Fig. 12.1
(a) Orthodontically distributed dentition in a younger patient. (b) During orthodontic treatment, closing of remaining anterior spacing with direct resin composite buildup
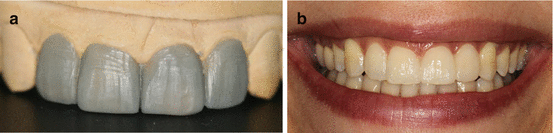
Fig. 12.2
(a) Diagnostic study models with wax setup or (b) direct mock-ups can be useful tools to optimize final restoration
Direct restorative approach with resin-based composites can be simple and relatively low cost compared to indirect restorations particularly porcelain laminate veneers, and also it does not impede future orthodontic treatment owing to its reversible treatment [3]. In addition, this conservative approach allows clinician to minimal or no tooth preparation in a single appointment (Fig. 12.3a, b) with esthetically and functionally pleasant outcome [2]. Current resin composite materials have adequate physical and mechanical properties, provide esthetically natural appearance with that of teeth structure, and are durable owing to refinement in the size of the inorganic fillers with optimal polishing capability [2, 22] (Fig. 12.4). Innovations in the filler technology have also led to the use of nanosized particles in the material composition, and this allowed to improve color stability of the materials itself besides the physical and mechanical properties of the resin composites [2, 22]. On the other hand, one of the advantage of the resin composite materials is that the intraoral repair in a single visit without needing laboratory process and at a lower cost with a desirable repair outcome of the chipping, defects, and stains [2, 22]. Resin composite materials can be used in the direct stratification of the material (Fig. 12.5) or layered with a fabricated silicone index from the study models to assist in material buildup during diastema closure (Fig. 12.6a–d) [3]. The clinician should bear in mind that if an enlarged frenulum is present between maxillary central incisors, it should be operated before restorative treatment procedure, and closure of the diastema is postponed after tissue healing (Fig. 12.7). During the application of the resin composite material, the clinician should carefully isolate the working area to avoid any contamination. Additionally, before initiation of the restorative procedure, clinician should also clean the tooth surface to remove any plaque, stains, and debris remnants (Fig. 12.8a, b). If the patient has a significant spaced area more than 3 mm, the clinician should prefer indirect restoration such as porcelain laminate veneers to maintain ideal tooth proportion. In that situation, direct restorative procedure with resin composite may cause distally tilted tooth appearance and disproportionate tooth form with an unpleasant outcome. Both direct and indirect restorative treatment choice should be limited to patients with good oral hygiene and who pay attention to oral care [2]. Although direct resin composite buildup in the treatment of diastema can provide good treatment outcome in a single visit, the clinician must pay attention not to create overcountered and biologically excessive intrasulcular restorations [2, 23]. One of the major difficulties in diastema closure is the creation of anatomical contacts with rounded counters and anatomical gingival margin adaptation. The use of wedges in order to create anatomical gingival adaptation may be useful in some cases, however, the use of wedge may also create undesired black triangles in the interproximal area. To overcome correctly countered and good intrasulcular restorations and limitations of the traditional clear matrix strips when closing diastema with direct resin composite, it has been proposed to use anatomic diastema closure matrix (Bioclear Matrix Systems, Tacoma, WA, USA) systems (Fig. 12.9) for intimate adaptation to the gingival margin and fully rounded counters of the restoration [24].
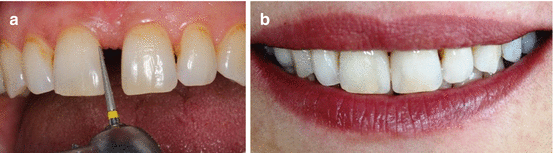

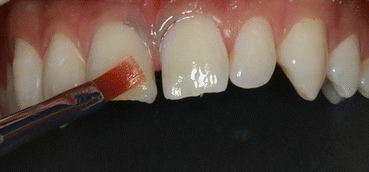
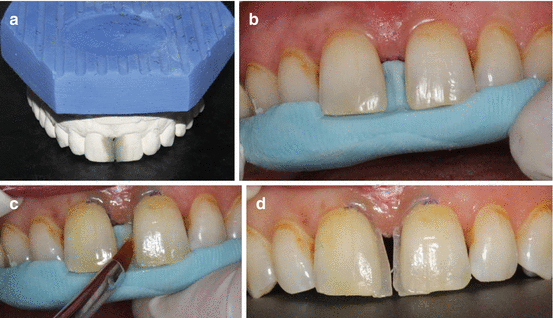
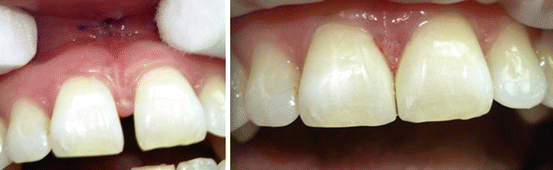
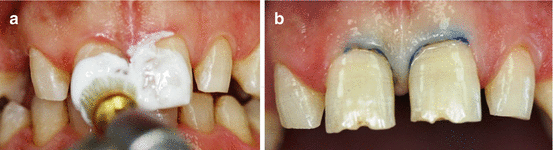
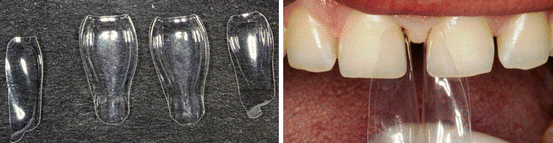

Fig. 12.3
(a) Minimal enamel preparation using fine diamond bur. (b) Final appearance of the case restored with direct resin composite in a single appointment

Fig. 12.4
Some examples of the current resin composite materials (Courtesy of Dr. Murat Tiryaki)

Fig. 12.5
Direct stratification of the resin composite material

Fig. 12.6
Resin composite buildup using silicone index. (a) Laboratory prepared wax setup on the study model. (b) Fabricated silicone index from the study model and placing onto the teeth. (c) Resin composite buildup with the help of silicone index. (d) Prepared palatinal contours of the restoration

Fig. 12.7
Operated enlarged frenulum between maxillary central incisors and after tissue healing, diastema closure with direct resin composite

Fig. 12.8
(a) Cleaning of the tooth surface to remove stains and (b) isolation of the working area using cotton rolls, retraction cords, and if possible rubber dam to avoid any contamination is necessary before initiation of the restorative procedure

Fig. 12.9
Different types of Bioclear Matrix Systems and trying on the patient teeth (thanks to Dr. Özgür Baydemir for providing the matrix systems)
Despite improvement in the formulations of the resin composite materials, the major drawbacks are still change of color, leakage and mechanical and/or chemical degradation of the material and hence, requirement of possible multiple replacement process by time [2, 3, 14, 25]. Therefore, the patient should be aware of the possible replacement requirement of the restoration due to color change and surface texture alterations within a reasonable time [2, 6].
Indirect restorations such as porcelain laminate veneers (PLVs) are the most common indications for diastema closure and offer clinicians as well as patients the most esthetically pleasant final outcome [10]. Requirement of minimal invasive tooth preparation (Fig. 12.10) for PLVs allow clinicians to obtain optimal esthetics with that of perfect mimicking tooth structures, perfect anatomical contours and correct tooth proportions. The other advantage of the restoration is also maintaining resistance to discoloration and surface degradation in comparison to resin composite materials (Fig. 12.11). Glazed perfect smooth surface can decrease plaque accumulation on the restoration, and also it has been reported that it increase the gingival sulcular fluid and hence promotes periodontal health by decreasing periodontal inflammation [2, 26, 27]. Disadvantages of PLVs are that they are time consuming, require technique-sensitive laboratory process, and have relatively high cost compared to resin composites [2, 17]. In addition, unlike resin composite restorations, PLVs can only be placed after the completion of orthodontic treatment procedure and must be placed after growth completion as well as when stable gingival margins are achieved [14]. During diastema closure with restorative procedures, clinician should pay attention to preserve or maintain ideal width/length ratio for a particular tooth [2, 10]. Careful multidisciplinary clinical evaluation and treatment plan will bring success, and diagnostic wax setup, composite mock-up, and digital smile design software (Fig. 12.12) can be helpful to the clinician in achieving an esthetically and functionally pleasant final restoration [1–3, 10, 14]. Preparation design and equal placement of restorative material on each side of the gap is very important during closing diastema. In general, small space between 0.5 and 1 mm does not require any restorative treatment, and patients feel happy to live with that spacing (Fig. 12.13). If any treatment is planned on a maxillary diastema that is 1 mm or less and the teeth is in ideal proportions, approximately 0.5 mm of restorative material adding to each tooth (Fig. 12.14) does not negatively affect the esthetic appearance and proportions [2]. Rounding the disto-incisal corners of the teeth and vertical lines for creation of illusion on the facial surface of the restoration can be used for a narrower tooth appearance [2, 10, 28]. In some situation where the teeth exhibit short clinical crowns, it should be necessary to perform crown lengthening procedures either apically by periodontal surgery, incisally with the addition of a restorative material, or combination of both procedures for maintaining ideal tooth proportion during diastema closure (Fig. 12.15) [2, 10]. At this point, the clinician should need to evaluate incisal display of the anterior teeth and if the incisal display is normal and the incisal edge in correct position but with teeth exhibiting short clinical crown; then periodontal crown lengthening procedure should be done (Fig. 12.16) before initiation of restorative approach to maintain proper tooth proportions [2, 10]. Without periodontal crown lengthening procedure, teeth will be appeared as squared form with disproportional short clinical crowns and will be perceived as unaesthetic [2]. If gingival level is correct and symmetric but length of the crown is short, then clinician can lengthen the teeth by using PLVs to achieve ideal width/length ratios (Fig. 12.17) during closing of the space [10
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


