Fig. 2.1
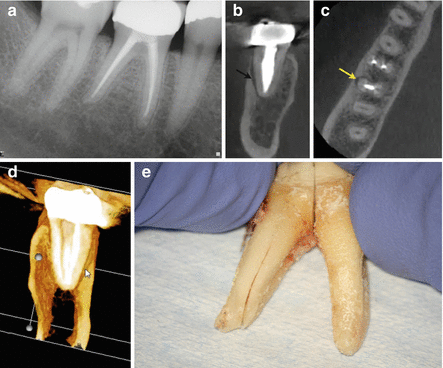
A 49-year-old male was referred for evaluation of tooth number 3 prior to fabrication of a new crown. The root canal treatment was completed approximately 15 years ago and the tooth is currently asymptomatic, periodontal probing depths are WNL, and the tooth is negative to percussion, palpation, and bite stress testing. The referring dentist wants to know if this tooth should have treatment revision or surgery prior to a new crown. The periapical radiograph (a) shows possible widening of the apical PDL on all three roots but the extent, or even definitive presence, of apical pathosis is uncertain. CBCT (b, c, and d) reveals a distinct 5.0 × 8.0-mm periapical lesion with elevation of the sinus floor and inflammatory sinus mucositis (b axial view; c sagittal view; d coronal view)
However, some caution is warranted in the interpretation of CBCT periapical findings since the CBCT-PAI score is commonly greater than the 2D PAI score, and some teeth with healthy pulps may demonstrate a widened apical PDL space on CBCT [9].
2.3 Differential Diagnosis of Pain When Etiology Is Unclear and Identification of Unusual Anatomical Relationships
Diagnosis of orofacial pain can be a challenging process for the clinician prior to and after endodontic treatment. In challenging diagnostic pain cases, the clinical and radiographic findings are often inconclusive. Inability to determine the true source of pain can be attributed in part to limitations in both pulp sensibility testing and 2D intraoral radiographic imaging (Figs. 2.2, 2.3, 2.4, 2.5, 2.6, 2.7, and 2.8).
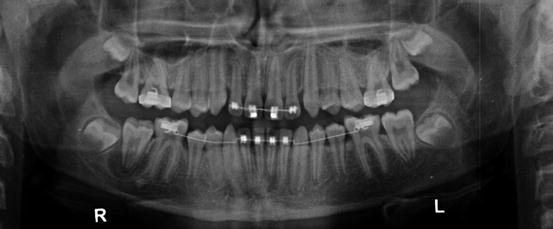
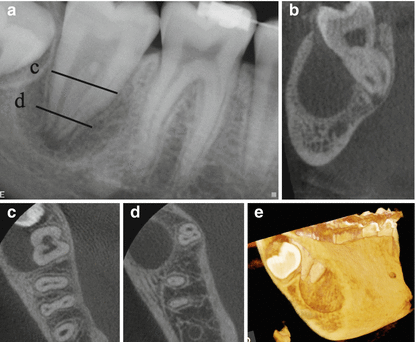
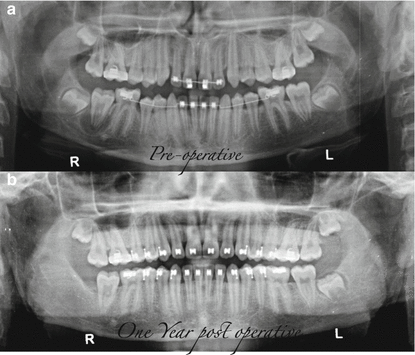
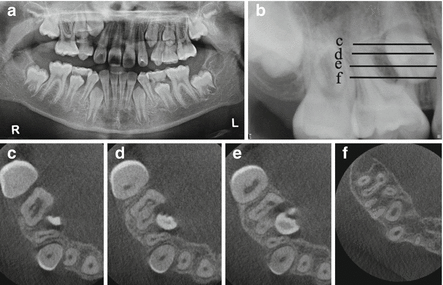
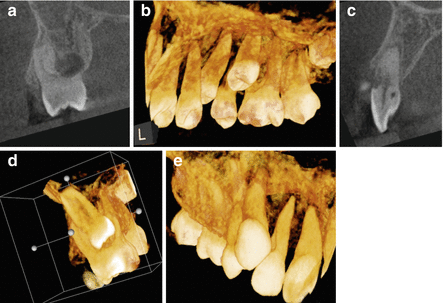
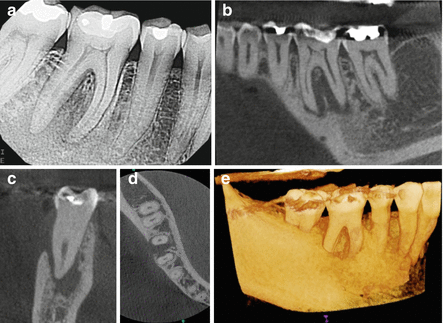
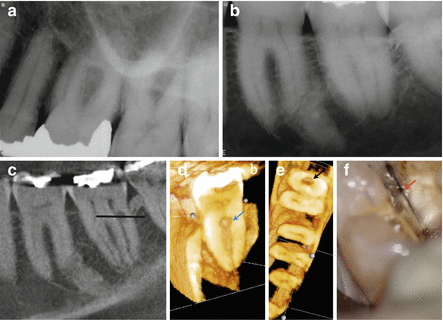

Fig. 2.2
A 14-year-old male was referred for consultation for tooth number 31. The panoramic radiograph revealed a radiolucency related to tooth number 31. The tooth responded positively to pulp sensibility tests, and periodontal probings were WNL except an 8-mm pocket on the mid-buccal surface. The patient was previously seen by two other dental specialists, and extraction of number 31 had been recommended by both

Fig. 2.3
Continuation of case from Fig. 2.2. (a) Periapical radiograph of tooth number 31. (b) Coronal view showing the buccal location of the periapical radiolucency in relation to tooth number 31. Notice the apical 1/3 of the root is surrounded by bone which explains the positive response to cold and EPT. The lines on the periapical radiograph correspond to the axial section views c and d. Axial sections c and d demonstrate the origin pf, the lesion as tooth number 32. 3D reconstruction (e) demonstrates the buccal location of the lesion and explains the isolated deep periodontal probing on the buccal aspect of tooth number 31

Fig. 2.4
Continuation of case from Fig. 2.2. Tooth number 32 was extracted and the lesion was submitted for biopsy. The biopsy result was a dentigerous cyst. Panoramic images (a) and (b) are preoperative and 1-year recall, respectively. Good bony healing around number 31 is evident

Fig. 2.5
(a) Panoramic radiograph of a 9-year-old patient that was referred to evaluate the path of eruption of tooth number 4 as part of orthodontic treatment planning. (b) Periapical radiograph of tooth number 4. The lines on the periapical radiograph correspond to the axial section views c, d, e, and f. (c–e) are the different coronal-apical cross section levels demonstrating the ectopic resorption of the mesio-palatal aspect of tooth number 3 by the cusp tip of tooth number 4. The resorptive pattern seen on the CBCT axial images cannot be detected on either the panoramic or periapical radiographs. (f) The most apical cross section showing no resorption at that level

Fig. 2.6
Continuation of case from Fig. 2.5. (a) Coronal view of the mesial furcation of tooth number 3 demonstrating the resorptive defect in the furcation and mesio-palatal aspect. (b, d) are 3D reconstructions demonstrating the same pattern from the palatal and mesial views, respectively. (c) Sagittal view of tooth number 7 demonstrating resorption caused by the ectopic eruption of tooth number 6. (e) 3D reconstruction demonstrating the relationship between teeth numbers 6 and 7. The information obtained from this CBCT scan will have a significant impact on orthodontic treatment planning

Fig. 2.7
A patient was referred for evaluation and treatment of tooth number 30. Patient presented with pain to percussion and no response to cold testing. Periodontal probing depths were WNL. Root canal therapy was indicated based on 2D radiographic findings and clinical tests. (a) Periapical radiograph of tooth number 30. (b) is a sagittal view of tooth number 30. A periapical radiolucency involving both mesial and distal roots as well as the furcation was detected. The lingual bone is still intact which gives the impression of greater bone volume and density in the furcation in the periapical (2D) radiograph than is actually present. (c) Coronal view of the distal root demonstrating complete loss of buccal bone. Due to the tight gingival attachment, periodontal probing was WNL. (d) Axial view demonstrating buccal plate perforation that cannot be detected from the 2D radiograph. (e) 3D reconstruction demonstrating the actual endo-perio defect. Considering the unfavorable prognosis for resolution of the extensive endo-perio lesion, extraction was recommended

Fig. 2.8
Patient presented for diagnosis of non-localized pain on the left side. (a, b) Periapical radiographs of the maxillary and mandibular posterior quadrants were inconclusive. All vitality, periodontal, and palpation tests were WNL. Tooth number 14 was slightly tender to percussion. A local anesthetic test was performed by administering 1.7 ml of 2 % lidocaine with 1:100,000 epinephrine via buccal infiltration to tooth number 14. The pain was not relieved. CBCTs were taken for both maxillary and mandibular quadrants. (c) Sagittal view of tooth number 18 demonstrating an internal resorptive defect in the distal root. The horizontal black line in (c) represents the axial section in (e). 3D reconstruction of the cropped distal root showing the extent of the resorptive defect in a coronal view (d – arrow) and axial view (e – arrow). (f) Clinical image of a crack (arrow) that extends into the distal canal
Persistent pain following root canal therapy or other therapeutic dental interventions can present a diagnostic challenge. Atypical odontalgia (AO), atypical facial pain (AFP), and persistent dentoalveolar pain (PDAP) are often used interchangeably to describe orofacial pain of uncertain etiology, although PDAP seems to be emerging as the preferred term [10, 11]. The diagnostic yield of intraoral radiographs and CBCT was evaluated in the differentiation between patients presenting with apical periodontitis and suspected PDAP without the evidence of periapical bone destruction. CBCT imaging detected 17 % more teeth with apical bone loss (apical periodontitis) than intraoral radiographs [12].
2.4 Detection of Cracked Teeth and Root Fractures
Two-dimensional radiographs (2D) are of limited value for the diagnosis of vertical root fractures (VRF) and usually only provide indirect evidence of the presence of a VRF. The three-dimensional nature of complex tooth anatomy and surrounding structures can make interpretation of 2D images challenging and unreliable (Figs. 2.9, 2.10, 2.11, 2.12, 2.13, 2.14, and 2.15).
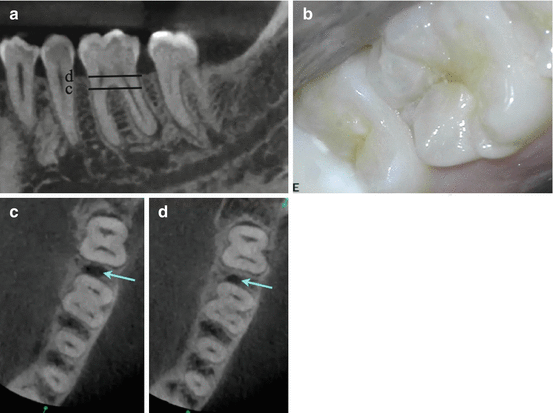
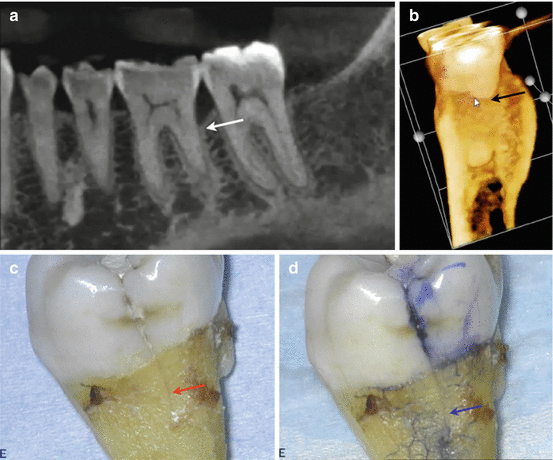
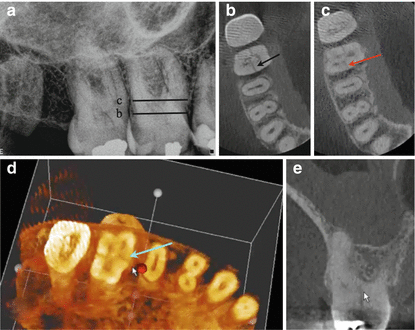
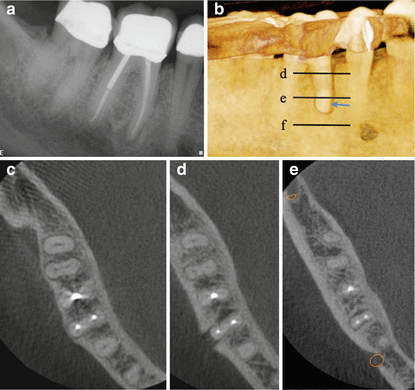
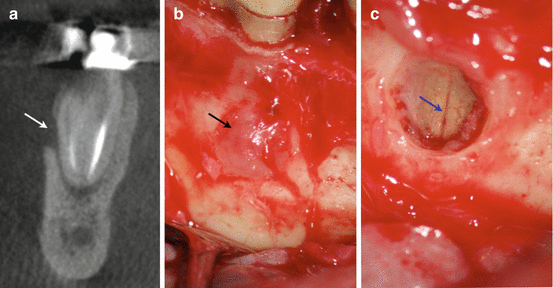
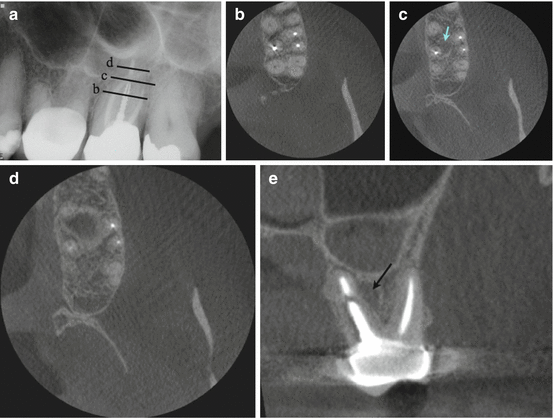

Fig. 2.9
Patient presented for evaluation and treatment of tooth number 19. The chief complaint was pain on biting and sensitivity to hot drinks. Clinical findings: no response to cold and positive response to bite stress testing. A diagnosis of a necrotic pulp and symptomatic apical periodontitis was established. The presumed etiology was extension of a distal marginal ridge crack. (a) Sagittal view of tooth number 19 showing a distal root periapical radiolucency. The lines on the sagittal view correspond to the axial section views (c) and (d). (b) Clinical image (occlusal view) demonstrating the distal marginal ridge crack. Axial views (c) and (d) demonstrate the distal bone loss associated with the fracture (blue arrows) and unfavorable prognosis

Fig. 2.10
Continuation of case from Fig. 2.9. (a) Sagittal view demonstrating an angled distal bony defect (white arrow). (b) 3D reconstruction view demonstrating the angled distal bony defect seen in (a) (black arrow). (c, d) show the extracted tooth before and after staining the longitudinal distal root fracture (red and blue arrows)

Fig. 2.11
(a) Periapical radiograph of tooth number 3. The patient presented complaining of pain to cold and biting. Periodontal probing depths were WNL. Lines correspond to the axial sections in (b) and (c). (b) and (c) are axial views showing the extent of the fracture (black and red arrows in (b) and (c), respectively). (d) 3D reconstruction, axial view of (c) showing the mesial-distal crack (blue arrow). (e) A coronal view demonstrating extension of the fracture into the furcation

Fig. 2.12
(a) Periapical radiograph of tooth number 30. (b) 3D reconstruction demonstrating the mid-root buccal defect (arrow). Lines correspond to the axial section views (c), (d), and (e). Note axial view demonstrating the mid-root buccal bone loss in (d)

Fig. 2.13
Continuation of case in Fig. 2.12. (a) Coronal view demonstrating the mid-root buccal bone loss (arrow). Surgical exploration was performed to confirm the presence of a vertical root fracture. (b) Note the granulation tissue at mid-root level (arrow). (c) Surgical degranulation of the defect demonstrating the vertical root fracture in the mesial root (arrow)

Fig. 2.14
(a) Periapical radiograph of tooth number 14. The three lines correspond to the axial section views in (b), (c), and (d). Note mid-root radiolucency (c) in relation to the palatal root at the apical level of the post (blue arrow). Intact palatal bone was observed coronal and apical to the mid-root level (b, d). (e) Coronal view showing the distal-buccal and palatal roots of number 14. The arrow demonstrates the lateral radiolucency in relation to the palatal root. Vertical root fracture of the palatal root was determined and patient was referred for extraction