Age group (yrs)
Year of investigation
20
30
40
50
60
70
80
1973
27.2
25.8
23.2
21.5
18.2
13.3
1983
27.4
26.9
24.8
22.7
18.6
15.5
13.7
1993
27.3
27.3
26.6
24.7
21.7
18.1
15.7
2003
27.4
27.2
26.5
26.1
23.3
20.7
18.4
18.2.2 Its Cornerstones
The topics that have played a major role in the development of the MID philosophy are presented below.
Fluoride: Many studies from 1940 onwards that have assessed the effect of water fluoridation and fluoride toothpaste, varnish, gel and mouth rinses on the progression of carious lesions have contributed greatly to the development of the MID philosophy. These studies have shown that the main long-term action of fluoride retards the progression of a carious lesion, rather than preventing its development (Backer-Dirks et al. 1961).
Sugar: Studies from the 1950–1970 period that assessed the effect of various forms of sugar-containing food and beverages revealed that free sugar is an aetiological factor in the onset and progression of carious lesions and that its detrimental effect can be countered by reducing sugar intake and frequency of consumption.
Dental biofilm: This topic was researched extensively in the 1960s–1980 period. The outcomes of this research resulted in the acceptance that dental biofilm, when allowed to become cariogenic, is the main cause of demineralisation of tooth surfaces. Biofilm should be at least disturbed or at best removed from tooth surfaces daily, if carious lesion development is to be minimised. In combination with fluoride toothpaste, biofilm removal with a toothbrush has become a major cornerstone in managing carious lesions for communities worldwide (Frencken et al. 2002).
Adhesive dental materials: With the appearance of the first research article on the use of composite resin in humans (Buonocore 1955), tooth cavities could be physically reduced in size, with the result that more healthy tooth structure could remain in place. With the appearance of the first glass-ionomer cement in 1969, a biologically based adhesive dental material was introduced (Wilson and Kent 1972), which provided preventive care (sealants) and restorative care (restorations).
Removal of carious tissue: Retaining sound tooth structure, and thus increasing the chance of maintaining tooth vitality and function, was further increased as a result of the work conducted by scholars such as Massler (1967) and Fusayama (1997) from 1960 to 1980. These authors showed that only the ‘infected’ (‘outer carious’ or ‘decomposed’) dentine needed to be removed as part of the cavity preparation process and that the ‘affected’ (‘inner carious’ or ‘demineralised’) dentine could remain. This demineralised dentine would remineralise under a well-placed, well-sealed and well-maintained restoration (Ngo et al. 2006; Alves et al. 2010; Peters et al. 2010).
Repeat restoration cycle: This important cornerstone of MID showed that ‘eliminating’ carious lesions to improve oral health through restorative procedures based on the G.V. Black concept does not keep teeth functional for life for all individuals. The repeat restoration cycle clearly demonstrated that preventive or nonoperative actions should go hand in hand with restorative care and that assessment of carious lesion development and progression plays a vital part in the provision of adequate oral health care (Elderton 1990).
By early 1990, research had shown that managing dental carious lesions should depart from the traditional surgical approach and move to a ‘biological’ or ‘medical’ approach. The research pointed to a completely new approach in the management of the carious lesion.
This new management approach is named minimal intervention dentistry. Its aim is to keep teeth healthy and functional for life. This is achieved through implementing the following important strategies for keeping teeth free from carious lesions: (i) early caries detection and assessment of caries activity and caries risk with validated instruments, (ii) remineralisation of demineralised enamel and dentine, (iii) optimal caries-preventive measures, (iv) minimally invasive operative interventions, and (v) repair rather than replacement of defective restorations (Tyas et al. 2000). It is evident from these strategies that MID does not exclusively equate to cutting smaller cavities than before, as many dentists had initially thought (McIntyre 1994; Burke 2008).
The aspects of the first three MID strategies ‘early caries detection and caries activity and risk assessment’, ‘remineralisation of demineralised enamel and dentine’, and ‘fluoride as a caries-preventive measure’ are presented in Chaps. 9, 14, 15, 16, respectively. These aspects of the strategies should be employed throughout a person’s life, and only when oral health maintenance has failed and a cavity has developed should a minimally invasive operative intervention be undertaken. The effectiveness of some non-fluoride caries-preventive measures and the last MID strategy (repair versus replacement of faulty restorations) are discussed in the present chapter.
18.3 Managing Dental Caries
‘Dental caries’ is the name of a disease and a carious lesion is the consequence of the caries process over time. A carious lesion appears in various forms, which vary from a small demineralised area in enamel to a large cavity in dentine with or without pulpal involvement. The two major aetiological factors that govern the development and progression of a carious lesion are the supply of fermentable carbohydrates, particularly free sugars, and the inability to remove the cariogenic bacterial biofilm from a tooth surface adequately and regularly. These factors are behaviourally determined and, therefore, form the foundation for the understanding that dental caries is a behavioural and not an infectious disease as many dentists erroneously think and are being taught in many dental schools in countries around the world. One should realise that removing microorganisms cannot cure dental caries, neither is a dental carious lesion caused by specific microorganisms as was thought in the past (Chap. 5).
18.3.1 Managing Enamel Carious Lesions: Therapies Other Than Fluoride and Infiltration
As was mentioned at the start of this chapter, a significant reduction of cavitated dentine carious lesions has been observed worldwide in the last three decades (WHO 2013). Because of this positive development, the need for concentrating more on the detection and registration of early signs of dental caries has become evident. Although caries detection and assessment systems, that included enamel carious lesions, have been available since the 1950s (Backer-Dirks et al. 1961; Marthaler 1966), new caries detection systems that include enamel lesions have been developed in the last decade. These systems are distinctly different from the one usually recommended by the World Health Organization (WHO), which only records obvious cavitation in dentine. Examples of such new systems are the Nyvad criteria (Nyvad et al. 1999), ICDAS (Pitts 2004) and the CAST instrument (Frencken et al. 2011). As a consequence of this shift in approach, a variety of nonoperative approaches, tailored to avoid the progression of enamel carious lesions into frank cavitation, have been developed and investigated. The most studied therapy for controlling enamel carious lesions concerns the use of fluoride in its different presentation forms. The mode of action and effectiveness of these forms are presented in detail in Chap. 15.
More recently, a microinvasive therapy initially developed for controlling enamel carious lesions located at approximal surfaces has been proposed (Paris and Meyer-Lueckel 2010). This therapy, called resin infiltration, has received a great deal of attention from researchers and has shown promising results that are discussed in Chap. 17. Therapies other than fluoride and resin infiltration that also aim at controlling enamel carious lesions are being propagated. These therapies are presented below.
18.3.1.1 Casein Phosphopeptides-Amorphous Calcium Phosphate
Studies in vitro, in situ and in humans have shown that casein phosphopeptides (CPP) have a caries-inhibiting effect, which is explained by their ability to stabilise calcium and phosphate and keep them in a soluble amorphous state (ACP) (Reynolds 1998). When in their ionic form and in the face of a cariogenic challenge, both calcium and phosphate ions can be released, which reduces the demineralisation and stimulates the remineralisation process (Andersson et al. 2007; Yengopal and Mickenautsch 2009).
CPP-ACP is present in chewing gums, mouth washes, topical creams, and, more recently, in varnishes. Moreover, as CPP-ACP has been shown to have a synergism with fluoride, some CPP-ACP-based products to which fluoride has been added, such as topical creams, are available.
Three systematic reviews have been published with regard to CPP-ACP effectiveness in caries prevention. Two of these reviews were published before 2010 (Azarpazhooh and Limeback 2008; Yengopal and Mickenautsch 2009) and suggested that more in vivo studies with long follow-up periods were needed, specifically to compare CPP-ACP with fluoride compounds, before the clinical benefits of the product observed in some clinical trials could be generalised. More recently, a review that was aimed at assessing the effectiveness of CPP-ACP formulations of Tooth Mousse® and Tooth Mousse Plus® (which contains fluoride) in preventing and treating enamel carious lesions did not identify any significant benefit of applying Tooth Mousse® over brushing with fluoridated toothpaste. Moreover, evidence that Tooth Mousse Plus® presents any advantages over Tooth Mousse® was not observed. Similarly to the other two reviews, the authors of the most recent published review concluded that more well-designed randomised clinical trials are required before Tooth Mousse® products can be recommended for preventing and treating enamel carious lesions (Raphael and Blinkhorn 2015).
18.3.1.2 Ozone
Ozone therapy for treating carious lesions relies on the fact that ozone kills bacteria by destroying microorganism cell walls and cytoplasmatic membranes (Yamayoshi and Tatsumi 1993). From a simplistic view, one might immediately conclude that such a therapy is likely to be very effective in avoiding the occurrence of carious lesions or in arresting the lesions already present, as such lesions will not be initiated or progress in the absence of bacteria. However, controversial results regarding the effect of ozone on cariogenic bacteria have been presented. The application of ozone failed to reduce the amount of viable bacteria in infected dentine beneath demineralised enamel (Baysan and Beighton 2007) and also in cariogenic biofilm (Müller et al. 2007b). Nevertheless, it was effective in killing Streptococcus mutans, Lactobacillus casei and Actinomyces naeslundii in an in vitro experiment (Johansson et al. 2009).
A systematic review of the literature in which the clinical application and remineralisation potentials of ozone in dentistry were assessed concluded that, while the results of laboratory studies have shown promise for using ozone in managing dental and root caries, clinical studies have not been able to prove that ozone therapy is superior to other nonoperative therapies (Azarpazhooh and Limeback 2008). The same conclusions have been pointed out in two other reviews that recommended, in addition, that more well-designed clinical trials are needed, specifically to compare ozone with other caries-preventive therapies such as fluoride, oral hygiene control, sealants and chlorhexidine (Burke 2012; Almaz and Sönmez 2015).
18.3.1.3 Chlorhexidine-Containing Agents
Chlorhexidine is available in mouth rinses, gel and varnish. At high concentrations, chlorhexidine is bactericidal; at low concentrations, it is bacteriostatic. The dental caries prophylactic effect of chlorhexidine in its various products has been investigated in a number of systematic reviews (van Rijkom et al. 1996; Zhang et al. 2006; James et al. 2010; Slot et al. 2011), with the latest, Cochrane Review, published in 2015 (Walsh et al. 2015). The authors of the latest review found ‘little evidence from the eight trials on varnishes and gels included in the review to either support or refute the assertion that chlorhexidine is more effective than placebo or no treatment in the prevention of dental caries or the reduction of mutans streptococci levels in children and adolescents’. Furthermore, evidence that in the absence of regular professional tooth cleaning and oral hygiene instruction, chlorhexidine varnish provides a beneficial effect in special needs patients is weak (Slot et al. 2011).
The overall conclusion about chlorhexidine as a carious lesion control agent is that evidence of its effectiveness in mouth rinses and gel products is not available (van Rijkom et al. 1996; James et al. 2010; Walsh et al. 2015). Chlorhexidine varnish can at best be considered a short-term option for carious lesion control in individuals at high-caries risk who have high microorganism counts (Whelton and O’Mullane 2001; Du et al. 2006; de Amorim et al. 2008) such as children suffering from severe early childhood caries, people wearing fixed orthodontic appliances (Derks et al. 2004) and elderly people with reduced salivary flow (Slot et al. 2011). Treatment by means of chlorhexidine varnish should be accompanied by biofilm removal.
18.3.1.4 Sealants
Indications for Placing a Sealant
As sealants are usually placed in erupted (pre)molars, the level of caries experience of the child in their primary dentition is a good predictor of carious lesion development in pits and fissures of permanent molars (Disney et al. 1992). But being a high-caries risk child is not enough of a reason to place a sealant according to cost-effective principles. Also the caries risk at the tooth surface level should be established. Pits and fissure morphology (medium and deep) in combination with or without signs of carious lesion activity (presence of biofilm, roughness and/or whitish colour of the surface) are factors that determine the state of carious lesion in pits and fissures (see Chaps. 9, 11, 16, 19).
Sealing aims to modify patent pits and fissures into smooth surfaces that are protected from bacterial colonisation and exposure to fermentable substrates and that can be cleaned easily. The strategy is effective not only as a preventive measure but also in arresting non-cavitated enamel carious lesions in pits and fissures (Griffin et al. 2008). The superiority of pit and fissure sealants over fluoride varnish application in the prevention of occlusal carious lesions has been reported (Hiiri et al. 2010).
Glass-ionomers are more hydrophilic than are resin-based materials. It is therefore logical to assume that a glass-ionomer rather than a resin-based material should be used in sealing carious lesion-prone pits and fissures that cannot be kept absolutely moisture-free, such as in just erupting molars and in children with behaviour problems.
Resin-Based Sealants
Resin-based materials, auto- and light-cured, have a long tradition of use as a material for sealing pits and fissures. Controversy exists about whether a resin sealant needs to be applied under rubber dam or under cotton wool roll isolation. If the latter method is used, the dentist has to ensure that the tooth surface will not be contaminated with saliva and kept moisture-free after washing the etch gel away. Four-handed dentistry might then be a necessity. Etching and light-curing time differs from one product to the other and it is therefore important to read the manufacturers’ instructions. When using light-cured resin sealant material, the dentist has to realise that the material can shrink by up to 4% and that unpolymerised sealant, containing Bisphenol A (BPA) and/or BPA-DM, is left at the surface layer. This layer can easily be removed when adjusting the bite or through wiping the surface with a cotton pellet.
One of the guiding principles of MID is that biomimetic dental material is used. As the toxic BPA and BPA derivates are released from dental resins (Fleisch et al. 2010; Kingman et al. 2012), this material needs to be adapted. These substances have been linked to a number of biological disorders (Eng et al. 2013; Jedeon et al. 2013; Yeo et al. 2013). This development has led the World Dental Federation (FDI 2013) to issue a policy statement on BPA, in which it discourages BPA use in the manufacturing of dental materials.
Atraumatic Restorative Treatment (ART) High-Viscosity Glass-Ionomers
ART sealants use a high-viscosity glass-ionomer, which is placed over carious lesion-prone pits and fissures under finger pressure. Hand instruments (such as an excavator and an applier/carver) are used for adjusting the bite and removing excess glass-ionomer material. In applying this approach, sealants can be placed in situations independent of the need for rotary instruments and thus electricity and running water.
Effectiveness of Fissure Sealants
In the literature, effectiveness is often expressed as the survival of fully and partially retained sealants and as the survival of cavitated dentine carious lesion-free tooth surface.
We know that sealants deteriorate over time. The rate of sealant deterioration varies from brand to brand but is on average higher among the group of glass-ionomer- than resin-based materials (Kühnisch et al. 2012). Among the glass-ionomers, retention of the high-viscosity type, particularly when applied under finger pressure as part of the ART approach, is on average higher than for the medium-viscosity type (van ’t Hof MA et al. 2006). Encapsulated high-viscosity glass-ionomers (HVGIC) show higher mechanical strengths values than the hand-mix version (Dowling and Fleming 2009).
Despite the early exposure of parts of pits and fissures to the oral environment, the failure rate, expressed as the development of a cavitated dentine carious lesion, is not higher in glass-ionomer-based than in resin-based sealants (Beiruti et al. 2006a; Yengopal et al. 2009; Ahovuo-Saloranta et al. 2013). This phenomenon led Frencken and Holmgren (1999) to state that sealant retention should be considered only a surrogate endpoint of sealant effectiveness. The true endpoint is the absence of a cavitated dentine carious lesion in pits and fissures.
Comparison Between ART Sealants and Resin Sealants
As most long-term comparisons between the effectiveness of glass-ionomer-based materials and resin composite sealants over the last decade have used HVGIC applied according to the ART approach, it is of interest to analyse the outcomes of these comparisons. A total of five research articles could be retrieved. These covered studies of 2–5 years long carried out between 2006 and 2015 in Brazil, China and Syria, using the hand-mixed high-viscosity glass-ionomers Fuji IX (GC, Tokyo, Japan), Ketac Molar (3M ESPE, Seefeld, Germany) and Ketac Molar Easymix (3M ESPE, Seefeld, Germany) and the light-cured resin sealants Clinpro (3M ESPE, Seefeld, Germany), Delton (3M, St Pauls, USA), Fluoroshield (Dentsply, York, USA) and Helioseal (Ivoclar, Schaan, Liechtenstein).
Of the five studies, one showed a significantly higher cavitated dentine carious lesion-preventing effect in occlusal surfaces for ART/HVGIC than for resin composite sealants (Beiruti et al. 2006b), while no difference was obtained in the four remaining studies. Three studies used the same ART carious lesion assessment criteria (Beiruti et al. 2006b; Zhang et al. 2014; Hilgert et al. 2015) while four studies sealed only high-caries risk occlusal surfaces in first permanent molars (Beiruti et al. 2006b; Zhang et al. 2014; Liu et al. 2014; Hilgert et al. 2015) (Table 18.2). Given that, in addition to the methodological differences, different brands of materials and different operators were used, it is remarkable that sealants produced through the ART procedure using high-viscosity glass-ionomers show a similar or significantly higher performance than resin composite sealants, which were considered to be the reference sealant material (Deery 2013).
Table 18.2
Comparison of the effectiveness of ART/HVGIC and resin composite sealants in preventing cavitated dentine carious lesion development in occlusal surfaces by year of study
|
Author
|
Year
|
ART/HVGIC
|
Resin composite
|
Test outcome
|
||
|---|---|---|---|---|---|---|
|
N
|
%
|
N
|
%
|
p-value
|
||
|
Beiruti et al. (2006b)
|
5
|
139
|
94.1
|
115
|
78.8
|
0.003
|
|
Barja-Fidalgo et al. (2009)
|
5
|
21
|
87.0
|
28
|
80.0
|
0.27
|
|
Zhang et al. (2014)
|
4
|
239
|
97.3
|
297
|
96.4
|
0.31
|
|
Liu et al. (2014)
|
2
|
179
|
92.7
|
178
|
96.1
|
0.17
|
|
Hilgert et al. (2015)
|
3
|
69
|
90.2
|
169
|
91.4
|
0.59
|
On the basis of extensive evidence, the use of dental sealants is strongly recommended for all at-risk surfaces. Both resin composite material and high-viscosity glass-ionomers, in combination with the ART approach, show good results (Table 18.3).
Table 18.3
Overview of the preventive agents and their evidence-based effectiveness
|
Non-fluoride agents
|
|
|---|---|
|
CPP-ACP
|
Lack of evidence that it is superior to protection offered by fluoride agents
|
|
Ozone
|
Lack of evidence
|
|
Chlorhexidine
|
The evidence for the varnish is low. It may be a short-term option for carious lesion control in individuals at high-caries risk who have high microorganism counts. There is a lack of evidence for mouthwash and gel
|
|
Sealants
|
The evidence is high compared to no sealing. Particularly suitable for high-caries risk children
|
18.4 Managing Dentine Carious Lesions
18.4.1 How Does One Manage a Dentine Carious Lesion?
Providing a response to this question is not straightforward. The answer will depend on the stage of the carious lesion. Activities aimed at managing such a lesion should be directed at inactivation/control of the disease process, preservation of dental hard tissue, avoidance of initiating the cycle of re-restorations, and preservation of the tooth for as long as possible (Schwendicke et al. 2016).
Inactivating the disease process is achieved by controlling the amount and frequency of free sugar intake daily and by removing the (cariogenic) biofilm from any tooth surface on a daily basis. Preservation of dental hard tissue is achieved by applying minimally invasive operative interventions and by removing only soft to firm tooth tissue from within a tooth cavity, allowing the remaining demineralised dentine to remineralise. The repeat restoration cycle can be avoided if the cleaned cavity is restored under optimal clinical conditions with an appropriate restorative material. An additional measure is the protection of the margins with a sealant material, which results in a so-called sealant-restoration (Simonson and Stallard 1977). Daily removal of the biofilm from all tooth surfaces will ensure that the tooth is preserved for a long time, provided that the periodontal tissues are kept healthy.
The MID philosophy seeks to preserve natural tooth tissue for as long as possible through not removing enamel and dentine tissue unnecessarily and by supporting remineralisation of demineralised enamel and dentine. Hence, non-restorative treatments have a place in managing dentine carious lesions within MID. For permanent teeth, such a treatment is suggested for non-cavitated dentine carious lesions, while in primary teeth this treatment is advocated for both non- and cavitated dentine carious lesions, as shown in Fig. 18.1.
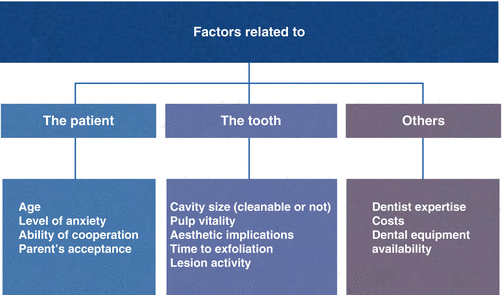

Fig. 18.1
Factors that should be considered when opting for non- or restorative treatment in the primary dentition
18.4.2 Non-cavitated Dentine Carious Lesions
Non-cavitated enamel carious lesions can be managed through diet control, biofilm control with fluoride-containing toothpaste and, on indication of high caries activity in pits and fissures, through the application of a fissure sealant. These activities have been shown to be effective in reducing or stopping the activity of the caries process (Frencken et al. 2012a). But what would be the treatment for a dentine carious lesion without an obvious cavitation? This condition is recorded when the ICDAS system and the CAST instrument (Code 4) are used. It is obvious that such lesions present a challenge to the dental practitioner. Can such a dentine carious lesion be sealed over in the same way as enamel carious lesions? Unfortunately, not many studies have investigated this condition; however, a few approaches have been proposed. It has been suggested that active lesions that are visible on radiographs can be either sealed or restored according to the MID principles (Ismail et al. 2013). Although not much evidence exists regarding the use of noninvasive procedures in this type of carious lesion, the application of pit and fissure sealants over non-cavitated dentinal occlusal carious lesions has been shown to be effective in arresting carious lesion progression after 36 months of follow-up in a group of high-caries risk patients (Borges et al. 2012).
It appears that insufficient evidence is available to guide the dental practitioner in the best way to treat such a condition. Strangely, more information, originating from decades ago, is available for treating small cavitated dentine carious lesions. A similar question as posed above can be formulated: Do small cavitated dentine carious lesions need to be treated restoratively or could a sealant be an effective treatment? This issue is dealt with in the section below.
18.4.3 Small Cavitated Dentine Carious Lesions
Evidence about sealing cavitated dentine carious lesions in permanent teeth comes from a clinical trial in which medium-sized cavities in occlusal surfaces were treated with a sealant restoration without removing soft ‘infected’ dentine. The study showed a success rate of 86% after 10 years (Mertz-Fairhurst et al. 1998). Since then, discussions have been held in the literature and in congresses about the need to remove all soft dentine tissue from tooth cavities in order to stop carious lesion progression. The slogan ‘The Seal is the Deal’ was born (Kidd 2004a). Would this slogan be applicable for treating small dentine carious lesions in pits and fissures? A few studies to this effect have been published.
Already in the mid-eighties, Mertz-Fairhurst et al. (1986) showed that sealing over small dentine lesions in pits and fissures stopped carious lesion progression. The authors based this finding on the assessment of lesion depth and bacterial counts and on radiographic and clinical examination. Years later, small dentine lesions (<0.9 mm orifice) in subjects that were on average 14-year-old were sealed with a medium-viscosity glass-ionomer according to the ART principles. These sealants had prevented dentine lesion progression in 87.4% of the cases after 3 years in this low-caries risk group, which was a significantly higher percentage than for small dentine lesions that were left untreated (Frencken et al. 1998). In a medium-caries risk group of 7-year old, dentine carious lesion progression was stopped in 68.2% of small dentine carious lesions (<0.9 mm orifice) that were sealed over with resin composite and high-viscosity glass-ionomers after 5 years (Beiruti et al. 2006b). These studies compared the therapeutic sealant to no sealant use but what might one expect if the effectiveness of the therapeutic sealant were compared to a restoration?
Such an investigation has been performed in primary teeth over 18 months (Hesse et al. 2014) and in permanent teeth over 2–3 years (Bakhshandeh et al. 2012). Compared to conventional restorative treatment, the survival of sealed over cavities with a resin fissure sealant material was significantly lower in both studies. The results of these studies show that not only should one attempt to stop carious progression in these cavities noninvasively but that this practice is limited by the strength of the sealing material used. According to an in vitro study, sealing small cavitated dentine carious lesions in pits and fissures showed a higher level of micro-leakage and insufficient penetration of resin sealant material into the cavity, compared to sound pits and fissures (Hevinga et al. 2008).
Evidence so far shows that sealing over obvious dentine cavities with a (resin) fissure material is not indicated but that sealing over small dentine carious cavities is worth pursuing. The reasoning for performing this treatment on small dentine carious lesions relates to the fact that an invasive intervention can still be performed should the sealant not function well anymore. More research regarding this noninvasive treatment is necessary before this treatment becomes commonly used.
18.4.4 Obvious Cavitated Dentine Carious Lesions in Primary Teeth
18.4.4.1 Cleansable Cavitated Dentine Carious Lesions
From a cariological point of view, removing the biofilm from within the cavity with a toothbrush and fluoride-containing toothpaste, sometimes supported by regular application of a fluoride varnish in the cavity or a glass-ionomer base, can inactivate open cavitated dentine carious lesions. But, for this strategy to be effective, the cavity should be cleansable or made cleansable by removing obstructing enamel structure and/or dentine tissue with rotary or hand instruments. G.V. Black (1908) wrote about this noninvasive, non-restorative cavity control treatment as follows: ‘All buccal and labial cavities in which decay is burrowing should be fully opened by clipping away all the overhanging enamel and left as wide open as possible in order to admit free washing, both in artificial cleaning and in fresh clean saliva.’ But, what evidence exists for recommending non-restorative procedures? Some techniques have been proposed and investigated for application in the primary dentition. These are discussed below.
Ultraconservative Treatment
Two retrospective studies carried out in the UK in which primary teeth remained unrestored but received preventive care showed that the majority of the teeth (82%) exfoliated naturally and symptomless (Tickle et al. 2002; Levine et al. 2002). Considering these results and the fact that primary teeth have a relatively short life span, a prospective study was performed that compared a mainly non-restorative procedure with two restorative procedures. The rationale behind the study design was that regular toothbrushing with fluoridated toothpaste (1 100 ppm) would be sufficient for preventing medium- to large-sized cavitated dentine carious lesions from progressing while the difficult-to-clean small cavities could be restored using the ART approach (Frencken et al. 2012b). Some medium and large cavities were opened further using hand instruments to allow proper removal of biofilm with a toothbrush. This protocol was termed ‘ultraconservative treatment’ (UCT). The UCT protocol was compared to the ART and to amalgam restorations in a group of high-caries risk children aged 6 to 7 years. Results showed no significant difference between the survival rates of teeth that were restored and those treated using the UCT protocol after 3.5 years (Mijan et al. 2014). There was also no significant difference in the exfoliation pattern of primary molars between the three treatment protocols after 3.5 years (Mijan et al. 2015). About 88% of teeth treated using UCT exfoliated without any pathology and/or toothache (Mijan et al. 2015).
Such results reinforce the idea postulated by Kidd (2004) that nonoperative treatments can lead cavitated deciduous teeth to exfoliate without pain. However, it is important that more studies in which similar approaches are tested are conducted. These are necessary not only to generate evidence about this treatment protocol but because nonoperative approaches based on diet and oral hygiene control may turn out to be the best strategy for overcoming the reality reported by Marcenes et al. (2013), that untreated cavitated dentine lesions in primary teeth affect more than 620 million children in the world. Treating these cavities restoratively is simply not possible and might not be needed.
Silver Diamine Fluoride
The effectiveness of removing the biofilm from within a cavity in controlling carious lesion progression was thought years ago to be increased by placing silver diamine fluoride (SDF) in the open cavity. SDF is a combination of silver nitrate and sodium fluoride (Ag(NH3)2F). When applied to carious tissues, it inhibits carious lesion progression by its interaction with bacteria (Knight et al. 2007). For that reason, open cavities have been treated using SDF, particularly in primary teeth. The main disadvantage of using SDF is that the lesions treated will be stained black and might displease some children and parents.
In terms of effectiveness, a series of clinical trials has shown that the application of 38% SDF was effective in arresting dentine cavitated carious lesions in upper anterior teeth of children aged 3 to 5 years (Lo et al. 2001; Chu et al. 2002) and in primary canines and molars of 6-year-old schoolchildren (Llodra et al. 2005). Different concentrations (12% and 38%) of SDF were tested in arresting dentine carious lesions in children aged 5, and the results showed that a single spot application of 38% SDF is more effective than the 12% concentration after 24 months but that the effectiveness decreases over time (Yee et al. 2009).
It is concluded that SDF can be considered an alternative treatment for primary teeth where other caries control strategies are not available. However, the optimum frequency of application needs to be investigated.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


