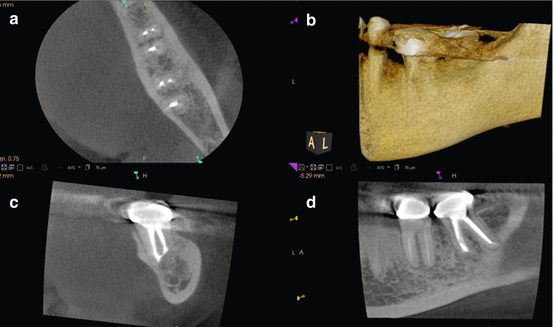
Fig. 6.1
Periapical radiographs of tooth #14, mesial and distal angles, respectively (a, b). Coronal view of the mesiobuccal root showing a missed mesiobuccal canal and periapical pathology not detected on the 2D radiograph (yellow arrow) (c). 3D reconstruction showing a crestal bony defect (blue arrow) (d). Axial view showing a previous distobuccal root amputation site (pink arrow) that was not detected on the periapical radiographs (e). (f) Sagittal view showing the crestal defect (black arrow) communicating with the periapical lesion and elevating the floor of the maxillary sinus, with no evidence of sinus perforation (f)
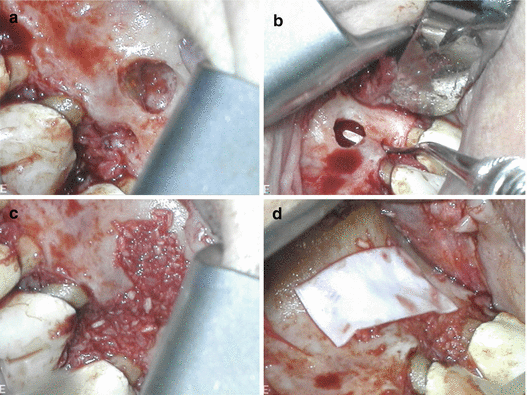
Fig. 6.2
Continuation of case presented in Fig. 6.1: clinical picture after flap reflection showing both crestal and periapical lesions (a). Communication between both defects (b). Both defects grafted with enCore™ combination allograft (Osteogenics Biomedical, Lubbock, TX) (c). CopiOs™ pericardium membrane (Zimmer, Warsaw, IN) (d)
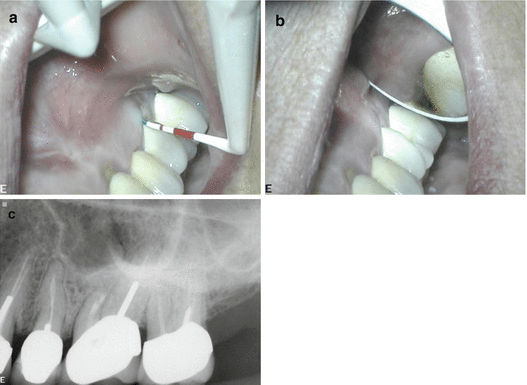
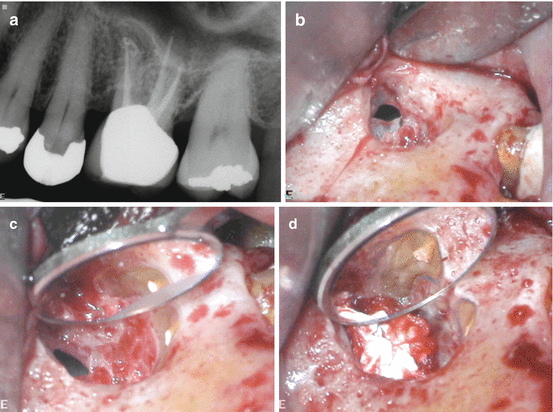
Fig. 6.4
Periapical radiograph of tooth #14 referred for periapical surgery (a). Clinical picture demonstrating sinus communication after degranulation of the defect (b, c). Clinical picture demonstrating the protection of the sinus communication with CollaCote™ and methyle ne blue staining of the MB root resection to confirm complete resection and locate the untreated mesio-palatal canal prior to ultrasonic root-end preparation (d)
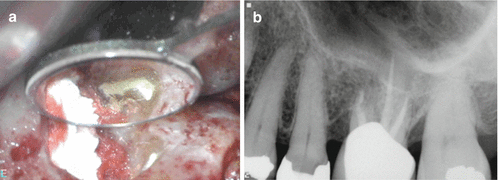
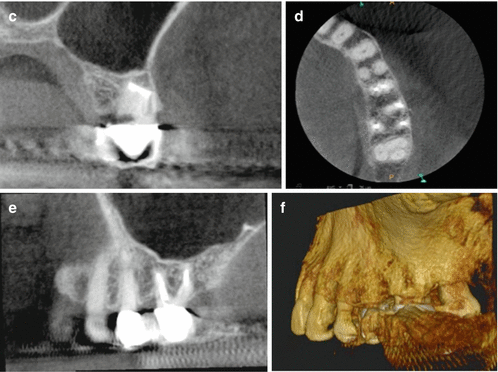
Fig. 6.5
Continuation of case presented in Fig. 6.4: root-end filling with MTA (a). Postoperative radiograph (b). 8-year recall CBCT demonstrating the coronal (c), sagittal (e), axial (d), and 3D rendering (f). Complete bone regeneration of the buccal plate as well as the floor of the sinus can be visualized
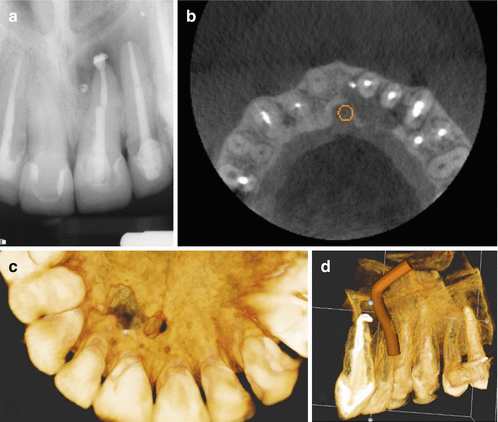
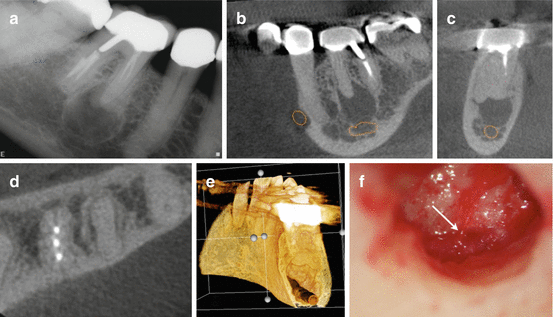
Fig. 6.6
Periapical radiograph of the maxillary anterior region showing a periapical lesion associated with tooth #9 (a). (b) Axial view showing the extent of the lesion, palatal plate perforation, and relationship of the nasopalatine neurovascular bundle to the periapical lesion (b). Palatal view of the 3D reconstruction showing perforation of the palatal plate (c). 3D reconstruction showing the nasopalatine bundle (d)
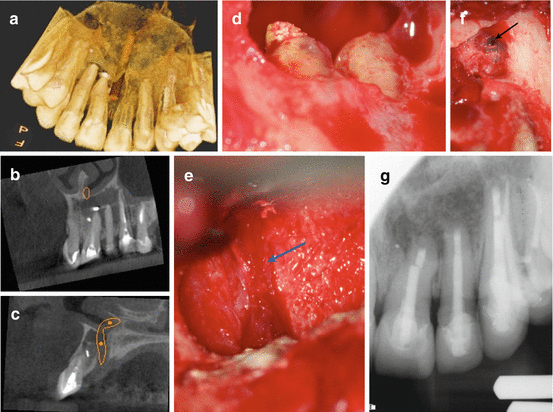
Fig. 6.7
Continuation of case presented in Fig. 6.6: palatal view CBCT reconstruction showing the exit of the nasopalatine bundle from the incisive canal (a). Coronal view showing periapical radiolucency involving teeth #9, #10, and #11 (b). Sagittal view of the exit of the nasopalatine bundle from the incisive canal (c). Periapical defect after degranulation showing the apices of teeth #9 and #10 before resection (d). (e) A clinical picture of the intact nasopalatine neurovascular bundle (blue arrow) after degranulation (e). Lateral wall of the maxillary sinus distal to tooth #11 (black arrow) (f). Immediate postoperative radiograph (g) after grafting the through-and-through defect with Puros allograft™ (Zimmer Dental, Warsaw, IN) material and CopiOs™ membrane
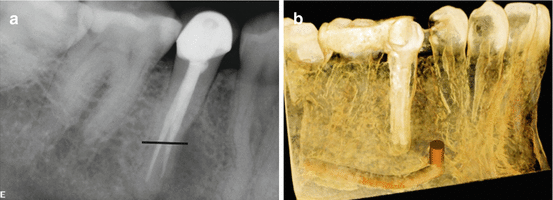
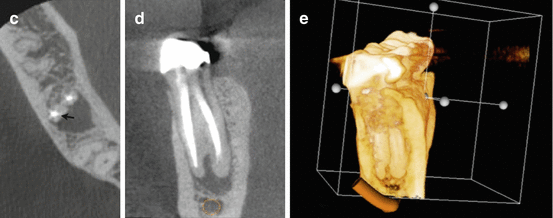
Fig. 6.8
Periapical radiograph of tooth #29 that was referred for apical microsurgery (a). The line corresponds to the level of the axial view in (c). Note the C-type-shaped canal (black arrow). 3D rendering demonstrating the relationship and proximity of the inferior alveolar nerve (IAN) and mental foramen to the apex of tooth #29 (b). Axial view of the apical 1/3 demonstrating the extent of the periapical defect (c). Coronal view demonstrating the relationship and the proximity of the IAN canal (d). 3D rendering demonstrating the relationship and the proximity of the IAN to the periapical defect as well the apex of tooth #29 (e)
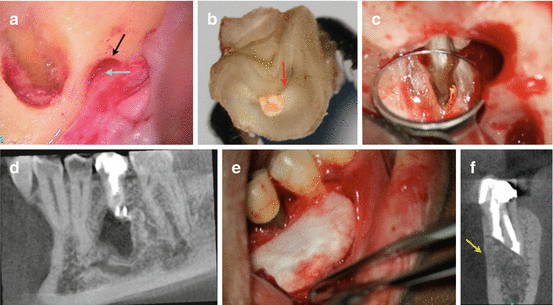
Fig. 6.9
Continuation of case presented in Fig. 6.8: clinical picture of the mental foramen (black arrow) and the neurovascular bundle (blue arrow) being identified (a). Clinical picture of the resected apex of tooth #29 after extraction and root-end resection, in preparation for root-end preparation, filling, and intentional replantation (b). Note the C-shaped anatomy which is similar to the axial view in the axial view (c). Replanted tooth after ultrasonic apical preparation of the C-shaped canal and MTA root-end filling of the apical preparation (d). Bony defect grafted with Puros™ allograft (Zimmer Dental, Warsaw, IN) and CopiOs™ membrane (e). One-year coronal view CBCT recall demonstrating complete remodeling of the defect including the buccal cortical plate (yellow arrow) (f)
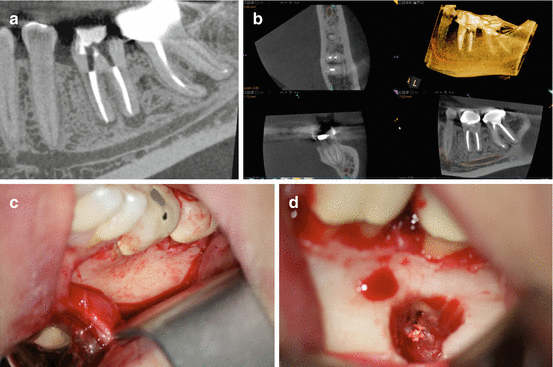
Fig. 6.10
CBCT sagittal view of tooth #18 that was referred for periapical microsurgery (a). CBCT of the axial, coronal, sagittal views, and 3D rendering demonstrating the proximity of the IAN to the mesial root of tooth #18 (b). Clinical picture after surgical flap reflection showing the buccal cortical plate (c). Osteotomy and resection of the mesial root (d)
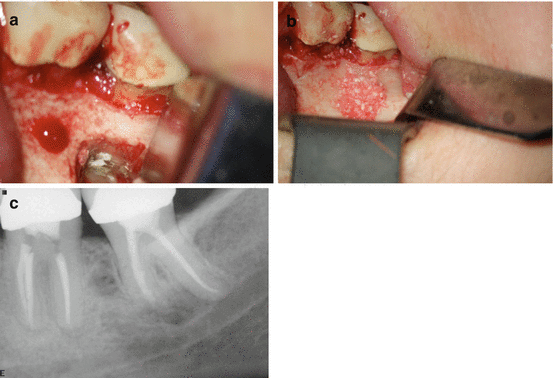
Fig. 6.11
Continuation of case presented in Fig. 6.10: clinical picture demonstrating the MTA root-end filling (a). Periapical defect grafted with Puros™ allograft (Zimmer Dental, Warsaw, IN) material and before placing CopiOs™ membrane (b). Immediate postsurgical radiograph (c)