of these “adhesions” around the orbital rims.4 Pitanguy was one of the first authors to describe fixation.5 In the late 1970s and early 1980s authors began describing acceptable and stable results utilizing different dissection planes from the subgaleal plane. These new techniques included the subperiosteal and subcutaneous planes of dissection.6,7 In the early 1990s, the first published reports of endoscope-assisted brow lifts appeared.8–10 Early enthusiasm waned with reports of relapse, leading to the application of fixation to this technique. Since then modifications and hybrid techniques have evolved including dual-plane dissection utilizing an open and endoscopic approach and limited access techniques from the temporal incision or a transplapebral access. As with any surgery that encompasses many different techniques to treat a common defect, controversy continues to remain regarding the most effective access, dissection plane, treatment of brow depressors, and fixation. Again, and as stated previously, the effective cosmetic surgeon must have many tools to treat the variety of patients with which he or she will be presented. As surgical advances continue, so will the evolution of the brow lift.
Epidemiology
According to the American Association of Cosmetic Surgery Procedural Census in 2009, the forehead lift has become significantly more popular as a rejuvenating procedure for the face. Its performance frequency has increased 19% over the last 4 years and is one of the top five most commonly performed procedures by these physicians. The mean age for the patient presenting for the brow lift was 53 years old for an average fee of $4080.00.11
This trend is not echoed in the American Society of Plastic Surgeons Procedural Data where this procedure has experienced a 33% drop in performance frequency over the last 4–5 years. The average fee quoted in this data for this service is $3155.00 and is most commonly performed on patients older than 40 years of age.12
Although there are many variants of error in collecting and interpreting this data, it would appear that patients are seeking a broader range of surgical professionals, outside those surveyed in the American Society of Plastic Surgeons, to provide this surgery. Alternatively, less plastic and reconstructive surgeons are offering these procedures.
Aging of the Upper Facial One-Third
The ideal brow has been studied and described based on multiple anatomical relationships. Westmore described the aesthetic brow as one where the arch of brow apex peaks corresponding to the lateral limbus below.13 The female hair-bearing brow should be at or above the supraorbital rim, whereas the male brow can be located at or inferior. The medial brow is club shaped and located at or slightly below the lateral brow to which it tails off with a lateral slant.14 The length of the brow is determined by boundaries drawn between a line tangential from the ala to the medial canthus and also between the ala and the lateral canthus.15 The brow should be greater than around 2.5 cm above the midpupil.16 The ideal height of the forehead is 5–6 cm from the eyebrow to hairline, shorter in females and longer in males.17 The male brow is thicker and flatter and tails much more gently. Higher arched brows are more common and desirable in individuals of Hispanic, Latin, and Mediterranean backgrounds.18 Nevertheless, these ideal contours vary considerably when it comes to overall esthetics and beauty. Models in fashion or glamour magazines frequently display a more horizontal brow and are still considered extremely feminine and “attractive.”
The process by which the brow produces an aged appearance is complex and multifactorial. There are both extrinsic and intrinsic factors that affect skin elasticity, fat deposit distribution, ligamentous attachment, and muscle activity including hypertrophy and or atrophy (Table 14.1). Extrinsically speaking, one of the primary factors is actinic damage but others include nutrition, exposure to chemicals, particularly with smoking, and of course gravity. Intrinsic factors include hormonal changes, genetics, sex, ethnic background, and the basic senile breakdown of the physiological capacity for the body to repair itself. As so eloquently put by Knize, “the vicissitudes of life” cause activation of the muscles of facial expression, especially grief, which potentates problems in the upper facial third.
Table 14.1 Intrinsic and extrinsic factors in brow aging
| Extrinsic factors | Intrinsic factors |
| 1. Actinic damage 2. Gravity 3. Chemical exposure 4. Nutrition |
1. Sex and hormonal changes 2. Genetics 3. Ethnic background 4. Senile physiology |
In the upper third of the face, the deleterious effects of the intrinsic and extrinsic factors on the skin including the dermis, and the retaining ligaments of the brow, coupled with the muscular tone of the brow elevators and the depressors, facilitate the aged brow position and forehead appearance. As we age, dermoelastosis and actinic damage cause the skin to become atrophic and inelastic. The epidermis undergoes thinning with disorganization of the dermal collagen and elastin fibers. This results in skin laxity and predisposition to wrinkling. Skin changes, in addition to loss of subcutaneous brow fat and volume depletion, lead to forehead and brow ptosis. The frontalis compensates, leading to hyperactivity and hypertrophy of this muscle. This results in dynamic and static horizontal forehead rhytides. Much in the same fashion, the corrugator, depressor, and orbicularis form vertical and oblique rhytides in the glabellar region, while the procerus produces a “bunny line” or horizontal wrinkle at the nasal radix.
According to Knize, the factors leading to lateral brow descent include the anterior inferior descent of the temporal soft tissue and the preseptal fat pads over the deep temporalis fascia laterally, the decrease in the resting tone of the frontalis, and the hyperactivity of the corrugator and orbicularis.19 Additionally, the frontalis has a variable length of insertion but typically ends along the temporal fusion line, which correlates along the brow with the junction of the medial and lateral one-thirds. The lack of frontalis activity laterally is one factor that leads to increased ptosis in the area. Finally, as suggested by Matros et al., the appearance of lateral brow ptosis may in fact be relative. The medial brow could remain at the same level or be elevated in approximately 70% of patients due to frontalis hyperactivity and absence of the orbital retaining ligament found laterally.20
Patient Evaluation
Regardless of the aesthetic position of the brow or lack thereof, the patient’s complaint is what should be treated. As previously noted, there is not only much variation in the ideal brow position with age, sex, and ethnicity but also variation in individual patient opinion. The surgeon should never be so narcissistic as to treat the brow to “societal norms,” but should listen to the patient’s complaint to produce a successful result and also avoid unrealistic expectations.21
Patients presenting for evaluation most commonly complain of an inappropriate facial expression indicating sadness or grief. These patients also commonly initially present for a blepharoplasty as they do not realize the primary problem may lie above in the brow. Thus, it is always important to evaluate the brow and the upper eyelids. Upper eyelid skin laxity can lead to hyperactivity of the frontalis to suspend the excess lid tissue. Reduction of the blepharodermatochalasia can actually result in worsening of the brow ptosis as the stimulation of excess upper lid skin for frontalis tone is removed. Thus, the brow should be evaluated with the patient in animation and at rest.
Once the patient has established realistic expectations and surgical candidacy, the next step is to determine the best approach through a thorough evaluation. There are a number of findings that can help to direct the most effective approach (Table 14.2). These include brow position medially and laterally, the forehead shape and height, the quality of the skin, and the location and severity of the rhytides. Also included is the shape of the anterior hairline and the density and character of the hair. Finally, the upper eyelids must be assessed.
Table 14.2 Brow lift patient evaluation
| Brow lift patient evaluation |
| 1. Medial and lateral brow position and form 2. Forehead height and form 3. Location and severity of rhytides 4. Skin quality 5. Hairline morphology and density 6. Upper eyelids 7. Symmetry |
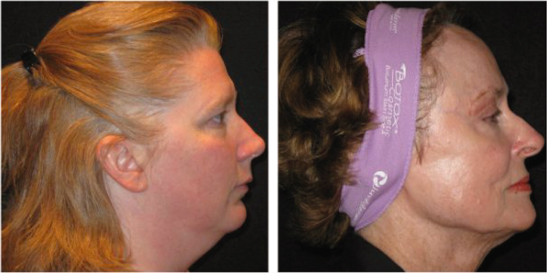
The coronal and endoscopic techniques will lengthen the forehead, while the trichophytic and direct techniques will shorten it. Additionally, a long and convex forehead makes the endoscopic instrumentation difficult (Figure 14.1). The thickness or thinness of the anterior hairline will dictate how well the scar will be hidden for a trichophytic incision and can also dictate how well alopecia will be tolerated should it occur. Thicker skin with deeper rhytides may respond better to a more superficial dissection than a subperiosteal lift. Severe brow laxity, >2 cm, may lend itself better to direct skin excision, whereas laxity less than 1 cm may make a subperiosteal lift difficult. Lastly, if the problem primarily lies only in the lateral brow, a limited temporal approach may be all that is needed.
Figure 14.1 Favorable versus unfavorable forehead anatomy for endoscopic brow lifting. Compare the short straight forehead on the left with the long curved forehead on the right.
Anatomy
Fascial Planes
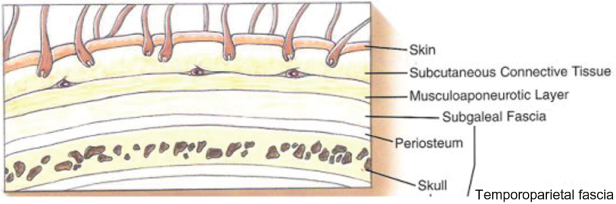
A complete review of head and neck anatomy of this region is beyond the scope of this text; therefore, the pertinent anatomy is given. The scalp is formed by five layers including the skin, subcutaneous tissue, frontalis or aponeurosis, loose areolar plane or subgaleal plane, and the pericranium (Figure 14.2). The skin and subcutaneous tissue are adherent to the galea. This slides over the loose subgaleal tissue providing movement over the periosteum when the frontalis is contracting. The galeal tissue envelops the frontalis to form a superficial and deep galeal layer, which then fuse back together with the periosteum 1 cm above the supraorbital rim. The superficial galea envelops the brow depressors. The periosteum is an inelastic layer, while those layers above it are quite mobile.
Figure 14.2 Fascial planes of the scalp.
(From Ellis EE, Zide MF. Surgical Approaches to the Facial Skeleton. Philadelphia: Lippincott Williams and Wilkins, 1995.)
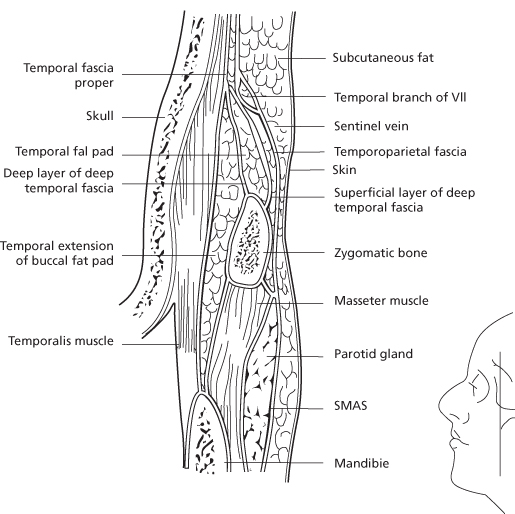
Critical nerves and vessels will be encountered at different locations depending on the selected plane of dissection. From cranial to caudal, the pericranium develops into the deep temporal fascia in the temporal region and the parotidomasseteric fascia in the face. The galea aponeurotica develops into the temporoparietal fascia, otherwise known as the superficial temporal fascia in the temporal region and the SMAS in the face. Most of the soft tissue vascular supply runs superficial to this layer, while motor innervation runs on its deep surface (Figure 14.3). The superficial temporal, supratrochlear, and occipital vessels form a rich vascular network superficial to the galea send branches to deeper layers where they anastamose with the middle meningeal artery.22 The subcutaneous plane is a relatively vascular plane, while the subgaleal and subperiosteal planes are relatively avascular dissections.
Figure 14.3 Fascial planes of the temporal area and face.
(From Trinei FA, Januszkiewicz J, Nahai F. The sentinel vein: an important reference point for surgery in the temporal region. Plast Reconstr Surg 1998;101(1):27–32.)
Frontal Branch of the Facial Nerve
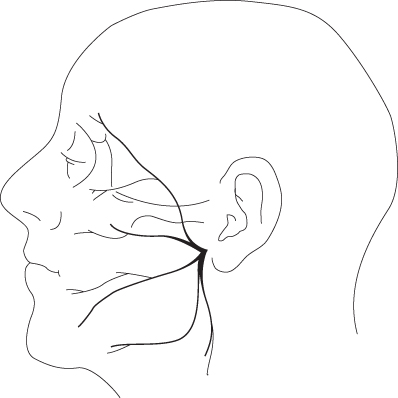
This nerve with the zygomatic branch arborizes to provide motor innervation to the frontalis, procerus, corrugator depressor supercilii and orbicularis. The temporal branch of the facial nerve leaves the frontozygomatic division in the parotid and travels roughly from an area 5 mm inferior to the tragus to 1.5 cm above the lateral eyebrow or the lateral extent of the lowest horizontal brow rhytid.23 It crosses the zygomatic arch between 8 mm and 3.5 cm anterior to the external auditory canal, usually an average of 2 cm.24,25 At this level, it is located on the undersurface of the temporoparietal fascia (Figure 14.4). It travels anteriorly and superiorly to innervate the frontalis from its undersurface around 2 cm superior from the superolateral orbital rim.26 According to a study by Lettieri, the nerve is always found to run parallel with the temporalis fibers it crosses over.27
Figure 14.4 Branches of the facial nerve. Notice the path of the temporal branch.
(From Trinei FA, Januszkiewicz J, Nahai F. The sentinel vein: an important reference point for surgery in the temporal region. Plast Reconstr Surg 1998;101(1):27–32.)
Sentinel Vein
This is a vessel originally described by De La Plaza as a group of vessels which pass through the temporoparietal fascia, deep temporal fascia, and temporalis lateral to the superolateral orbital rim in the frontozygomatic area. The sentinel vein has a consistent location and relation to the frontal branch of the facial nerve and this is really its value. In the recumbent position, the sentinel vein is 1.5 cm above and lateral to the lateral canthus.28 Some authors feel skeletonization of the structure is necessary to ensure release of the appropriate adhesions in the endoscopic lift.18 The frontal branch of the facial nerve is usually found cephalad to the sentinel vein ranging from 2–9 mm at an average of 6.4 mm.25 As astutely pointed out by Lettieri though, utilizing the skeletonization of the sentinel vein as a safety net to avoid trauma to the frontal branch is problematic as dissection from above to identify and skeletonize this vessel may lead to a traction injury to the frontal branch itself.27
Supraorbital and Trochlear Nerves
The supraorbital nerve is found around 2.7 cm lateral from the midline. Cuzalina and Holmes found it to approximate the medial limbus of the iris29 (Figure 14.5). It usually exits the rim from a notch but has been found in up to 10% of patients exiting a foramen up to 2–4 cm above the rim. It typically has two branches, superficial and deep30 (Figure 14.6). The superficial division is generally unharmed during surge/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


