Chapter 9
Cardiopulmonary resuscitation in the dental practice
INTRODUCTION
Cardiopulmonary arrest accounts for 0.3% of all medical emergencies encountered in the dental practice (Müller et al., 2008). A recent study showed that cardiopulmonary arrest occurs in 1 in approximately 300,000 patients (Müller et al., 2008).
Effective cardiopulmonary resuscitation (CPR) and early defibrillation are the only two interventions that have been shown to improve survival following a cardiopulmonary arrest: attention must therefore be focused on these while undertaking CPR. Following guidance from the Resuscitation Council (UK) (2012), dental practices are purchasing automated external defibrillators (AEDs), thus enabling defibrillation before the arrival of the ambulance (if indicated). The procedure for using an AED is discussed in detail in Chapter 11. The principles of airway management and ventilation are discussed in detail in Chapter 10.
The aim of this chapter is to understand the procedure for CPR in the dental practice.
RESUSCITATION COUNCIL (UK) AUTOMATED EXTERNAL DEFIBRILLATION ALGORITHM
Ventricular fibrillation (see Chapter 1) is the commonest primary arrhythmia at the onset of an adult cardiac arrest outside hospital (Resuscitation Council (UK), 2011).
It is an eminently treatable rhythm, with most eventual survivors coming from this group (Tunstall-Pedoe et al., 1992). Early defibrillation is the definitive treatment; the chances of success decline substantially with each passing minute. This process can be slowed, but not halted, by effective basic life support (Resuscitation Council (UK), 2011). Effective CPR and prompt defibrillation within the first few minutes of the onset of cardiac arrest can produce survival rates as high as 75% (Colquhoun et al., 2008).
The Resuscitation Council (UK) automated external defibrillation algorithm (Figure 9.1) therefore focuses on the need to minimise any delay between the onset of cardiac arrest and defibrillation, if it is required. Until an AED is attached, only the first part of the algorithm will be followed (up to CPR 30:2). Hopefully, the dental practice will have immediate access to an AED, thus facilitating its early attachment and, if indicated, rapid defibrillation. Otherwise, CPR 30:2 will need to be performed while awaiting the emergency ambulance.
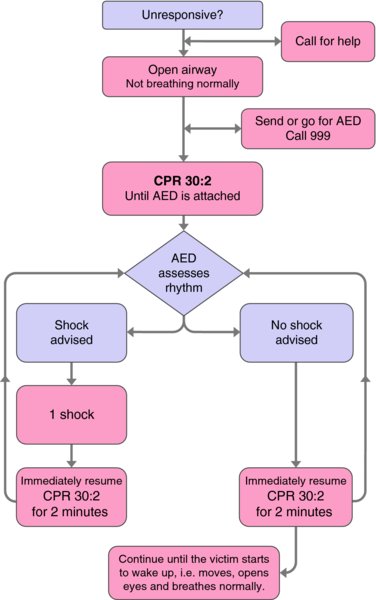
Figure 9.1 Resuscitation Council (UK) automated external defibrillation algorithm.
Source: Resuscitation Council (UK). Reproduced with permission.
Modern AEDs will be programmed to follow the current Resuscitation Council (UK) automated external defibrillation algorithm (Resuscitation Council (UK), 2012). Some older AEDs may follow previous (pre-December 2005) guidelines. Some of these devices can be simply updated in line with the current guidelines (usually with an inexpensive item of software); others will not. If the latter is the case, the user should follow the AED’s instructions (Resuscitation Council (UK), 2006).
The automated external defibrillation algorithm is designed to be an aide-memoire, reminding the practitioner of the important aspects of assessment and treatment of cardiac arrest. It is not designed to be comprehensive or limiting. Each step that follows in the algorithm assumes that the previous one has been unsuccessful. Looping the algorithm reinforces the concept of constant assessment and reassessment.
PROCEDURE FOR CARDIOPULMONARY RESUSCITATION IN THE DENTAL CHAIR
The procedures described below and the sequences in which the actions are carried out are based on Resuscitation Council (UK) (2011) recommendations and the automated external defibrillation algorithm. When more than one dental practitioner is present some of the actions described will be undertaken simultaneously. The main emphasis is on establishing as soon as possible whether defibrillation is required. Guidelines for safe handling during CPR should be followed (Resuscitation Council (UK), 2009) (see Chapter 1).
The following procedure also applies if the patient collapses on the floor, but with some modifications, e.g. chest compression technique (see Chapter 9) and ventilation technique (see Chapter 10).
Patient collapses in the dental chair
If the patient collapses in the dental chair, check whether he is responsive: gently shake his shoulders and ask him loudly ‘are you alright?’ (Figure 9.2).
- Patient responsive: try and establish the cause of the collapse. The most likely cause is a vasovagal syncope (see Chapter 7). It will probably be necessary to put the dental chair into a horizontal position.
- Patient unresponsive: follow the automated external defibrillation algorithm (Figure 9.1).
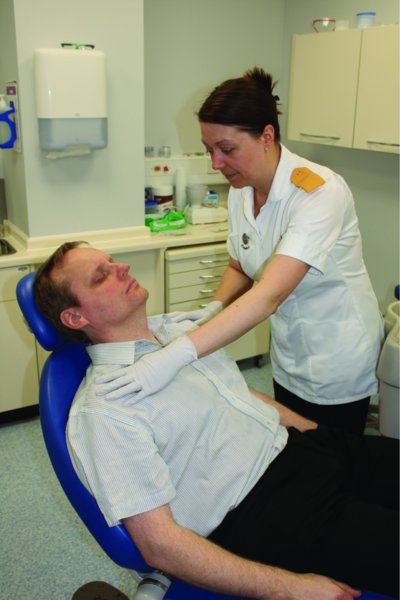
Figure 9.2 CPR: assess responsiveness – gently shake and shout.
Unresponsive
- Call for help from colleagues following local protocol. For example, this may simply involve shouting ‘help’ or shouting a certain code word such as ‘code red’, pressing an emergency buzzer or sending a message via the computer system. It would be helpful if a colleague could fetch the emergency equipment and oxygen.
- If not already done, recline the dental chair into the horizontal position. It is possible on most dental chairs to press an emergency button on the chair to activate this position.
Open airway
As the patient is unresponsive and appears to be lifeless, it is important to establish whether he has had a cardiopulmonary arrest. Open the airway and look for signs of life.
- Open the airway by tilting the head and lifting the chin.
- Ensure the airway is clear; it may be necessary to apply suction.
- While maintaining the head tilt and chin lift, assess for signs of normal breathing; look for chest movement (breathing or coughing), listen for breath sounds at the patient’s mouth and feel for air on your cheek (Resuscitation Council (UK), 2011) (Figure 9.3). During the first few minutes following a cardiac arrest the patient may be barely breathing and may be taking infrequent noisy gasps; do not mistake this for normal breathing signs of life and circulation (Handley and Colquhoun, 2010; />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


