Chapter 11
Automated external defibrillation
INTRODUCTION
Defibrillation is the delivery of an electrical current across the myocardium of significant magnitude to depolarise a critical mass of the myocardium simultaneously to enable the restoration of organised electrical activity. A key component in the chain of survival (see Chapter 1 and Figure 1.1), defibrillation is one of only two interventions that have been shown unequivocally to improve long-term survival following a cardiac arrest, the other being basic life support (Resuscitation Council (UK), 2011).
The modern automated external defibrillator (AED) abolishes the need for the operator to have ECG interpretation skills. Spoken and/or visual prompts guide the operator through the safe use of the AED. As minimal training is required, it can be used by a wide range of personnel, including dental practice staff. The Resuscitation Council (UK) (2012) now recommends that every dental practice should have immediate access to a defibrillator. If required, defibrillation should be undertaken by dental staff before the arrival of the paramedics.
The aim of this chapter is to understand the principles of automated external defibrillation.
VENTRICULAR FIBRILLATION
‘The cardiac pump is thrown out of gear, and the last of its vital energy is dissipated in a violent and prolonged turmoil of fruitless activity in the ventricular walls’ (McWilliam, 1899).
In ventricular fibrillation (Figure 11.1), the myocardium is depolarising at random, resulting in uncoordinated electrical activity, with subsequent loss of cardiac output and cardiac arrest. Causes include myocardial ischaemia, electrolyte imbalance, hypothermia, drug toxicity and electric shock.
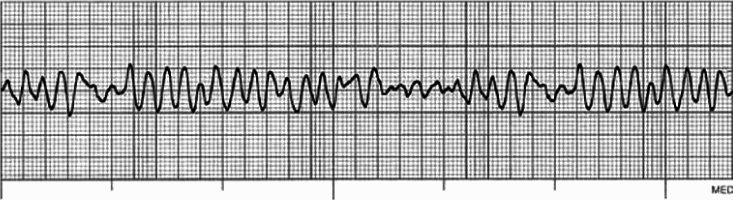
Figure 11.1 Ventricular fibrillation.
Ventricular fibrillation is the commonest primary arrhythmia at the onset of cardiac arrest in adults (Resuscitation Council (UK), 2011). It is an eminently treatable arrhythmia, with most eventual survivors of a cardiac arrest belonging to this group (Tunstall-Pedoe et al., 1992).
Early defibrillation is the definitive treatment; the chances of success decline substantially (7–10%) with each passing minute of delay to defibrillation (Waalewijn et al., 2001). There is a slower decline if there is adequate basic life support (Resuscitation Council (UK), 2011).
PHYSIOLOGY OF DEFIBRILLATION
The heart can respond to an extrinsic electrical impulse just as it can respond to an impulse from the sino-atrial node or from an ectopic focus. It is thought that successful defibrillation occurs when a critical mass of myocardium is depolarised by the passage of an electric current (Resuscitation Council (UK), 2011); if 75–90% of myocardial cells are in the repolarisation phase when the current is removed, successful defibrillation occurs and the sino-atrial node or another intrinsic pacemaker can then regain control.
Success will depend on the actual current flow rather than shock energy. This current flow is influenced by transthoracic impedance (resistance of the chest tissues), electrode position and shock energy delivered. Only a small proportion of the energy delivered actually reaches the myocardium; an effective defibrillation technique is essential to optimise the chances of successful defibrillation.
FACTORS AFFECTING SUCCESSFUL DEFIBRILLATION
If defibrillation is to be successful, sufficient electrical current needs to pass through the chest and depolarise a critical mass of myocardium. Transthoracic impedance and incorrect positioning of the adhesive pad electrodes are two key factors that can affect successful defibrillation.
Transthoracic impedance
/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


