Chapter 12
Paediatric emergencies
INTRODUCTION
Paediatric emergencies in the dental practice are fortunately very rare. However, if an emergency occurs, it is important to be able to respond quickly, effectively and safely. A sick child can deteriorate rapidly; it is most important to promptly recognise that a child is ill (ABCDE approach) and ensure appropriate help is sought. This may involve contacting the GP or calling 999 for an ambulance, depending on the situation. It is also important not to forget the child’s parents or carer as they will usually be very upset and anxious.
If the child has a cardiopulmonary arrest in the dental practice, the adult resuscitation guidelines can be followed with just a few modifications to make them more suitable for a child. Cardiopulmonary arrest will most likely be secondary to a problem either with the airway or with breathing; hence the initial importance of oxygenation and ventilation.
To avoid misunderstanding, in this chapter, the terms ‘child’ and ‘children’ refer to both infants and children; when infants and children are specifically referred to, an infant can be defined as less than 1 year and a child from 1 year to puberty.
The aim of this chapter is to provide a brief overview to the management of paediatric emergencies.
ABCDE ASSESSMENT OF A SICK CHILD
The ABCDE assessment of the sick patient has been described in detail in Chapter 3. The same approach can be adopted when assessing a child, but with some modifications and additional considerations.
Whenever possible, keep the parent with the child when undertaking the assessment. Taking the child away from the parent may cause distress. If it is necessary to administer oxygen, ideally use a paediatric non-rebreathe mask (Figure 12.1); if the child does not tolerate this, asking the parent to hold an oxygen source near the child’s face may be helpful.
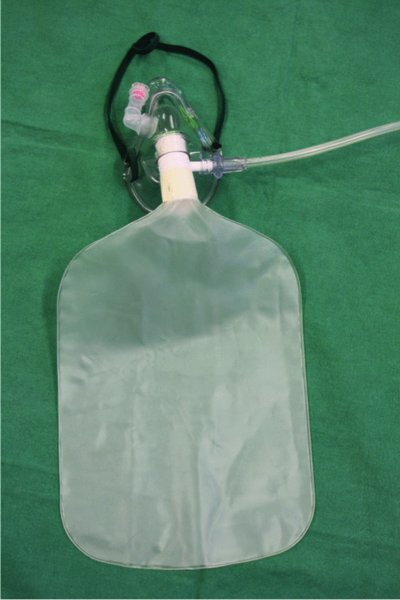
Figure 12.1 Paediatric non-rebreathe mask.
Airway
Asking an infant or small child to talk in order to confirm airway patency will not be appropriate – look for other indicators of airway patency, e.g. vocalising and crying (Resuscitation Council (UK), 2011).
Breathing
Normal respiratory rates are higher in children:
- <1 year: 30–40 breaths per minute;
- 1–2 years: 26–34 breaths per minute;
- 2–5 years: 24–30 breaths per minute;
- 5–12 years 20–24 breaths per minute;
- >12 years: 12–20 breaths per minute.
Source: Resuscitation Council (UK) (2011)
Look for chest recession or retractions (sternal, subcostal or intercostals) (indication of respiratory distress) (Resuscitation Council (UK), 2011).
Circulation
Normal pulse rates are higher in infants and children who are awake:
- 3 months–2 years: 100–180 beats per minute;
- 2–10 years: 60–140 beats per minute;
- >10 years: 60–100 beats per minute.
Source: Resuscitation Council (UK) (2011)
Disability
Assess the child’s interaction with his parents and surroundings. The parents will probably be able to advise whether this interaction is normal or not. Assess posture and tone: a seriously ill child becomes floppy.
Exposure
In any child who is unwell, look for the presence of tiny pin prick spots that can develop into purple bruising (purpuric rash) (Meningitis UK, 2013). This suggests bacterial meningitis. Try the tumbler test: press a glass tumbler against the rash – the rash will be visible through the glass and does not fade (Figure 12.2).
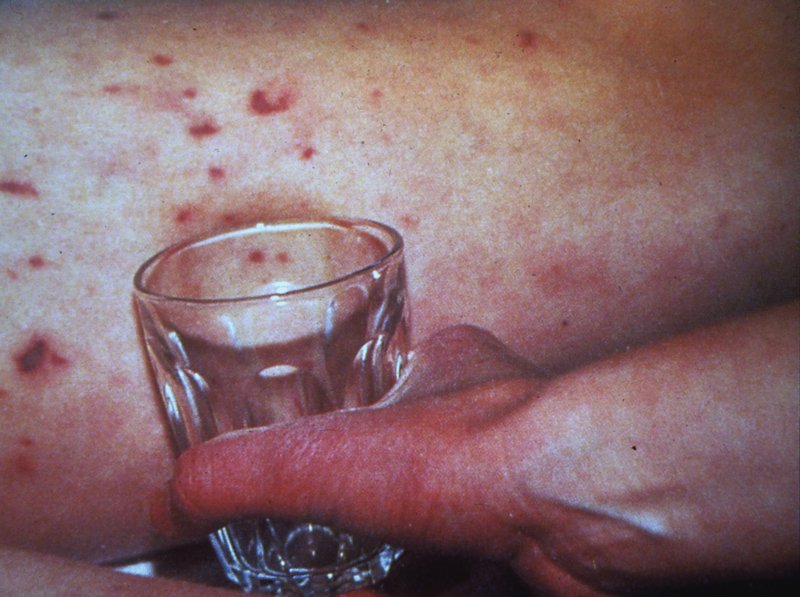
Figure 12.2 Suspected bacterial meningitis: the tumbler test. Source: Meningitis Research Foundation, Registered Charity 1091105. Reproduced with permission.
If exposing a child, take appropriate measures to minimise heat loss (particularly in infants) and respect the child’s dignity (Resuscitation Council (UK), 2011).
If possible record a core temperature, particularly if pyrexia is suspected.
PRINCIPLES OF PAEDIATRIC RESUSCITATION
When undertaking paediatric resuscitation, the adult resuscitation guidelines described in Chapter 9 can be followed, with some minor modifications (Resuscitation Council (UK), 2013). In this section, the modifications are listed, together with some background information, which the reader may find helpful.
Priorities
The two key priorities of resuscitation in children are:
- Oxygenation and ventilation: cardiorespiratory arrest in children is usually due to hypoxia (low oxygen levels in the blood);
- Effective basic life support: the most common cardiac arrhythmia is profound bradycardia (very slow heart rate) deteriorating to asystole (therefore, the defibrillator is not usually required) (Resuscitation Council (UK), 2011).
Therefore, the adult sequence of resuscitation described in Chapter 9 would not be ideal if it was followed when resuscitating a child. However, a few minor modifications would make it suitable.
Modifications to the adult resuscitation guidelines
The procedure for resuscitation in children can follow the adult resuscitation guidelines; however, four minor modifications will make the sequence more suitable for use in children (Resuscitation Council (UK), 2011; Jevon, 2012):
- Administer five initial ventilations before starting chest compressions.
- If alone, perform CPR for 1 minute before calling 999 for an ambulance.
- Compress the chest approximately one-third of its depth.
- Use two fingers when compressing the chest in an infant and in a child use one or two hands as needed to achieve the recommended depth of compression.
When to call 999 for an ambulance
As soon as it is confirmed that the child is not breathing normally, send someone to call 999 for an ambulance immediately. It is an emergency situation.
If the dental practitioner is alone (extremely rare), it is recommended to perform CPR for approximately 1 minute first before calling 999 (even if she has a mobile phone) (Resuscitation Council (UK), 2011). The rationale for this is that prompt effective CPR may actually revive the child. It may be possible, after performing CPR for approximately 1 minute, to actually carry an infant or small child to the phone and continue CPR while calling 999 for an ambulance; this is recommended by some authorities (St John Ambulance et al., 2011).
Airway management
The airway in an unconscious child can easily become obstructed by a combination of flexion of the neck, relaxation of the jaw, displacement of the tongue against the posterior wall of the pharynx and collapse of the hypopharynx; sometimes just opening the airway may revive the child (Jevon, 2009).
The airway can be open/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


