11
The index of orthodontic treatment need
Indices to assess orthodontic treatment need and outcome are not a recent development. Some have been around for over 35 years.1 Others look at specific regions of the occlusion such as the lower incisors2 while others limit themselves to the assessment of certain groups of patients.3
Since the introduction of the new National Health Service (NHS) primary care dental contract in April 2006, the index of orthodontic treatment need (IOTN) has been used to assess whether or not a patient can receive NHS orthodontic treatment. As such, all general dental practitioners are required to have a working knowledge of this index and anyone providing orthodontic treatment within the NHS must have detailed knowledge to know who they can accept for treatment and who they cannot.
A comprehensive review of all types of orthodontic index is beyond the scope of this chapter and the content will be limited to IOTN, which is currently widely used in the UK. The aim is to give the reader some background in how the index was developed and to enable application of the index in clinical practice.
DEVELOPMENT OF THE IOTN
In 1986 the UK government published a report into unnecessary dental treatment.4 Within this report, orthodontics received a lot of criticism stating that much of it was unnecessary and carried out for appearance only. As a result of this the orthodontic profession thought the development of a treatment priority index would be useful. After reviewing the literature, it was felt that an index with two components, one evaluating appearance and one evaluating dental health would be the best way forward, and details were first published in 1989.5 A modification of the index used by the Swedish Dental Health Board was used to record the need for orthodontic treatment on dental health and functional grounds. This index was modified by defining five grades, with precise dividing lines between each grade. A visual analogue scale was used to assess independently the aesthetic treatment need of the patients. This scale was constructed using dental photographs of 12 year olds collected during a large multidisciplinary survey. From this, the dental health component (DHC) and the aesthetic component (AC) of IOTN were developed.
CLINICAL APPLICATION OF IOTN
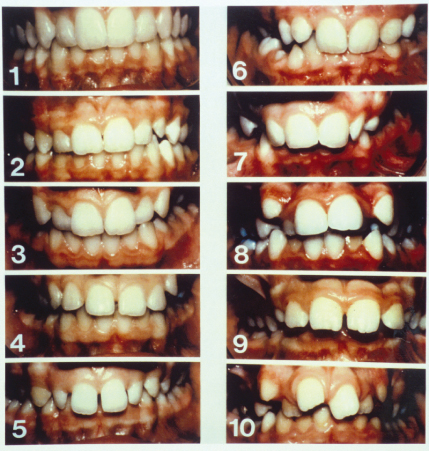
Application of the AC is very simple. The patient is asked to close the front teeth together and the examiner compares the appearance of the patient’s teeth with the visual 1–10 scale (Figure 11.1). Factors such as poor oral hygiene and fractured or discoloured teeth should be ignored. Morphological similarity should not be sought. The examiner should think what number on the AC does this patient’s teeth look ‘as bad as’ or ‘as good as’ rather than what they look like. The AC is also useful for patient counselling. Patients and parents may be invited to suggest how they think their own teeth would score on the scale. It is, however, important to note that it is the dental professional’s score that should be recorded as the AC score and not the patient’s/parent’s opinion.
Figure 11.1 The visual analogue scale used to score the aesthetic component of the IOTN.
Application of the DHC involves following a hierarchical scale using the acronym ‘MOCDO’ as a prompt. Further details can be found in the booklet ‘An introduction to occlusal indices’.6 MOCDO stands for:
- M – Missing teeth (5,4)
- O – Overjet (5,4,3,2)
- C – Crossbites (4,3,2)
- D – Displacement of contact points or crowding (4,3,2,1)
- O – Overbite (4,3,2).
The aim is to ensure the examiner surveys the dentition in a systematic manner and scores the correct grade. The numbers in parenthesis after each occlusal feature represents the DHC grade which can be given in that section. The aim is to award the highest number highest up the scale. For example, if a patient scores grade 4 in the missing teeth and overjet section, the IOTN grade relating to the missing teeth section is the one awarded. The majority of the information required to score IOTN can be found on the IOTN ruler (Figure 11.2). A comprehensive list of all IOTN grades is shown in Appendix 11.1.
Appendix 11.1 IOTN Categories: the Dental Health Component
| Grade 1 | No treatment required | |
| 1 | Extremely minor malocclusions, including contact point displacements less than 1 mm | |
| Grade 2 | Little | |
| 2a | Increased overjet >3.5 mm but ≤6 mm (with competent lips) | |
| 2b | Reverse overjet greater than 0 mm but ≤1 mm | |
| 2c | Anterior or posterior crossbite with ≤1 mm discrepancy between retruded contact position and intercuspal position | |
| 2d | Contact point displacement of teeth >1 mm but should be as symbol in 3e 2 mm | |
| 2e | Anterior or posterior open bite >1 mm but ≤2 mm | |
| 2f | Increased overbite ≥3.5 mm (without gingival contact) | |
| 2g | Prenormal or postnormal occlusions with no other anomalies. Includes up to half a unit discrepancy | |
| Grade 3 | Borderline need | |
| 3a | Increased overjet >3.5 mm but ≤6 mm (incompetent lips) | |
| 3b | Reverse overjet greater than 1 mm but ≤3.5 mm | |
| 3c | Anterior or posterior crossbites with >1 mm but ≤2 mm discrepancy between the retruded contact position and intercuspal position | |
| 3d | Contact point displacement of teeth >2 mm but ≤4 mm | |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


