Fig. 19.1
Diagnostic criteria for the three painful pulpal and periradicular conditions
Treatment of Pulpal and Periradicular Conditions
Treatment for symptomatic irreversible pulpitis, symptomatic apical periodontitis, and acute apical abscesses usually involves treatment with the removal of the inflamed/necrotic pulp either with an endodontic procedure or extraction and only rarely require antibiotics.
19.2 Other Sources of Perceived Toothache Pain
Three Categories
There are three main categories of conditions that can lead to a patient perceiving and reporting pain as coming from the tooth but are not related to caries, pulpitis, or periradicular pathology. First, chronic conditions (musculoskeletal primarily) can create nociceptive (i.e., pain impulses) pain signals that include referred pain to teeth. Second, neuropathic conditions which are nonnociceptive (pain signals are generated by the neural pathways themselves and not as result of tissue injury) can create perceived pain that can “shoot” or “stab” in an area that can include teeth, gingiva, and other oral structures. Third, there are less understood conditions that are associated with a tooth or teeth and are “nonodontogenic” in nature. The pain is perceived and centered in the tooth, but there is no detectable pulpal or periradicular pathology.
Chronic Pain’s Contribution
Chronic pain conditions are more likely to be associated with multiple concurrent (comorbid) diagnoses and referred pain than acute conditions. Acute conditions in one tooth may refer pain to other teeth in the posterior regions of the dentition. Diagnostic confusion from this type of pain referral is apt to be short lived since acute inflammatory conditions are usually self-limiting, will usually reveal the actual source of the pain in a few days, and will resolve upon treatment (Bender 2000). Chronic pain referral presents a more different dilemma because of the architecture of the central nervous system (CNS). Long-term pain has been shown to create changes in the CNS through an increasing ability for pain transmission to occur (plasticity) and central sensitization (sensitization of the central nervous system) which results in a significantly lowered pain thresholds and a widening of field of reported pain (Woolf 2011; Fernandez-de-las-Peñas et al. 2009). Convergence occurs from a decreasing number of neurons moving from peripheral to central. The cervical and trigeminal systems have been shown to converge into the same region of the brainstem (spinal trigeminal nucleus) creating decreasing thresholds, upregulation of pain, and pain referral (Ge et al. 2004). As an example, a cervical muscle such as the trapezius can influence pain and referral in the anterior temporalis muscle on the face. It is very understandable that this could impact patient perception. The result is that chronic pain conditions can result in consistent pain referred from a distant site to the dentition. One study reported demonstrated an 85 % incidence of pain referral for chronic orofacial pain patient during the examination. Of the same group, 11 % reported pain referred to their teeth (Wright 2000). Pain chronicity and central sensitization have significant implications for the differential diagnosis of a reported toothache.
Management of Chronic Pain Differs from Acute Pain of Tooth Origin
The presentation of chronic pain and acute pain differ greatly. Therefore, the management is also very different. Acute pain is primarily monofactorial, associated with inflammation which occurs following injury, usually has a short duration, and resolves with the healing of the insult. Chronic pain is multifactorial (often presents with several diagnoses), usually not associated with inflammation, displays a long duration, and continues often after resolution of the initial injury. Acute pain occurs in the periphery, and pain is transmitted via nociceptors (pain receptors) through the afferent neurons to the brain. Chronic pain is associated with the central sensitization as described in the previous paragraph in the CNS. Treatment for acute pain is associated with supportive therapy to promote healing and, if necessary, nonsteroidal anti-inflammatories for pain relief. Chronic pain requires a management strategy that addresses each of the known contributing factors or risk factors. Each diagnosis must be included. Patient-centered care is key including patient education, self-physical therapy and self-behavioral modification, and support for coping skills. Patients need to be educated about the importance of eight hours of sleep. Interuption of sleep has been shown to negatively impact anti-pain neuro transmitters and mood. Pharmacology utilizes psychotropic medications that help re-regulate and dampen the central sensitization of the trigeminal system such as tricyclic antidepressants (Books 1). Management strategies begin with reversible approaches and escalate only as necessary. A multidisciplinary approach with other providers including clinical psychology, physical medicine (physiatrists and physical therapists), and sometimes otolaryngology or neurology is often necessary (Fricton 2014).
19.3 Myofascial Pain in the Head and Neck
Overview
Myofascial pain is a chronic musculoskeletal pain condition that involves the muscles and their attachments including the masticatory or cervical regions for our discussion. Palpation of the muscles reveals painful areas of hyper contracted tissue or “taut bands” which were called “trigger points” by Dr. Janet Travell (Book 2). The quality of the pain is often dull and achy which will vary in intensity often in the moderate to severe range from day to day. The duration is usually hours to days and may be continuous for months or years. The condition is bilateral, but one side often predominates in intensity. Other chronic conditions such as headaches, fibromyalgia, sleep disturbances, depression, otalgia, and bruxism are comorbid (Fricton 2007). The muscles of mastication likely refer pain to the dentition more than any other structures (Ehrmann 2002).
Keys to Diagnosis
During muscle palpation, the patient will report a painful muscle that duplicates the pain of the chief concern including both the local discomfort and the referral pattern – without prompting from the examiner. This duplication means that the pain descriptors are very similar (familiar) to the chief concern and the pain occurs not only at the muscle site but also at the distant referral site (i.e., the tooth or other structure). Removal of the trigger point or source of pain leading to the referral will also eliminate the pain at the distant site. Diagnostic anesthesia such as 3 % mepivacaine can be utilized to anesthetize the suspected trigger point.
Muscles That Refer to Teeth
The superficial masseter, the most commonly implicated muscle, may refer pain to the ipsilateral maxillary or mandibular posterior teeth (Handa et al. 2013). Different aspects of the muscle refer to different distant sites. The superior section refers to the maxillary teeth, and the insertion or more inferior section refers pain more often to the mandibular teeth. The temporalis muscle may refer pain to the ipsilateral maxillary teeth (Wright 2000). The most anterior segment reported will refer to the anterior teeth, the middle section to the premolar teeth, and the more posterior segment to the molars. The anterior digastric muscle may refer pain to the mandibular incisors.
Imaging
A panoramic survey would be utilized to rule out any gross pathology, and additional imaging would be appropriate to evaluate dental pathology.
Management
-
Patient-Centered Plan
-
Patient education about the nature of the condition and how pain referral can occur
-
Self-regulation that includes postural exercises, diaphragmatic breathing, self-behavioral modification to decrease diurnal parafunctional habits (such as clenching)
-
Self-physical therapy with stretching, thermal therapy (moist heat and ice)
-
Implement coping strategies
-
Utilize nutritional supplements such as calcium and magnesium
-
-
Dental Orofacial Pain Plan
-
Provide patient education, appropriate referrals, needed pharmacotherapy
-
Provide occlusal guard therapy where appropriate
-
Provide trigger point injections were appropriate as part of an overall management plan
-
Provide follow-up care
-
-
Physical Therapy
-
The therapist can provide manual therapy to stretch shortened muscles in order to mobilize greater range of motion.
-
Help train the patient to strengthen postural muscles to help stabilize core muscle groups that influence posture.
-
Provide pain relief through different modalities such as iontophoresis and tens treatments to the painful muscles.
-
-
Pharmacotherapy
-
Tricyclic antidepressants such as amitriptyline (10–25 mg) below antidepressant dosages to help decrease central sensitization
-
Central acting muscle relaxants or antispasmodics to help with muscle tone and facilitate self-therapy and physical therapy. Baclofen 10 mg three times per day, cyclobenzaprine 10 mg at bedtime (not likely utilized with amitriptyline), or tizanidine 4 mg at bedtime are examples.
-
-
Clinical Psychology
-
Can provide life coaching to help patients develop more effective coping strategies
-
Can teach cognitive behavioral therapy to help patient recognize thinking patterns
-
Can provide imagery, relaxation, and hypnosis strategies for patient
-
The goal of management is provide a comprehensive plan that includes all of the different problems and multiple diagnoses.
19.3.1 Degenerative Joint Disease (and Arthralgia) of the Temporomandibular Joint
Overview
Most pain in the TM joint is of inflammatory origin from the capsule, synovial tissue, or tissues in the retrodiscal region. Osteoarthritis is often associated with orthopedic overload of forces upon the joint which is displayed on images as flattening of the condyle or other osteophytic changes. It may or may not be associated with articular disc displacement in the joint. Sharp severe pain is usually associated with function from chewing, opening wide, or clenching the teeth. The sharp pain is often intermittent but may be accompanied by a dull background pain that lasts for hours (Okeson 2007).
Keys to Diagnosis
The patient will usually present a history of pain with function. Examination will reveal palpation soreness or pain directly associated with the TM joint (lateral pole, posterior lateral aspect, and load testing) as opposed to the deep masseter (in close proximity to the joint) or superficial masseter. If there is pain in both the TM joint and the masseter, an auriculotemporal block with 3 % mepivacaine may be utilized. If the pain is removed with the anesthesia, then the likelihood is great that the TM joint is the source of the pain. Auscultation of the TM joints will likely reveal moderate (or coarse) crepitus throughout most of the mandibular movements in all directions.
TM Joint Pain Referral to the Teeth
Pain referral to teeth from the TM joint is infrequent. There are case reports of diagnostic confusion with third molar pain (DeAngelis et al. 2009).
Other Complications
If the articular surface of a TM joint condyle degenerate rapidly, increased occlusal pressure is generated upon the second molars (or most posterior teeth). This can lead to wear, cracking, or mobility. If the condylar change is sufficiently rapid, an anterior open bite will occur.
Imaging
If significant degenerative joint disease is suspected from the examination, a CBCT (cone beam computed tomography) scan would be indicated. It would require the ability to view sagittally corrected images of the TM joint condyles. The images would reveal the articular surface of the condyles and articular eminence, the intra-articular spacing between the condyle and eminence, and the position of the condyle in the glenoid fossa.
Management
The management of TM joint pain relates to the pain associated with the localized inflammation within the joint itself and the decrease in range of motion. If the condition is chronic, the same principles of management apply with patient education, management of overload with occlusal splint therapy when needed, physical therapy if the range of motion is decreased, and anti-inflammatory medications (either steroid or nonsteroidal) (Okeson 2007). The most documented approach for pain management is the utilization of nonsteroidal anti-inflammatory medications such as ibuprofen, naproxen, or meloxicam (Okeson 2007; Argoff 2011). These medications all have the same pharmacotherapeutic effect with the inhibition of prostaglandin synthesis. The inter-medication differences are associated with drug potency and duration of efficacy (½ life of drug metabolism). Newer research has also differentiated different potencies in different tissues and fluids. Meloxicam is selectively absorbed in higher concentrations in synovial fluid than other NSAIDS and even greater in inflamed joints with fewer gastrointestinal side effects. Ibuprofen would usually require four dosages per day, naproxen two dosages but displays greater gastrointestinal irritation.
19.3.2 Rhinosinusitis
Overview
This can be an acute or chronic condition that affects the maxillary and other sinuses. An acute rhinosinusitis is usually associated with a recent viral upper respiratory infection with a short duration of up to 4 weeks which “worsens” after an initial improvement. The patient reports a purulent nasal discharge, nasal obstruction, a feeling of fullness, and at times facial pain. Most acute episodes are viral and rarely bacterial (only .5 to 2.0 %). A chronic sinusitis is associated with nasal congestions of more than 12 weeks or four annual episodes. The chronic condition is more apt to be associated with bacterial infection but is not usually associated with pain. The chronic condition occurs with stasis or lack of clearing of the mucus in the ostiomeatal complex. Historically, sinusitis has been over diagnosed and treated with antibiotics with little efficacy (Ferguson 2014).
Keys to Diagnosis
Acute rhinosinusitis must be associated with purulent discharge and with one of the following: with either nasal obstruction or facial pain or both (Ferguson 2014). If facial pain occurs but no purulent discharge is present, the condition does not match the criteria for acute rhinosinusitis. A recent or recurrent upper respiratory infection is also very likely. Unilateral pain upon palpation of the lateral wall of the maxillary sinus is often present.
Maxillary Sinus Pain Referrals to Teeth
The maxillary sinus primarily refers pain to the ipsilateral maxillary 2nd premolar and the 1st maxillary molar. The maxillary 1st premolar or maxillary 2nd molars can be implicated too (Ferguson 2014).
Imaging
A CBCT scan with air-fluid level opacity in the maxillary sinus would confirm the diagnosis.
Management
Most rhinosinusitis is associated with a viral origin and will run its course without intervention. The patient can irrigate the ostiomeatal complex with saline solutions through sprays or nasal irrigation devices. Antibiotic therapy has historically been overutilized and should be avoided unless the condition has recurred and the purulent discharge continues. The main dental concern is to avoid unnecessary dental procedures and a likely referral to otolaryngology (Rosenfeld et al. 2015) (Fig. 19.2).
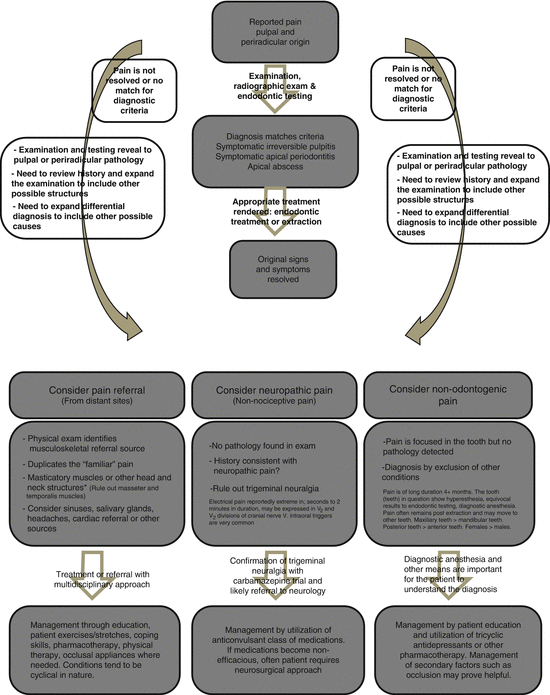

Fig. 19.2
Diagnostic flow chart for reported toothache pain. Most toothache pain follows the center pathway, but when the diagnosis doesn’t fit, other conditions need to be considered
19.3.3 Sialadenitis of the Submandibular Gland
Overview
Sialadenitis of the major salivary glands is associated most often with blockage by a sialolith or calcification of the major salivary duct, which occurs most commonly in the Wharton’s duct of the submandibular gland. The blockage leads to salivary retention in the gland associated usually with swelling and pain. As the flow diminishes, bacteria may move into the duct toward the gland with possibility of a sialadenitis developing in the gland itself. The condition can become chronic with a decrease in pain over time (Mandel 2011).
Keys to Diagnosis
The pain history will usually report pain either initiated or exacerbated with meal times. A submandibular sialadenitis will likely be reported as a deep pain near the angle of the mandible which a patient may have difficulty in localization. The salivary flow would be decreased from the affected gland. Bidigital palpation will reveal a painful submandibular gland (or occasionally a parotid gland) and possibly a sialolith in Wharton’s duct if the calcification is of sufficient size.
Submandibular Gland Pain Referral to Teeth
The submandibular gland may refer pain to the ipsilateral body of the mandible and the mandibular molars.



