Fig. 7.1
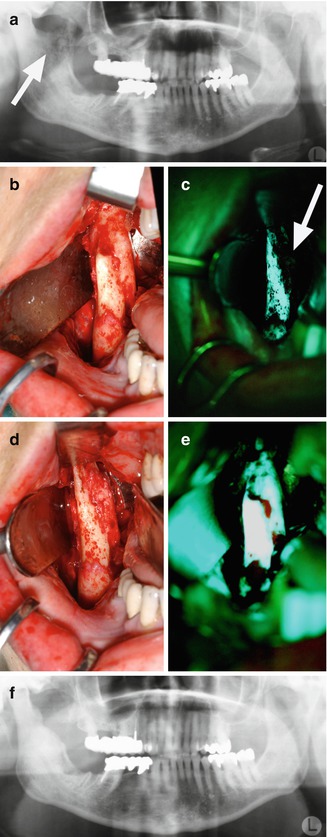
(a) A 68-year-old female patient suffering from multiple myeloma presented with a BRONJ stage I lesion in the left mandible. (b) The radiologic situation (orthopantograph) showed the typical signs of BRONJ, such as the absence of bone remodeling in the extraction sockets 7 months after tooth extraction. At that time, the patient refused surgical therapy, so the BRONJ was managed conservatively. (c) Clinical situation of the same patient 7 months later. Despite intensive conservative therapy, the disease progressed to a BRONJ stage II lesion with more exposed bone accompanied by a purulent and painful infection. (d) Displays the corresponding radiologic situation. All the remaining teeth in the left mandible were radiologically involved in the osteonecrosis (case published in 2011 [8] (Reprinted with kind permission of Elsevier))
Thus, after the first reports, BRONJ became the attribute of being very therapy refractory. Indeed, it was already recognized in 2004 by Ruggiero and coworkers that surgical therapy was necessary in most of the 63 cases of his study to improve or resolve BRONJ [10].
The treatment recommendations then changed with time: the more experience and knowledge with different BRONJ treatment strategies were gathered, the more the surgical therapy gained importance.
In 2006, it was suggested that the stages 1 and 2 should be treated conservatively, while extended cases (stage 3) should be treated surgically by debridement [11, 12].
In 2007 and 2009, the American Association of Oral and Maxillofacial Surgery (AAOMS) published stage-specific treatment recommendations for BRONJ [13, 14] (Table 7.1) which are still up to date. Summarized, conservative treatment of BRONJ stages 0 and I, superficial debridement of stage II, and debridement stage III is recommended.
Table 7.1
Staging and treatment strategies of bisphosphonate-related osteonecrosis of the jaw according to the position paper of the American Association of Oral and Maxillofacial Surgery 2009 [14] (Reprinted with kind permission of Elsevier)
|
Stage
|
Description
|
Treatment strategies
|
|---|---|---|
|
0
|
No clinical evidence of necrotic bone, but nonspecific clinical findings and symptoms
|
Systemic management, including use of pain medication and antibiotics
|
|
I
|
Exposed and necrotic bone in asymptomatic patients without evidence of infection
|
Antibacterial mouth rinse
|
|
Clinical follow-up on quarterly basis
|
||
|
Patient education and review of indications for continued bisphosphonate therapy
|
||
|
II
|
Exposed and necrotic bone associated with infection as evidenced by pain and erythema in region of exposed bone with or without purulent drainage
|
Symptomatic treatment with oral antibiotics
|
|
Oral antibacterial mouth rinse
|
||
|
Pain control
|
||
|
Superficial debridement to relieve soft tissue irritation
|
||
|
III
|
Exposed and necrotic bone in patients with pain, infection, and one or more of the following: exposed and necrotic bone extending beyond the region of the alveolar bone (i.e., inferior border and ramus in the mandible, maxillary sinus, and zygoma in the maxilla), resulting in pathologic fracture, extraoral fistula, oroantral/oronasal communication, or osteolysis extending to the inferior border of the mandible or the sinus floor
|
Antibacterial mouth rinse
|
|
Antibiotic therapy and pain control
|
||
|
Surgical debridement/resection for
|
||
|
longer-term palliation of infection and pain
|
Although newer (from 2012), the guideline report for BRONJ of the German Dental and the German Oral and Maxillofacial Associations is less concrete abstaining therapy recommendations for certain stages of the disease [15]. The reason might be that there are significant drawbacks in current BRONJ staging as suggested by the AAOMS [14]. First, neither the extent of the exposed bone nor its localization is taken into account. Definitely, a large area of exposed bone is more difficult to treat than a small one. Second, combinations of different BRONJ symptoms (i.e., no exposed bone (stage 0) and sinusitis maxillaries (stage III)) cannot clearly be classified. Third, the general condition as well as the patients’ burden of suffering are not considered. In a stage I disease, a patient might not have pain, but symptoms such as halitosis might reduce the quality of the social life significantly. Indeed, it is of great importance whether a patient is treated because of osteoporosis without any comorbidity or because of bone metastasis in a final stage receiving additional chemotherapy and suffering from various comorbidities such as diabetes or peripheral artery disease.
With regard to the development of the treatment recommendations, the author (as Oral and Maxillofacial Surgeon) suggests further advances in the BRONJ therapy will be achieved if all BRONJ stages are treated surgically.
This is for several important good reasons:
(i)
The diagnosis of an osteonecrosis should be confirmed by a histopathological investigation. Although until now the histopathological proof of an osteonecrosis is not a part of its definition, it can be excluded that other pathologic conditions such as jawbone metastasis [16] induce the clinical picture of the exposed bone. This is important as the therapy of a jawbone metastasis and BRONJ differs significantly.
(ii)
Exposed bone is an entrance gate for bacterial colonization and infection such as for actinomyces bacteria [17, 18]. For this particular microbial strain, a possible role in the pathogenesis as well as an aggravating effect of an existing BRONJ is discussed. Therefore, the exposed bone always increases the risk of BRONJ progression. Due to the fact that conservative treatment approaches do commonly not resolve the exposed bone [7, 19], there is the risk of worsening of the BRONJ stage or secondary infection leading to abscess or pain, particularly in patients who are immunocompromised by chemotherapy (see Fig. 7.1).
(iii)
The success rates of surgical approaches are significantly higher compared to conservative treatment regimens [20]. Given that a therapy success includes the removal of exposed bone and an intact mucosa, conservative management shows disappointing results of less than 20 % [7, 19, 21, 22]. In contrast, surgical approaches reveal success rates exceeding 85 % [8, 23–25]. A timely treatment has a positive effect on the outcome [10, 26], which is another reason to perform surgical therapy in the stages 0 and I.
(iv)
The conservative therapy commonly takes months to years with weekly or twice a week consultations for conservative wound management [21, 22], which can be considered as additional burden for the affected patients. In contrast, the surgical treatment is usually completed 3–4 weeks after surgery [8]. It should be taken into account that effects similar to habituation of the microbial wound flora will take place after weeks or even months of antibiotic treatment [27]. Side effects such as microbial resistances or oral candidiasis might aggravate the treatment.
“Therapy literally means ‘curing, healing’ and is the attempted remediation of a health problem, usually following a diagnosis” [28].
BRONJ is currently diagnosed by the presence of exposed jawbone for a period that exceeds 8 weeks [13, 14, 29] (in combination with a positive drug history for bisphosphonates and no radiation of the head and neck region). Consequently, a therapy success is achieved when the exposed necrotic bone is removed and a mucosal integrity is restored. Therefore, the aim of the BRONJ therapy should resolve the leading symptom: the exposed bone.
Indeed, confusion is caused by studies applying conservative measures to treat BRONJ and reporting success rates exceeding 50 % [30, 31]. To understand this obvious discrepancy, it is important to take a closer look of how the success of a therapy is defined in these studies. The maintenance of the status quo, i.e., no worsening of the situation of the exposed bone [30, 31], can be considered as improvement of the patient’s situation but not as therapy success with respect to the definition of the disease. Furthermore, studies on therapy success should not use retrospective but prospective study designs. In retrospective studies conducted with questionnaires without oral investigations, it is impossible to detect early stages with exposed bone that are not accompanied by infection or pain. Due to the fact that these “silent” BRONJ stages are a frequent finding, a significant number of BRONJ cases are not recorded in retrospective studies.
In spite of these considerations to treat all BRONJ stages surgically, the conservative therapy is useful and necessary to control the disease when the patient’s general condition does not allow surgical intervention or when chemotherapy cannot be discontinued. Applying conservative measures, patients’ condition improved or stay asymptomatic in up to 70 % of the cases [32].
Indeed, it is of crucial importance that the patient is thoroughly informed about the different treatment options, the duration and burden of each therapy way, as well as the success rates. In addition, the specific needs and discomforts of the patients should be considered for the choice of therapy.
Due to the fact that the necrotic and exposed bone will not be revitalized and turned into a vital bone again, BRONJ should be removed even if only small bone areas are affected. Thus, the aim of the surgical therapy is the complete removal of the osteonecrosis because even small residuals might lead to a recurrence or progression of BRONJ both by mechanical injury of the mucosa as well as by microbacteria remaining in the affected bone.
The therapy should be well planned beginning with the choice of the surgical approach. The mucosal incision should always be performed in consideration of a tension-free mucoperiosteal coverage of the area of the exposed bone. Mucosal dehiscences as well as fistulas should be included in the incision line. Subsequently, the marginal mucosa of these areas should be cut out, because the mucosa adjacent to BRONJ lesions is altered due to the chronic infection and less useful for reconstruction [33]. If teeth have to be removed, a marginal incision has to be performed in order to allow the wound closure with a mucoperiosteal flap. Unlike in osteoradionecrosis, the deperiostation of the bone has no unfavorable effect in the treatment of BRONJ. Indeed, a sufficient bone exposure helps to remove the osteonecrosis completely, to even sharp bone ridges, and to achieve a tension-free wound closure.
The exposed bone in BRONJ commonly shows a darker and yellowish color compared to the unaffected sites. The porosity is often increased, and the necrotic bone is often softer compared to the normal bone. Frequently, BRONJ is surrounded by sclerotic bone areas, which are harder and less vascularized pretending an avascular necrosis. The osteonecrosis including bone sequestra must be removed completely even if this causes large bone defects of the jawbones or broad oroantral fistulas.
If the osteonecrosis reaches or surrounds the teeth, the respective teeth have to be extracted in order to remove the osteonecrosis completely. After the surgical elimination of the osteonecrosis, it is of crucial importance to smooth sharp bone ridges such as the crestal bone of tooth extraction sockets in order to avoid failure. This is an important step in the treatment of BRONJ, because the bone turnover is reduced by the bisphosphonate administration and sharp bone sites will be remodeled very slowly. Spiky ridges can either hamper the mucosal healing or injure the mucosal coverage of the wound and increase the risk of recurrence of the exposed bone. There is an overlap of therapeutic and prophylactic measures. With respect to the conclusive pH-dependent BRONJ pathogenesis theory [34, 35], surgical procedures such as root resections or tooth extractions are recommended to eliminate chronic infections. Indeed, sharp bone ridges must also be removed following these procedures.
In most cases, buccal mucoperiosteal flaps are best suited to achieve a tension-free mucosal coverage. On the one hand, the mobilization of the buccal mucoperiosteum is easier compared to the palate mucosa in the maxilla or parts of floor of the mouth. On the other hand, the functional limitations are much less when using buccal mucoperiosteal flaps. Some surgeons suggest a two-layer coverage of the exposed bone to achieve safer wound closure. In the mandible, this can be achieved either by a muscle flap of the mylohyoid muscle [36] or a buccal fat flap. The latter is also suitable for a two-layer coverage in the maxilla in particular when oroantral fistulas are present after the BRONJ resection [37, 38] (see Fig. 7.2). The nasolabial flap is an additional option to reconstruct defects of both the mandible and the maxilla [39]. While a two-layer wound closure might be of use in broad oroantral fistulas, a monolayer coverage using a mucoperiosteal flap is usually sufficient when the osteonecrosis is completely removed. Although the mucosa in BRONJ patients can be of inferior quality and stability [33], soft tissue free flap reconstruction is only necessary in rare cases.
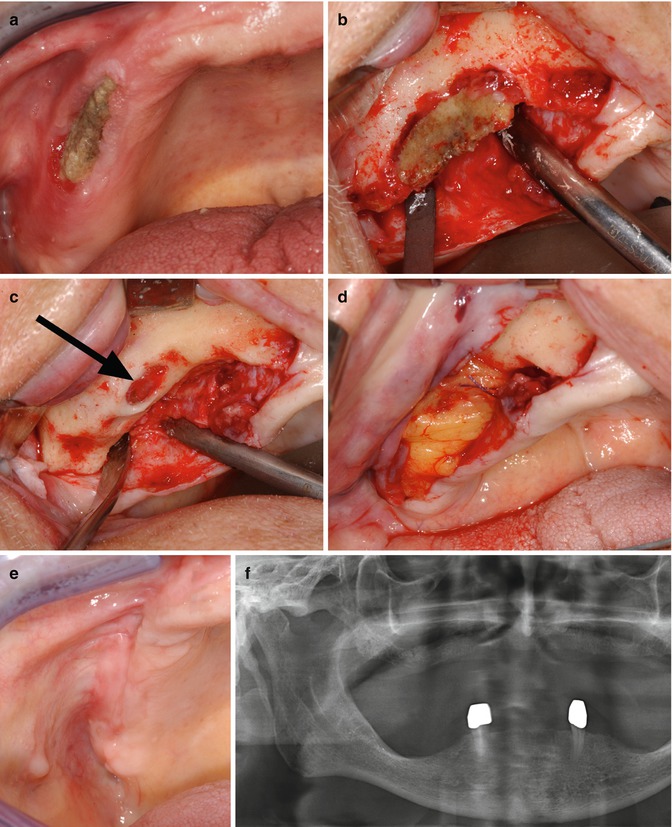

Fig. 7.2
(a) 79-year-old man suffering from prostate cancer presented (a) with a BRONJ stages I–II lesion in the right upper jaw. The patient was treated surgically. (b) Intraoperative presentation of the BRONJ. (c) Intraoperative situation after complete surgical resection of the osteonecrosis. Note the broad oroantral fistula (arrow). (d) Wound closure was performed in a two-layer technique using Bichat’s buccal fat flap and mucoperiosteum. (e) 4 weeks postoperatively, the patient was free of symptoms and showed complete mucosal healing. (f) The postoperative radiograph (case published in 2012 [34] (Reprinted with kind permission of Elsevier))
The demand for bony reconstruction arises more frequently, in particular when parts of the mandible have to be resected. The treatment options range from a resection without reconstruction [25], the stabilization of the jaw with osteosynthesis plates [25, 40, 41], to the bony jaw reconstruction using avascular [41] or microvascular bone flaps [42–44]. Although success rates of free flap bone reconstructions are good, the burden of the operation for the patients is not negligible. Indeed, the dental rehabilitation using dental implants is contraindicated in patients with intravenous bisphosphonate administration as well as a BRONJ in the medical history according to the recommendations of the AAOMS [14]. It should always be considered that the transplanted bone is also loaded with bisphosphonates. As a matter of fact, the transplanted bone can again be affected from BRONJ [45] not to mention failure of the transplant because of a higher operation risk due to the comorbidities. The limitations have to be considered especially the general condition of the patient suffering from bone metastasis as well as the prognosis and the stage of the underlying disease. Thus, a free flap bone reconstruction might be in option in the treatment of extended BRONJ cases, but it is not recommended as the first step in the therapy.
The exposed bone in BRONJ is always colonized with bacteria of the oral cavity such as actinomyces. Furthermore, the microbial adhesion to the bone appears to be altered under bisphosphonate therapy [46]. Thus, there is always a more or less active infection of the exposed bone [47]. Consequently, adjuvant measures that aim for disinfection of the bone are of use to support the surgical treatment such as ozone application [48], laser therapy [49], and in particular a prolonged antibiotic therapy [50]. Antibiotic prophylaxis had a significant impact on the incidence of BRONJ after dental procedures in patients under bisphosphonate medication. The administration of penicillin derivates is recommended. In case of allergy to penicillin, tetracycline derivates or clindamycin are an alternative treatment option. Due to the fact that tetracycline and its derivates bind to calcium, there might be a depot or long-term effect.
Additional measures such as the application of stem cells [51] and platelet-rich plasma [52], providing an alkaline environment [53], or the administration of parathyroid hormone [54, 55] are promising approaches; however, still on an experimental level.
The challenge as well as the limitations of the surgical therapy of BRONJ is that the margins of the osteonecrosis cannot be exactly determined; thus, a clear demarcation of the necrotic bone is difficult if not impossible [13, 29, 56]. However, the complete removal of the necrotic bone is of crucial importance as otherwise there is the risk of disease recurrence or progression [25, 57]. On the other hand, it must avoided to unintentionally and unnecessarily remove the healthy bone without signs of osteonecrosis in order neither to weaken the jawbone (danger of fracture) nor to make the situation for dental or prosthetic rehabilitation more difficult. The bone debridement cannot be standardized, as it is the surgeon who decides how much bone to be removed, because there is no modality, which is able to objectify the margins of the necrosis. Hence, the surgical therapy is dependent on the surgeon and neither comparable nor reproducible in another department.
There are numerous studies using various imaging modalities in attempts to objectify the extent of the osteonecrosis including panoramic radiography [58], CT, SPECT/CT [59], PET/CT, MRI, cone-beam CT imaging [37, 60], or bone scintigraphy [61]. However, none of these modalities is able to clearly depict the margins of the necrosis [15]. It could be demonstrated that the changes of the bone structure (depicted by x-ray techniques such as panoramic radiography, CT, or cone-beam imaging) are more helpful for operation planning compared to the depiction of the soft tissue reactions including the infection (e.g., by MRI, PET, or scintigraphy). Osteosclerosis around sites of inflammation (e.g., teeth with periodontitis), density confluence of cortical and cancellous bone, and prominence of the inferior alveolar nerve canal, and a persisting alveolar socket can be early radiologic signs [58]. In later stages, bone sequestra, radiolucencies due to osteolysis, and cortical disruption as well as periosteal bone formation might be present [62]. However, these findings are not stage specific and cannot objectify the exact extent of the necrosis.
One of the most reliable parameters is the intraoperative impression of the surgeon [60]. The surgical debridement in BRONJ therapy is commonly performed until the bone appears to be “normal,” i.e., the bone structure (porosity), color, and texture are similar to the non-affected bone sites. However, the personal feeling of a surgeon is neither reproducible nor transferable. As a consequence, the comparability of studies with different surgeons is limited. What is more, the bleeding of the bone is widely accepted to be a sign of a viable bone in the surgical therapy of osteonecrosis and in particular in BRONJ. However, it has been shown that bone bleeding does not correlate well with the histological findings of the vital bone. Thus, this finding is no appropriate parameter to determine the extent or the margins of an osteonecrosis [8, 40, 56].
A helpful technique to distinguish between viable and necrotic bone is the use of bone fluorescence [8, 40, 56, 63, 64]. In addition to the antibiotic effect of reducing inflammation and pain in patients suffering from BRONJ, tetracycline and its derivates possess fluorescence properties [65]. Under appropriate excitation light, tetracycline derivates show a greenish fluorescence at approximately 525–540 nm [66]. Due to its affinity to calcium, tetracycline is incorporated in the bone in particular in areas of bone remodeling and bone apposition [67]. Viable bone shows a green fluorescence that can be visualized intraoperatively by using a VELscope fluorescence lamp (LED Medical Diagnostics, British Columbia, Canada), a certified medical device approved by the American Dental Association for the detection of mucosal tissue abnormalities [8, 40, 56, 64, 68]. In contrast, the necrotic bone shows no or only pale fluorescence (see Figs. 7.3 and 7.4). Recent reports suggest that the VELscope system induces an autofluorescence of vital but not of necrotic bone leading to similar bone fluorescence findings without tetracycline bone labeling [69].
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses