Fig. 4.1
Control of the occlusion with diagnostic wax-up model to observe current occlusal pattern on the articulator
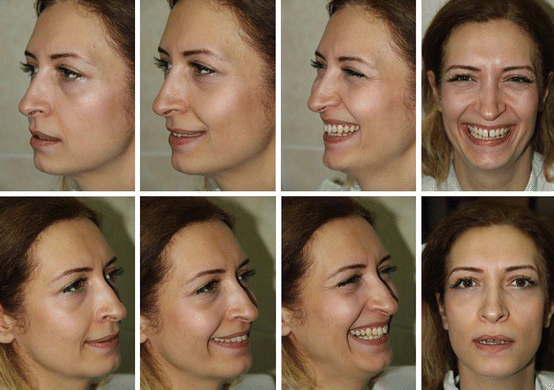
Fig. 4.2
Capturing extraoral digital photographs of the patient from different directions for appropriate diagnosis of the situation
For creation of an esthetically pleasing final restorative treatment, the clinician should also consider the patient’s age, personality, and sex, and develop a bioesthetic procedure in accordance with these criteria [1]. Several diagnostic techniques are currently used by clinicians to create an optimal outcome and patient understanding for the recommended treatment plan as previously described, such as diagnostic wax-ups, direct mock-up with resin composites, computer-based digital imaging techniques, and before-after photographs of other patients [1, 2, 5, 7].
Diagnostic models with the application of wax by modifying the size and shape of the teeth on a plaster model are useful tools for evaluating the current condition, restoration design, occlusion, and expected esthetic outcome in the spaced anterior region, even in simple cases [2] (Fig. 4.3a, b). A diagnostic plaster model with the wax-up is one of the best tools for esthetic diagnosis of a spaced dentition and for consultation with the patient [1]. It allows both clinician and patient to three dimensionally visualize the anticipated changes in form and function in a reversible way [8, 9]. These wax-up plaster models are also useful for evaluating the current clinical condition, restoration design, and education of the patient for the recommended treatment design protocol, and for determination of the occlusion [2]. This diagnostic wax-up model can be evaluated by patients and clinicians on the plaster, or on the articulator by the clinician for occlusion analysis, and can also be used intraorally with the use of silicone or acetate matrices (Fig. 4.4a–c). A well-prepared diagnostic wax-up can also aid clinicians to visualize the skipped necessary details which are not observed during clinical examination, and create predictable final results. These diagnostic models can resolve most of the critical questions regarding the restorative treatment plan and completion of treatment [2, 7, 10, 11]. In a multidisciplinary treatment procedure, this wax-up model can facilitate communication with other clinicians involved in the treatment procedure and can help clinicians to precisely communicate about the desired esthetic and function [8]. With this wax-up, other specialists (e.g., orthodontist, periodontologist) can precisely evaluate the model and make suggestions and recommendations in their field of expertise for creation of a functional, esthetically pleasing final outcome. Diagnostic wax-up study models also stands for the dental technician to evaluate the incisal edge position, dental midline, and teeth length and width [9]. By allowing visualization of the patient’s current condition and proposed restorative treatment, the dental technician can also help the clinician regarding choice of material, preparation design, and treatment sequence [8]. These discussions with the other experts and dental clinicians in regard of the diagnostic wax-up should not be overlooked, especially in the multidisciplinary approach as in the case of diastema closure. It is advisable that the clinician always keeps an unmodified plaster model for future before-after comparisons and reference [6]. Sometimes it is difficult for the patient to visualize the proposed final results by simply observing a wax-up either directly (Fig. 4.5) or on the articulator; therefore, it is recommended that the clinician makes the wax-up model more understandable for the patient so that the proposed final outcome is more easily discerned [1]. An easy method of making realistic plaster wax-up models is to use pink matrix or wax (Fig. 4.6) around the teeth to simulate the gingiva [1]. This technique can give an opportunity to the patients to see final result in a more realistic environment compared to a simple wax model. Although diagnostic cast models are important tools for the patients to envision the final results either directly or on the articulator, it is sometimes difficult for patients to understand the proposed final outcome even with the use of a pink matrix (Fig. 4.7). Therefore, the clinician should also use these wax-up models for the creation of temporary composites intraorally with the use of acrylic overlays or silicone acetate matrices [1] (Fig. 4.8a–c). Through this provisional restoration, the clinician can determine and test whether the overlays fit with the patient’s occlusion, teeth, gingiva, lips, and face; if any negative aspect is detected, appropriate modifications can be carried out as necessary [8]. These provisional restorations are previews of the final restorations whereby both clinician and patient can envision the final restorations in terms of esthetics, function, and harmony with the surrounding structures and smile, though less than optimal. Diagnostic models and radiography are useful to evaluate the current conditions of teeth, but are insufficient for the evaluation of the relationships between soft tissues and teeth. Digital imaging and a direct composite resin mock-up are more beneficial in achieving this goal. Diagnostic mock-up is the clinically equivalent procedure of the diagnostic plaster wax-up model [9, 12]. Direct composite resin mock-ups without incorporation of an adhesive system are simple, creative, and beneficial to both patient and clinician in foreseeing the possible final restorations before proceeding with any definitive restorative treatment [1]. It can also help the clinician to determine the final expected color shade and can serve as a more realistic alternative to diagnostic cast models. However, it is important to use a proper composite resin color matched with the adjacent teeth to avoid any bias, since a patient’s perception of shape can be influenced by the color of the material used [9]. Diagnostic mock-up is easy to produce, either directly on the teeth or by obtaining silicon matrices from the wax-up model, filling it with auto-cured temporary filling material, and placing it intraorally [6] (Fig. 4.9a–d). This technique is an advantageous diagnostic tool to anticipate the expected outcome intraorally during a short time in the clinical chair. The proposed restoration is visualized in three dimensions by placing resin composites directly on the teeth intraorally or by filling the obtained silicone or- acetate matrices with an auto-cured temporary filling material and placing it onto the teeth. In this way, the consistency of the placed restoration with other teeth, gingiva, lips, and face of the patient is visualized in three dimensions. The use of a mock-up is useful especially in diastema closure because the proposed restoration can change the patient’s appearance and phonation and, hence, the clinician is able to create a harmonious and phonetically relevant final restoration. Creation of the mock-up for diagnostic evaluation is simple. Resin composite material can be placed on the teeth by free-hand stratification without any adhesive application, and after polymerization the clinician can correct the restoration with burs and/or polishing disks to create a harmonious restoration with the teeth, soft tissue, lips, and face. This allows both clinician and patient to see eventual changes and contours of the restoration fit with the lips and face. In addition, phonation of the patient, especially with the “F” and “V” sound, can be tested for the evaluation of correct incisal edge position of the maxillary centrals [9, 13] (Fig. 4.10). Owing to closure of the space between the teeth, potential alteration or change in phonation may be noted by the patient, and adaptation to this new position may take few days; this aspect should also be discussed with the patient [9, 14, 15]. In an alternative procedure, a silicone impression is obtained from the vestibular aspect of the diagnostic wax-up model using polyvinyl siloxane putty material for creation a silicone matrix that is arranged in the patient’s gingival architecture by using a scalpel. An auto-cured resin material with the proposed shade is placed into the silicone matrix and then placed directly onto the patient’s teeth until the resin polymerizes. Before the full polymerization of the resin material, any excess must be removed with an explorer or hand instrument from the gingival margins before removal of the silicone matrix (Fig. 4.11a, b). If there is any excess after removal of the silicone matrix, this can be removed with a scalpel, or diamond or carbide round burs. This temporary resin material forms a perfect duplicate of the diagnostic wax-up with the selected shade for the definitive restoration (Fig. 4.12) [1, 6]. After these corrections, the patient can see the proposed restoration immediately [6
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


