Fig. 4.1
Schematic drawing of the initial carious lesion including a surface zone, the subsurface lesion (or body of the lesion), the condensation zones (dark zone and translucent zone), and the normal enamel above the mantle dentin

Fig. 4.2
Ground section of an initial carious enamel lesion. The surface layer is due to mineral re-precipitations. In the subsurface, the body of the lesion is triangular in shape, with a summit oriented toward the dentinoenamel junction. The lesion displays two borders: one dark zone that is in progress and a reaction zone (limiting or translucent zone)
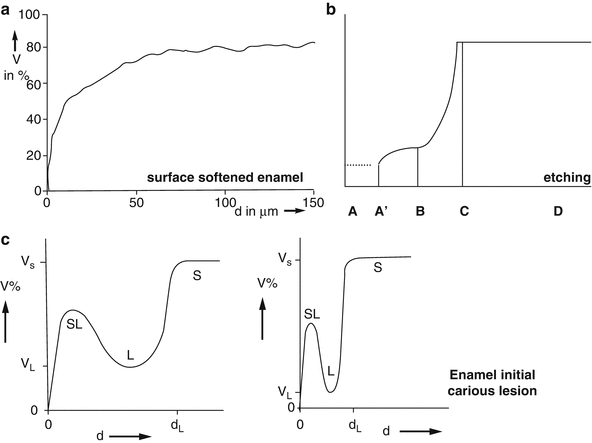
Fig. 4.3
Schematic percentage of mineral in volume: (a) in the softened enamel, (b) after acid etching, (c) in the initial carious lesion. SL surface layer, L body of the lesion, S normal enamel surface
1.
The most superficial “unaltered” surface zone (the surface enamel layer) (#20 μm–50 μm). The lesion remains covered by a surface layer, which seems relatively unaffected by the carious attack. Dissolution/precipitation mechanisms and protection by adsorbed agents provide some explanations clarifying the basis of porosity or solubility gradients. The formation of enamel caries does not imply initially a subsurface formation. The thickness of the surface layer develops during the progress of the carious lesion. However, the thickness of the surface layer seems to be fairly constant. The mineral-rich layer develops later. Inhibitors such as F or proteins play important role in the surface layer formation. After the initially surface-softened enamel where dissolution takes place (inhibitor action), a subsurface region is created where dissolution occurs. The point of entry of the “cariogenic agent” through the surface layer was found to be related to several Retzius striae. The surface zone has a pore volume of less that 5 %.
In the surface zone of artificial carious lesions, tiny microchannels about 0.5–1.5 μm in diameter and roughly 100 μm in length have been observed (Goldberg et al. 1981). This suggests that these channels are involved in the lesion development, playing role in the diffusion processes. The microchannels originate in prisms in the perikymata of the surface enamel. They extend in the direction of Hunter-Schreger bands, mainly in connection with diazones. In conclusion, the initial artificial lesion formation is related to the organization and ultrastructure of enamel (Goldberg et al. 1981).
In a 40–50 mm-thick surface layer, an average of 9.9 % reduction in mineral content was found. In this zone, only the magnesium content was unchanged compared with adjacent surface zones.
2.
The subsurface layer (or body of the lesion) (30 μm), which may appear either parallel to the surface or adopt a triangular shape, with a top oriented toward the dentinoenamel junction. The pore volume in the body of the lesion was approximately 10 %–25 % in the central part of the lesion and shows enhanced incremental lines. The Retzius striae are well marked. They demonstrate a pattern of cross-striations. Alternate radiolucent lines (slightly demineralized) and radio-opaque (more mineralized Retzius striae) were spaced 6–8 μm. For some authors, the demineralization process unmasked the Retzius striae. The lowest mineralization content was 29 % by volume. The lesion showed well-mineralized bands passing through the body of the lesion, giving a laminated appearance. Microchemical studies indicate a reduction of 24 % in mineral per unit volume compared with sound enamel. Magnesium was reduced by 20.1 %.
3.
Two parallel inner zones: a dark zone seems to be hypomineralized. This is the second zone of alteration from normal enamel. Occurring in 85–90 % of the lesions, positive birefringence contrasts with the negative birefringence of the sound enamel. The pigmentation may be due to the arrest of microorganisms, which are present within the dissolved enamel parts. The dark zone contains a pore volume of 2–4 % of spaces and behaves as a molecular sieve. The mineral is reduced by 6 % per unit volume, with a loss of 12 % in magnesium.
4.
The last identifiable zone is the translucent zone, with hyper (remineralized) mineralized layers and an increased crystalline volume. The translucent zone is not always present along the whole advancing front of the lesion. The width of the translucent zone was found to vary from 5–100 μm, with an average of 40 μm. It contains approximately 1 % of spaces, whereas the sound enamel contains about 0.1 % of spaces. These enlarged spaces are probably located at the periphery of prisms, where the orientation of crystallites changes abruptly. Microchemical studies reported that the fluoride content of the translucent zone is increased. There is an associated loss of magnesium, together with a lower carbonate content. The cone-shaped structure (triangular shaping into enamel) displays an apical part oriented toward the dentin.
See references (Silverstone and Poole 1969; Moreno and Zahradnik 1974; Goldberg et al. 1981; Thylstrup and Fejerskov 1986; Arends and Christoffersen 1986; Kidd and Fejerskov 2004).
This configuration is also detectable in artificial carious lesion, established on abraded labial surfaces of calf teeth, either on windows subjected to mild acid treatments or exposed to acid vapors. However, morphological, chemical composition, and physical property differences must be took into account in the interpretation of the results obtained with bovine teeth substrate when compared with human (Yassen et al. 2011).
The earliest visible change is a loss of transparency, enamel becoming opaque and chalky. Enamel caries may progress slowly (white spots) or become arrested (inactive lesions). In such case the carious lesion becomes brown or yellow. This is related to the presence of wide dark zones in arrested or inactive carious lesion, where it appears as a brown spot. This phenomenon may be controlled by spontaneous remineralization due to saliva and/or toothpastes.
4.3 Occlusal and Proximal Caries
Initial enamel caries may also develop in fissures or in deep occlusal invaginations. In occlusal fissures, a morphological classification has been reported (Newbrun 1983).
1.
V type, wide at the top and gradually narrowing toward the bottom of the fissure. In occlusal fissures, 34 % of such lesions are concerned.
2.
U type displays a constant width in the top and bottom of the fissure (14 %).
3.
I type appears as a narrow space between cusps (19 %).
4.
IK type, with a narrow space associated with a larger space in the bottom (26 %).
5.
Other types (7 %).
Food debris and dental plaque accumulate in fissures and produce acid fermentable carbohydrates, which give rise to initial hard tissue dissolution and consequently to carious lesions. The carious lesion starts often at both sides of the fissure wall rather than at the base. The cone-shaped lesion penetrates nearly perpendicularly toward the dentinoenamel junction. These lesions precede cavitation and occur without apparent break in the enamel surface.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


