Children with special needs
Neeta Prabhu, Wendy J Bellis and Angus C Cameron

Introduction
Although the oral health of people with disabilities is similar to the rest of the population, it is generally accepted that many persons with disabilities have extensive treatment needs, which for a variety of reasons, are not adequately met. Throughout the world, the standards of oral healthcare for this population have failed to achieve what would normally be expected for those without a disability.
What is special care dentistry?
It is a discipline targeted to meet the needs of individuals with a variety of limitations that require more than just routine dental care.
A disability may be:
Barriers to care and philosophies of management
Access to dentistry is often influenced by:
• The attitudes and willingness within the dental team to treat special needs children.
• A perception that the clinician may not have the skills or have the facilities to manage their care.
The successful management of these children depends fundamentally on the dentist’s ability to:
Consent
Providing dental care for people with cognitive impairment who are unable to consent to treatment can raise ethical and legal problems for the practitioner. There is variation in the practice of consent ranging from the ability of an individual to legally consent to their own treatment to the delegation of authority to their parents, caregivers or a guardianship board. Because these ethical predicaments are not obscure, healthcare professionals who routinely care for such patients must complement their clinical skills with their ability to recognize and clearly address these legal responsibilities.
Where are special needs children to be managed?
General dentists have often expressed concerns about a lack of adequate training in appropriately managing these patients in practice, leading to an increase in the number of referrals to the tertiary hospitals. While there has been an overall strategy of integration and normalization of these individuals into mainstream society, unfortunately, most have become reliant on the already stretched hospital-based healthcare system leading to extended waiting times. It must be emphasized that children with special needs require dental appointments that are tailored to make best use of their abilities. The majority of children can be managed successfully in a general practice setting with appropriate training of the dental team. All of the required preventive and maintenance programmes and much of the restorative work can be performed under local anaesthesia and/or sedation. However, there will always be a cohort for whom dental treatment under general anaesthesia is the only alternative. This incurs high costs and has its own problems of access and additional risks and should be recommended only when all other forms of behaviour management have failed or are clearly inappropriate. Additionally, the patient’s ability for oral health maintenance postoperatively must always be factored in the treatment planning process to avoid the misuse of these expensive facilities.
There is no doubt that the provision of care for many children with disabilities is challenging. Clinicians should be aware of their own limitations and should consider who and where the child is best managed.
Prevention
The best means of establishing good oral health is by a combination of early contact with dental services and increasing the awareness of regular dental check-ups. Many studies have demonstrated that certain groups of people with disabilities can be instructed in oral hygiene measures if sufficient encouragement and motivation was provided. It is important to introduce these measures from an early age and clinicians should not be deterred from providing comprehensive preventive programmes.
Attention deficit hyperactivity disorder (ADHD)
Attention deficit hyperactivity disorder (ADHD) is a common developmental disorder affecting about 3–5% of the population. The term ADHD is currently used to describe a range of children with varying functional difficulties, but who share the feature of poorly sustained attention. The exact causes remain unknown, however most theories indicate abnormalities in the brain function that are mostly genetic in origin.
Features of ADHD
Assessment
The assessment of a child for the diagnosis of ADHD requires a number of essential components including:
Management
Management of the child with ADHD involves three broad approaches:
Many other approaches are commonly applied to these children, including dietary modification, ‘natural’ or complementary therapies of diverse types and behavioural optometry, however, there is little evidence to support the broad use of any of these interventions, though some individuals report benefits.
Pharmacological management
Psychostimulant medication is the principal pharmacological therapy for ADHD. The two stimulants most commonly prescribed are methylphenidate (Ritalin) and dexamphetamine.
Dental implications
The visit to a dentist is likely to raise anxiety levels in any child and indeed their parents. In a child with ADHD, this anxiety may manifest in overexcited behaviour and many parents worry about the effect of their child’s behaviour on others. They have become accustomed to failure having taken their ‘difficult’ child to dentists only to be told that it is not possible to provide treatment/care. This may result in either an excessively protective/embarrassed parent with constant apologies on behalf of the child or else an overly firm parent exerting inappropriate, heavy-handed disciplinary actions throughout the encounter. In either situation, the child’s behaviour is likely to be reactive towards the parent, thus precluding the establishment of a successful relationship with the dental practitioner.
Successful management of these children may be facilitated using similar strategies to those employed in other disabilities.
Autistic spectrum disorder
Autism or autistic spectrum disorder (ASD) is defined as a severe developmental disorder characterized by the classic triad of impairments:
ASD is polygenic in origin, however, there are still aspects of the aetiology that are not fully understood. Approximately 50% of affected children also have moderate to severe learning difficulties and there may be other comorbidities such as Fragile X, Rett syndrome, tuberous sclerosis, PKU and epilepsy. As ASD is predominantly a genetic condition, there may be other family members who are affected, including the parents themselves.
Asperger syndrome
Asperger syndrome is a form of autism. These children have fewer problems with speaking and are often of average or above average, intelligence. They do not usually have the accompanying learning disability associated with autism, but they may have specific learning difficulties.
Problems associated with the dental treatment of a child with ASD
The dental management of children with autism can be a huge challenge for the paediatric dentist, mainly because of the child’s behaviour and their impaired communication.
Impaired communication
Impaired behaviour
Sensory problems
Many children with ASD have problems with sensory processing and consequently may be hyper- or hyposensitive to sights, sounds, smells and tastes in their environment. They may have an elevated pain threshold and are also known to restrict their diet to certain foods only. Sensory overload and anxiety can result in extreme behaviours such as ‘meltdown’.
Medication
Many medications may cause xerostomia and some may not be sugar-free in some countries.
Trauma
Injury to anterior teeth is not uncommon due to the association with epilepsy and dyspraxia.
Late diagnosis
Difficulties and delays in confirming the diagnosis of ASD often results in a delay in accessing early preventive dental care.
Problems with therapies
Linked to the huge number of proposed therapies, there may be dietary restrictions and limitations imposed on specific dental materials. Confectionery may be being used for the reinforcement of good behaviour and as part of a behavioural approach.
Clinical management
Dentists are one of the few professionals who we permit to enter our personal space. Many people find this uncomfortable but understand that the dentist needs to be so close in order to examine teeth. For children with ASD, this close proximity may well be extremely distressing.
Therefore, prevention is the key element to managing these children. Local anaesthesia and inhalation sedation is limited to the higher functioning children with autism, where their communication is not severely compromised.
General anaesthesia and deep sedation are the most frequently used approaches, especially for those children who are young and present with extensive disease. Such treatment should obviously be definitive and comprehensive, including preventive as well as curative elements.
Important tips for management
• Send out a pre-appointment questionnaire-style letter and an information leaflet.
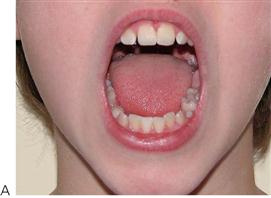
• Some echolalic children (automatic repetition of vocalizations) are able to copy words and expressions, and if this applies to the treating dentist, then the parents can be taught to encourage the child to say ‘AHHHH’. This not only helps the parent to brush, it allows the dentist to examine the teeth visually, and also facilitates examination of the pharynx by the child’s medical practitioner. The sound ‘EEEEEEE’ can help display the upper anterior gingival margins, that are sometimes difficult to access (Figure 13.1).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


