Chapter 12. Endodontic aspects of traumatic injuries
H.E. Pitt Ford
CHAPTER CONTENTS
Summary209
Introduction209
History, examination and immediate management210
Types of injury211
Effects of trauma on the dental tissues212
Auto-transplantation of an immature premolar into the incisor space223
Orthodontic treatment226
Learning outcomes226
References226
SUMMARY
Correct diagnosis and treatment planning are fundamental to successful endodontic management of traumatized teeth. The preservation of pulpal vitality in a young tooth is very important for further development and maturation, allowing the tooth to attain structural strength, otherwise it is very liable to fracture. The elimination of infection during root canal treatment is critical to achieving a successful outcome. The introduction of Cone Beam Computed Tomography (CBCT) is a valuable new development in the diagnosis of complex traumatic injuries. The efficiency of root canal treatment of non-vital immature teeth has greatly improved with the more widespread use of Mineral Trioxide Aggregate. Better illumination and magnification through the use of an operating microscope facilitates the management of complex cases, which may be best referred to a specialist centre. Clinicians should always bear in mind the possibility of non-accidental injury in cases of trauma.
INTRODUCTION
This chapter is principally concerned with the endodontic aspects of traumatic injuries of the teeth, and does not attempt to cover dental traumatology comprehensively. For this, reference should be made to a textbook on dental traumatology or to current guidelines.1.2. and 3. Since most general practitioners see only a small number of patients with traumatic dental injuries, it may be appropriate to refer the more complex injuries to a colleague with specialist experience.
When a tooth has been damaged through trauma, a good history and thorough examination are essential to ensure a correct diagnosis and the best treatment outcome. The status of the pulp of all involved teeth must be assessed, and their vitality maintained wherever possible. Many injured teeth are immature, and their development and maturation depend on maintaining pulp vitality. It should be borne in mind that vital teeth may not respond to sensitivity testing immediately after an accident. Maintaining dental pulp vitality is covered in Chapter 5.
HISTORY, EXAMINATION AND IMMEDIATE MANAGEMENT
A dental injury should always be treated as an emergency. Management of any severe bleeding or respiratory problems takes priority. Any period of unconsciousness, amnesia, headache, nausea or vomiting may indicate cerebral involvement, and the patient should be referred immediately for medical examination and appropriate care. 1,4 It is important to give a full explanation of the extent of the injury and the prognosis to anxious parents. Inconsistencies between the history and the injuries sustained, particularly if accompanied by late presentation, should alert the clinician to the possibility of non-accidental injury. 1
A full account of when, where, and how the injury occurred must be recorded. The circumstances of the accident may have legal implications and a photograph may be especially useful. The time interval between injury and presentation can influence the choice of treatment, and may be critical to the success of replantation of avulsed teeth. The place where the injury happened may suggest possible contamination of open wounds and the need for tetanus prophylaxis. The way the injury occurred may give some indication of the type and the extent. Any previous injury or treatment should be recorded. The medical history must be reviewed as this may influence treatment planning, for example, if the patient suffers from an immunological or blood disorder. The current National Institute for Health and Clinical Excellence (NICE) guidelines state that antibiotic prophylaxis against infective endocarditis is not recommended for patients undergoing dental procedures; however, it is essential to keep up to date with current guidelines and to liaise with the patient’s medical practitioner where appropriate. 5 There is further coverage on this subject in Chapter 2.
The clinical examination should include assessment of the soft tissues and facial skeleton. Disturbances to the occlusion are investigated as these may indicate jaw fracture or condylar displacement. Any soft tissue injury is noted and the possible presence of a foreign body considered; radiographic examination may be necessary to locate this. Injuries to the oral mucosa are investigated, especially bleeding from the gingival sulcus; lacerations may occur with displaced teeth; bleeding from a non-lacerated gingival margin may indicate periodontal damage. The probing depths of the gingival sulci are recorded. It should always be remembered that the effect of an injury may not be confined to the visibly affected teeth, and adjacent, apparently unaffected teeth should always be included in the examination and investigations. Infractions, fractures, pulpal exposures, mobility or displacement are noted along with any colour changes. A dark discolouration immediately after the injury indicates haemorrhage within the pulp space. There may be potential for repair and, therefore, this is not an indication for root canal treatment. If, however, the tooth becomes dark some months after the injury this usually indicates pulp necrosis. Yellow discolouration some time after the injury is associated with pulp calcification and is not an indication for root canal treatment, even if there is no response to sensitivity testing. 6 Lost pieces of fractured teeth should be accounted for; in case they are embedded in soft tissue, or have been swallowed or inhaled. Thermal sensitivity of the teeth may be a consequence of exposed dentine or pulp. Mobility and percussion testing should be carried out as they may indicate damage to the supporting tissues.
Response to pulp sensitivity testing should be recorded. Some injured teeth may have the potential to recover but may not respond for up to 2 years after trauma; 7 the results of sensitivity tests will provide a baseline for later comparison. A negative response to sensitivity testing should not, therefore, be taken as an indication for root canal treatment. Blood flow in severely luxated teeth has been shown some time ahead of their pulps responding to electric pulp testing.7.8. and 9. In assessing vitality of luxated teeth it is not unusual for the findings to be contradictory. 61 Radiographic examination of permanent teeth should include a paralleling technique periapical film of each affected tooth using a film holder to standardize projections for later comparison. For luxation injuries a further film, with the tube rotated horizontally, is often helpful. 11 If a root fracture is suspected in the maxillary incisor region an occlusal radiograph should be taken. If an immature tooth has been non-vital for some time, its development will have been arrested, leaving the pulp space larger than would be expected. For primary teeth an occlusal film alone is usually sufficient. Cone Beam Computed Tomography (CBCT) is a very valuable new development in the diagnosis of traumatic injuries; the three-dimensional picture gives much more information than a standard radiograph12.13.14.15. and 16. (Fig 12.1).
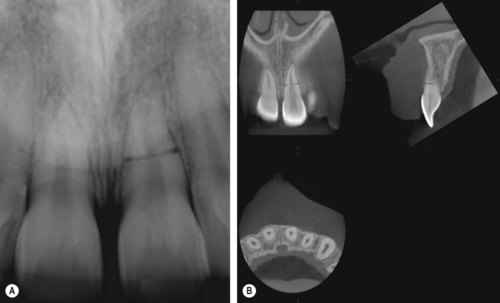 |
| Figure 12.1
Maxillary left central incisor. (A) Radiograph showing the horizontal root fracture. (B) Cone beam CT scanning gives a more comprehensive three-dimensional view of the fracture
(reproduced courtesy of S Patel).
|
Following a thorough clinical and radiographic examination, a diagnosis is made for each injured tooth. The importance of this cannot be overstated. The outcome of treatment is dependent on a correct diagnosis as inappropriate treatment may readily be initiated at this stage. 1,17 The prognosis should be considered and the value, or otherwise, of endodontic treatment determined. Newer treatment methods, such as the introduction of Mineral Trioxide Aggregate (MTA) (ProRoot MTA, Dentsply, Weybridge, Surrey, UK) have resulted in a reduced number of treatment visits, less stressful and demanding of patients who have sustained dental injury. Also, methods of strengthening the cervical region of immature teeth reduce the risk of loss through fracture (see later). A tooth is the best space maintainer and, provided it is free of infection, its retention preserves alveolar bone for later restoration.
Soft tissue injuries should be cleaned and sutured if necessary, and any tooth fragments embedded in the lips removed. Exposed dentine is covered and pulp exposures treated; displaced teeth are repositioned and splinted when appropriate. If a permanent tooth has been avulsed, the socket is irrigated with saline to remove blood clot, and the tooth replanted and splinted. These injuries are covered in more detail later. If the patient is very upset, it may be better to delay non-urgent treatment until a subsequent visit. In the case of a traumatically exposed pulp, inflammation has been shown not to extend beyond 3–4 mm after several days. 18 Unless unavoidable, it is most important not to remove the pulp of an immature tooth which has the potential for further maturation.
TYPES OF INJURY
Trauma may cause the following damage to the teeth:
• infraction of enamel
• fracture of enamel
• fracture of enamel and dentine
• fracture of enamel and dentine with pulp exposure
• crown-root fracture involving enamel, dentine, cementum and pulp
• intra-alveolar root fracture
• concussion
• subluxation
• extrusive luxation
• lateral luxation
• intrusive luxation
• avulsion.
Sudden contact of upper and lower teeth caused by, for example, a blow to the mandible can result in damage to posterior teeth. These injuries are rare but can result in a range of damage, from minimal loss of hard tissue to vertical crown-root fracture or avulsion.
EFFECTS OF TRAUMA ON THE DENTAL TISSUES
Many traumatized teeth are immature. These teeth have large pulp spaces and short, wide dentinal tubules. Infection may, therefore, readily spread to the pulp if the crown is fractured. This may lead to loss of vitality due to severance or crushing of the apical vessels during luxation injuries. The pulp of an avulsed tooth may also become infected via the apex, if contaminated. Teeth depend on a vital pulp in order to develop their potential maturity and strength. A tooth that loses its vitality while immature is always prone to fracture, especially in the cervical region of the root. 19
The cementum on the root surface may be damaged by luxation injuries; the natural repair mechanism involves limited surface resorption. However, where there is extensive damage to the cementum, ankylosis associated with replacement resorption is a frequent complication. If infection from the pulp complicates damage to cementum, then external inflammatory root resorption may be very rapid, particularly in immature teeth. 1,2
MANAGEMENT OF PRIMARY TEETH
When a primary tooth is injured, a major consideration is avoidance of damage to the successional tooth. This may occur either mechanically at the time of injury, during treatment, or as a result of infection. 1,20 Young children may not be very cooperative, particularly after a traumatic injury when the soft tissues are sore, swollen and bruised, therefore, immediate treatment may need to be limited.
Fractures
Crown fractures
Enamel fractures should be smoothed, while fractures into dentine should be covered. If the pulp has been exposed and if there is sufficient cooperation, a partial pulpotomy and restoration may be carried out with a view to preserving pulp vitality; this does not need to be at the emergency visit. 18,21 Otherwise, extraction of the tooth may be indicated. The technique of pulpotomy is covered in the section on permanent teeth. Root canal treatment of primary teeth has been covered in Chapter 11. An infected primary tooth should not be left untreated as the infection may cause damage to the permanent successor (Fig. 12.2).
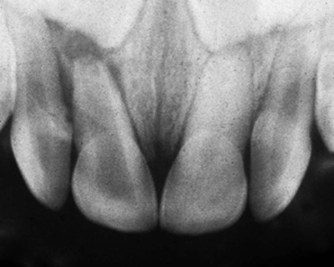 |
| Figure 12.2
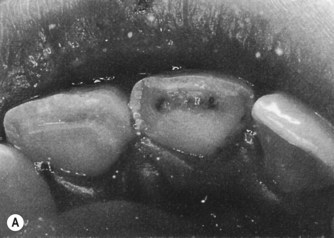
Primary maxillary central incisors that have suffered a traumatic injury. The maxillary left incisor has responded with calcification of the pulp space, while the right incisor has developed an abscess.
|
Intra-alveolar root fracture
This is less common in primary teeth than in permanent teeth. Active intervention is rarely required. If the coronal fragment is very loose and at risk of being inhaled or grossly displaced, or if pulp necrosis and infection develop, extraction is usually indicated; however, the apical fragment is normally left in situ to resorb naturally and to avoid surgical damage to the developing permanent successor.
Luxation injuries
In general, a conservative approach to management is adopted with primary teeth. Laterally luxated primary teeth are frequently repositioned naturally in time by occlusal and muscular forces. If a laterally luxated tooth interferes with the occlusion, the injury is mild and there is no risk to the permanent successor, it may be carefully repositioned. 1,22 If the root apex is directed palatally towards the developing permanent tooth then it should be extracted atraumatically. If a tooth is very mobile and in danger of inhalation, or if occlusal interference is too great, it should be extracted. Intruded teeth will usually re-erupt albeit sometimes over several months. If the pulp becomes non-vital and infected, root canal treatment may be considered (see Ch. 11). Replantation of avulsed primary teeth is not normally carried out because of the potential risk of direct physical damage to the developing permanent tooth, or damage from later infection of the pulp of the primary tooth.
Tooth discolouration
Pulp damage is a frequent complication of injuries, and as a result primary teeth may discolour. Immediate discolouration indicates bleeding in the pulp and the possibility of repair. Later darkening of the tooth signifies pulp necrosis and if there is associated infection, root canal treatment or extraction is indicated. Later yellow discolouration indicates pulp canal obliteration and no intervention is required (Fig. 12.2).
MANAGEMENT OF PERMANENT TEETH
Fractures
Infractions and fracture of enamel
Infraction of enamel rarely requires operative treatment, but the pulpal status should be monitored. Infection may very rarely enter the pulp through enamel infractions. There is no effective treatment to avoid this. Fractures of enamel may be either smoothed or repaired with composite resin. The likelihood of pulp canal obliteration or pulp necrosis occurring is low for both enamel infractions and enamel fractures. 23 The chance of pulp damage is increased if there is associated luxation of the tooth. 24
Fracture of enamel and dentine
In children, trauma to anterior teeth commonly affects sound teeth, which frequently have large pulps and wide dentinal tubules. Any injury that exposes dentine can, therefore, result in damage to the pulp. Fractures involving dentine open up numerous dentinal tubules. If left untreated, microbial plaque will grow on the exposed surface and cause pulpal inflammation, which may lead to pulp necrosis. The early placement of a restoration prevents permanent pulp damage and relieves sensitivity. The use of etched and bonded composite resin restores the appearance and does not hinder subsequent monitoring of pulp vitality (Fig. 12.3). This has been shown to seal more effectively than conventional glass ionomer cement. 25 Restoration of the contour of the tooth may be left until a later visit. A fractured fragment may be successfully reattached with composite resin retained by etched enamel. The likelihood of pulp canal obliteration or pulp necrosis occurring is low following fractures involving dentine, provided the dentine tubules are effectively covered. 1,23 The chance of pulp damage is increased if there is associated luxation of the tooth. 24,26
 |
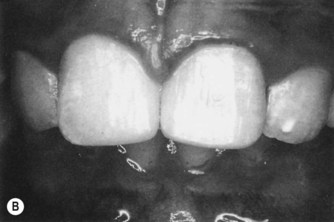 |
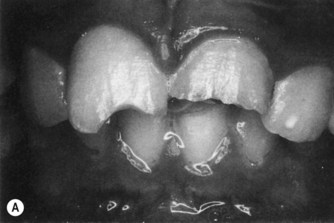
| Figure 12.3
(A) Fractured incisal edges of maxillary central incisors exposing dentine. (B) Restoration of incisal edges using composite resin retained by etched enamel.
|
Fracture of enamel and dentine with pulp exposure
Immature teeth
If this type of injury occurs in a young patient whose permanent tooth is immature, then treatment is directed at maintaining pulp vitality to allow continued tooth maturation; this considerably improves the long-term prognosis of the tooth by reducing the risk of subsequent root fracture. 19 Permanent incisor teeth have been shown to reach maturity at the age of about 13 years. The pulp can usually be treated conservatively as it has a good blood supply and rarely becomes necrotic. 27,28 Partial pulpotomy is the treatment of choice.18.27.29.30. and 31. The advantages of partial pulpotomy over pulp capping are that inflamed pulp tissue and adjacent infected dentine are removed, and that the pulp dressing is placed in a cavity where it can be covered by a protective base. If the restoration is lost, the cavity dressing should not be displaced.
Local anaesthesia is necessary to carry out a pulpotomy. The tooth is isolated with rubber dam to exclude salivary contamination; retention of rubber dam on an immature tooth is facilitated by a suitable clamp (e.g. Ash EW, Dentsply). A small cavity approximately 2 × 2 mm is cut in the fractured dentine surface at the exposure site, with the periphery of the cavity floor in dentine (Fig. 12.4). Pulp removal is usually confined to the superficial 2 mm since infection does not normally extend beyond this level. 18 The pulp is best removed with a bur in the turbine handpiece using copious water spray; this causes less damage than a bur at slow-speed or an excavator.29.30. and 32. Haemorrhage is arrested using a cotton pellet soaked in saline and the wound is covered with MTA.31.33.34.35. and 36. Over this is placed a layer of resin-modified glass ionomer cement, before restoring the tooth with composite resin. Should the composite resin be lost the restoration within the cavity should remain intact. MTA has been shown to give better results than calcium hydroxide in this situation. 31,33 Alternatively, the cavity may be restored with a calcium hydroxide base (either a slurry which is subsequently compressed and dried with cotton wool or a hard setting base material) and a resin-modified zinc oxide-eugenol cement (IRM, Dentsply) followed by glass ionomer cement.
 |
 |
| Figure 12.4
(A) Maxillary right central incisor with a fracture involving the pulp. (B) After placement of medicament in the partial pulpotomy preparation.
|
The coronal contour should then be restored with etched-retained composite resin. A hard tissue barrier should form beneath the dressing.29.30.34. and 35. The tooth should be reviewed after six months, and then at least annually for several years, to ensure continued pulp vitality by regular pulp testing, and continued root development by examination of radiographs. Should the restoration fail, it must be replaced immediately in order to prevent infection of the pulp via the pulpotomy site, as the hard tissue barrier is usually porous. 18 This treatment has a high success rate; the pulp may be expected to remain vital and healthy.18.27. and 29. There is no need for root canal treatment subsequent to pulpotomy, unless necrosis and infection develop. 32
Mature teeth
Where crown fracture of a mature tooth involves the pulp, conservative treatment by partial pulpotomy should still be considered as the first treatment option. However, where the entire clinical crown has been lost, pulpal extirpation, root canal filling and construction of a post-retained crown is usually indicated.
Crown-root fracture involving enamel, dentine, cementum and pulp
In this type of extensive tooth fracture, the coronal fragment is usually retained by a limited amount of periodontal ligament. These teeth may have a poor prognosis, especially if the fracture line is a long way subgingival on the palatal aspect. When the patient first presents, the coronal fragment is often loose and painful to bite on. It is usually necessary to give local anaesthesia to allow removal of the fragment and to assess the extent of the fracture. If time does not allow this, the fragment may be bonded temporarily to the tooth to minimize discomfort. Where the fracture does not extend far subgingivally, it is often possible to restore the tooth without crown lengthening. Otherwise periodontal surgery to expose the margin of the fracture, or orthodontic extrusion, will need to be considered. In an immature permanent tooth with an exposed pulp, where the fracture does not extend far subgingivally, pulpotomy should be carried out (as described above). Where loss of the root is more extensive, the tooth will be difficult to restore and is likely to have a poor long-term prognosis. While its loss will be planned for, in the longer term, it may be possible to carry out a pulpotomy, restoring the supragingival contour with composite resin and retain the tooth while the dentition continues to develop.
In a mature tooth where the fracture is superficial, pulpotomy may still be the first line of treatment, or it may be more appropriate to carry out root canal treatment and restore the tooth with a post-retained crown. If the fracture is deeper, it will be difficult to isolate the tooth for root canal treatment, and orthodontic extrusion of the root followed by crown lengthening will need to be considered before restoration by a post-retained crown. 1 When the fracture is very deep, there may be insufficient root remaining to support a restoration even after orthodontic extrusion; such teeth are also more likely to fail subsequently. Where the prognosis is very poor, extraction of the remaining root should be considered if it is infected; otherwise, elective decoronation may be used to preserve the alveolar ridge.
Intra-alveolar root fracture
Intra-alveolar root fractures are relatively uncommon, and fortunately, often occur without the complication of microbial contamination from the mouth. The coronal fragment may be mobile with the fulcrum coronal to the apex, and may be extrusively or laterally luxated. The tooth should be examined carefully for any periodontal injury whereby the gingival sulcus communicates with the fracture; this substantially reduces the prognosis. Diagnosis of intra-alveolar root fracture is made by radiological examination with two films, taken at different vertical angles. Root fractures are more frequently observed on an occlusal film than a film taken with a paralleling technique (Fig. 12.5). CBCT has greatly contributed to diagnosis of complex fractures, as it gives a three-dimensional view.14.15. and 16.
 |
 |
| Figure 12.5
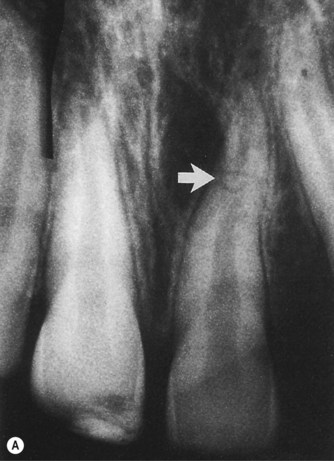
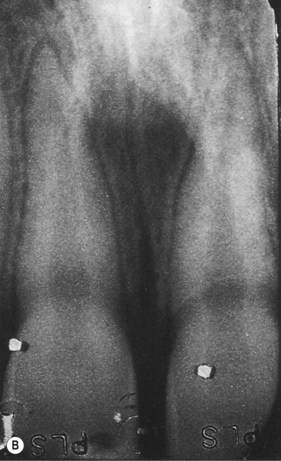
Maxillary left central incisor. (A) Part of an occlusal radiograph more easily demonstrates an intra-alveolar root fracture (arrowed) than (B) a paralleling-technique radiograph on which the fracture is more difficult to see.
|
The apical fragment almost without exception remains vital, and does not require treatment. This is, therefore, in effect a luxation injury of the coronal fragment. If there is no mobility or displacement, immediate treatment is not required and the fractured root should heal with hard tissue formation; the pulp is likely to remain vital. Teeth that have fractures remote from the gingival sulcus have the best long-term prognosis (Fig. 12.5). If the fracture is close to the neck of the tooth, the prognosis will be poorer, but extraction need not be indicated, unless there is a communication between the gingival sulcus and the fracture line. Teeth with a transverse fracture have a poorer long-term prognosis than those with an oblique fracture because of the risk of future displacement37. and Andreasen, Andreasen, Mejàre, Cvek, 2004 (Fig. 12.6).
 |
| Figure 12.6
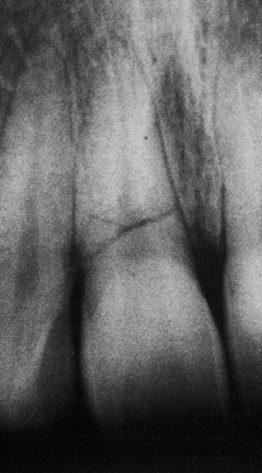
Radiograph of a maxillary right central incisor with a horizontal root fracture close to the gingival margin. The pulp responded to electric pulp testing one year after trauma; however, the long-term prognosis is poor.
|
If the tooth is displaced or mobile, immediate treatment consists of repositioning the coronal fragment and splinting if it is very mobile, typically, for approximately 4 weeks. Recent work has failed to show a correlation between splinting method, duration and healing. 38 No displacement of the coronal fragment and preserved vitality of the pulp are highly indicative of fracture healing.37.Andreasen, Andreasen, Mejàre, Cvek, 2004 and 39. A splint should allow physiological movement to avoid ankylosis. The patient is advised to use a chlorhexidine mouthwash to maintain oral hygiene, and the tooth reviewed at the time of intended splint removal. Pulp sensitivity is checked. Where there is no response, the tooth should be reviewed clinically at 3-monthly intervals. Where no vital response is obtained, provided there is no tenderness to palpation, nor a sinus tract, pulp testing should be carried out at 3 and then 6-monthly intervals either until a response occurs, or evidence of pulp necrosis appears. Radiographic review should normally be restricted to once or twice yearly unless there is a risk of external inflammatory root resorption.
The most favourable response is uniting of the two fragments by hard tissue laid down both in the root canal and on the root surface. A less favourable but still satisfactory outcome is continued pulp vitality in the coronal fragment but no union of the fragments. The sharp edges at the fracture line become rounded by remodelling, and connective tissue and/or bone lie between the fragments; the space between the fragments may increase with continued alveolar growth in younger patients. Often the pulp in the coronal fragment calcifies and radiologically shows an obliterated pulp space; the pulp may not respond to sensitivity testing. 40,41 Pulp canal obliteration itself is not an indication for root canal treatment. 1,42
Pulp necrosis occurs in approximately 20% of intra-alveolar root fractured teeth and is associated with initial coronal displacement, lack of pulp sensitivity after the accident, coronal position of the root fracture, a communication with the gingival sulcus, maturity of the root and coronal fracture.37.Andreasen, Andreasen, Mejàre, Cvek, 200439. and 41. Pulp necrosis is invariably confined to the coronal fragment. 1 As well as the loss of response to thermal and electrical stimuli, there is frequently radiolucency in the bone around the tooth at the fracture line (Fig. 12.7). Root canal treatment should be carried out in the coronal fragment alone unless there is definite evidence to implicate involvement of the apical fragment. Following cleaning of the canal in the coronal fragment, a well-packed dressing of calcium hydroxide may be placed, if required, to assist disinfection of the canal; MTA is subsequently placed in the first 3–4 mm at the fracture line, followed, if desired, by back filling with gutta-percha (see section on root filling of immature teeth for method) 35 (Fig. 12.7). This treatment has a high success rate. 43 If there is an inadequate stop at the apical end of the coronal fragment, the first 1–2 mm may be packed with calcium hydroxide, or a sterile resorbable material (e.g. Surgicel, Johnson and Johnson Medical Ltd., Gargrave, N. Yorks, UK) may be inserted to limit extrusion of MTA at the fracture site. It is not normally practical to attempt to root treat both fragments. If the apical fragment is non-vital surgical removal is indicated.
 |
 |
 |
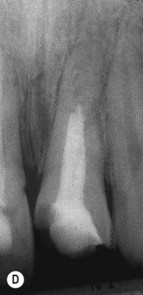 |
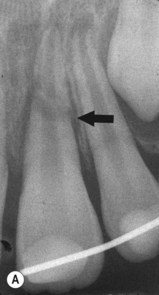
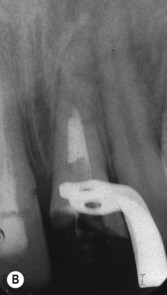
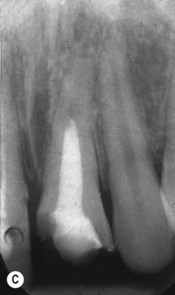
| Figure 12.7
(A) The maxillary left central incisor has a root fracture in the mid-third and has been splinted; there is a radiolucency at the fracture line (arrowed). (B) The root canal of the coronal fragment has been disinfected and filled with MTA to the fracture line. (C) The neck of the tooth has been filled with etched and bonded composite resin. (D) One year later, healing has taken place and further calcification has occurred in the apical fragment indicating that it is still vital.
|
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


