Fig. 7.1
Periapical radiographs can be suboptimal in representing complex anatomy compared with CBCT. A 71-year-old male presented with discomfort in the maxillary right quadrant. (a) Periapical radiograph shows an area of low density in the middle third of the palatal root (arrow) and an impacted third molar. Clinical testing revealed pulp necrosis. CBCT images of the (b) cross-sectional reformation, (c) axial reformation, and (d) sagittal reformation show features consistent with external inflammatory resorption of the palatal root (arrows) and a periradicular periodontitis, which could not be localized in the periapical radiograph. The excessive pressure from the impacted third molar may have caused the resorptive defect. The maxillary sinus within the CBCT image has features consistent with chronic sinusitis. The tooth was non-restorable and extraction was recommended. The CBCT image data was used to assess the position of the maxillary right third molar for surgical planning
External inflammatory root resorption is a common complication of dental trauma, affecting up to 18 % of patients after luxation injuries of all types [19] and up to 30 % of replanted avulsed teeth. External inflammatory resorption after trauma is a well-known complication after intrusive luxation injuries and replantation of avulsed teeth, progresses quickly, and is radiographically distinguished by cavitation-like areas of low density along the root surface and surrounding alveolar bone.
CBCT provides improved assessment of the presence and type of root resorption, especially in the apical third of the root [20] (Fig. 7.2). Simulated external resorption in 131 cavities using single-slice CT scans showed higher sensitivity and excellent specificity in the detection of resorption in small cavities in the apical 1/3 of extracted human incisors [21]. Laboratory studies using extracted teeth with simulated resorptive lesions [12, 22] suggest that CBCT provides high sensitivity and specificity in the detection of simulated resorptive lesions on mandibular incisors. However, these ex vivo studies do not exactly replicate the clinical situation, where changes in the supporting structures such as the periodontal ligament and surrounding bone may have influenced the result. In addition, the synthetic resorption cavities in the teeth studied were created with round burs that may not have accurately replicated the irregular nature of some resorptive lesions, which may have influenced detection.
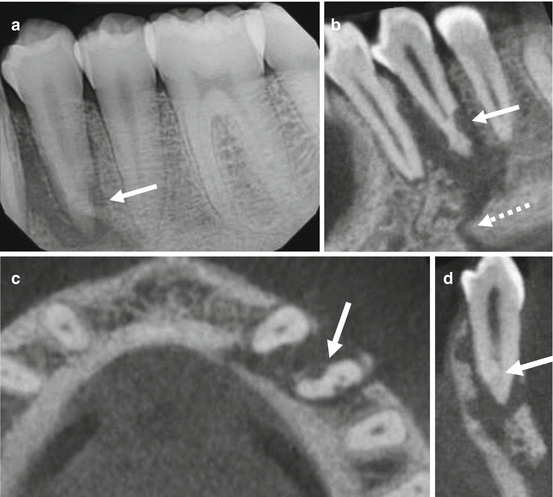

Fig. 7.2
A 21-year-old male presented for evaluation and possible treatment with a history of trauma to the mandibular left quadrant. The left mandibular body fracture was directly fixated for 6 weeks prior to endodontic evaluation. (a) Periapical image shows an area of low density associated with the mandibular left first premolar. This feature extends laterally and apically. There is a well-defined area of low density on the distal aspect of the apical third of the root (arrow); a feature consistent with external inflammatory resorption. CBCT images of the (b) sagittal reformation demonstrates the full extent of the lesion, which is contiguous with the fracture line (dashed arrow). (c) A separate area of low density (arrow) shows on the mesial aspect in the axial reformation. (d)There is an apical split of the canals visible in the cross-sectional reformation
The advantages of serial cross-sectional imaging have been well documented in the orthodontic and endodontic literature [23]. Several ex vivo studies in the orthodontic literature have demonstrated the advantages of CBCT in the detection of root resorption in maxillary teeth in close proximity to impacted canines [24]. External apical root resorption in orthodontics is estimated to affect at least one root in 94 % of patients investigated [25].
Diagnosis and management of external cervical resorption (Fig. 7.3) is challenging to diagnose and manage and is most commonly associated with orthodontic treatment, dental trauma, cervical restorations, and/or bleaching [26]. This type of resorption is characterized by a circular lesion that progresses in a coronal and apical direction (Fig. 7.4). The root canal is not invaded in the early phases. External cervical resorption may be distinguished from caries by a “non-sticky” feel upon exploration. A pink area may be noticed by the patient or clinician, a result of vascular granulation tissue visible through the resorbed dentin. Two-dimensional radiographs may not show the full extent of the lesion nor the portal of entry, complicating treatment. CBCT shows the extension of the lesion and assists with the determination of the expected outcome and location of important anatomic structures to facilitate a surgical approach, if indicated. According to Heithersay, orthodontic treatment was potentially related to 24.1 % of external cervical resorption cases studied, with a time to diagnosis of between 1.5 years and 33 years and predilection for maxillary canines, maxillary incisors, and mandibular molars. External cervical resorption was also associated with trauma and bleaching, with 15.1 % and 7.4 % of teeth involved, respectively [26]. Many case reports of multiple idiopathic external cervical resorption have been published, with the number of teeth involved ranging from 5 to 24 per patient. While there was no unique region of the mouth that was affected, 13 of the 18 patients were female [27].
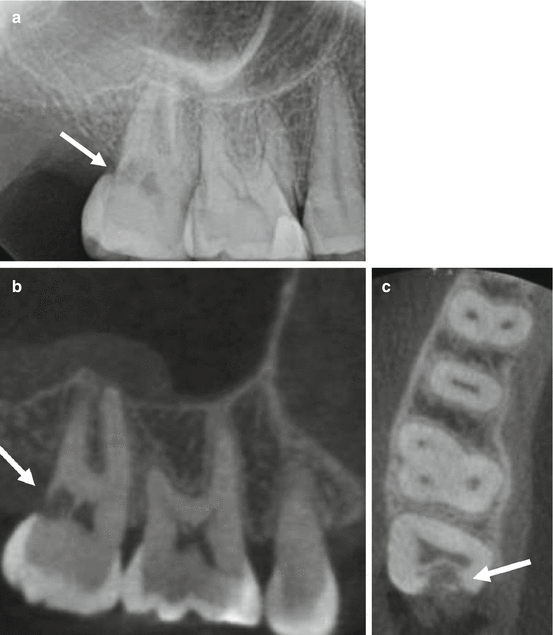
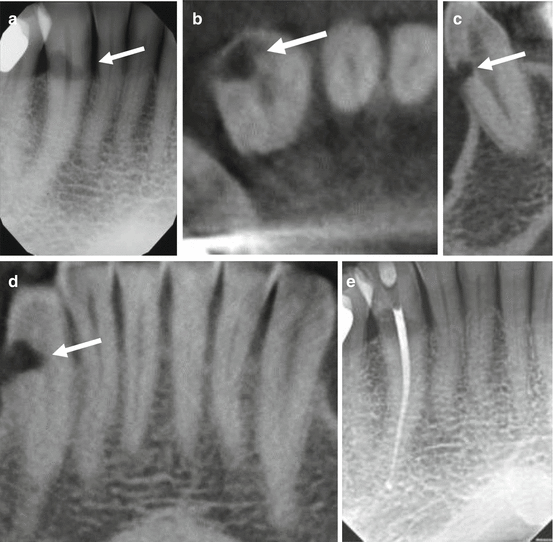

Fig. 7.3
CBCT has been shown to be more accurate than periapical radiography in the detection of invasive cervical resorption. A 41-year-old female patient presented with a history of orthodontic treatment during childhood. (a) Periapical radiograph of the maxillary right second molar shows an irregular area of low density in the coronal third, with ill-defined margins and penetration into the dentin (arrow). CBCT images of the (b) sagittal reformation, and (c) axial reformation demonstrate the full extent of the resorptive defect including the portal of entry (arrows). The pulp space was preserved by the peritubular dentin and there is a moderate mucositis superior to the second molar. The tooth was deemed non-restorable and extraction was recommended. The acquired CBCT scan was used for implant site assessment

Fig. 7.4
External resorption may be inconsequential or cause significant damage to the tooth and supporting structures if the resorptive process continues. (a) Periapical radiograph shows an irregular, well-defined area of low density (arrow) in the CEJ area of the mandibular right canine; features consistent with external cervical resorption. The canal space appears to be unaffected. CBCT images of the (b) axial reformation, (c) cross-sectional reformation, and (d) cropped panoramic reformation, and (d) sagittal reformation demonstrate the full extent of this feature (arrows) affecting the facial dentin. The lamina dura appears intact. Orthograde endodontic treatment was performed (e) and restored after crown lengthening using an apically positioned flap and ostectomy
7.5 Internal Root Resorption
Intraradicular internal root resorption is inflammatory in nature, relatively rare when compared with external root resorption, asymptomatic in its early stages, slowly progressing, and usually detected on routine radiographic examinations. Diagnosis using two-dimensional radiographic modalities is difficult; however, internal root resorption has clearly defined borders, usually round or oval shaped [28], with no canal radiographically visible in the defect (Figs. 7.5 and 7.6). In contrast, external resorption usually presents with an irregular radiolucency and intact root canal [29]. Internal root resorption has been described as either apical or intraradicular based on the location of the lesion [30].
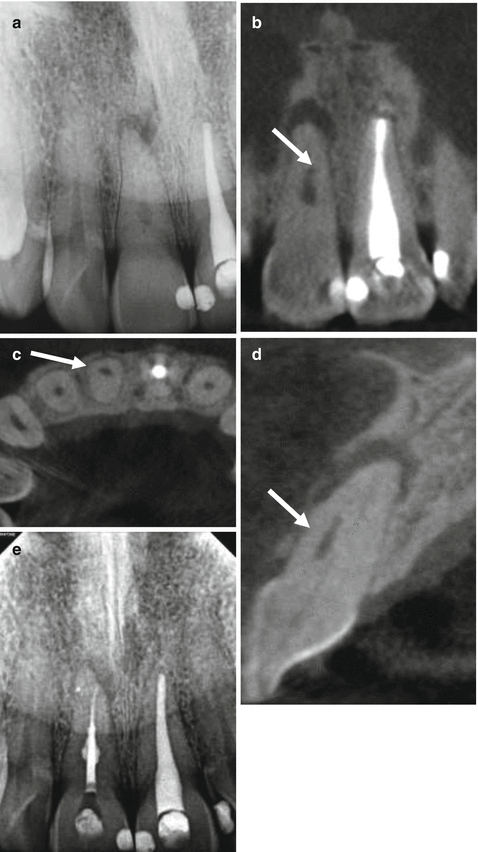
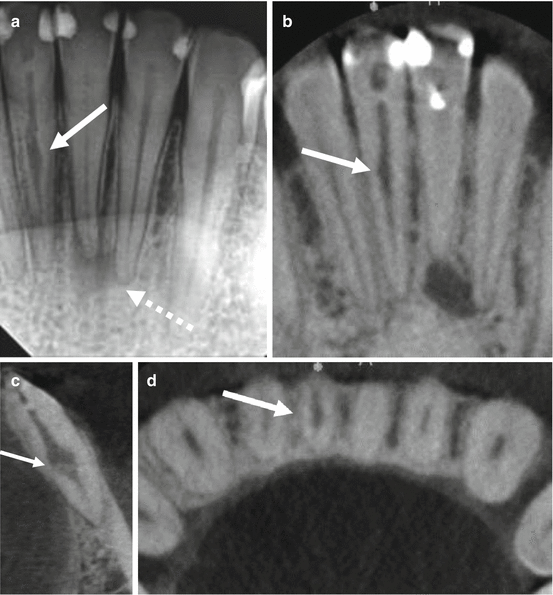

Fig. 7.5
A 39-year-old male presented with a history of trauma to the maxillary anterior region. (a) Periapical radiograph of the maxillary right central incisor reveals an approximately 3–4 mm long, 1 mm diameter, oval, well-defined area of low density centered mesiodistally, with calcification of the remaining pulp space (arrow); features consistent with internal resorption and canal calcification. CBCT images of the (b) sagittal reformation, (c) axial reformation, and (d) cross-sectional reformation show the location of the resorptive lesion (arrows) and its relationship to the calcified canal. The resorptive lesion was non-perforating, positioned facially, and separate from the pulp space. An area of low density extending facially to the junction of the middle and apical thirds was appreciated. Conventional nonsurgical endodontic treatment was performed (e) and the resorptive defect was incorporated into the three dimensional obturation

Fig. 7.6




Clinically detectible internal root resorption is considered a rare occurrence. A 33-year-old female presented for evaluation and possible treatment with a history of trauma to the mandibular anterior region. (a) Periapical radiograph shows a centrally located, well-defined, irregular area of low density (arrow) in the mandibular right central incisor; features consistent with internal resorption. The mandibular left central incisor shows a well-defined, uniformly radiolucent area of low density centered over a point at the apex; features consistent with pulp necrosis and calcification of the canal. CBCT images of the (b) coronal reformation (c) cross-sectional reformation, and (d) axial reformation demonstrate the same low-density area (arrows) of the mandibular right central incisor with greater dentinal penetration in the faciolingual dimension. Note the severe calcification of the mandibular left central incisor. Orthograde endodontic treatment was recommended for both teeth. The CBCT scan provided useful guidance to localize the calcified canal
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


